“My name is Chelsea Mathieson, and I am 34 years old. Less than two years ago, my life was turned upside down when I suddenly went from being a vibrant, outgoing, athletic young woman to being unable to leave my bed with my life slipping away before my eyes. Now I am living with complex chronic illnesses, including lupus, scleroderma, Lyme, and borrelia. I am a chronic infection and autoimmune disease warrior, and this is my story.
Early Symptoms
My symptoms of chronic illness first began on September 1, 2020. It started with a mild abdominal ache, nausea, and loss of appetite. I had just started an elimination diet (cutting out grains, dairy, sugar, alcohol, and caffeine) to address some other health issues I was having, and I had been warned by my naturopath at the time to expect to feel lousy for the first week. I was also experiencing some other stressors in my life at the time, and I was all too familiar with the ‘butterflies’ associated with an anxious stomach. So, when my insides started feeling a little upset, I thought it must be related to a bit of anxiety combined with my change in diet.

A week went by, however, and I was still not feeling better. If anything, I was feeling worse. I decided to speak with a doctor just to be safe. He ordered some bloodwork, but when everything came back normal, he speculated I probably just had a stomach virus, and I should feel better in a week or so. Another week passed, but I just kept feeling worse. The pain in my abdomen was beginning to interfere with my sleep, and I was feeling so nauseated I was no longer eating full meals. I saw a doctor the following week and he ordered more bloodwork. Again the test results were normal, and his nonchalant reiteration was ‘It’s probably just a virus, you will feel better in a week or so.’
Feeling dismissed and disheartened, I conceded he must be right, and I just needed to wait it out. I considered going to the hospital for a second opinion, but at that time the world was only six months into the Covid-19 pandemic, and the overwhelming message was ‘If you are sick, stay home!’ I certainly didn’t want to risk getting Covid, or even worse, spreading whatever my ‘virus’ was to anyone else.
Worsening Health
‘Are you okay?’ I opened my eyes and saw my partner staring at me in bed. He had been checking in with me multiple times per day, and he was growing more and more concerned. It has now been over a month since the onset of my symptoms. I was constantly nauseated, eating nothing more than a couple of water crackers and a sip of Ensure meal replacement each day. I was losing weight rapidly, and the deep ache in my abdomen had become so severe I was unable to sleep at all.

