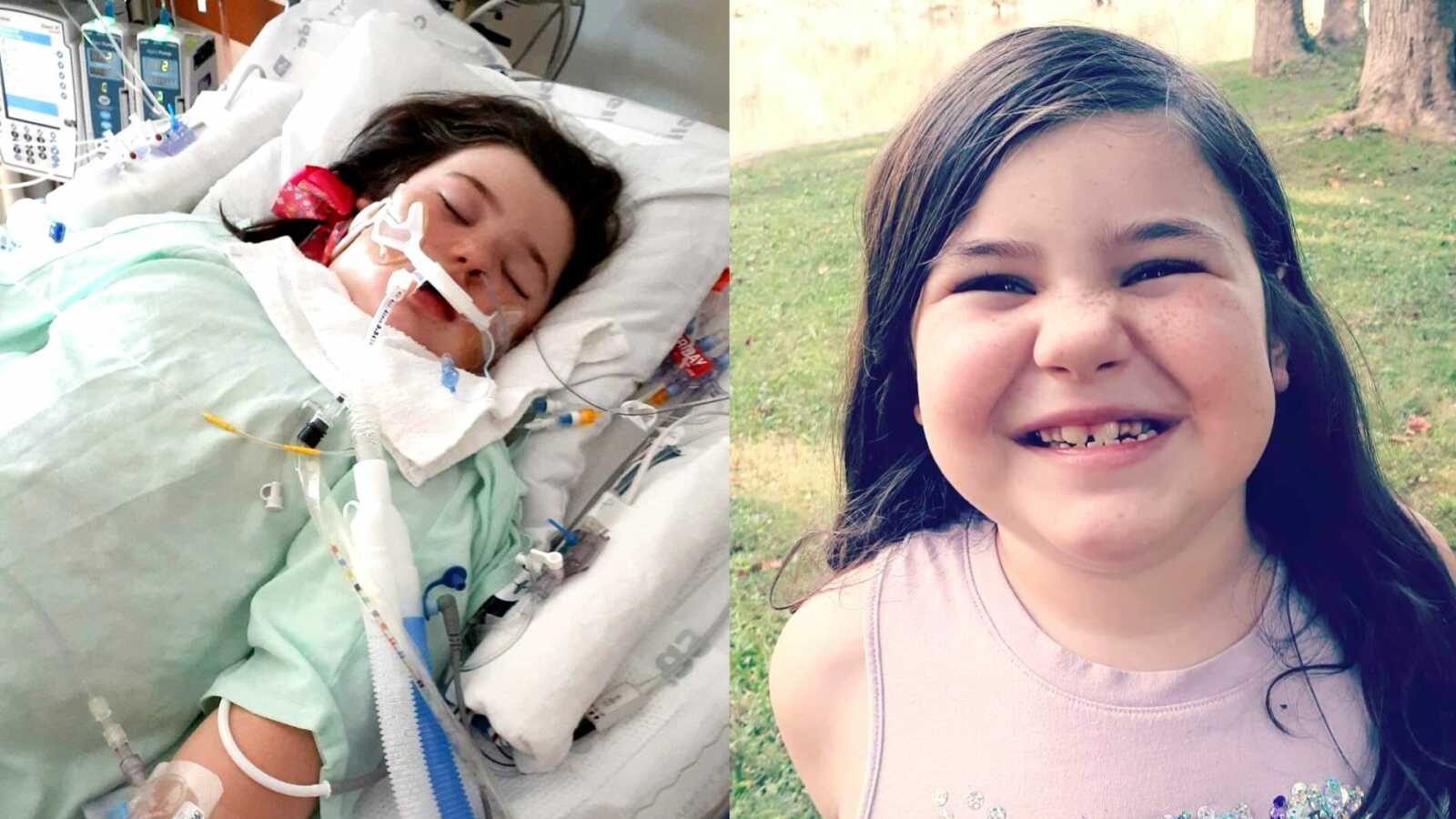
Early Signs Of Contraction
“In the summer of 2021, our daughter, Stella, became very ill and was hospitalized. It would be months later, in August, before the doctors would finally be able to give us a diagnosis for her disease when discharged from the hospital: Tularemia (Rabbit Fever).
Our daughter, Stella, had gotten pretty sick at the beginning of June. She started having severe headaches in her frontal lobe and fever ranging from 101-104.5 for a couple days. We initially tried to treat the fever with over-the-counter medications like Tylenol and Ibuprofen like the walk-in clinic suggested, but they did not help lower her fever.
In the end, Stella spent 21 days total in the hospital, or rather four different hospitals to be exact. Of those 21 days, she had to be intubated, sending her into an induced coma for 14 of those days.
First, a little background about our family. Our family is from a small town in Northeast Tennessee called Elizabethton. We are about 20 miles from the North Carolina border. We live in the foothills, as some people call it, of the Appalachian Mountains where the Appalachian trail runs through.
Our family likes to hike and just be anywhere outdoors where we can explore the beautiful world around us. Stella is our youngest of 4 children, 3 girls and a boy. She is for the most part a pretty healthy kid with no underlying issues of any sort.

Stella loves singing and dancing and loves nurturing her furry little pets at home. We have all kinds of pets, from chinchillas to cats to bearded dragons, and Stella loves them all! She loves animals.
When Stella originally got sick, the doctors at the first hospital we took her to thought she might have a UTI (urinary tract infection). She was lethargic with fever, her Oxygen was at a low 87 percent, and her heart rate was pretty high at about 145. She complained of a constant headache and just felt bad.
