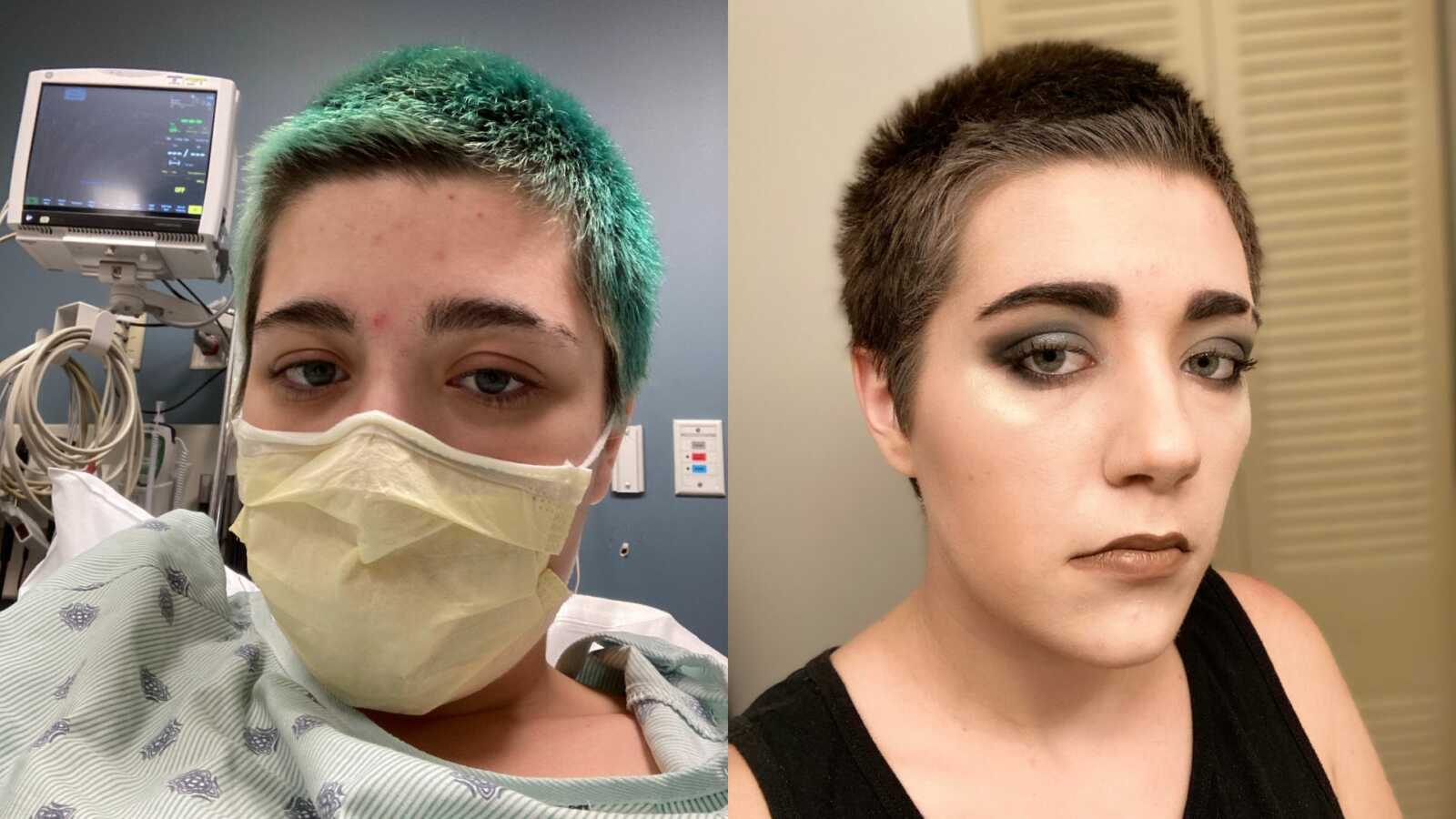
History Of Chronic Illness
“Chronic illness has ruled my life from the time I was a young child. I spent the formative years of my life bouncing between specialists to figure out why my body wouldn’t work right. Between these regular appointments were trips to the ER and prolonged hospital stays. I’ve tried many medications, lost the ability to take part in my hobbies, and had to change the type of food I eat.
Until this year, I was forcing myself to push through even when I felt my worst. After all, I grew up with the idea you have to work hard no matter how bad you feel. Eventually, all this pushing led to my body forcing me to slow down. Now I am taking time to connect with others going through this and raising awareness on social media.
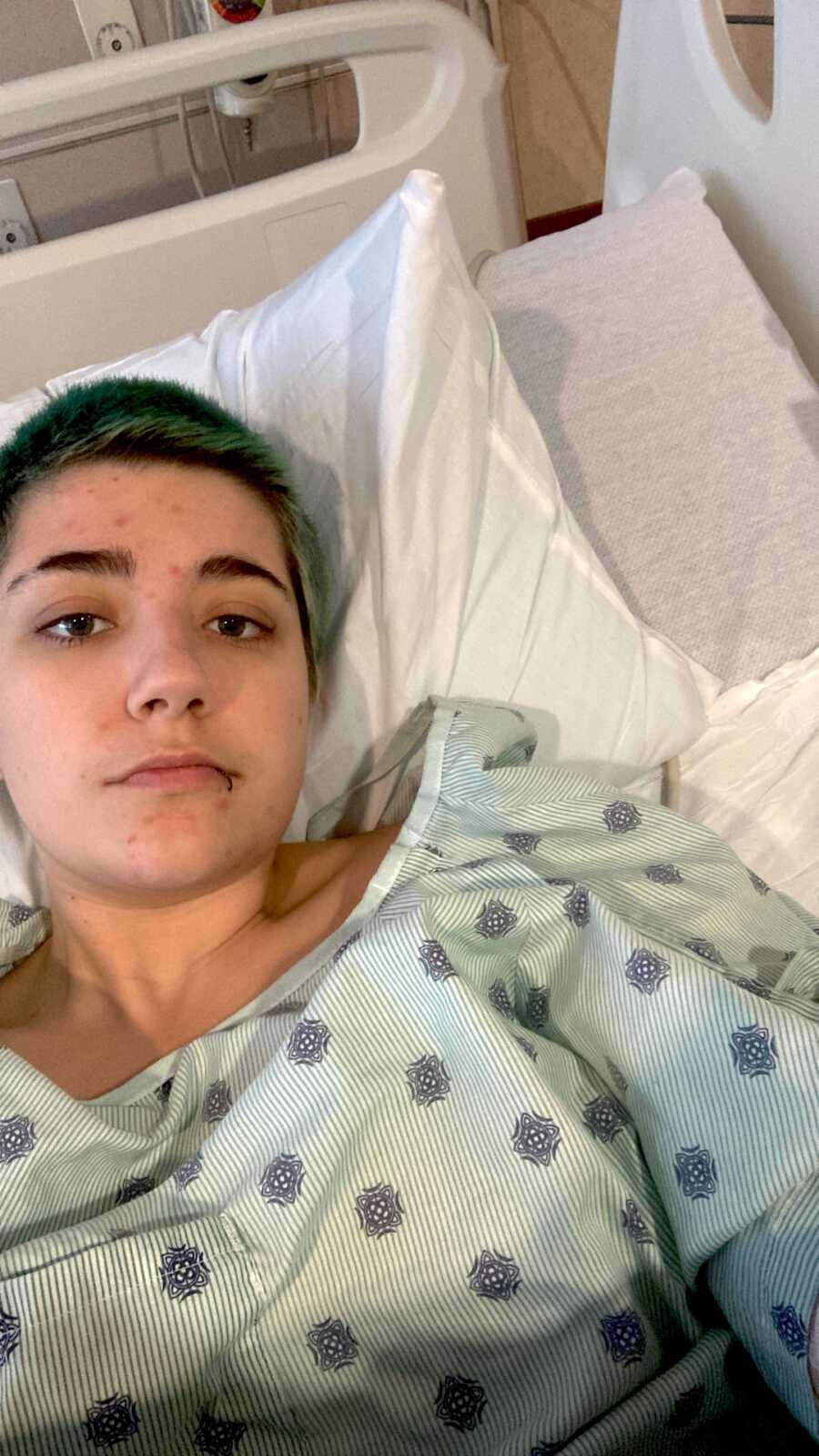
I started my journey at the age of 8, when I got my first migraine. It happened when I was at school. By the end of the day, while I was getting my backpack from my locker, I had tears running down my face because of the pain. At the time, I had no idea what was going on and why light made my head feel like it was going to explode.
At this point, I didn’t go to a doctor because my parents assumed it was a one time thing from a virus. But over the next few months I would come home from school at least twice a week with the same symptoms. At my next annual check up my mother mentioned these headaches to my doctor. She expressed surprise I was having migraines at such a young age, and gave me a referral to a neurologist.
The first neurologist I saw was rude and dismissive. He said, ‘It’s impossible for a child to have migraines. You must be lying to get out of school.’ This was only one of many times I had my health concerns dismissed by a doctor due to age. Luckily, my primary care doctor was persistent and referred me to another neurologist. The second appointment went better. I got sent for multiple scans to ensure nothing more serious was going on. I walked away with a diagnosis of chronic migraine, and a prescription for amitriptyline.
The next stage of my journey began when I was 14 and I woke up with severe vertigo. At this point, I was very active. I took dance classes for 3 hours a day, went for daily walks with my mother, and enjoyed weight training. Before the onset of vertigo, I had been having incidents where I would stand up and black out.

