Disclaimer: This story contains details of child loss which may be upsetting for some.
Excitedly Expecting
“Like most first time moms, I truly felt my journey to motherhood began the day we found out I was pregnant. Something inside me seemed to click, and my mind began to process that, at every moment of the day, there were two hearts beating within me. This is the time I seemingly cherished the most – quiet moments with myself and my growing belly. I was glowing and growing!
At my 20-week anatomy scan, I was diagnosed with placenta previa. According to my OB, this was nothing to be worried about, as nearly 85% of cases resolve themselves. The biggest risk factor for previas is bleeding, and he informed me bleeding typically occurs in three phases, so we would do our best to get as far along in the pregnancy as possible. The care plan was to repeat the scan at 36 weeks to determine if my placenta had moved. If it had not moved enough to deliver safely vaginally, ‘worst case scenario’ would be a scheduled c-section three weeks prior to my due date, so hemorrhaging could be controlled.
I was put on pelvic rest (no sex, no bike riding, no extreme exercise, and no horseback riding). ‘Keep living your life,’ my OB told me week after week. We sailed through the next seven weeks with no concerns. My fiancé painted the baby’s nursery, I prepared my job for my maternity leave, and together with our families we planned to have our son’s baby shower. We were living!

Emergency C-Section
At 27 weeks and 4 days, a glowing and uneventful pregnancy took a drastic turn. It was Memorial Day weekend, and the weather was rainy and gross. I took a nap that Sunday afternoon, and when I woke up, I had an alarming amount of hemorrhaging. The time was 5:07 p.m. I called my OB, and we immediately went to the hospital. When we arrived at Labor & Delivery, the nurse was calm and informative. I will always remember her for this. She let us know that, based on the amount of hemorrhaging that already occurred, I would be admitted under observation for at least 24-hours. I remember thinking back on conversations I had with my OB prior, and just thought this type of hemorrhaging is what was expected for women with a placenta previa diagnosis. We settled into the room, but I continued to hemorrhage. I was starting to read the nonverbal cues of the nurses and doctors. Concern. Change in my care plan. ‘Worst case scenario.’
We were told that, based on the amount of blood I was losing, I was going to be administered magnesium through my IV in case we had to deliver, as it would help protect our baby’s brain. They reviewed the symptoms I would feel as a result of the magnesium. ‘It will feel like you have the flu. Fever, chills, maybe nausea.’ Within the first 30 minutes, I felt my body responding to all of these symptoms and I was struggling. I became hypotensive and our son’s heart rate was dropping. The two hearts in my body were fighting to stay alive and, before I knew it, I was being rushed into the operating room for an emergency C-section under general anesthesia all alone. In 3 hours and 35 minutes after my first placenta previa bleed, our sweet son, Lorenzo Francisco, was born on May 30, 2021 at 8:38 p.m.
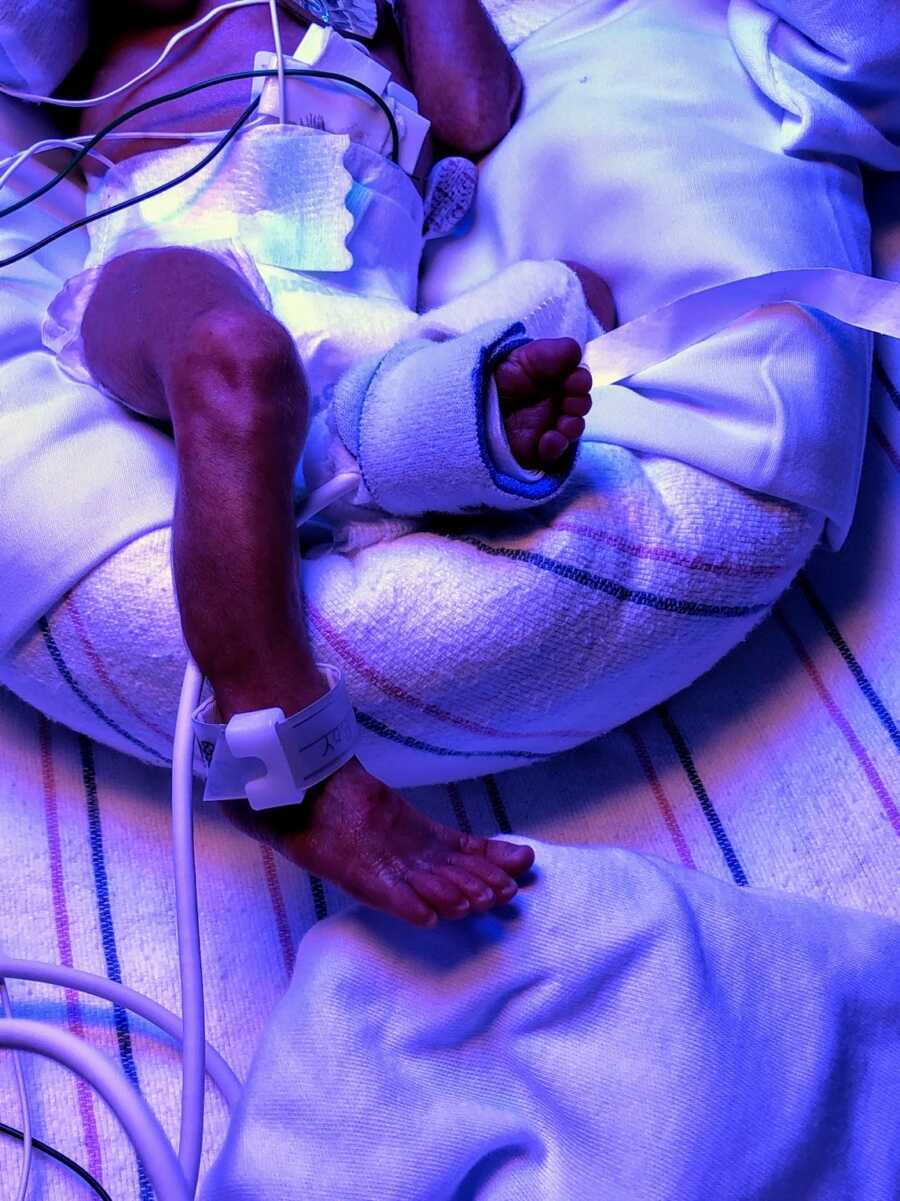
It took me nearly two hours to wake up in recovery, as I had endured a significant trauma and received two liters of blood as part of the massive transfusion protocol. When I was more alert, the neonatologist who delivered Lorenzo came and sat with us. He began explaining our son was settling into the NICU and what we could expect over the next 12-24 hours. I was trying to comprehend everything he was saying, but one thing I knew for sure was I instantly felt like a mom.
NICU Parents
We got a crash course on what it meant to have a premature baby, and what life in the NICU would start to look and feel like. We spent the next few days in the hospital with 24-hour access to Lorenzo, learning about each monitor, tube, and medical term that now described our son and his care. Lorenzo’s first NICU nurse who cared for him at his delivery and his first two days of life, helped me process and prepare for what life would mean for us now as a NICU family. She was the first person to talk to me about my son, but was also the first to ask me how I was doing.