The hospital we were at did not treat children so they decided to have EMS transport us to the local children’s hospital about 15 miles away. We got to Niswonger Children’s Hospital very late at night. By this time we had spent about 10 hours in the ER.
The children’s hospital decided that they wanted to run more tests on Stella. They believed she did not have a UTI, but perhaps appendicitis. So, they ran the tests.
The test on her appendix came back fine. By this time, Stella had started to complain of abdominal pain too. Mind you, she was 6 years old and it was hard for her to tell us exactly what was hurting.
The Fight For Diagnosis
The nurses were giving her fluids (boluses) for low sodium and low blood pressure. The fluids did not help raise her blood pressure the way they should have and her heart rate was still very high. The doctors decided to rush her to the PICU.
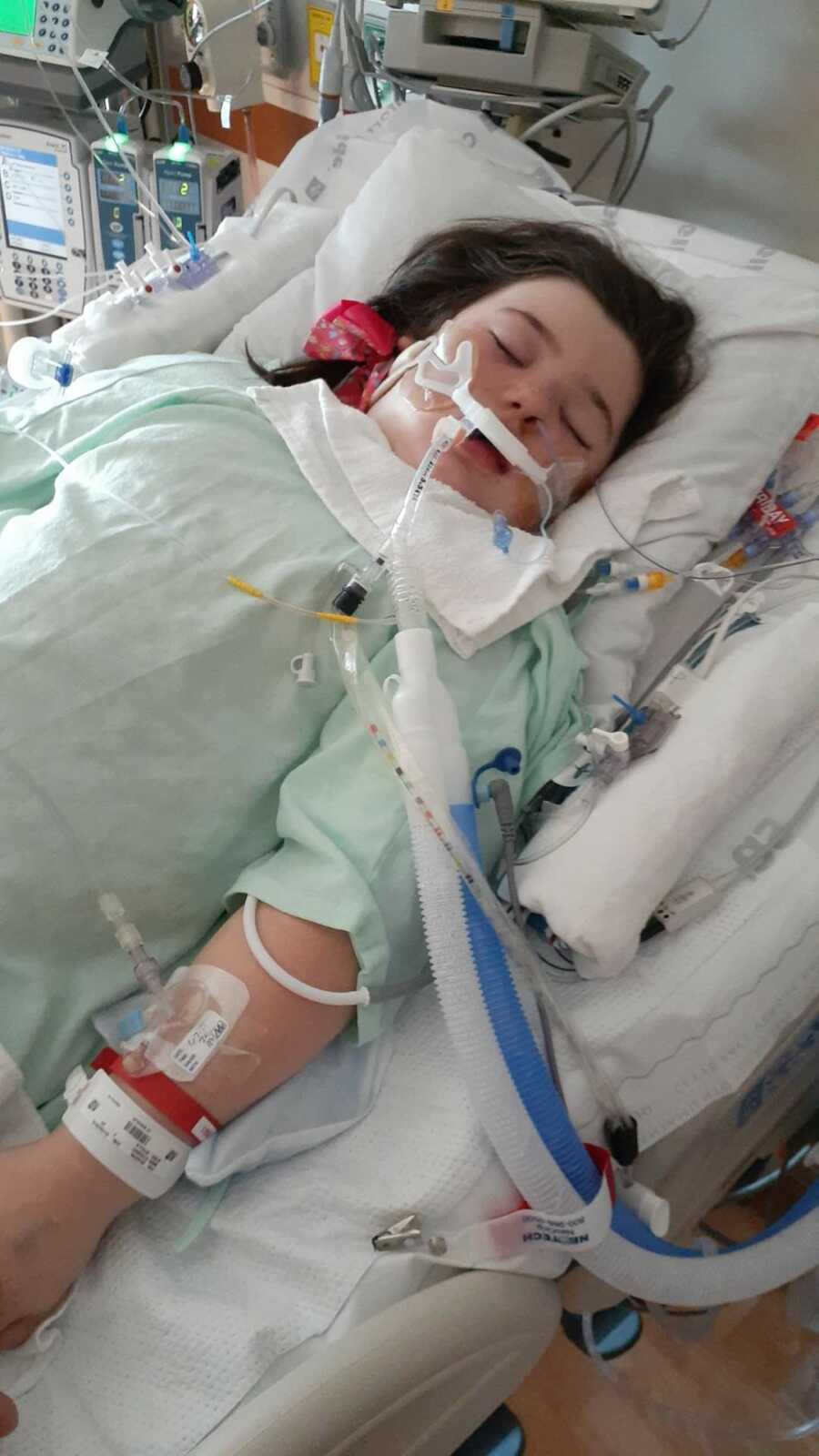
The doctors did more tests. The tests revealed that she had swollen lymph nodes in her ileum (stomach). By this time, her blood pressure was in the 80s/30s and they were still giving her fluids to try to give her little body a boost.
The fluids did not do what they were supposed to do and were instead collecting in her body and putting pressure on her organs. She did not urinate for about 8 hours. The fluid retention in her body had begun to put her organs into failure mode.
Stella was retaining 14 pounds of excess fluid throughout her body. The lead surgeon came in and decided that emergency exploratory abdominal surgery was needed in order to relieve pressure on her little organs. That meant she would have to be intubated for the procedure.
They performed the surgery and took a lymph node from her stomach in order to biopsy it. The surgery went okay. They brought her back to her room after the procedure and she was stable.
