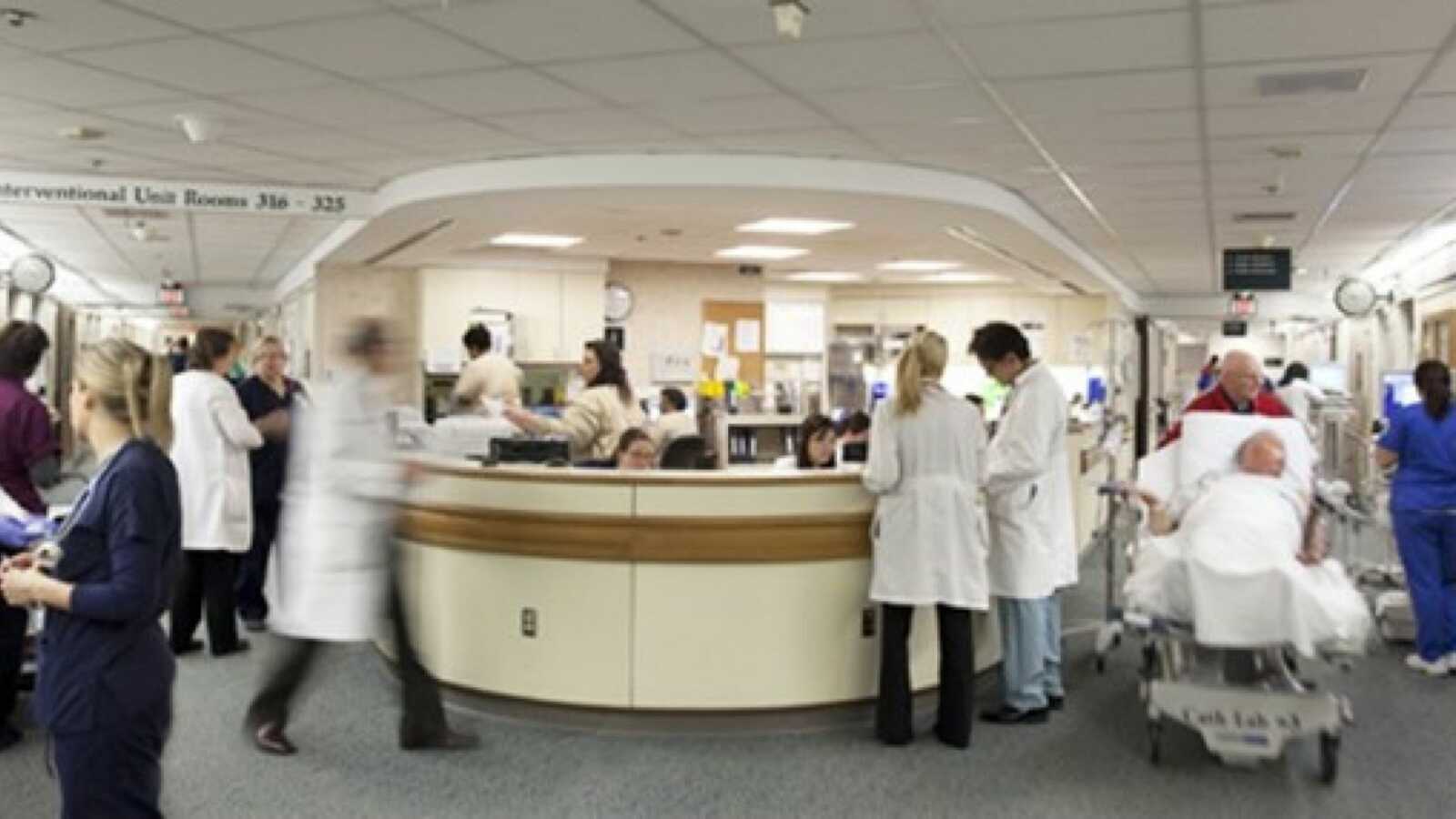
Nurse Duties
“Imagine this…
You walk onto the floor and there are 25 patients.
25 humans your team is responsible for, and 5-6 humans you will have to know everything about.
When they eat, if they eat; how much they pee; what color it is; when their last bowel movement was; what color, shape, and consistency it was; what their labs look like; and their cognitive status.
If they have wounds, what meds are due, and what are their vitals?
And there are only four nurses on the floor that night including you.
