Living With Chronic Illness
“Each morning before work I take my dog, Maggie, on a walk. Today I set my alarm a bit earlier to allow extra time for a leisurely stroll through the woods. The first thing I do as I take my first breath of this new day is a body scan, beginning with my head and ending with my toes. I quietly make a mental note of each muscle, nerve, or organ my pain has chosen as its feeding grounds for the day.
I roll out of bed gingerly, taking care as I never know whether I’m able to support the weight of this broken body until I step into the unknown. Today, I noticed the old dull pain radiating from deep in my pelvic bowl, and searing zaps slicing between my ribs. I can work with this.
I take my pain medication, plaster cooling patches across today’s invisible wounds, and stuff my inhaler in my pocket. When Maggie and I walk out the door I slip in my ear buds and choose today’s guided walking meditation. I think today I’ll go with ‘grounded.’
From a young age I practiced meditation. My mom had her own personal struggles and found help in Buddhism. Her influence strengthened my ability to cope with life’s hurdles significantly. She gave me the tools to manage the enveloping thoughts that seemed to darken every corner of my mind; tools to accept these thoughts, fold them up into a neat little paper airplane, and let them fly away. Combined with the benefits of seeking counseling at a young age, I was armed for whatever else might be around the corner.
As Maggie and I pass through the red wooden gate into the forest, I feel yesterday’s emotional weight evaporate with my breathing. Breathe in the new day, breathe out the stale air of yesterday. Ever since I began practicing breathwork daily, my respiratory symptoms have noticeably improved. I haven’t used my inhaler in 3 months, but I carry it with me nonetheless.
Autumn has officially settled into Hastings and, while my favorite season, it brings with it a host of anxieties for me. Last November I began coughing up rusty, blood-tinged phlegm. I developed chronic chest pain and recurring infections that left me susceptible to the most innocent virus, not to mention Covid. I had a myriad of tests that year, and in vain I hoped for a diagnosis of something the NHS would be equipped to treat.
Reflecting On My Medical Journey
When my specialist was convinced I had tuberculosis I was genuinely hopeful, for at least this was well understood. I didn’t care how serious such a diagnosis was as long as I wouldn’t be dismissed. I wanted anything except for what I knew in my bones was the truth: thoracic endometriosis.