We were informed that the doctors believed the swollen lymph nodes to be cancerous. The doctors were 95% sure that it was Non-Hodgkin’s Lymphoma to be exact. The doctors came in and explained that they wanted to life flight Stella to St. Jude’s Research Hospital in Memphis where she could receive better treatment for her condition.
After her abdominal surgery was completed, they put a wound vac on her stomach. They explained that they would have to leave her stomach open, covered by a wound vac, for about a week to get all of the fluid off of her that had built up in her body from the infection.
The next morning after her surgery, Stella and her father, Derrick, flew from Johnson City, TN to Memphis, TN. I stayed at our home in East Tennessee until the very next day to make sure things were taken care of at home and our other children would have somewhere to stay while we were away at the hospital with Stella.
The next morning, I made the 8-hour drive to Memphis. When Stella arrived via life flight to St. Jude’s, she was quickly taken into the PICU where more tests were performed. They ran more blood work and cultures, followed by CTs on her brain and an echo of her heart.
At this point, we still did not have a diagnosis and the doctors were still nowhere close to finding out what her illness was. She was on 9 different IV medications while she was in the PICU. She had a picc line, a central line, and art line, and another IV line running through her body, which were all held in place by stitches in her arms.
I work at a hospital as a CNA on a medical/surgical floor, and I have never seen that much medicine run through one person at one time, much less my own daughter. It was overwhelming and it terrified me. I was scared and angry and many times I asked God why this was happening to MY daughter.
Entering Critical Condition
The nurses and doctors were giving her every antibiotic they could think of because they were still not sure which one was actually going to treat her. The next day the nurses were changing Stella’s bed pads and bandages and they had to roll Stella onto her side. When they did this, the wound vac that had been placed on her abdomen, back at the other hospital a couple days prior, had come loose from her skin and she coughed.
When Stella coughed, the force caused her intestines to push out of her stomach. The doctors had to react quickly. They could not push her intestines back into her stomach because she was still very swollen from all the fluid retention in her little body.
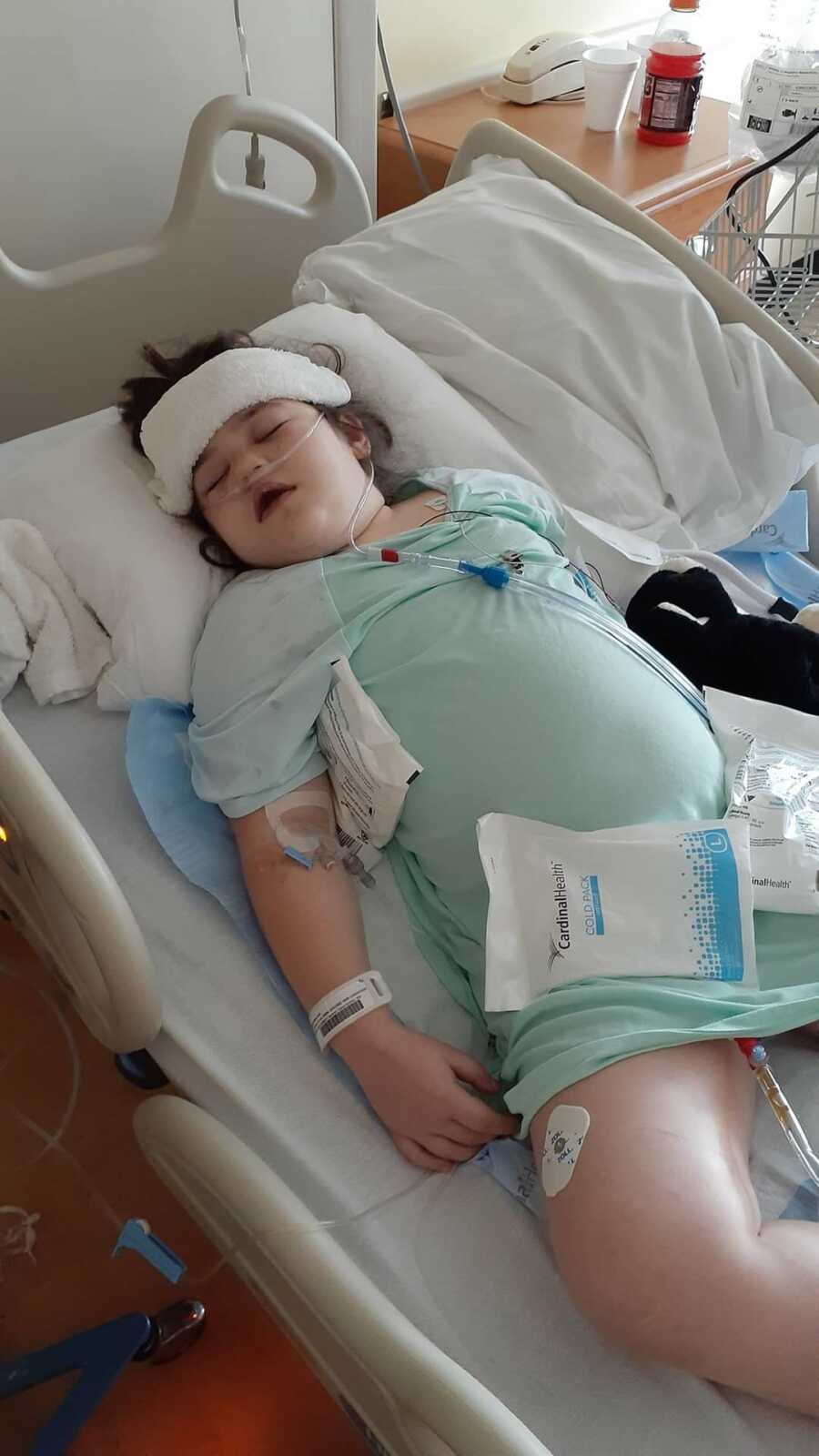
The doctors decided that they would put a silo over her intestines. It basically looked like a plastic zip-lock bag on top of her stomach that would keep her intestines moist and secure until the surgeons felt that it was safe to push her intestines back into her stomach and sew her abdomen back together.
