Symptoms Out of the Blue
“In March 2021, I had developed a cough out of nowhere that would not go away. I tested for COVID, but it kept testing negative, so I thought it must be some kind of bug, which would go away in time, I had no reason to think it would be anything more sinister than that.
In April, things started to get worse—my neck became really swollen, and it hurt so much. I thought maybe I had slept funny and started looking at chiropractors, but it became so swollen on one side it was quite obvious something more serious was wrong. My lymph nodes had started swelling in my shoulder and chest, making my collar bone disappear into the swelling on one side. At this point, I contacted my general practitioner (GP) to work out what was wrong with me.
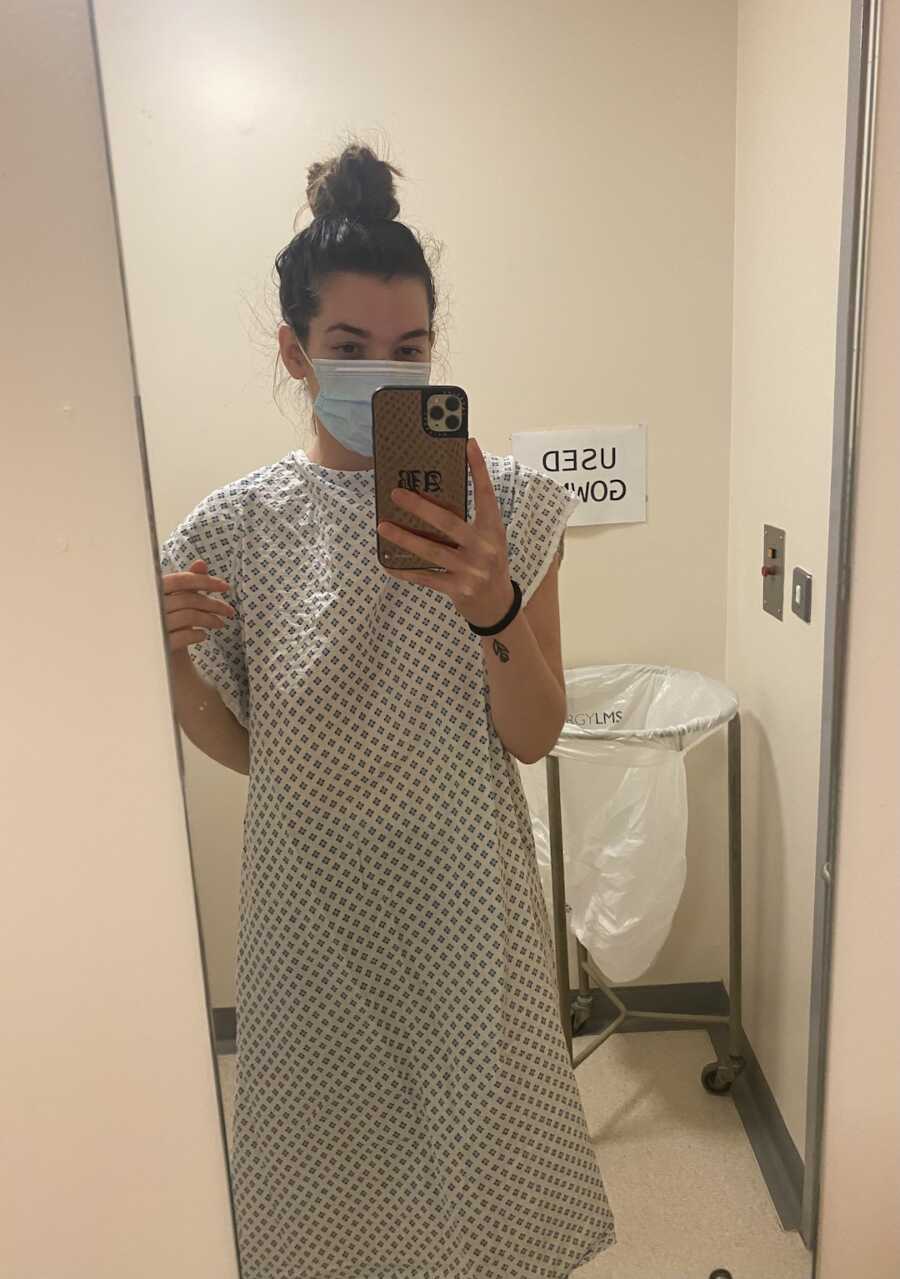
I had a blood test, and we ruled out glandular fever. It was thought I had a bad chest infection so I started antibiotics. At the end of April, I moved houses, but the cough was still there and the antibiotics hadn’t improved my health. I called my new GP, who asked me to have a chest X-ray, and I was given yet more antibiotics. I kept calling the doctors when I felt unwell, but they only suggested cough syrup to help, and wouldn’t see me in the GP because of COVID.
