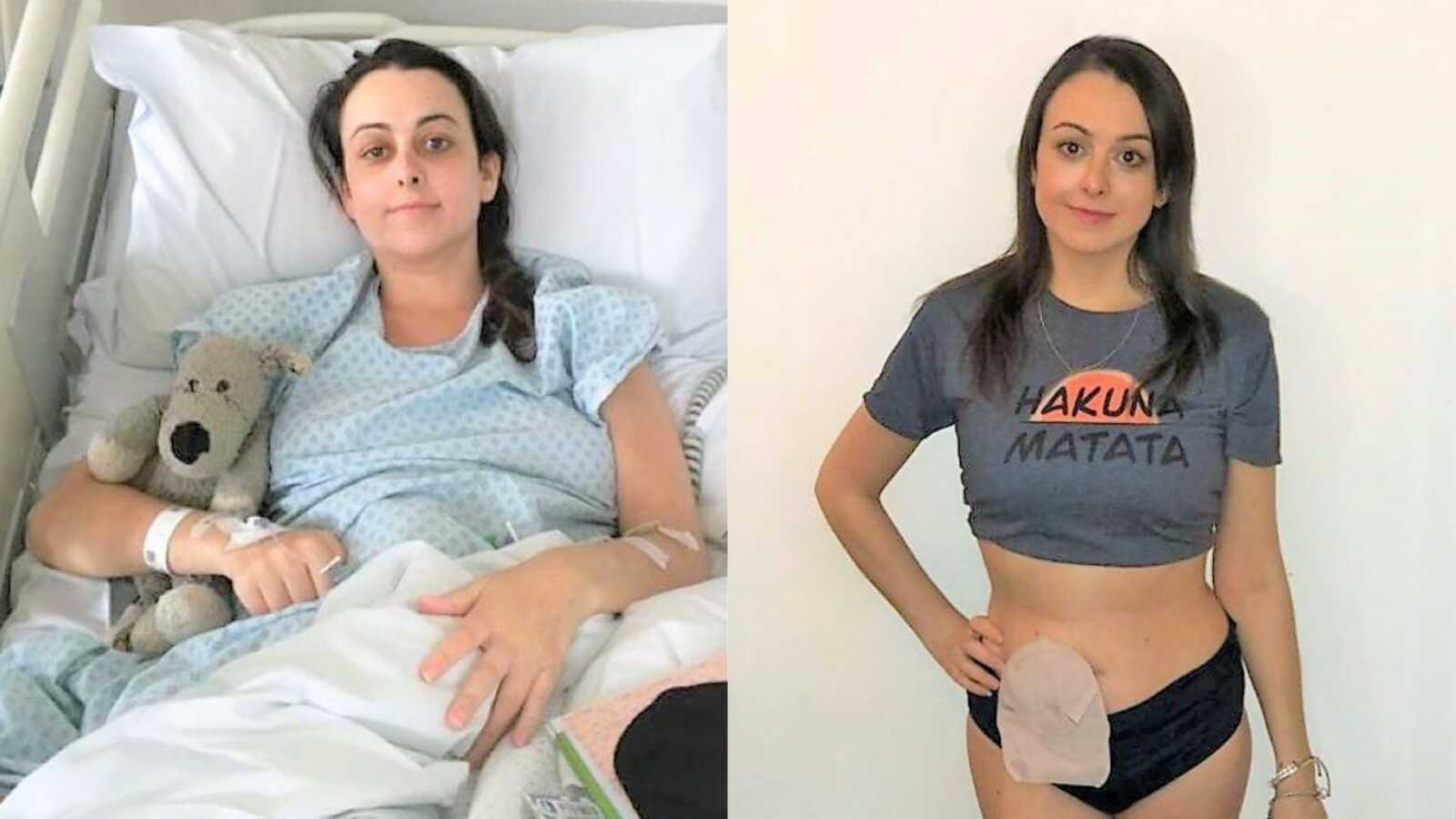
“In summer 2021, my world changed forever. I’ve been so lucky in my life to have never spent time in the hospital, never broken a bone, never been seriously ill, then all of a sudden I was in a potentially life or death situation. In December of 2020, I started to see blood in the toilet. I went to my GP in January as this was becoming a regular thing. They didn’t suspect ‘anything sinister’ and tried me out on various creams and suppositories for hemorrhoids over 3 months (I was later told in the hospital I did not have hemorrhoids).