Stella’s vitals were still stable. The leukemia doctors had come in at one point and told us that they were not sure it was in fact cancer that Stella had and so they made a list of possible diseases they thought Stella might have contracted instead. They were all zoonotic diseases like Bartonella (cat scratch fever), Taxoplasmosis (from cat litter), or Tularemia (Rabbit Fever).
How do you treat a rare bacteria that no one knows anything about? The doctors had asked us if anyone else in the family had gotten sick like Stella. They hadn’t. Everyone else was perfectly fine and the doctors thought that to be weird.
We found out through Stella’s blood work that she had antibodies for Covid-19. The best we could figure is that she had contracted Covid back in the spring and was asymptomatic (as a lot of kids are). Stella had not been sick at all this year other than the occasional runny nose.
The doctors had also asked if we had seen any ticks on her, and we said no. We did mention that sometimes she gets scratched by the cat but that there were no areas of infection we could find. The biopsies came back on the lymph node that they had extracted and we learned Stella was cancer free!
We were so relieved to hear the news. But if it wasn’t cancer, then what was this mysterious disease that was making our sweet girl so sick? None of the infectious disease doctors knew.
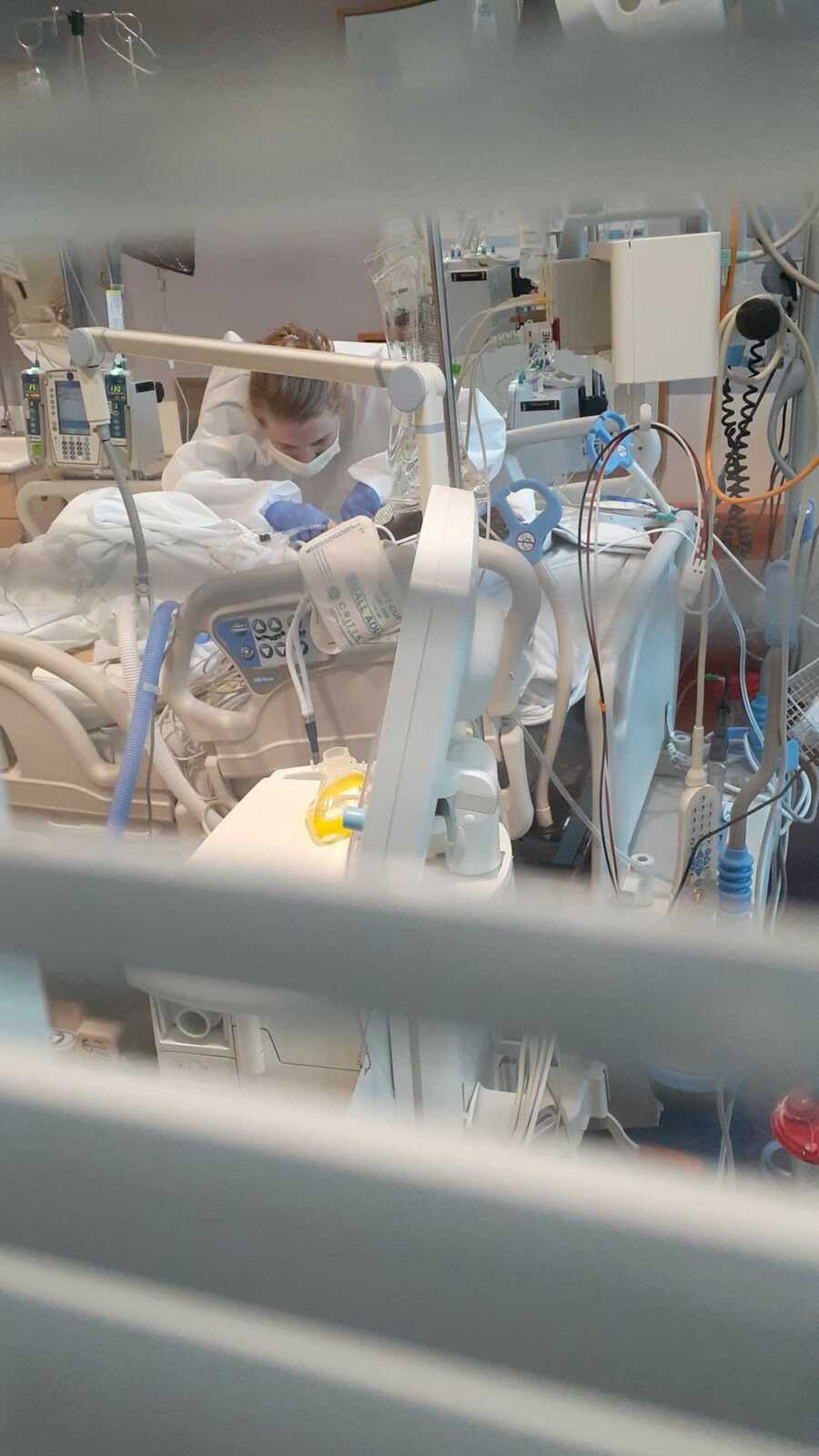
We were told that since Stella did not have cancer, we would have to transfer to the trauma 1 children’s hospital (Le Bonheur Children’s Hospital) where they treat more medical/surgical based issues. They assured us that she would be in great hands and that the surgeons over there would be the ones to close up her abdomen when the time came.