On Lorenzo’s fourth day of life, we were discharged from the hospital. My postpartum nurses made sure we had everything we needed to support my physical recovery and reviewed the risks of postpartum depression. I haven’t mentioned this yet, but I am a licensed clinical social worker. I made a point NOT to share this with too many people in the hospital because I didn’t want to be treated as if I knew anything. The truth was I did, but not as a mother. And in all of these moments, I was a mother, not a therapist. But even as a therapist, I internally rolled my eyes and remember thinking, ‘Yeah, yeah I won’t need this depression and anxiety scale, but thanks.’ I left the hospital feeling like I had nothing to be depressed about. My son was here and alive. What was there to be sad about? But later that night, we had to make the gut-wrenching journey out of the hospital, to our car, and then home without him, and I knew there was a whole lot to be sad and anxious about.
While we knew Lorenzo was in the best place for the care he needed, he was no longer just a floor above us. We were 18 miles away from him. The first few days home from the hospital were filled with so many emotions. We began sharing the news of Lorenzo’s birth with family and friends. I was pumping every two hours, since that was the only thing I could truly do to care for my own son physically. We went back and forth to the hospital every day together. We held hands and talked to Lorenzo, while getting updates from nurses, neonatologists, and respiratory therapists. While not every update was positive, we rode each wave as best we could. We got to know his care team and, to this day, we believe he received the most exceptional care.