During May, things started to decline quickly, I was struggling to breathe and couldn’t talk without running out of air. I was coughing up phlegm constantly and couldn’t leave the house without a cup to cough up into. I had intense night sweats and was really struggling. I had lost so much weight that none of my clothes fit me anymore, and I would often cough so much that I would be sick. I called the doctors again, and they asked me to come in to be examined. Once I was seen, I was sent straight to A+E at my local hospital.
At the hospital, I was put into a separate room while I went through all kinds of tests. Initially, they thought maybe I had TB, but I came back negative. It was suggested I should have a CT scan, but I was sent home instead as I’d been there all day. After a few visits to the hospital, I did finally have a CT scan, and that’s where everything changed for me. I remember when they first injected me with blood-thinning medication, it was all too much and I nearly passed out. As soon as I’d had the CT scan, doctors started talking to me in a different manner, and it was then it was suggested this was something more ‘sinister.’
The Diagnosis
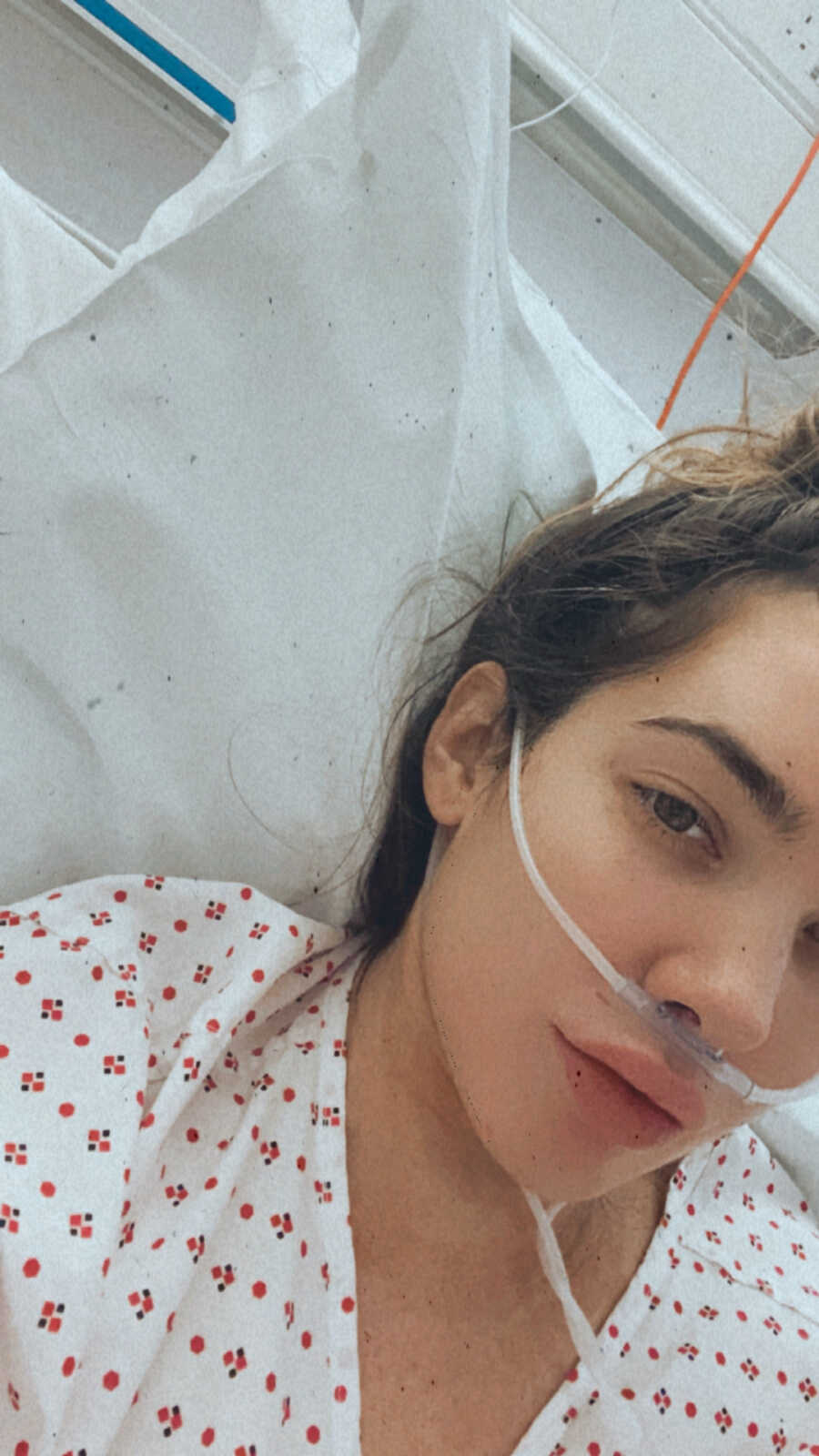
I spent a week living in the cancer ward, where I had a biopsy and a PET scan and was on several IV bags of antibiotics as I was suffering from pneumonia. It was during this time I was told I had cancer. They weren’t sure of the primary location of my cancer and were suggesting it was likely lymphoma initially. I couldn’t believe what was happening to me—I wasn’t expecting any of this at all. I thought I had a chest infection, and I would get better. I was always really healthy; I’ve never smoked, rarely drink, exercise, and eat plant-based.