Stella was still intubated when they transferred her to our 4th and final hospital. It was also in Memphis so, thankfully, we didn’t have to travel too far.
The first day we were at Le Bonheur, the surgeons decided it was time to close up her abdomen. They did the surgery and it went well. They decided to stop the drug that paralyzed her body.
When they did that, even though she was still sedated, she panicked and started fighting against the ventilator and her vitals started to drop. The doctors came into the room and began manually using an ambu bag to give her oxygen. While they were doing that her right lung collapsed because she had fluid built up in her lungs.
Doctors began trying different ventilators and settings to see if that would bring her O2 levels back up. The new ventilators did not work. At one point her oxygen dropped to 55% and we were terrified that she was not going to pull through. The doctors were on the verge of having to call a Code Blue on her.
As a last resort effort, the doctors said they were going to have to flip her over onto her stomach. Doing this would help move the fluid that was puddled in the back of her lungs (from laying on her back for a whole week) move around more freely and hopefully get her collapsed lung to open back up. The doctors turned Stella onto her stomach and her vitals stabilized, so they left her like that for 16 hours.
Stella stayed in the PICU at Le Bonheur for about a week. The doctors were finally able to extubate her after a couple days. She did well with that. We finally moved out of the PICU and into a new room.
When she woke up, she could not speak, eat, or walk. Her mouth and tongue were swollen from all the tubes in her throat, the doctors still had a feeding tube in her nose, and she hadn’t been on her feet in almost a month.
Many things had changed for our sweet girl in a very short amount of time. She was scared and mad and overwhelmed by everything that was going on.
Family Support & Road To Recovery