Over the next few months my symptoms expanded. I developed extreme fatigue and lightheadedness, vertigo, loss of feeling in my fingers, random bruising, rashes, mouth sores, enlarged lymph nodes, and pain in my shoulders and inner ears. The potential diagnosis gradually became less clear as the doctors began suspecting autoimmune dysfunction on top of the endometriosis.
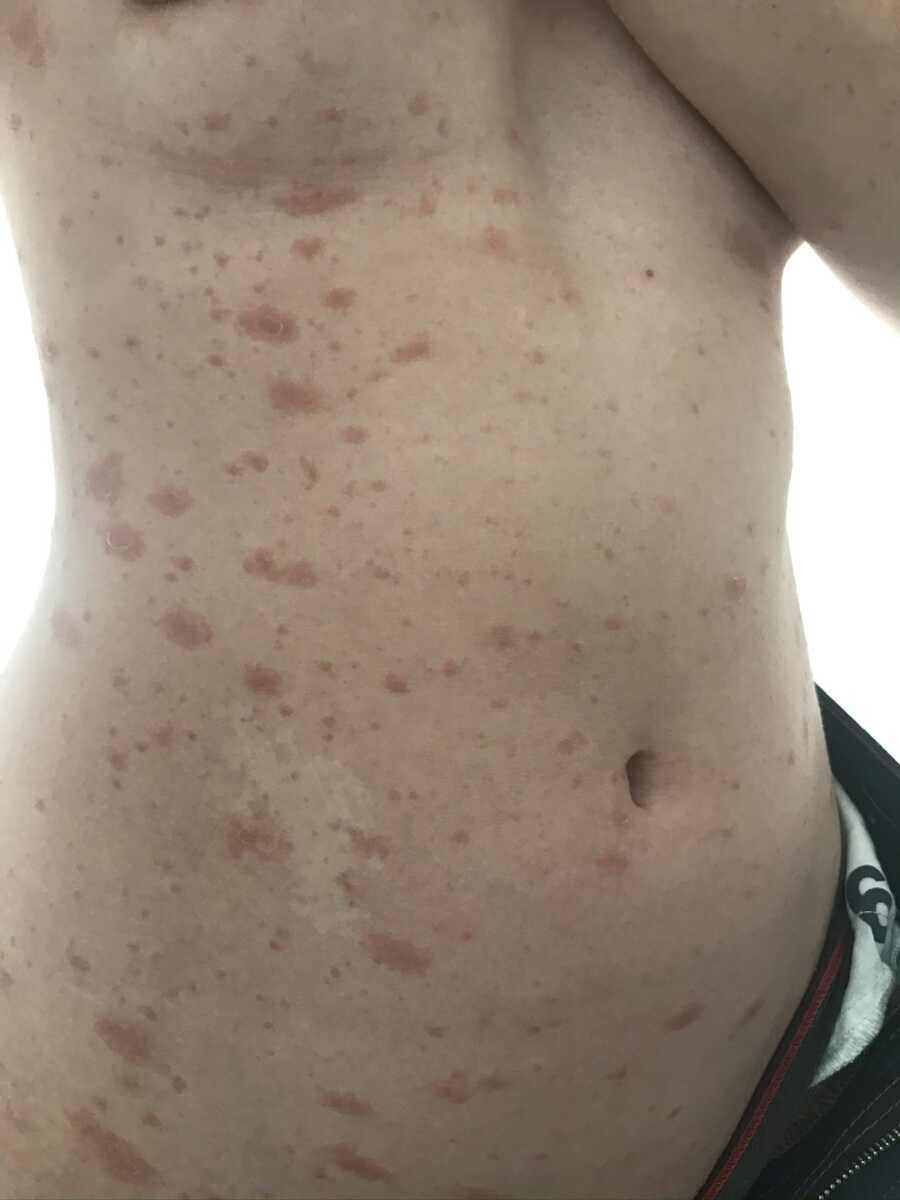
With each test, however, came the dreaded result: normal. The word ‘normal’ is the most terrifying word of all. It means no diagnosis, and subsequently, no treatment. And in my case, it means an ever stronger case for thoracic endometriosis.
I had been speaking to my private specialist who had operated on my pelvis in my most recent surgery for endometriosis, and he was convinced the disease was colonizing my lungs and my diaphragm. We have discussed the only available treatment I have yet to try – a thoracoscopic surgery – and I am in the process of working through the logistics of this prospect.
This, however, does not have the evidential data required to be suggested whole-heartedly as a treatment for such a disease. The medical research for thoracic endometriosis is still in infancy. But I am not scared of surgery; I’m scared of the potential for a lifetime of chronic, disabling pain and I am willing to do anything to change course.
For multiple reasons, however, this surgery won’t be in my near future, and for the time being I must find ways to hold on. As I look up at the tree canopy and admire the silhouette of oak leaves against the stark white overcast, I take a deep breath. The air smells of fresh rain and churned earth.
I let the breath dance down to the lower lobes of my lungs and with this light pressure against my diaphragm I count to four before releasing. Simple breathwork such as this has eased the labor of coping, both physically and mentally. I recall walking through these woods in the summer and having to hobble home breathless after a mere 20 minute stroll.
I still experience the fear and anxiety of stepping outside my home, not knowing when and where the pain will strike; and the pain will indeed strike. However, that fear doesn’t grip me the same way. It kindly alerts me of any signs my body might be giving away, rather than locking me in my room and throwing away the key. It is a calculated, cautious fear born of compassion for myself.
The pressure on my pelvis increases and I feel the elastic waistband of my trousers give way to my bloating stomach. It will always fascinate me how quickly it expands – typically two or three sizes in a half hour. My discomfort grows with fleeting zaps at my six scar sites. I take notice of this, but I don’t clutch at the thought. As I keep a steady walking pace this thought slips from my mind, floating away between the trees.