There was nothing in my lifestyle that would make me think cancer was even a possibility. I spent the whole time I was in the hospital on my own, I wasn’t allowed a single visitor because of COVID. I went through some of the hardest, most upsetting days of my life without a single familiar face, and I found it really hard. I would Facetime my boyfriend most of the day so I had someone to talk to while I was alone in my hospital room. I’d sleep a lot because I struggled to stay awake for too long, and I miserably ate the hospital food.
The biopsy was sent off to be examined, but they did confirm it was adenocarcinoma—a physical cancer, not lymphoma as first thought. I didn’t really understand what this meant, and it took another doctor to explain to me I had incurable cancer. I was heartbroken at the news. I remember telling a friend and saying to her I’m likely to die of this disease one day.
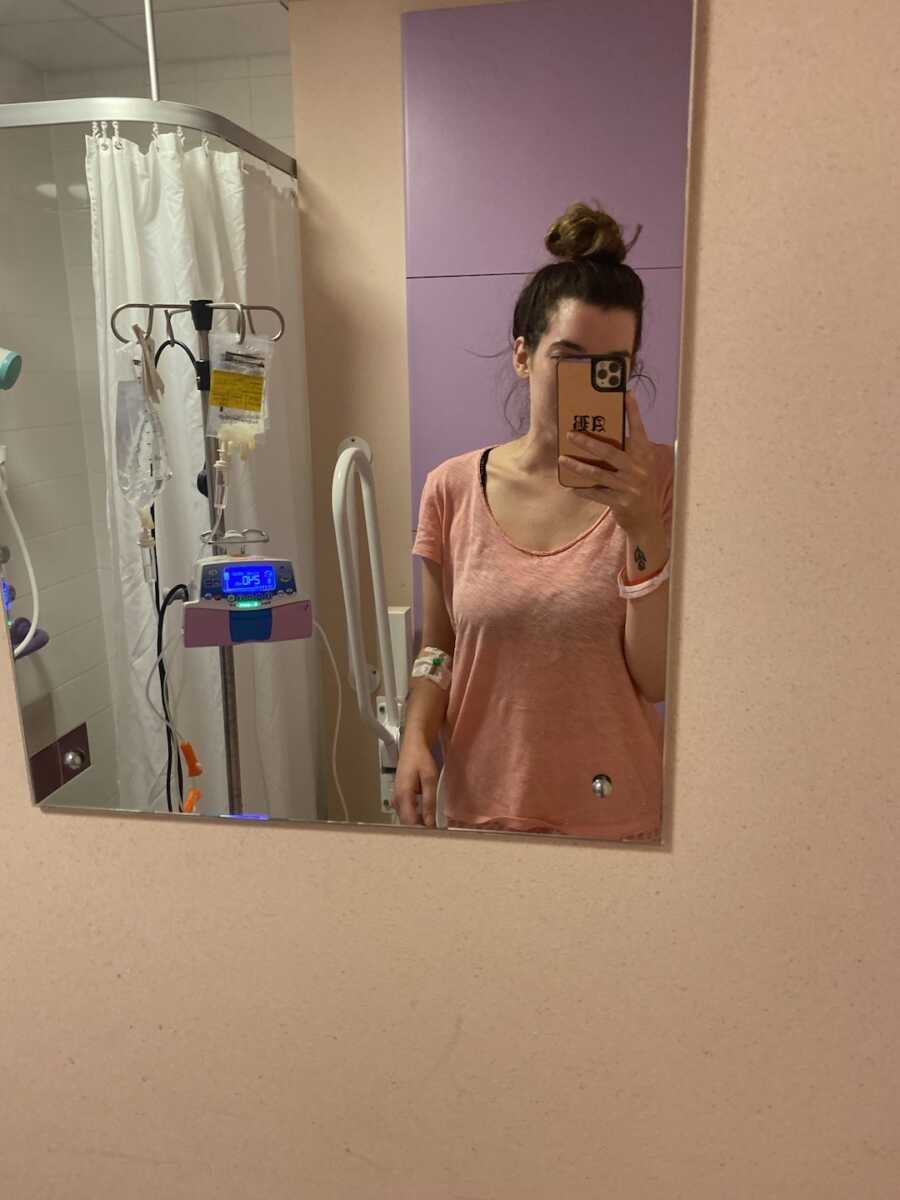
I was sent home for two weeks while we waited for the biopsy results to be sent back. In those two weeks, things got really, really bad—I was sleeping all the time, and I was so weak I couldn’t really stand. My boyfriend had to carry me up and down the stairs because it was too difficult for me to do. I had to move my bedroom down a floor so it was easier day-to-day. I would be coughing all day and all night so I was only sleeping in short bursts.