By March, I was seeing blood every day, so they took a blood test, a stool sample, and sent me for an appointment at the hospital where I was booked in for a colonoscopy. My blood came back with ‘slightly increased inflammation levels’ in my bowel, but I was reassured they were not overly concerned. My colonoscopy happened in June and they were clearly worried as they put a rush on my results.

After 2 days I was experiencing urgency and pain when going to the toilet, and on the third day, I was vomiting. Something was seriously not right. I went to A&E and was admitted 11 hours later. The next day, they explained they expected Ulcerative Colitis; an Inflammatory Bowel Disease whereby an abnormal immune response causes your immune system to attack the cells in the digestive tract causing inflammation and ulcers in the large intestine (colon).
Over the following 3 weeks, I was extremely unwell. I was going to the toilet in severe pain 10-15 times a day, I was being sick regularly, I couldn’t eat and became malnourished, and a lot of the time I couldn’t muster the strength to get out of the hospital bed. Over these 3 weeks, the doctors put me on steroids, which showed no effect, and then on an infliximab infusion to try to bring down the inflammation and stop my immune system from attacking my bowel.
Doctors would pop into my room every day to see how I was doing, and there were hints at the surgery, which I knew meant having a stoma, but I kept being assured we ‘aren’t there yet!’ Due to it being COVID times, I couldn’t see anyone until I had been in at least a week. Looking back this seems like nothing, but at the time I was so shocked and petrified about what was going on it felt like forever, and I felt so alone in my circumstances.
After the first week, I was allowed to see my mom for one hour, and I completely broke down about the whole thing, convinced I wouldn’t be leaving the hospital without a bag on my tummy. My sister kept asking me via text, ‘When can you come home?’ and I kept saying, ‘When I’m better’–and none of us had any idea what it meant. I remember thinking over this time, ‘Why is my body doing this to itself?’ I was so angry at my immune system for failing me. I even laughed and sneered at how stupid it was, imagining how it would have caused its own demise if I were to die. By this point, I felt separate from my own body.
Eventually, after being told I ‘probably would not need surgery,’ a specialist surgeon came in and knelt by the side of my bed. He said, ‘Kathryn, I have to be honest with you now. You’re severely unwell. You’re pale white, your eyes are black, and you look thinner every day. I’m so sorry, but you need this surgery. You are risking your life without it.’ I felt devastated but also relieved I was being told the absolute truth. I waited 2 more days before consenting to the surgery so I could try another round of infliximab and know for sure this was the only way–and by the last day I knew!