The doctor first thought it was dehydration or standing up too fast. The next assumption from doctors was that it was a new migraine symptom. So they prescribed meclizine to stop the vertigo. This treatment was unsuccessful. I was still blacking out upon standing and having months of vertigo where I couldn’t get out of bed. This made school impossible, but I managed not to fall behind by doing my work at home.
Diagnosis Journey
The first time any doctor considered a diagnosis besides migraines was when I had severe chest pain during ballet class. I went to the hospital immediately after class, and my pulse was 195 when I got there. I left the hospital with a cardiology referral for a Holter monitor and an echocardiogram.
Going to a cardiologist at 14 was a strange experience. Everyone in the waiting room was over 60, and the person at the check-in desk asked me if I was lost. No, I wasn’t lost. I was unlucky. Even more unlucky than I realized. During the Holter monitor I discovered I was allergic to adhesive. After the results came back, the cardiologist said I had sinus tachycardia which would go away once I got older. Another concern dismissed because of my age.

It wasn’t until last year I found a doctor determined to get to the bottom of things. It took 10 years for me to find a doctor who listened when I said something with my heart wasn’t right. When I said my symptoms match Postural Orthostatic Tachycardia Syndrome (POTS) he looked into it. I ended up with an event monitor that I wore for a month. Even though the heart monitor showed no rhythm abnormalities, he was still concerned. He listened when I said I was still having symptoms. I am now working on finding a medication that works for me.
Being listened to made my willingness to go to the doctor much higher. Before I dreaded it. Now, if I have a concern I am comfortable making an appointment. Yet my faith in the medical system is still low. The hospitals in my area miss important things in blood tests. They rush people out without listening. They don’t tell you everything they find. They send you home to die.

Colitis Journey
In April 2022, I ended up catching COVID. The initial symptoms lasted a week. Other than a high fever, it was manageable. Two weeks later, my entire digestive system shut down. The pain was like nothing I had ever experienced before. I couldn’t stop vomiting. I went to the ER, but they refused a CT scan to avoid exposing me to radiation. I received naproxen and nausea medication. I ended up back at the ER that night when I couldn’t move from the pain.
I was finally given a CT scan where it showed severe acute colitis. The doctor prescribed antibiotics. The antibiotics made me even sicker, and I ended up back at the ER two days later. This time I got another CT, and discovered it had progressed into segmental colitis. My white cell count was over 20,000. I finally got admitted, as the on call gastroenterologist had concerns.
I was inpatient for one day. Their main priority was stabilization and getting me to be able to eat solid food again. Upon discharge, I read the notes from my stay and found out they admitted me for sepsis. This was only the start of my colitis journey.
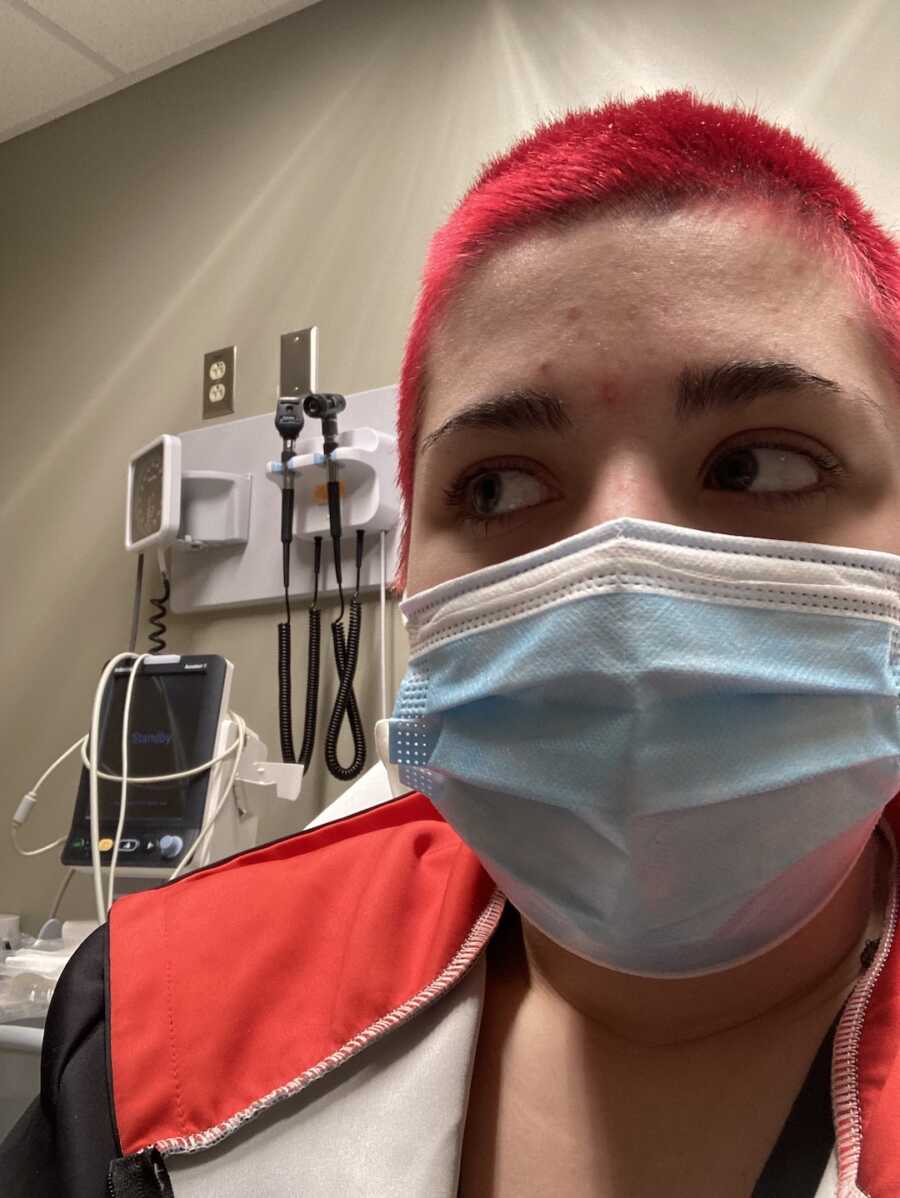
In June, the stomach pain returned once again. It followed the same pattern until I was unable to move. I went back to the ER. This time they immediately ordered a CT scan, and I was expecting to discover I had acute colitis again. I did in fact have colitis, but this time it was stercoral colitis.
Stercoral colitis is a rare form of colitis most often found in individuals over the age of 60. It has a 62% mortality rate. To say I panicked is an understatement. In the span of minutes I found out I could be dying. I received an aggressive regimen of MiraLAX and had to follow a liquid diet for 2 weeks. Luckily, I survived to tell my story.
During this time, my partner and I decided to get married so he would be able to be my medical proxy. He has been my biggest supporter through everything the past two years. He helped me with my most basic needs when I was unable to do anything, and held my hand through the pain.

