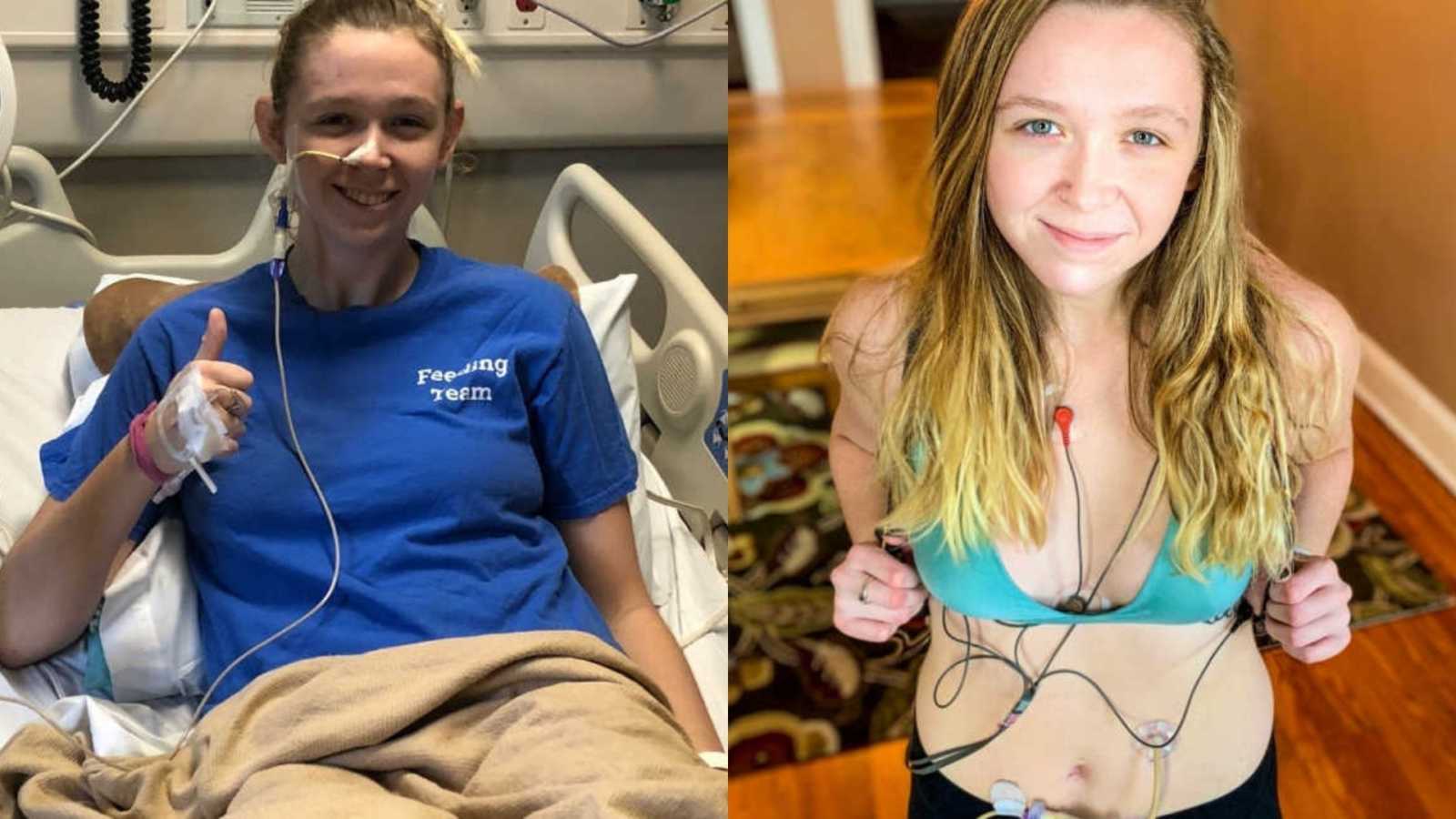
“I sat at my graduation ceremony from Emory University in May of 2017, smiling because I knew I would begin my dream job in two weeks. I received my Bachelor’s in Psychology, and had found the field I wanted to go into; feeding disorder therapy. My senior year I had a practicum placement at Marcus Autism Center working in their feeding disorder program, and within a few hours of being there I knew it was what I wanted to do. I felt as if my entire life had led to this job; I had found my calling.