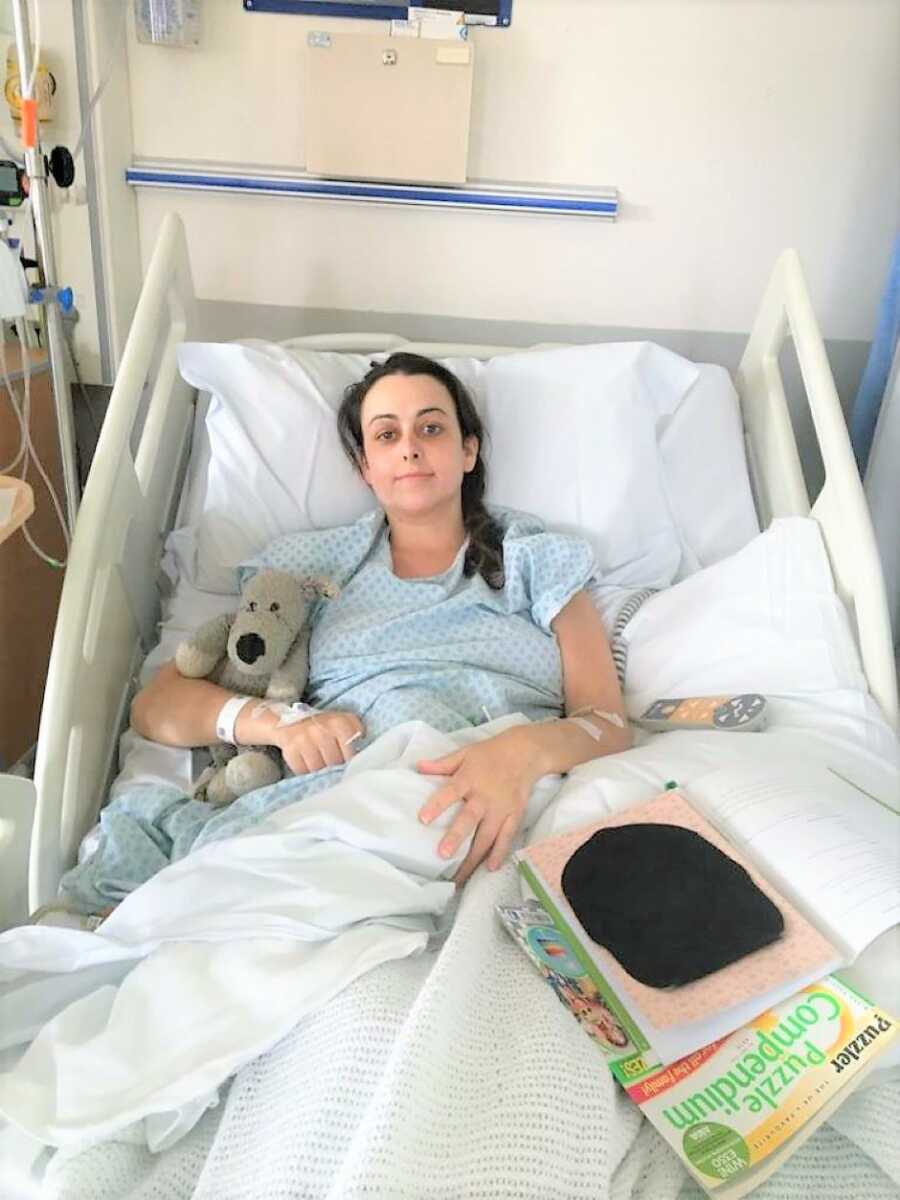
I signed the consent form, had a nurse help me shower and change gowns, had a blood transfusion for anemia, and said, ‘Just take me up, I don’t care anymore.’ I had the surgery. It was a subtotal colectomy, which meant I was given an Ileostomy–my colon was removed and my small intestine pokes out of my tummy like a little button, and I wear a bag over this 24/7 to collect waste; this is called a stoma. About 10 seconds after coming around, I told the nurse I felt like a demon had been exorcised from my body.