We got married this July in a simple courthouse ceremony. I wouldn’t have been able to get through everything without him. There were many days where I was ready to give up, but he helped me get through the worst. He’s supported all my diet changes I’ve had to make to stay healthy. He’s held me while I cry about how unfair life has been. I wouldn’t be able to do this without him.
Lifestyle Changes
The diet changes have been one of the hardest parts of everything. I have to eat gluten free, lactose free, and low FODMAP. The majority of my diet before this involved gluten to some degree, so that has been the hardest to adjust to. It is also the most expensive. To stick with this diet change I have had to start cooking more often and finding new recipes.


As an Italian, pasta is one of my favorite foods. Adjusting to gluten free pasta has been challenging to say the least. I had to try so many new pasta brands to find one that had a good texture. After a lot of experimentation I found some I enjoy, but then came the challenge of low FODMAP sauce. In the end I realized making my own sauce was likely to be the best option as I could control the spices I use.
Even still, I miss the foods I used to eat. I’ve slipped up a lot and regretted it after. I needed to find a way to stay on track, so I turned to Instagram.


I created my Instagram to post about my journey with colitis to try to build a supportive community. I also wanted to post the recipes I tried, and rate them. Chronic illnesses can feel isolating, as often you can’t leave your house for days on end. A virtual friend circle is helpful when you feel like you need to talk to people that understand. Even if you have supportive friends or family, they don’t always get what you’re dealing with.
Alongside my Instagram I also write a personal blog. I share more details of my journey with chronic illness and share tips on managing low energy and pain. In the future I plan to write about products I use to make my life easier. Especially on days where the pain is too intense to do much of anything. I didn’t know where to start, and I know others may not either. I want to become a place for people to go to feel less alone in their own journey. I know those first months after diagnosis, and even years later, can be isolating.

If you’re entering your own chronic illness journey, please know you aren’t alone. There are so many people you can reach out to for support. Even if you feel hopeless, there is hope. Don’t give up on finding a medical professional who will listen to you and advocate for you with insurance. If you don’t know where to start, look to a chronic illness creator on your favorite social media platform. They may have posted advice you can follow or adapt to your own needs.
If you can’t find a community to join, create your own. It can be as easy as going on Instagram and saying, ‘I’m here, I’m chronically ill, and this is my life.’ If I hadn’t done that this year, I would never have found so many people I can relate to. People I can share health memes with or turn to for advice. I hope someday my account will be a place people turn to for that same sense of community I’ve found.”

This story was submitted to Love What Matters by Andy Morgenstern of Indiana, US. You can follow their journey on Instagram and their blog. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Provide beauty and strength for others. SHARE this story on Facebook with friends and family.