‘I think we should go to the hospital,’ he said. ‘Okay,’ I sighed. He had been urging me to go to the hospital for a while, but up until that point, I had been resisting. I was afraid I would get told (yet again) condescendingly it was ‘just a virus.’ But enough was enough, and I couldn’t go on like this. He helped me get into the car, and we went to the emergency room.
The following weeks and months were a bit of a blur. As my pain and nausea worsened and my weight dropped, I was in and out of emergency rooms, urgent care clinics, and doctor’s offices. I had countless blood tests, heart tests, CT scans, ultrasounds, and scopes. But every time, my test results were unremarkable, and the message from the doctors was the same. ‘Everything looks normal.’ ‘It’s probably just a virus.’ ‘You’ll feel better in a week.’ Nobody seemed to believe me.
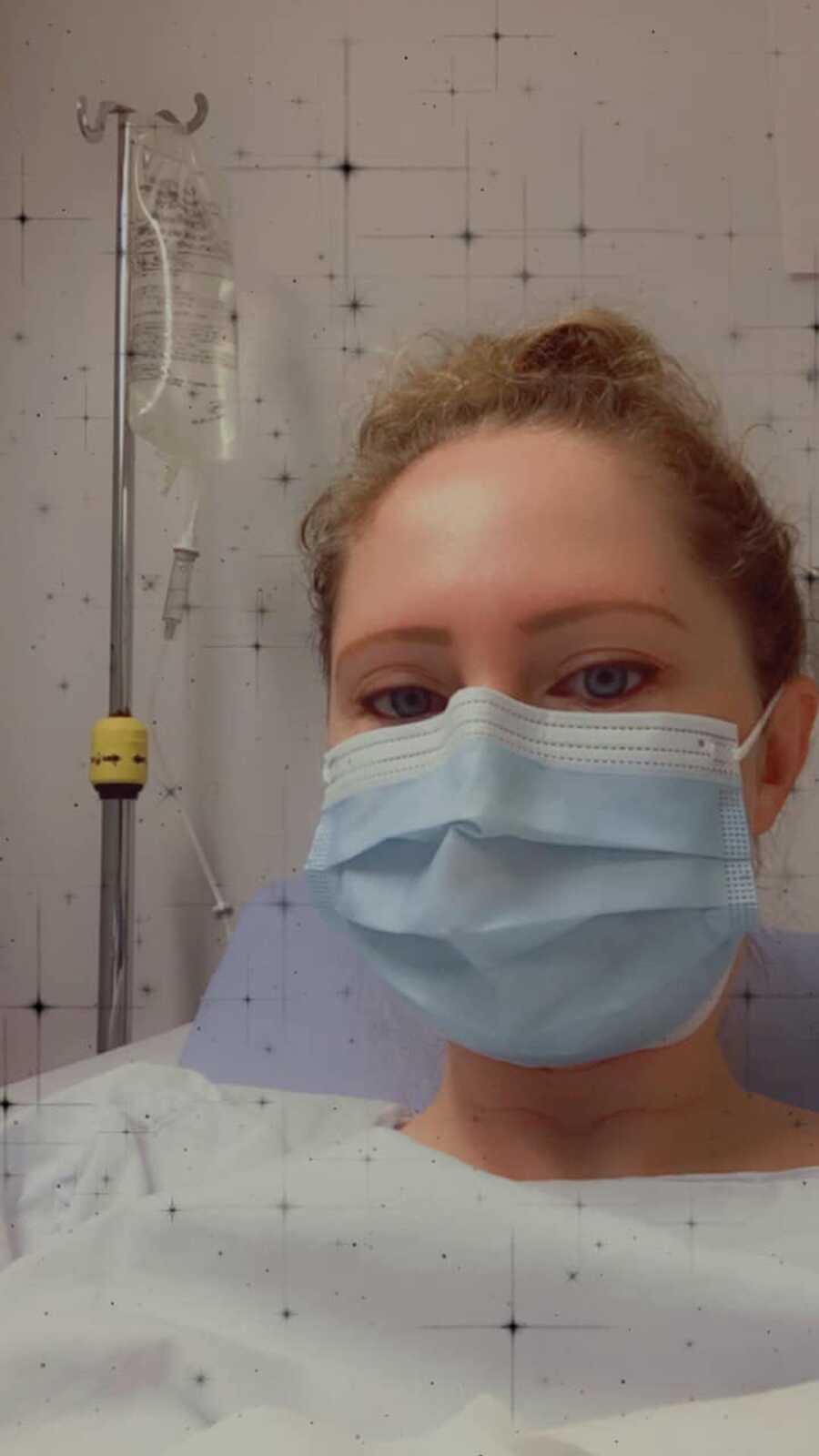
I felt like I was dying, yet I kept getting turned away. How could nothing show up in my tests? Was there really nothing wrong with me? I was feeling so lost and disregarded, and I was exhausted from the pain. I started to pray for any positive test result—even if it was life-threatening—just so I could feel validated something was actually wrong. I remember going into my endoscopic surgery thinking, ‘Come on, please be an ulcer! Please be celiac disease! Please find something. Anything!’ But they didn’t, and I was sent back home.
More time passed, and I declined even further. It had now been months since I had slept or eaten a meal, and I was so sick and in such excruciating pain I could barely walk more than a few steps. I’d lost over 40lbs (30% of my body weight), and I was losing sight of reality. Every morning for me became about just making it through the day, and every evening was about surviving the night until morning. Every minute of every day became about survival. Finally, in the middle of November, I had a turning point. For what felt like the hundredth time, my partner, who was getting more and more concerned, took me back to the urgent care center.