I am drawn again to my breath, the sound of the mud lightly squishing beneath my boots, and the cool humidity against my face. Maggie turns around to make sure I’m still behind her, and satisfied, returns to her scent trail.
The return of my pelvic pain has brought more trauma than I realized I had housed. After six years of undiagnosed pain – which brought dozens of hospital trips, scans, trial-and-error treatments, medical tests, and unceasing anguish – I received a diagnosis of endometriosis in an NHS hospital the day before Christmas Eve.
At the time, it was the sweetest gift. The validation of a diagnosis was soothing, and it brought the promise of answers, now that the problem was identified. It was not so simple.
My symptoms were only exacerbated by my initial surgery, prompting episodes of pain so severe it stole my ability to walk, eat, and breathe. Doubling over and vomiting was a regular occurrence. As I struggled through the last year of my degree, I would find myself huddled over my swollen belly in a toilet stall, streaming blood and tears, gritting my teeth, and grieving over whatever lecture or seminar I was missing. On my way to work I would hobble into alleys and sob as I wretched. I felt like I was half alive.
In April of 2021 I once again found myself in an ambulance. This particular episode was accredited to possible appendicitis, after the EMTs asked me several times if the pain that had bed bound me and made breathing a struggle could just be my period (because every medical professional knows a normal period leaves you crippled and gasping for breath. Totally normal.)
A resulting emergency laparoscopy confirmed a ruptured ovarian cyst and a mildly inflamed appendix, which was removed; but most importantly, a confirmed negative diagnosis of endometriosis. I was devastated. I had a private excision surgery planned with an endometriosis specialist in four week’s time. What was the point of having this operation if there was nothing on which to operate?
I contacted my surgeon who reassured me many of his patients arrive with a history of misdiagnosis from the NHS, who unfortunately are not equipped to properly identify and treat endometriosis. He said my inflamed appendix was likely caused by endometriosis, and that an NHS general surgeon isn’t trained to recognize it. With this reassurance, I had my third operation.
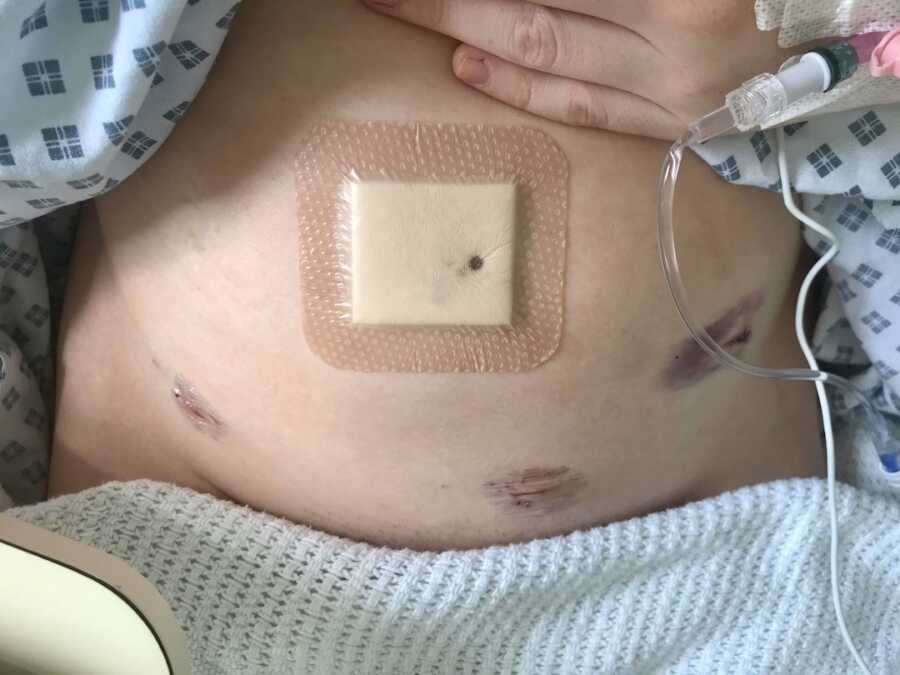
For 15 months I lived nearly free of pelvic pain. Albeit, the chest pain surfaced quite soon after the operation, but I was clinging to my wins. I felt able to take care of myself through this new minefield of thoracic medicine knowing I could walk without worry. I could carry myself. That was enough to encourage my smile.