I started working at Marcus, and within eight months was promoted to a Clinical Specialist in the feeding disorders program. I had absolutely found my niche; it was my job to work one-on-one with children on feeding tubes and slowly transition them towards oral intake. Frequently, children were admitted to our program with 100% feeding tube dependence and by discharge, they were able to have their feeding tubes removed. These moments of success in which children were able to transition off of their tubes were some of the greatest moments of my life. The feelings of accomplishment, pride, and excitement were unparalleled. Parents would frequently write us handwritten notes thanking us for the impact we’d had on their children’s lives and their own, explaining how meaningful it was to have their child no longer depending on a tube to sustain themselves.
About a year after I began my job at Marcus, I started to notice I was throwing up frequently. I thought it was related to my diet, so I cut out several foods, but the vomiting persisted. After awhile, I found I could only eat a few things without being extremely sick for hours. Finally, I realized this was interfering with my ability to do my job, and I went to a doctor who ordered a test of my esophagus and stomach. During the first test, a barium swallow, a doctor pulled me aside and asked me if I had ever heard of the term ‘gastroparesis.’ I didn’t know it at the time, but this would be a word that changed my entire life. What I thought was a reaction to my diet turned out to be incurable paralysis of my stomach. My doctors ordered another test, referred to as a Gastric Emptying Scan, to confirm the diagnosis of Gastroparesis. I was sitting at work, about to start a session with a patient, when I got the call from my doctor. It felt like time stopped moving, as I picked up my phone and answered him. The only part of that conversation I remember is him telling me there are no known cures and even the existing medications to help with symptoms are not very successful. I sat at my desk with my heart pounding in my chest and cried; the reality of what this meant was slowly sinking in… my stomach wouldn’t ‘get better,’ I might never eat normally again, and it could spontaneously get much worse… But it didn’t stop there.
The next few months were full of invasive tests including an Esophageal Manometry study showing that my esophageal function was between 20-30%, a Tilt Table Test showed I have a rare form of am autonomic nervous system disorder called Hyperadrinergic POTS, and several other gastric MRI’s and x-rays. It felt like every time I stepped foot in a doctor’s office, I had another diagnosis that was incurable. By this point I was almost fully bed-bound, but my mom convinced me to give one more doctor a shot. So together, we flew to the Cleveland Clinic to see Dr. Michael Cline, head of the gastroparesis department. Within five minutes of meeting Dr. Cline, I found out what had caused essentially my entire body to fall apart: I have a very rare genetic disease called Elher’s Danlos Syndrome. It affects the connective tissues in my body, causing my joints to be unstable and my organs to be too loose.
Due to the severe decline in my health, and the knowledge that this wasn’t going away anytime soon, I was forced to take disability leave from work. By this point I was on an almost fully liquid diet and was throwing up almost daily and losing weight quickly. I got questions from cashiers at grocery stores when I purchased baby food and formula, I got glares from strangers at restaurants when I wasn’t ordering anything, and I felt judgement in every public restroom I threw up in. It began to weigh me down; I was starving because even a small amount of food would leave me in excruciating pain and severely bloated, and I felt the world was judging me for not being ‘normal.’ Eventually, I agreed to have a temporary naso-jejunal feeding tube placed in order to bypass my stomach entirely. In that moment, the irony of my situation became abundantly clear; I had gone from helping children get off of feeding tubes, to needing one myself.