Turning Points
I exhaustedly repeated my now well-rehearsed story of symptoms and events. The nurse practitioner listened patiently, then asked, ‘What do you want from this visit? Clearly, we haven’t been able to figure out what’s wrong, but I want to help.’ I fought back my tears and answered, ‘I just want to be able to sleep. I just can’t take this pain anymore.’ She wrote me a prescription for Tramacet and sent me back home. It wasn’t a cure or a diagnosis, but I finally felt like someone believed my suffering and was willing to help me.
Given their well-known addictive properties, I was terrified to take the opioids. I got the prescription filled, but spent two more sleepless nights in pain, too scared to take them. When I finally did take one, it did not take away the pain by any stretch, but it took the edge off just enough for me to get a few hours of sleep. It was the first time I had slept in months. That was the one and only time I took Tramacet, but that night of sleep gave me just enough clarity to keep going, keep looking for answers, and keep advocating for myself.
A few days later, I had an even bigger turning point. My partner’s parents had explained my situation to their family doctor, and he had agreed to take me on as a patient. I was cautiously optimistic at the prospect of having a family doctor, since finding a family doctor in British Columbia is incredibly difficult, but given the past couple of months, I was also skeptical as to whether or not he would treat me any differently than all the other doctors I had seen. However, my concerns were unfounded. Once I had completed my intake form, I received a phone call almost instantly saying he wanted to see me immediately.

The very next day I was in his clinic, where he spent more than an hour thoroughly examining me and listening to every detail of my experience. He ordered extensive blood tests, another CT scan, and scheduled a follow-up appointment with me for the following week. He had a curious mind and a calm and caring demeanor, and he treated my situation like a puzzle to be solved as opposed to a squeaky wheel looking for grease. At the end of the appointment, he looked into my eyes and promised. ‘We are going to figure this out. I have some ideas, and if it’s not what I think it is, we will look for other possibilities. I’m here for you, my friend.’ For the first time in months, I felt like instead of dismissing me, a doctor believed me, cared about me, and wanted to help. For the first time in months, I felt a flicker of hope.
Positive Results
The following week, my test results came back, and I finally had a positive result! My ANA (antinuclear antibodies—a nonspecific autoimmune disease marker) was absolutely off the charts. Speaking with my doctor about my results, I had a whirlwind of emotions. I felt a deep sense of relief, almost excitement, to finally have a positive test result, and to finally have a direction to look for treatment. But I was also terrified about what this would mean for my life moving forward. I didn’t know anything about autoimmune diseases, but a quick google search showed they aren’t good.
My doctor immediately prescribed a heavy tapered regimen of prednisone (a corticosteroid used to suppress the immune system) and referred me to a rheumatologist, who prescribed hydroxychloroquine (an antimalarial drug also used to treat many autoimmune diseases). By February 2021, I was given a symptom-based working diagnosis of SLE (lupus) with limited scleroderma.

The medications did not kick in right away, but over time my symptoms gradually improved. The organ damage caused by autoimmune diseases is irreversible, and I feel incredibly fortunate to have caught it relatively early before too much damage was done. Today, while my symptoms are not nearly as extreme as they were initially, they have never gone away. They still prevent me from doing so many of the activities I used to thrive on like hiking, backpacking, traveling, and playing hockey, and I am still seeking new hobbies to fill the void.
Life with Chronic Illness
Throughout my health journey, I have always tried to keep a positive mindset, focus on the things within my control, and maintain a good sense of humor. Even still, my chronic illness took a huge toll on my mental health. I have always had mild to moderate anxiety, but as my physical health declined in 2020, my anxiety became extreme, and I sank into depression. When my symptoms first began in 2020, I had just started a dream job working abroad on National Geographic Lindblad eco-cruise ships as a naturalist in climate change. The onset of my symptoms and subsequent diagnoses had meant giving up my job.