Recently, however, another hospital trip for severe pelvic pain and a subsequent ‘normal’ scan led my doctors to believe the pelvic endometriosis had returned. The road ahead of me seemed doomed.
I’d had the privilege of undergoing the gold standard of endometriosis treatments with one of the most skilled surgeons in the world, and that still was not enough to grant me relief for the 5 years that had been hoped. The disease was creeping up my body and ravaging organs where medical science had developed no sure solutions thus far. I was in the dark and there was no light out.
I needed to begin processing the possibility of living in pain for the rest of my life. Perhaps peace would be found in this acceptance rather than hoping in vain for a medical miracle, although this will never stop me from advocating for treatment that should not be considered a miracle at all.
Practicing Mindfulness
These thoughts spurred me into action. Using what little motivation I had left, I started seeing a therapist and talking openly to my managers at work about my struggles. I did my best to allow those around me to share my weight, without replacing that weight with guilt as I so often do. I started a new anti-inflammatory diet and got creative in the kitchen. I retreated back to my passion, painting, as an outlet for my grief.


But at the epicenter of these positive changes was the realization that mindfulness was going to save my life. I began to meditate daily. Don’t get me wrong: my symptoms are not determined by my mind. They are very much a physiological reality and must be treated via medical intervention and pain management.
I cannot leave the house without my pain medication and I rely on this to elevate me to a functional level. I use a TENS machine on high-pain days. I have regular hospital appointments for tests and scans. My health and wellbeing depends on taking proper steps to manage my disease. However, my perspective is framed by my mind, and with this I’m able to experience the same pains in different ways.
Actively practicing mindfulness has allowed me to exercise so much compassion toward myself. My heightened awareness of my own body helps me notice triggers and identify the beginning of a flare up so much faster, and I can then take care of myself accordingly.
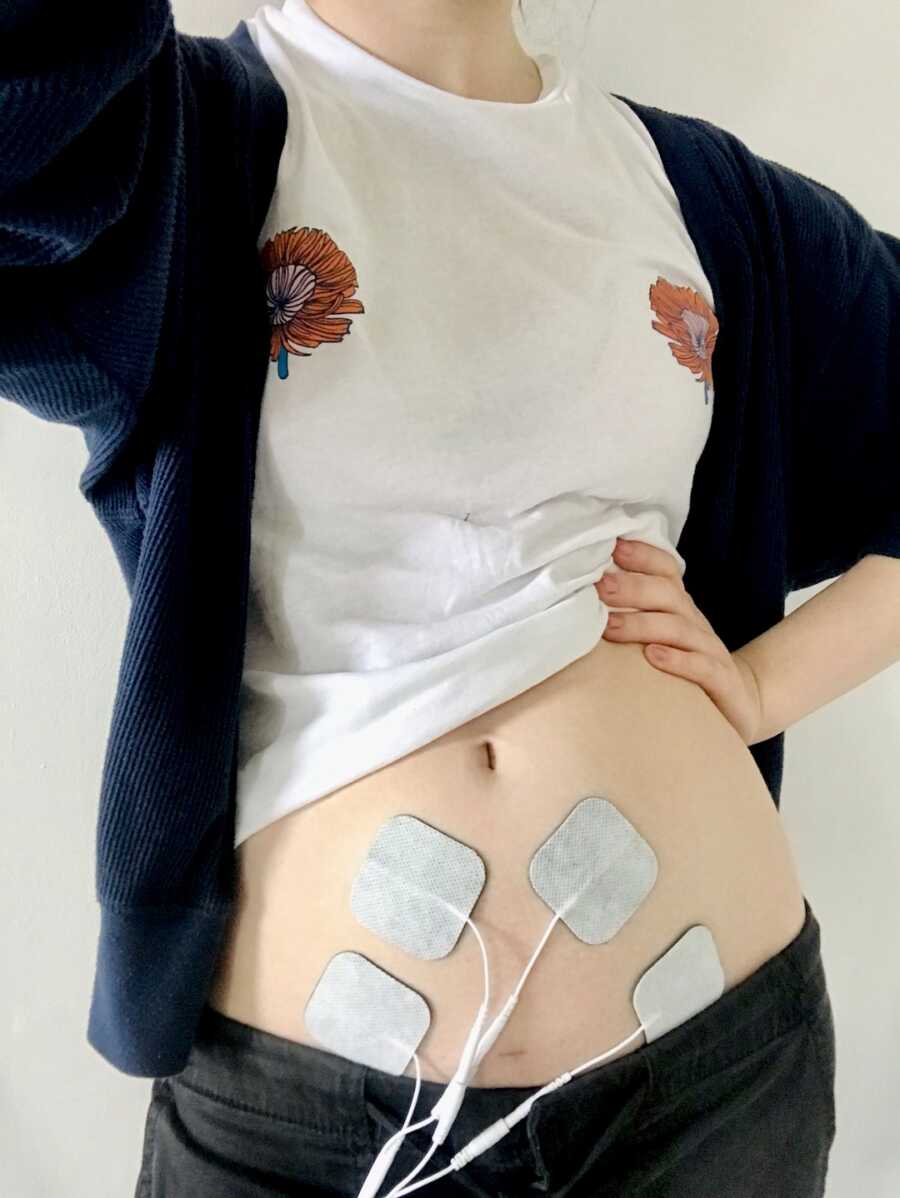
As I sharpened these mindfulness techniques, I decided to share them with others. I created the Instagram page Mind Your Endo with the intention of learning and sharing mindfulness coping strategies alongside other chronic illness warriors. I also have leaned into my art practice as an emotional outlet, and I feel both of these practices have generated spaces for community building, education, and empathy.