Because we were so far away from home, Stella received a lot of care packages, balloons, and cards from everyone back home. We also created a Facebook page, Stella Strong, to keep everyone updated with her progress. We made bracelets that read #stellastrong for everyone to wear to show their support.

Since we were still no closer to getting a diagnosis from the infectious disease doctors or anyone else, they suggested that maybe the illness Stella had could be MIS-C. MIS-C is an inflammation that kids sometimes get as a result of catching Covid. Since Covid was a new disease, the doctors still didn’t know much about the lasting effects from it.
The doctors decided that they would begin a whole new round of medications followed by her antibiotics that she was currently on. They checked her eyes and checked her heart for traces of MIS-C.
They began giving her antivirals and steroids to boost her system in hopes that these new medications would wipe out whatever Covid she still had in her body. They gave her the MIS-C medicines for a couple days and then decided to quit them altogether because her body was not responding to the treatment.
Back to square one. Well, not really. The antibiotics were working but they still had no official diagnosis and still had no clue as to what it could be.
Infectious disease was still waiting on some of the tests to come back but so far they knew what it wasn’t. It wasn’t MIS-C or Cat Scratch Fever or Cancer or Parvo or Rocky Mountain Spotted Fever. The list goes on.
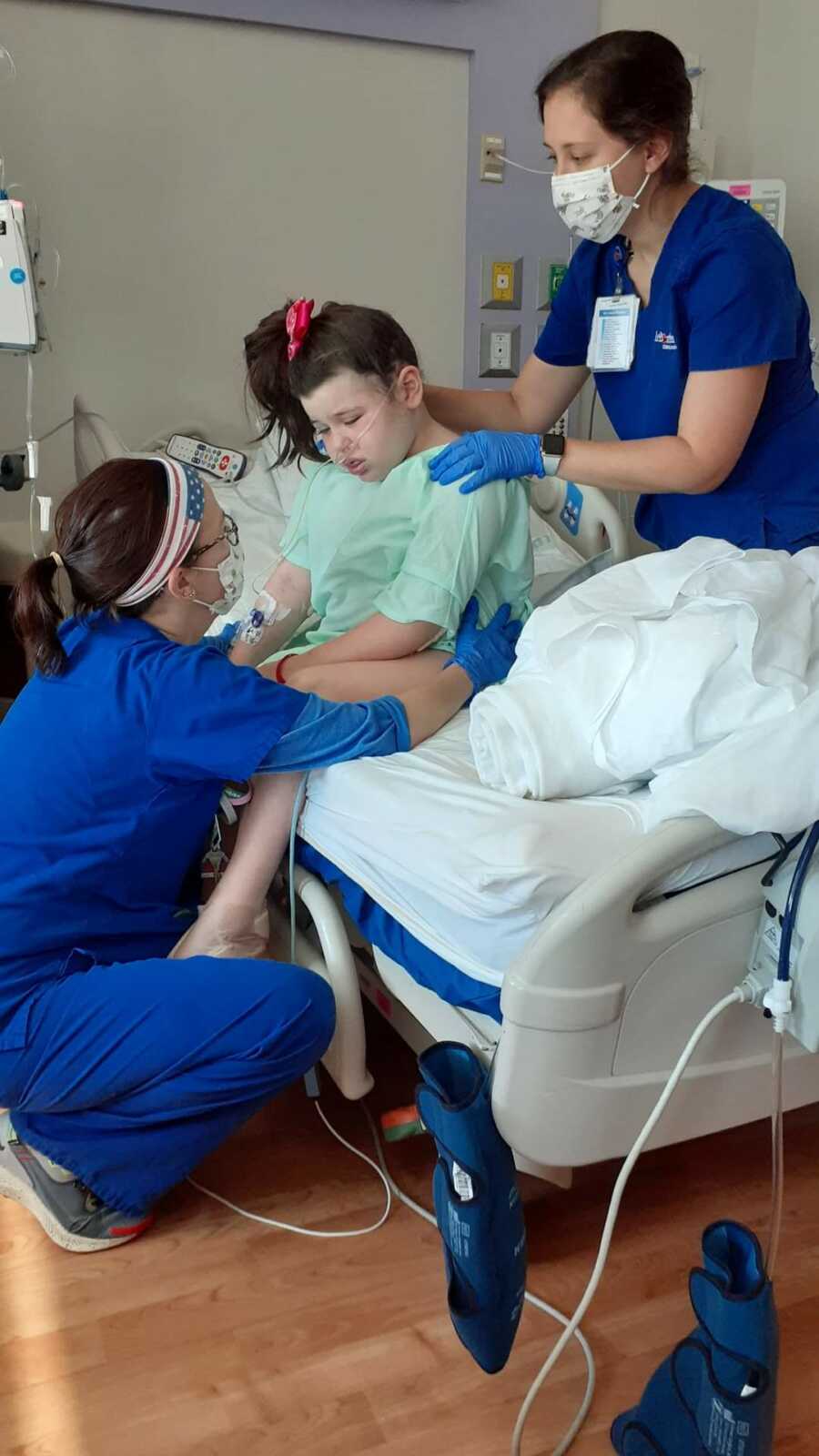
Physical therapy and OT came and worked with Stella everyday and eventually got her back on her feet after about a week of exercise. She got her NG tube (feeding tube) removed and began eating normal food again after all the swelling in her mouth went down. While we were in the hospital, Stella lost about 20 pounds.
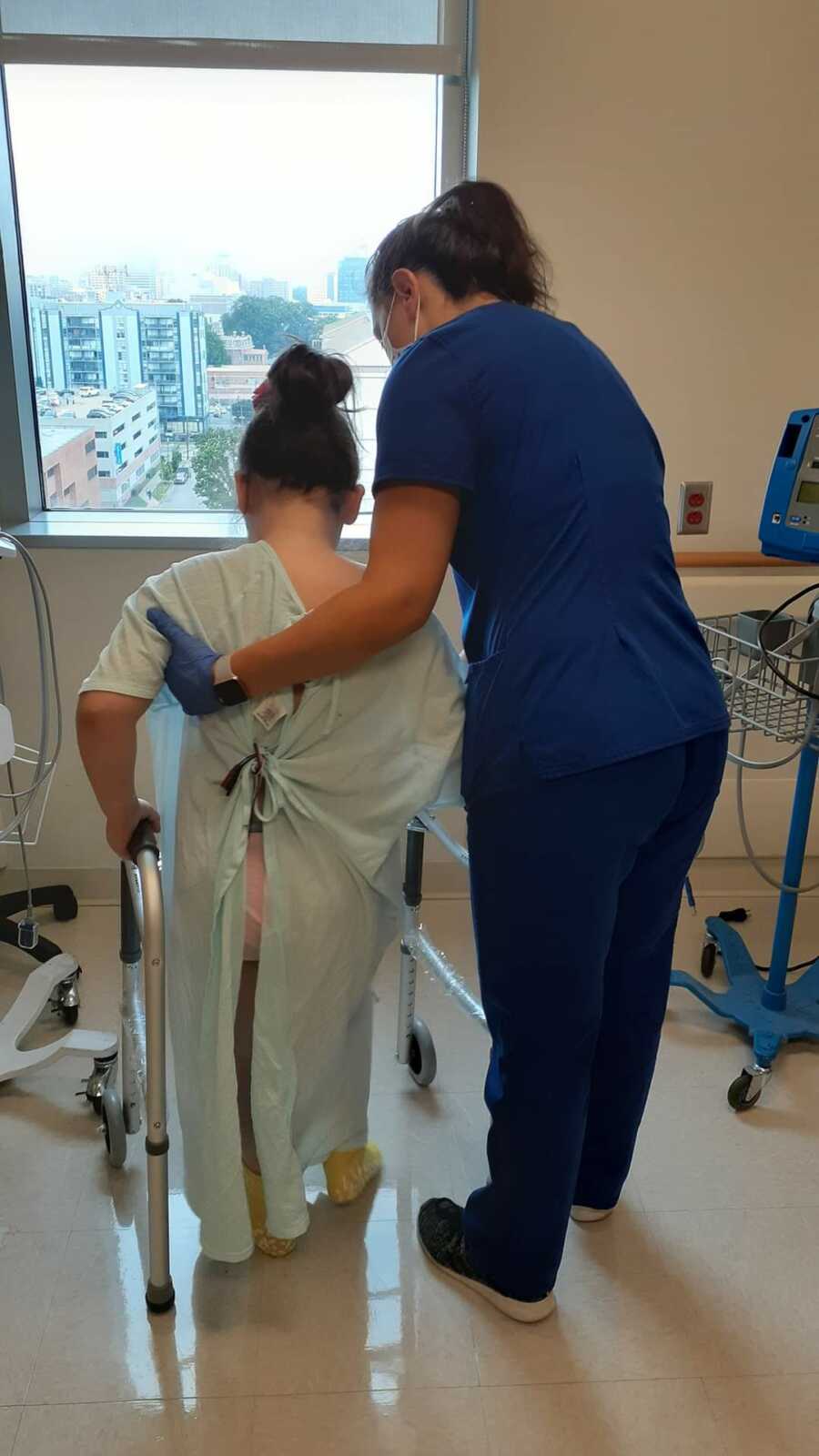
Stella soon finished the rounds of antibiotics that she had been taking and finally got to a point where she could be discharged after spending 21 days in the hospital. She was stronger and happier and healthier than she had been in a long time.