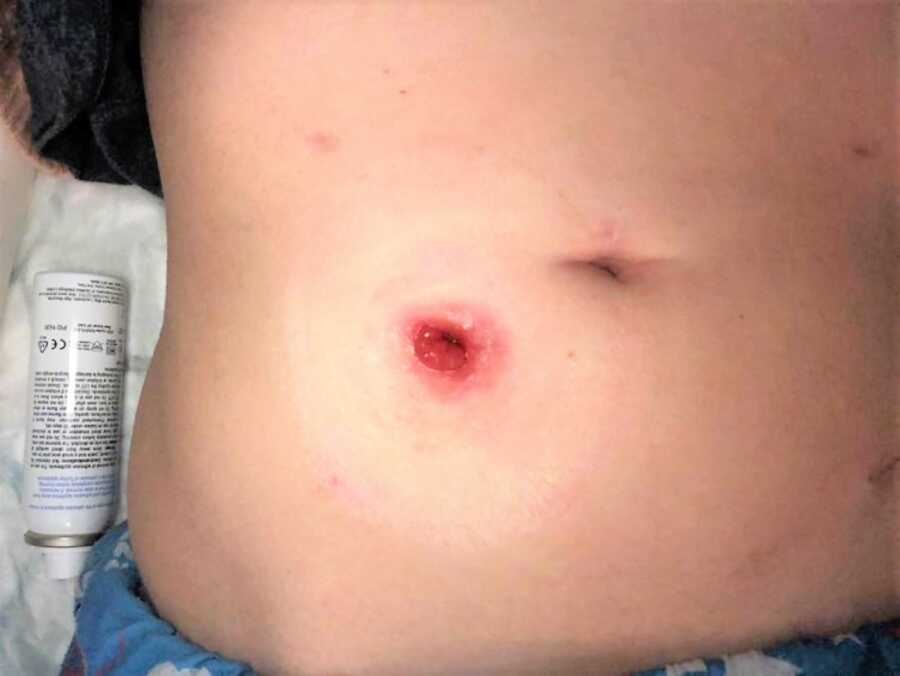
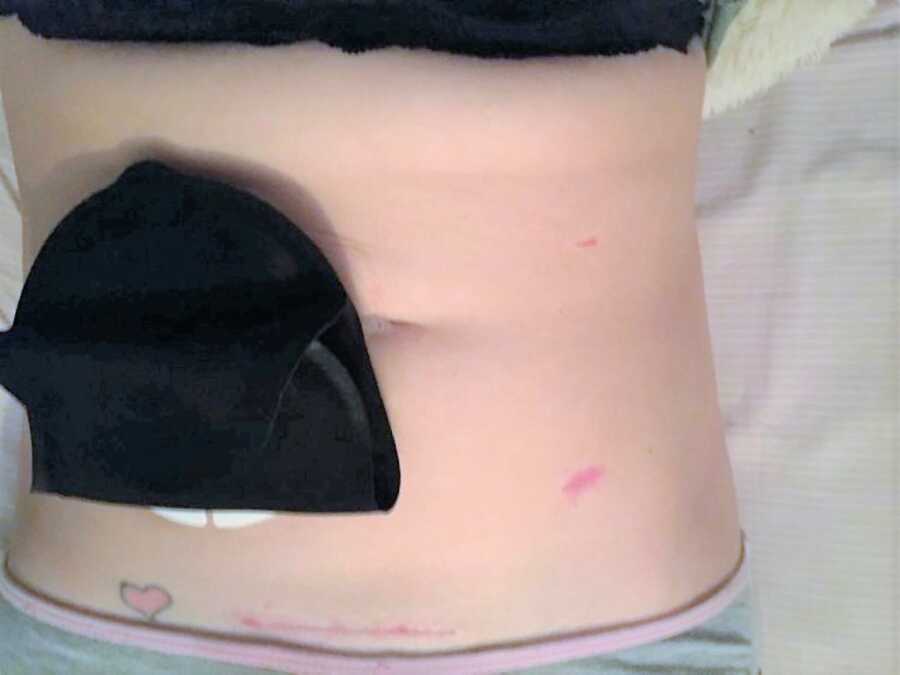
The next few weeks were rough; my bowel went to sleep and I developed an infection. I felt even worse than I had before the surgery. I went onto TPN, which meant being linked up to a feeding tube via an artery, and I wasn’t able to eat for the next 3 weeks. It was tough. I remember feeling completely out of it one day and hearing the doctors rummaging around me. One of them asked if they should get some advice from a specialist they had been in contact with downstairs, and the other replied, ‘Yes, just whatever you can get!’ I knew I was really unwell.
Towards the end of my time on TPN, I started to get SO hungry. I fantasized about fresh fruit, cucumber, and pizza in Italy! I thought about being by the beach with a cocktail, laughing, and I wondered if I would ever get there. I’ll never forget the day I walked up and down the ward for the first time–I literally couldn’t understand how people just walked around normally. I had completely forgotten how to use my limbs. But I did it, and all the staff and the beautiful people who had seen the state I had been in cheered and clapped for me. It was special.