On Lorenzo’s tenth day of life, his progress and our journey as NICU parents took a hellish turn when we were met with information that Lorenzo had developed an infection that had localized in his lung and was wreaking havoc on his body. We waited anxiously and impatiently for the lab to confirm the worst, which was that it was MRSA. The next 48 hours were horrible, and I can say without any hesitation, I didn’t think once about my own body and what it might need from me. We spent every hour possible with him and, other than pumping, I’m not sure if we ate or even drank water – my entire body was numb and zombie like.
Losing Lorenzo
On Lorenzo’s twelfth day of life, I called the NICU around 5 a.m. to see how he was doing. A panicked nurse passed the phone to a calm, but direct, neonatologist who encouraged us to come to the hospital as soon as possible. We rushed out the door and drove in silence for the 18 miles it took to get from our home to the hospital. Neither one of us wanted to speak and say what we were both thinking which was, could today be the day our baby dies? We entered Lorenzo’s room, and the nurse shared his condition had improved slightly, and they were continuing to do everything they could for him. I prayed nonstop, rosary beads never left my hand that day.
The same neonatologist that delivered Lorenzo was on shift and noticed. He gently asked if we would like them to facilitate a baptism for Lorenzo, to which we immediately said yes. Later that afternoon, we were able to have my parents and my fiancé’s mother come to the NICU and meet Lorenzo for the first time and witness his baptism. This would be the only time they would be able to share with their grandson.
On June 11, 2021, around 6:30 p.m., in a room full of nurses and doctors bearing witness to our pain, Lorenzo’s journey on earth came to an end and we held him in our arms as he took his last breath. I remember someone asking if we wanted them to take pictures for us and it all felt so wrong, but we knew now those pictures would be the only ones we had holding our son.

The next few hours were catatonic. We listened to the nurses share information about memory making and burial options. They made us a memory box of his hand and footprints, hospital bracelet, blanket, and strands of his beautiful curly hair. When we mustered up enough courage to leave, our only physical memories of our son were packed up into a plastic ‘Patient Belongings Bag.’ We exchanged goodbyes with the NICU staff and walked out of the unit, into the elevator, and out through the lobby for the last time as NICU parents. We sat outside on a cement bench for what felt like another hour before making the impossible decision to go home.
Home without our first child, our sweet baby boy. Home with only a plastic bag representing our time with him. Home didn’t feel like home anymore. It felt empty and dark. My breasts were heavy and warm, reminding me it was time to pump out the milk for a son who no longer needed it. I sat on the couch in the dark to pump that night. The darkness felt all encompassing; it felt like the only safe place now. When I was done pumping, without hesitation, I handed the bottles to Pedro, and he courageously dumped them for me. Wow, we really underestimate the resilience of fathers. We laid in bed that night, and for weeks, unsure of what had just happened. How did our life spiral out of control so quickly? What do we do now?
Surviving Child Loss
Survive – that’s what we do now. Somehow, we managed to call our church and plan a funeral mass, make the decision to cremate Lorenzo, and pick out an urn for his final resting place. Even as I type these words, I am unsure of how we made this happen. The only explanation is we have so much love for Lorenzo and nowhere else for it to go but into things honoring his life. This was the moment I realized there were other families like ours out there. There were other parents whose child died, but they survived. We take each moment at a time now. Some days it’s by the minute, others it’s by the hour or day, and before you know it, you’ve survived 14 months without your son on this earth.

Surviving, for me as a bereaved mother, meant connecting with other bereaved families. It is in those moments we heal, we unite, and we survive. As a natural born advocate, therapist, and now bereaved mother, I was so unsettled by the emotional support offered to our family. I channeled this energy and established Courage in Time Inc., a 501(c)(3) nonprofit organization dedicated to supporting families who have experienced stillbirth and infant loss through cursed bereavement boxes, grief, and postpartum resources, and connection to other bereaved families. We have been able to send courage and support to 172 families since our launch in February 2022. Our strength, our survival, lives alongside other bereaved families who get up every day and honor their children who were taken from this earth too soon. We live for our son and honor him in all we do.

To all the bereaved families, we are so sorry you are here. We are so sorry you now know the immeasurable pain that is the death of your baby. We want you to know you are not alone. We want you to know there is no perfect way to walk through this journey and this is not your fault. Our hearts are with you, sending gentle love and gentle courage.”

This story was submitted to Love What Matters by Jillian DeGroot of Northern New Jersey. You can follow her journey on Instagram, Facebook, and her website. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories.
Read more stories like this:
Do you know someone who could benefit from this story? SHARE this story on Facebook to let others know a community of support is available.