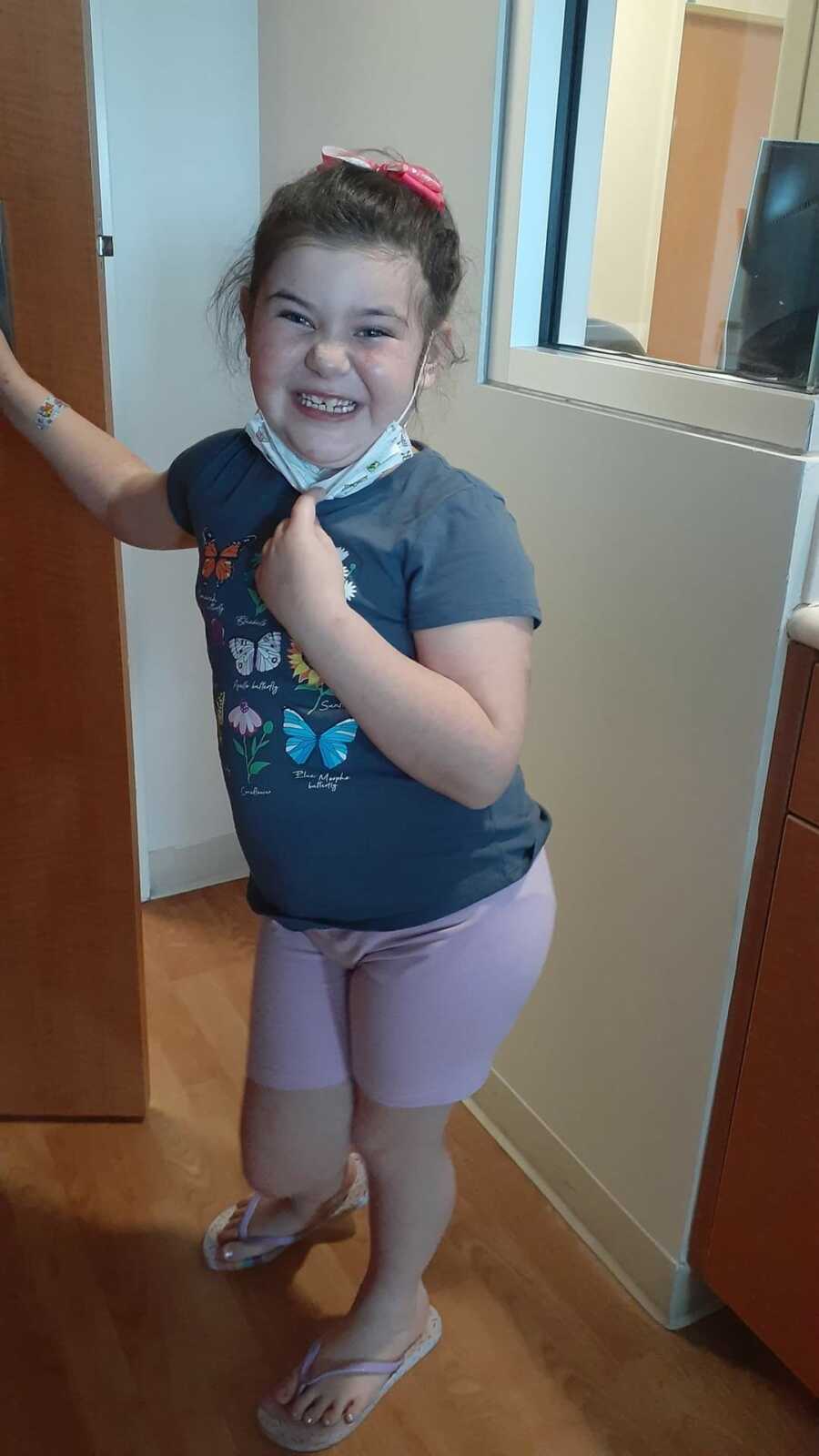
Even when we were discharged from the hospital we still did not have a diagnosis as to what made Stella so sick and sent her fighting for her life. The doctors told us that we may never know what the disease was but at least she was healing and getting better and stronger.
I think her father and I accepted that we would never find out what had caused all her issues. We wondered if it might have been from the Covid. Our main concern was for Stella, but also the fear that if we didn’t know what had caused all these issues, then we didn’t know how to prevent them from happening again to her in the future or anyone else in the family.
Official Tularemia Diagnosis
We finally made it back home to East Tennessee at the end of June. When we arrived, our kids and all of our family members were standing with a giant sign in our front yard that read, ‘Welcome Home Stella.’ Stella was still on some of her meds but she was thriving and so happy to finally be home.