In the days and weeks following my diagnosis, negative thoughts took over my mind, and I started to spiral. I felt like I was losing my life, and I couldn’t help but wonder if I would ever be able to work, travel, study, or do any of the things I loved ever again. On top of that, I was also dealing with trypanophobia—an intense fear of needles—meaning every time I had to get tests involving needles, I experienced severe anxiety and panic attacks. I realized I needed to pull myself out of this hole. I signed up for an online CBT skills workshop and attended weekly counseling appointments. Over time, I have learned techniques for managing my anxiety and depression, and while I still experience bouts of anxiety, I am no longer depressed, my anxiety is under control, and am now able to do my monthly blood tests completely free from anxiety (as long as I’m lying down!).
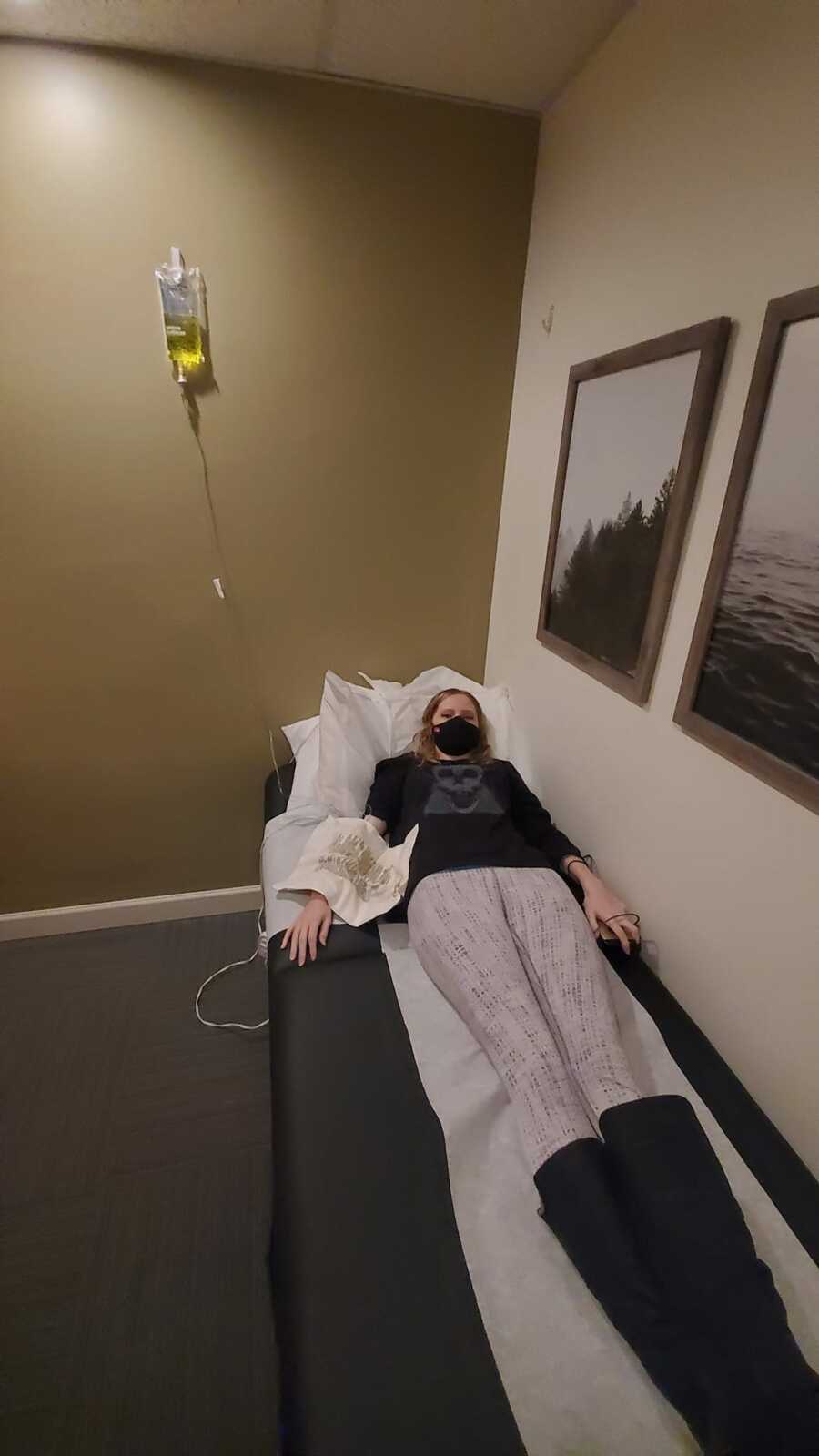
I had also always dreamed of getting my master’s degree, so I started writing applications to universities and scholarships from my bed. In 2021, I received a full government scholarship and began graduate studies in September at Simon Fraser University (SFU).
As a master’s student, research and studying occupy most of my daily time and energy. When I’m not up at SFU or working from home cuddled up on the couch with my two orange kittens, you can find me going for walks along the English Bay Sea Wall, visiting the Vancouver Aquarium, and occasionally bringing out my DSLR taking nature photographs. On a good day, I may tackle a small hike and have even been able to go skating a couple of times. No two days are quite the same: some days I have almost no symptoms, and some days my symptoms are so severe I can barely get out of bed (known as an autoimmune ‘flare’).