You get to the floor and get a report on your 5-6 people.
All is not well, some with orders that need completing.
One has bladder scans every 6 hours and has to be cathed if they are over a certain limit. At least three are on IV infusions every 4-6 hours and require frequent monitoring.
1-2 are aggressive and need to be kept away from others.
At least one had a fall requiring neuro checks every hour. One is dying with no family at their side. And one is suicidal and requires constant supervision by a sitter, and if one isn’t already with them that sitter is you and you can’t leave that room.
Five are on telemetry monitoring and their heart-monitoring electrodes have to stay connected.
Three are on oxygen and constant pulse oximeters to monitor their saturation levels. If they remove their oxygen, their stats drop into the 80s or lower.
One is confused and needs a bed alarm. They are constantly trying to get out of bed and ‘go home’ – and are routinely incontinent of bowel.
Two are already cathed, two have central line IVs, and your confused patient is on their fourth peripheral IV because they keep ripping them out.
Two will be NPO (nothing to eat or drink) at midnight for AM surgeries, so they’ll need chlorhexidine wipe baths before morning as well as pre-procedure checklists done.
Some need doctor’s orders for medications they don’t have in their orders, some don’t even have pain meds ordered and need them.
You call or page the covering doctor just to get orders and then wait for those orders to get filled and sent up by the pharmacy, which could take hours if they’re not in the Accudose.
Then imagine being short-staffed.
Then imagine the family calling wanting a check-up on their family members and complaining when you can’t get on the phone right now.
Imagine you are in the middle of cleaning up a patient, alone, when the family calls, and you can’t stop to take the call but will call them as soon as you’re done.
Imagine your manager reprimanding you for not taking the call as the family is angry and complaining.
When you do get on the phone they are either angry or need comfort themselves, and so you spend 20-30 minutes soothing their fears, going over their loved one’s entire med list, and explaining treatments.
Along with any other of a half hundred questions you might or might not be able to answer, or can’t answer because you can’t diagnose.
Then imagine four of those six calling out for pain meds every two hours.
Some of it is pain seeking, and some of it is actual pain from cancer or other causes.
Then the one who is dying needs pain meds for comfort every hour and just wants someone at their bedside.
Oh, and don’t forget the high fall-risk patients that you have circled around your station so you can keep an eye on them.
Burn Out
When you do go to get medications for your patients, some are in the chartbox lockboxes, some are in the central floor Accudose med cart, some are locked in a double key narcotic box, and some… aren’t there at all, so you spend 5 minutes or more just requesting meds from the pharmacy or running down to pick them up.
Finally, add in 1-2 hour vital signs, including B/P, respiration, heart rate, temperature, O2 saturation %, and 1-2 hourly charting on each patient using a prototype computer software system that isn’t user-friendly.
It’s counter-intuitive and appears to have been designed by at least four people who weren’t communicating with each other during the design process.
Then imagine doing everything you can for all these humans you are responsible for and getting cursed at, talked down to, criticized for not being ‘fast enough,’ and asked, ‘Where were you?’ or told, ‘I’ve been on the light for 20 minutes?!’
NOW imagine also not having enough CNAs – the backbone of the skilled nursing system!
So now, with all of that, you’re also TRYING to help respond to call lights, bathroom calls, changing patients, turning patients every 2 hours, getting water, getting snacks, emptying catheters, measuring intake and output, bathing, and more changing.
Imagine a patient getting upset because you didn’t bring them coffee and snacks quickly enough because you were giving meds for comfort to your dying patient.
And now… you have a new admit coming to the floor with a wound vac, needing pain meds you don’t have because the pharmacy is swamped and is 3-4 hours behind on filling med requests.
At least two of your patients have late meds you must make a note of to ensure your documentation reflects the fact that you simply didn’t have the meds available.
Another human, another life to take care of.
Now imagine administration always complaining you never do enough, dressings aren’t changed on time, tubing isn’t labeled correctly, and rooms are messy.
Charting isn’t done, and write-ups are threatened.
Now try and find time to use the bathroom or take lunch.
This is nursing.
This is why we are burned out.
This is why we are short-staffed.
This is why nurses and CNAs are leaving the profession.”
This story was submitted to Love What Matters by Brion Woods. Join the Love What Matters family and subscribe to our newsletter.
Read more stories like this here:
Help us show compassion is contagious. SHARE this story on Facebook with friends and family.