It brings me so much joy to be able to trade experiential knowledge with others like me and to enlighten those who will fight alongside us for proper care. None of us are alone, and together we are so fiercely loud. I love it fervently.

From a mental health view, I have been working through the guilt cycles I have thoughtlessly put myself through. I have felt as though I’m not good enough; not able to keep up; not a team player; a complainer; weak. But by sitting with these thoughts, looking at them from different angles, and letting them go completely, I have been able to cope. I’ll admit, I’m not what I would call flourishing, but I am in a place where I feel I can and will survive this. That, to me, is enough.
Maggie’s scent trail leads us up a steep, decaying set of stairs which dissolve into a thick darkness of bramble at the summit. She’s quite strong and I like her to have some freedom despite the leash, so I generally let her lead me. She hustles up the stairs without hesitation and lands her nose straight back to the forest floor at the top. I try to match her pace but a joint resistance in my ribs and deep in my abdomen holds me back.
I feel a subtle rise in temperature in the back of my head. Anxiety creeps over my shoulder. I lock eyes with Maggie and take another step. The resistance grows stronger and louder and a kebab-skewer pang pierces my chest. I gasp and instinctively clutch at my heart. Do I need to go to the hospital? I drown out the pain by bringing the chorus of birds to the foreground of my mind. There are so many of them and it’s so loud. It’s so strange how such a thing can hide in the background of your consciousness so easily. The sharp pain fades into a dull, nauseating ache.
I look back at Maggie and tell her it’s time to go home, and she reluctantly obliges. If I head back now, I think I’ll be able to beat the pain before it consumes me. I’m going to be working from home today so I can rest in bed with my hot water bottle. If it gets worse, I’ll rest knowing my team will understand. I’ll take my pain medication. I’ll put on my TENS machine. I’ll be okay. I’ll just need to take extra care. I’ll be fine.”

This story was submitted to Love What Matters by Maeve O’Briant of Hastings, UK. You can follow her journey on Instagram and check out her art here. Join the Love What Matters family and subscribe to our newsletter.
Read more stories like this:
Do you know someone who could benefit from reading this? SHARE this story on Facebook and Twitter to let others know a community of support is available.