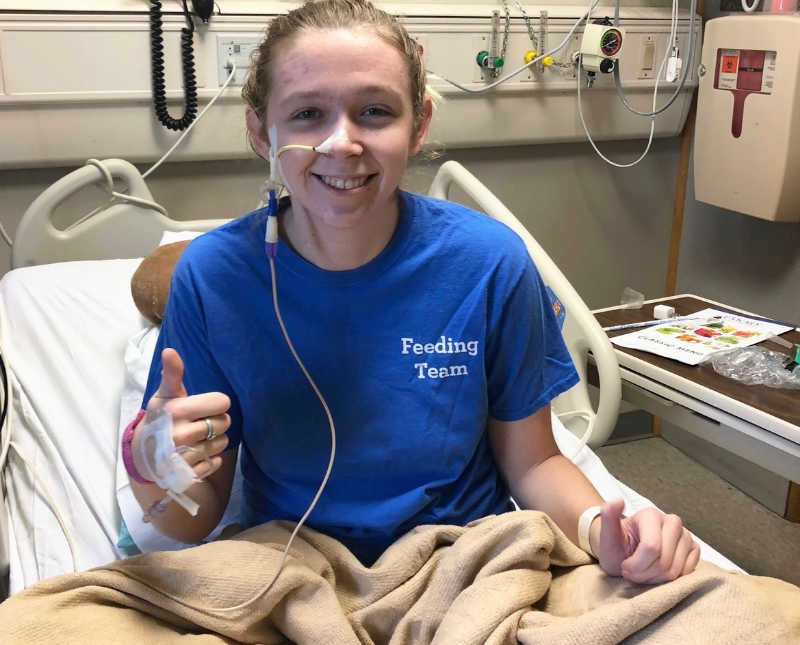
I spent the majority of that hospital admission sobbing; grieving the life I had walked away from, feeling indescribably helpless my sustenance was entirely dependent on this tube coming out of my face that anyone could see. I was terrified that my boyfriend would leave me because the tube made me look different, or because it was just too much for him. Fortunately, despite the irony of the situation, the nasal tube worked and showed that this was a viable method of receiving nutrition.
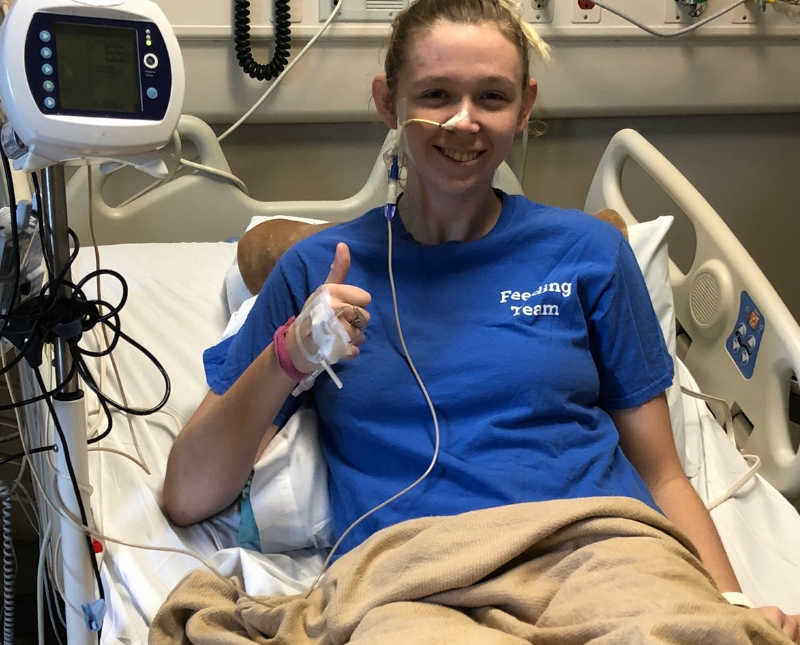
Unfortunately due to my esophageal dysfunction, the nasal tube had to be removed after about a week, and I was left once again with no nutrition.
These were some of the darkest weeks of my life; I was literally watching myself decay. My face didn’t even look like my own anymore, my ribs were visible from a distance, and I was too frail to shower standing up. I was throwing up so often I carried around a bowl with me at all times for spontaneous episodes. At my absolute sickest, I genuinely thought I might starve to death. My mother stayed with my boyfriend and I to give me 24/7 care because they knew I couldn’t be left alone safely. I couldn’t even stand up to get a glass of water without risking falling or blacking out. I felt my boyfriend distancing himself from me out of fear; he kept telling me how scared he was for me and how he didn’t understand how this could have happened to me, how it all happened so quickly.
Finally, my mom and I realized I would die if I kept living the way I was. My mom is the bravest woman I’ve ever met; if she’d ever been scared before in my life, she hadn’t shown it. But during this time, the fear was so clear in her eyes, I could feel it in my own soul. So she and I returned to the Cleveland Clinic and within minutes I was seen by a surgeon and scheduled for an urgent surgical Jejunostomy tube placement and admitted to the hospital for dehydration and malnutrition. Four days later, I woke up from surgery with my lifeline; a permanent feeding tube that delivers nutrition directly to my small intestine, bypassing my paralyzed stomach.