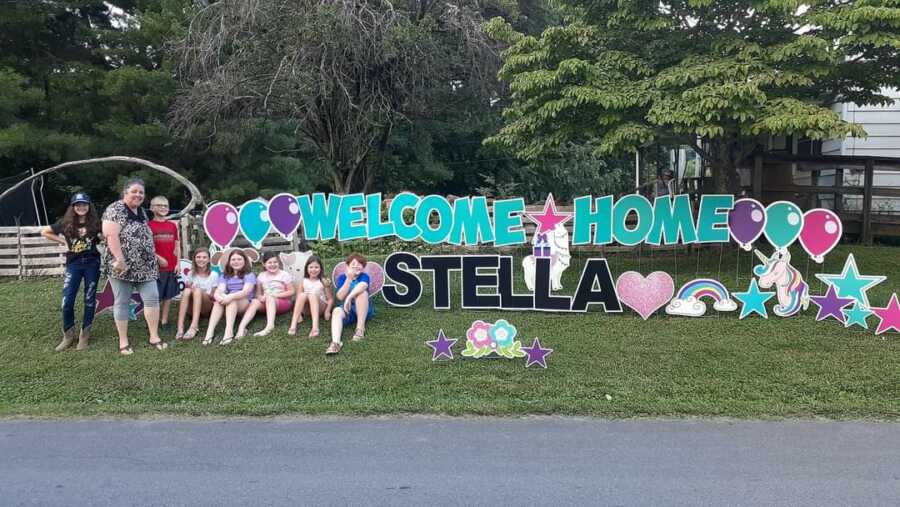
Fast forward to August. Things were going really well with Stella and the family. We were finally starting to find a sense of normality again. As far as we knew, there had been no lasting effects from her illness. She was almost back to 100%, except for the giant scar she has down the middle of her stomach.
One night in August, Stella got sick and just started projectile vomiting all over the living room. We decided not to take any chances and her father and I took her back to the children’s hospital just to be safe. She ended up only having a UTI that time and the doctor sent her home that night with some antibiotics.
While we were there, however, the doctors had read her chart and they knew that she had had a rough couple of months. One doctor came in and said, ‘Hi, Stella. I know you. You’re famous here! No one could figure out what was wrong with you!’
The doctor continued, ‘But we figured it out!’ I replied, ‘Oh, really? That’s funny because no one had told us what it was.’ The doctor then said, ‘It was Tularemia, or rabbit fever!’
The funny thing is, we don’t even have rabbits, but we researched and learned all about Tularemia and how it can be transmitted from contaminated soil, or water, or rodents, or even ticks. How sometimes cats can carry it or that it only takes a tiny, tiny amount (10 organisms) to make someone deathly ill.
In Stella’s situation, the doctors said that the way she had contracted Tularemia was by ingesting something through her mouth; that’s why all of her issues took place in her stomach. We don’t know where she contracted it from but whatever it was had gotten on Stella’s hands and into her mouth either through contaminated water or maybe an animal she had picked up on one of our outings.
In the United States alone, there are less than 200 people annually that contract ‘Rabbit Fever’ and because it is so rare it is super hard to diagnose. The only reason they even found out that Stella did in fact have Tularemia is because her test results came back as testing positive for Tularemia antibodies. Those results didn’t come back until after we had been discharged from the hospital.
Stella’s Tularemia was so severe that she ended up in septic shock. With ‘Rabbit Fever’ animals can give it to other animals, and that is how complete colonies of animals (rabbits and rats) have been wiped out in the past. Humans, however, generally can’t give it to other humans. That is why no one else in our family had gotten sick with it.
Today Stella is 8 years old and doing pretty good! She does have some pulmonary issues the doctors think might be lasting effects from Tularemia. She also experiences some asthma and increased heart rate sometimes, but we are keeping our eye on it.
Other than that, she still loves to sing and dance and play with her friends. She still loves her critters and likes to play doctor sometimes. She talks about her trip to Memphis and about all the doctors and nurses that took such good care of her.
It wouldn’t surprise me if one day she grows up and becomes a nurse herself.

What You Need To Know
What I want others to gain from this story is that diseases like Tularemia and other tick-borne diseases can happen to anyone. You hear about Lyme disease a lot of times but never any of the other tick-borne diseases out there. I didn’t even know there was such a thing as ‘Rabbit Fever’ before it happened to my family.
Because there is such a lack of information, a lot of times, super rare tick-borne diseases like ‘Rabbit Fever’ are misdiagnosed. There is not a lot of research or information about such a thing. If it hadn’t been for the hundreds of doctors and nurses that worked with Stella in all 4 of those hospitals, she probably would not be here today.
As of now, scientists and doctors are still working on creating a cure for Tularemia. I would like to see more research dedicated to this cause. The mortality rate right now for severe cases of Tularemia is about 60%. That is way too high.
The best way to protect yourself from Tularemia and other tick-borne diseases is by washing your hands after being outside or touching animals, checking for ticks, and using insect repellent.
As for the lasting effects of Tularemia, we are taking things one day at a time with Stella. While we are dealing with lingering pulmonary issues, but we are just glad that Stella is home and she is happy and she is, for the most part, healthy and doing all the things that she loves to do.
We are letting her live her best life with her friends and her family. We still let her hike and go out into nature, but we are just more cautious with our surroundings and the things that we touch.”


This story was submitted to Love What Matters by Jeannie Montalbo. Be sure to subscribe to our free email newsletter for our best stories.
Read more about tick borne illness:
Do you know someone who could benefit from reading this? SHARE this story on Facebook with family and friends.