Six weeks after going to A&E, a Saturday in June, I was living my worst fear at the time – having come home with a stoma and a bag. It took me a long time to actually feel the stoma was mine and not the property of the hospital, as I had been so out of control of my own body. I felt like an alien was attached to my stomach. I had also been dissociated and shut off emotionally in the hospital, and now was the time to let it all sink in and adjust to life. I felt terrified to tell people, but I felt I needed to for my peace of mind.
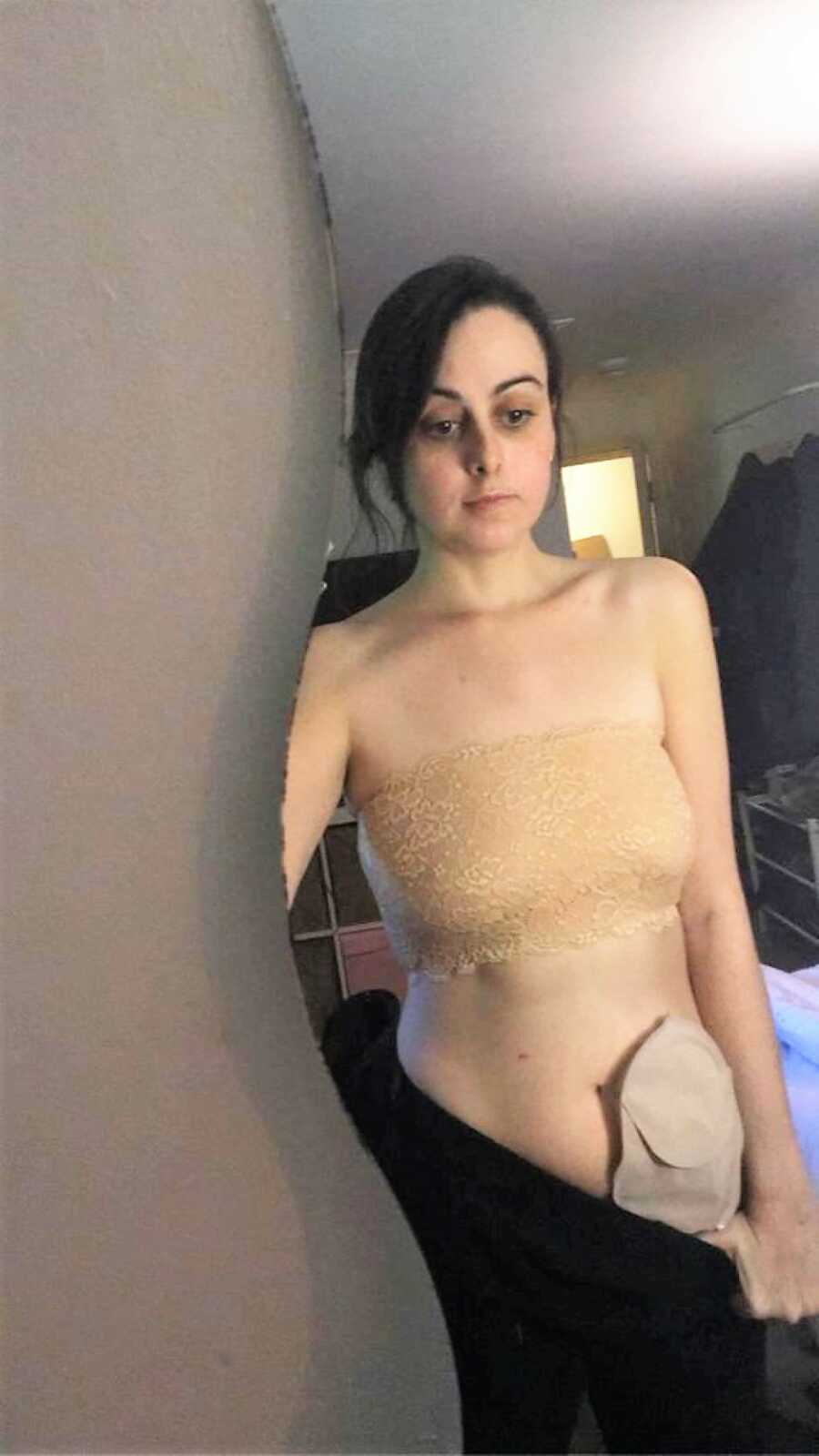
I’ve always been an incredibly social person, and the thought of being out with people and having no control over leaks and passing wind was hard for me. It still is sometimes. The support I have gotten from everyone around me has been amazing; people have asked questions, been empathetic, and talked to me about people they know who have been through the same! I even found out a neighbor who lives close to me who has a stoma too, and I had no idea! This is why I talk about it almost every day, and I will never stop talking about it – to challenge the stigma so no one has to feel embarrassment and shame.