I regularly experience fatigue, nausea, abdominal pain, joint pain and stiffness, brain fog, hair loss, and mouth and nose ulcers. I am relearning my own energy budget (I often overdo it) and am still figuring out how to find balance in my life. I get monthly blood tests to monitor the progression of my diseases and have medical appointments throughout the month to consult with specialists or check in with my family doctor.
Lessons About Chronic Illness
I am still at a point of discovery in my journey. Even though I continue to test highly positive for ANA, I test negative for all other blood markers that indicate specific autoimmune diseases, meaning my diagnoses of lupus and scleroderma are based largely on my symptoms. I also recently tested ‘weakly positive’ for chronic Lyme and borrelia (vector-borne infections) and have responded somewhat positively to experimental antibiotic treatments. My entire medical team considers me a medical anomaly, which can feel overwhelming at times, but I am trying to embrace this opportunity to learn more about my own body.
I am figuring out how to manage my symptoms, and how to live and thrive with chronic illness. I have been blessed with an incredibly supportive partner, family, and solid group of friends, and I have had tremendous support from my professors, colleagues, and classmates at the university. From the beginning, I have tried to be very open and honest with others about my experience and journey with chronic illness. My hope is others who are out there suffering will hear my story and know they are not alone. So far, every time I tell people about my condition, I receive an outpouring of love, support, advice, and encouragement.

One thing I would like others to know about chronic illness is that it is an invisible disability. People suffering with chronic illness might appear perfectly okay or ‘normal’ on the outside, but inside we may be in pain, fatigued, nauseated, or in a fog. I was once ridiculed by someone for sitting in the ‘accessible seating’ area on the bus. I was experiencing a severe flare, but to the people around me, I looked like a ‘selfish, lazy, young, healthy girl’ who should stand so ‘someone who needs it’ gets a seat. Not all disabilities are visible, so, when in doubt, be kind. Similarly, be kind to yourself and trust your intuition. You know your own body better than any physician or specialist.
If you feel like something may be wrong and your doctor is dismissive, get a second opinion. Get a twentieth opinion. See as many doctors as necessary to get the answers you need. I firmly believe my family doctor saved my life, but I never would have found him if I had accepted my initial diagnosis. I had to see over twenty different medical professionals to finally find the one that helped me.

My hope for my own future is to be a leader in marine science and environmental conservation. I am currently studying for my Master’s in Resource and Environmental Management and Planning at Simon Fraser University, and I eventually hope to go on to get my Ph.D. Living on the west coast of Canada, I have developed a passion for the ocean, and I hope to build a career where I can make positive changes for ocean ecosystems. I also hope to be an inspiration for others who are dealing with chronic illnesses. This journey has not been easy or straightforward, but it has shown me just how strong I am. Even when my body is weak, my heart and my mind are stronger than ever. While my prognosis at this point is unclear, I am determined to make the most of the life I have.
It was a deep struggle for me to write my story. I do not want to glorify my situation, nor do I want to complain about my circumstances. I am simply trying to share my story in the hopes people reading my story will take away a message of hope, appreciation, and love. We will all face circumstances in life where things happen that are out of our control. Think of this adversity as an opportunity for growth. Everyone out there who is experiencing adversity, I want you to feel hope, know you are strong enough to make it through, and you can live the life you want.
Your circumstances and your path might change, but you can still reach your goals and live your dreams. Believe in yourself, trust yourself, love yourself. And most importantly, appreciate the life you have and the world around you. No matter what your situation is, look around and choose to appreciate what you see. Life is too short not to.”

This story was submitted to Love What Matters by Chelsea Mathieson of Vancouver, British Columbia, Canada. You can follow her journey on Instagram, Facebook, and LinkedIn. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Do you know someone who could benefit from this story? SHARE this story on Facebook to let others know a community of support is available.