My recovery from surgery hasn’t been easy physically or emotionally. The first day I spent at home after the surgery, I cried for hours because I realized I would never have a ‘normal’ life again. My mom’s apartment was full of formula and gauze and syringes, I was hooked to an IV pole, and it just sunk in that this was how I lived now: a patient. A few days later, my boyfriend of almost 3 years broke up with me for the exact reasons I had feared: I was too sick, and required too much from him. While it broke my heart to lose someone I had planned to marry, and at such a vulnerable time in my life, I am incredibly grateful for his choice to end things. I had to recover from the biggest thing I’d ever undergone, without any help from the person I relied on most, but this made way for my mom, the rest of my family, and my incredible friends to step in and pick up the pieces of me he wasn’t strong enough to handle. It also forced me to realize I was strong enough to withstand anything life throws my way because I had no choice but to be strong and keep fighting for my life.
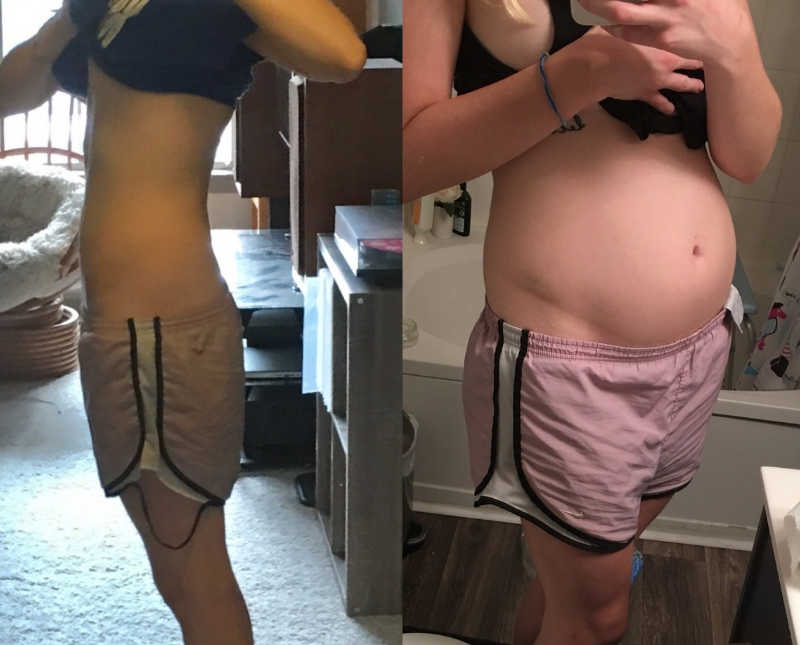
While my transition from feeding disorder therapist to having a feeding tube myself was extremely scary, painful, and at times devastating, I am eternally grateful for my tube. It is the reason I am still alive today. My memories of being a feeding therapist will always be important to me, but I am learning to find just as much meaning in being a patient. My whole time working as a feeding therapist and early in my own feeding tube journey, I saw feeding tubes as a tether; something that held people back and tied them to a pole. Now, I see them as a life-line. What once symbolized captivity, now symbolizes TRUE freedom; the freedom to live my life how I want to.
Right now, I don’t know if I will ever be able to work a full-time job again. Elher’s Danlos can be progressive; meaning it can get worse. I recently spoke to my doctor and asked him if he’s worried about more of my organs being affected or failing. He told me he can’t promise me anything, but that he believes in me and that I need to go live my life NOW, exactly the way I want to. I’ve stopped waiting until the ‘timing is better’ to do the things that matter to me, because I’ve realized that no one truly knows what the future has in store. My plan for the next year is to convert a van into a camper van and travel the west coast with my dog, Sadie. I’ve had this dream for years, but kept putting it off until ‘after.’ Now. I’m making it a priority right now. No one can promise me what my body will do or what my life will look like five years, ten years, however long down the road. So I’m going to enjoy the life I have right now, and not take a second of the freedom my feeding tube has given me for granted.”
This story was submitted to Love What Matters by Allyson Quirk of Washington, D.C. Follow here journey here. Submit your story here. For our best stories, subscribe to our free email newsletter.
Read more about chronic illness:
SHARE this story on Facebook or Twitter to support those battling chronic illness.