I had days where I felt I just couldn’t do it. I have experienced obstructions in my small bowel, which have put me in the most pain I have ever experienced, and I’ve woken up a few times with my own poo all over my tummy! And yes, it gets me down, but at the same time, I just get on with it because I have my life.

When I saw one of my doctors 3 months after my surgery, he told me I was days away from my bowel perforating, and due to how weak I was, there was a good chance my situation could have been fatal. At this point, I was also told my formal diagnosis would be ‘Indeterminate Colitis’ and this was because there was so much damage to my colon, they couldn’t determine what had made me so unwell. They still suspect Ulcerative Colitis, but they cannot officially be sure.
This was scary as I knew it was possible I could be affected by Crohn’s Disease, but I had an MRI and luckily there is no sign of it at this time. I do have a retracted stoma, meaning it sits very small in a dip in my skin, and this has brought skin issues and leaks along with it, but I’m expecting another small-scale surgery very soon to refashion my stoma and make it more manageable for me.

One of the biggest worries when I realized I was going to be living with a stoma, was finding a relationship. I’ve had traumatizing relationships in the past and have been through a lot when it comes to love. Like many of us have. But now I say jokingly, ‘Well, my self-esteem issues were already a 10, so they can’t get any worse!’ But in all seriousness, I see my stoma as a filter–it will filter out people I wouldn’t want in my life in the first place, and what an amazing superpower it is to have!

In terms of my mental health, anxiety has always been a huge issue for me. It’s nothing new, but I find myself saying yes to things I would have avoided previous to my surgery. It’s not just about the anxiety now. For me, it’s given me a new sense of fight I didn’t have before, and I want to do it not only for myself but for every other person who goes through this surgery and feels they can’t do things or they’ve lost their confidence. This is why I share my journey on Instagram. Some of the amazing Ostomates I found on Social Media while in the hospital helped me get to this point. They were so important for me in terms of eradicating shame and stigma, and also building my sense of self back up again.

The most important thing I have learned in life, and more so now, is to have a positive relationship with myself and to be my own best friend. Don’t get me wrong, I’m lucky to have a few amazing friends and a loving, supportive family. But we can all be our own biggest critics, and we all have the potential to be our own biggest supporters! I practice self-care every day by being gentle with myself, giving myself a break, forgiving myself for my mistakes, and telling myself how strong I have been in this life. And if I don’t find that someone, I will always have myself.
I am now 7 months on, and I’m back at work–I’m a therapist and also a support worker for people who have been affected by sexual abuse or violence. I stuffed my face and indulged in wine and cocktails at Christmas, and I’ve even been abroad and away on trips with friends. I had the cocktail by the beach, and I ate the pizza in Italy! After just 6 months. At one point, I thought I would never be able to spend my time as I did, but now I’m doing even more than I did before.