It was really miserable, my GP would call me to check in on me, and I would be too breathless to have a conversation. When I went to meet my oncologist, it was obvious how bad a state I was in, and I was admitted straight back into the same ward as before so I could attempt to get better—my oncologist explained the cancer in my lungs was stopping the pneumonia from being treated properly, so we would have to treat both for me to improve.
During my time in hospital, my oncologist confirmed my diagnosis to me, ALK-positive lung cancer—which had spread to my liver, lymph nodes, shoulder, spine, and pelvis. I was due to start Alectinib, which is a targeted therapy taken orally as soon as possible. The same week I had to spend a weekend in ICU because I needed a ventilator due to my condition—there was a potential I would need an induced coma if I didn’t improve, but thankfully I did. I started taking Alectinib, came off of oxygen, and was discharged to go home.

Redefining Myself
My diagnosis came as such a shock, stage four lung cancer at 28. I was too unwell to process it at first, it took a while for me to recover from the pneumonia and for the oral chemotherapy to start to work. Eventually, over time, I learned to understand I am, and will be, living with incurable cancer. I would be too unwell to look after my dog, I couldn’t walk myself, let alone a strong bulldog. I would have to take time away from my job. I cut my hair in case I lost it due to treatment. I was still underweight. I looked different, I felt different—I felt like I had lost my whole identity to this diagnosis.
Everything I used to enjoy and define myself by had changed—my job, my hobbies, my home, my pets. I had to learn how to pace myself when I started using the stairs again, I was given physio instructions and felt like I was basically starting from scratch in terms of who I was and how I identified. My diagnosis was really life-changing—I thought I had my life sussed out, what I would do in my career, my home, my life. I wasn’t expecting a cancer diagnosis, where I can’t even plan more than a few weeks in advance.

My cancer is more common in non-smokers, so screening for it isn’t great. ALK-positive lung cancer is a relatively rare form of lung cancer, caused by the abnormal rearrangement of the anaplastic lymphoma kinase gene. The vast majority of patients are non-smokers, half are under fifty years of age when diagnosed – some are much younger, and the majority of patients are female. Most patients are stage four at diagnosis.
Since being diagnosed, I have tried my best to live the best life I can. I make sure I rest and listen to my body, but also try to go for walks and exercise when possible to help my body while on treatment. I’m now on my third treatment line, Alectinib drastically stopped working after five months, I became extremely breathless again and had a noticeable deterioration of my lungs.
I changed to Lorlatinib, which worked for slightly longer, but after seven months and a biopsy, I moved to Crizotinib because my cancer was growing again. With ALK-positive lung cancers, some people can have years on their first and second line, so it is heartbreaking I have flown through my treatment lines in the way I have. There are very limited targeted therapies available, and if they don’t work, IV chemotherapy treatment is not known to be as successful typically.

Living with such a life-threatening disease at a young age has been a real challenge at times. I’ve had to come to terms with my own mortality, and really consider what matters most in life. If I die soon, what do I want to do with the time I have now? I’ve learned in this situation, as another lung cancer patient put it, it’s not how long you live, it’s how well you live, and it’s so important to make the most of the life you have—even if it’s limited. I just want to spend time with those I love most, I want to travel, I want to be in nature, and I want to be as well as I can be.
I think it’s clear anyone with lungs can get lung cancer, and if you have a persistent cough, please don’t ignore it. Speak with your GP and get it checked, it could save your life.”

This story was submitted to Love What Matters by Alix Burnard of Newbury, UK. You can follow her journey on Instagram. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Do you know someone who could benefit from this story? SHARE this story on Facebook to let others know a community of support is available.