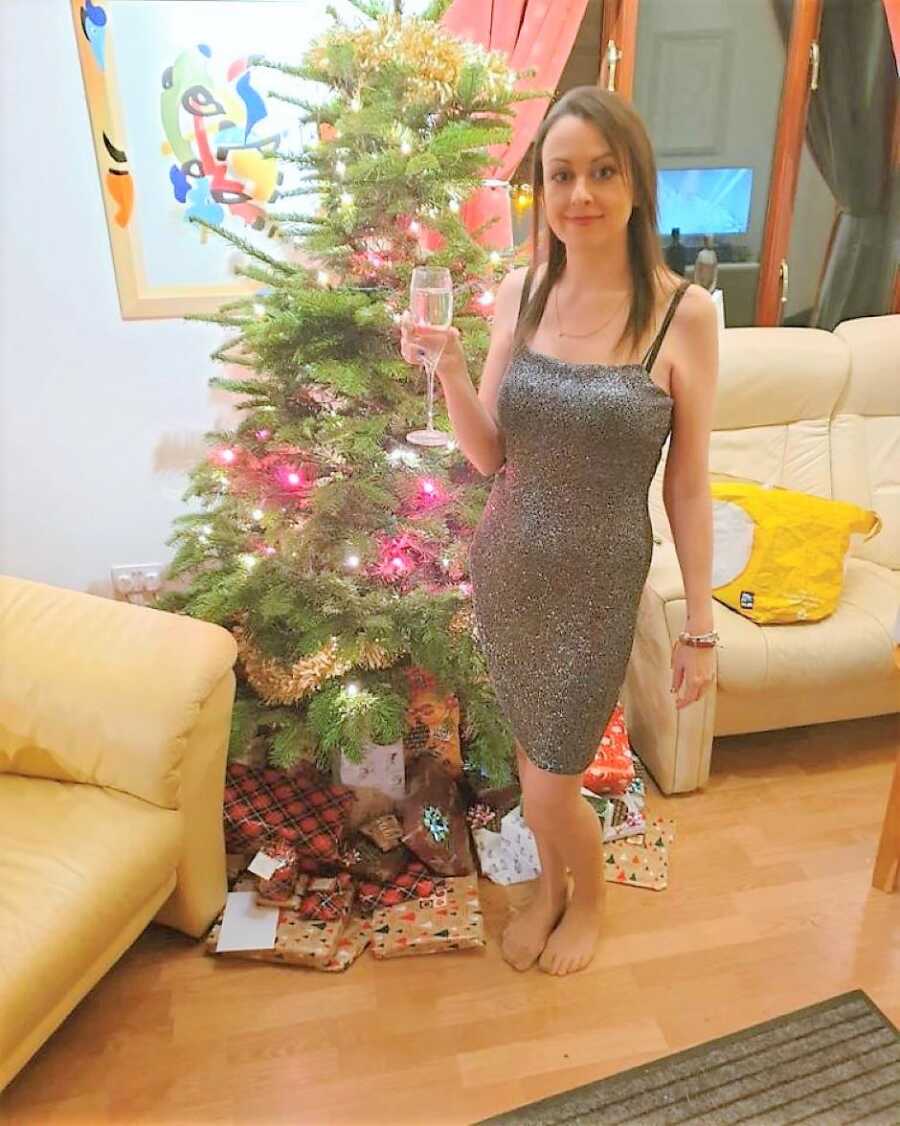

My advice for anyone who might be going through the choice of whether to have a stoma, or anyone who didn’t really have a choice, is to let yourself go through the emotional process; talk to people, have faith in others, and know you can get through it, and always give yourself time. I’ve seen so many stories about people’s lives changing for the better after having their surgery, and although I could never really relate to this, I now know I am lucky I didn’t have to go through the pain of suffering from Inflammatory Bowel Disease for years.
I did have to adapt quickly, and based on how I felt about all this in the beginning, I honestly believe if I can do it, anyone can. This experience has given my life new meaning. I can’t even explain it, but there’s something different within me now. Who knows where this journey will take me, but I’m here for it!”

This story was submitted to Love What Matters by Kathryn Evans. You can follow her journey on Instagram. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Do you know someone who could benefit from this story? SHARE this story on Facebook to let others know a community of support is available.