“I have never shared my entire story. While it’s not the easiest, I am here to break the silence… to share my story, in hopes that others who have gone through this can feel a connection in the ‘club’ none of us want to be a part of.
Kennedy was a little over 1 and a half when we decided we wanted to grow our family. We got pregnant on our first try and were over the moon excited to give Kennedy a sibling and grow our family. My pregnancy was average – a little morning sickness, kind of tired, but nothing out of the ordinary. Around 15 weeks I started noticing a little bit of blood when I’d use the bathroom. I was frightened, but thought, ‘Ohhh that’s probably just this… or that… (really trying to calm my own nerves).’ One morning especially, it was darker. My husband had already gone to work and I was sure I was losing our baby. I called my OB and sat in bed crying until my husband was able to come take me to the doctor. At the office, we were told I had Placenta Previa, which is basically a low-lying uterus and I was put on pelvic rest. We were also able to learn that our sweet baby was a GIRL, which we decided to name Hattie.

A week later I was still bleeding sort of heavily, so we went BACK in, and I was then put on moderate bed rest…No heavy lifting, including Kennedy, and to try to limit my ‘on my feet’ time to an hour a day. Placenta Previa isn’t fairly uncommon and I NEVER thought it would be harmful to Hattie. We had to cancel our plans to fly to California, ‘in case’ I started hemorrhaging. This seemed SO extreme to me, but it was more dangerous to ME bleeding than harming Hattie herself. Fast forward to Easter Eve 2015…
IT happened. I woke up around midnight, soaked in a pool of blood. I immediately yelled ‘hospital!’ to my husband as I jumped up to go to the bathroom. A trail of blood followed me. I wrapped myself in a towel, and thank God for my mother-in-law, who was staying at our house, whom we threw the baby monitor to and bolted out of the house. That drive to the ER was scary. I thought I might die – I was literally hemorrhaging, scared to death that this was it. I was admitted to the Labor and Delivery/Women’s floor. The nurses and doctors were great. They told me while I may be in the hospital a lot, they’d do anything they could do keep my baby alive. I was put on Magnesium, which basically felt like an actual fire IN my body. I was SO sick… Vomiting, sleeping, couldn’t eat… it was terrible. While I know I was doing what I could to help Hattie and I, I felt so guilty being away from a young Kennedy, who didn’t understand why her mommy wasn’t home. A few days later I was released from the hospital, but put on total bed rest. After just 4 hours of being home, the bleeding was heavy once again. I called the hospital, and of course was told to come back in. Devastated, I obliged and back I went. After a few more days in the hospital, I was given Procardia – a medicine normally given to patients with heart problems, but it also helps to relax the Placenta to stop any contractions/early labor. We also found out the ultrasound showed my fluid levels weren’t where they should have been.

My 20-week appointment had arrived and I had SUCH high hopes of being released off bed rest since my bleeding wasn’t as heavy anymore. Wrong. My fluid levels were still low, but a huge worry still hadn’t crossed my mind. My mother-in-law was still staying with us to help with Kennedy and my husband was out of town for work that week. I woke up around 2 a.m. on April 22nd with cramps. I was in a group text with my 2 best friends in California (one of whom is a nurse) since they were awake with the time difference out there. I was on the bathroom floor, crying, cramping and I just knew. I called my mom, who picked me up and took me back to the hospital. The tocodydamoter (machine which measures contractions) didn’t show much, even though I could still feel them. The on-call doctor thought maybe I had a UTI, or something else. When he decided to do an ultrasound is when my world was turned upside down. It was of course when my mom was running to grab her coffee, so there I sat. Alone, with an on-call doctor, doing an ultrasound which looked like nothing. His look on his face said it all. I had zero fluid and could see just the top of sweet Hattie’s head. I tried to hold back the tears, tried to stay strong, since at that moment I had no one but myself.
When my mom came back in the room, I lost it. I felt almost guilty to tell her what we discovered. The on-call doctor told me that a High-Risk specialist would come in to do a detailed ultrasound around 8:30 that morning, but it wasn’t looking promising. I was able to get ahold of Josh and he was on his way (around 3 hours away for work). The two women that did the high-risk ultrasound had a look of despair the entire time. She confirmed I had lost all my amniotic fluid, but Hattie was still alive. She told me she had about a 1% chance of survival and to basically not keep any hope. After that we had grievance counselors coming in telling us what to expect. What would we do with her post-delivery? Here are the arrangement options. Do you want to hold her? In my mind, I was still holding onto that 1% chance while also fighting reality that I would soon deliver my baby girl. The baby we prayed for, planned for; the baby we wouldn’t take home to join our family. They said it could be days. I laid in that hospital bed all day, in and out of reality. I got up to go to the bathroom and I felt her. It was the first time I truly felt her move during this pregnancy. I called the nurse in and said, ‘I think I felt her fingers and toes moving – and LOW.’ Sure enough, she was at the end of my cervix, ready to enter this world 19 weeks too soon.
My OB was called in, two nurses also came in. One was the same nurse who helped deliver Kennedy nearly 2 years prior. The other was a nurse who was there the first night I was admitted. I thought this would be quick. I was wrong. Her feet and body basically slipped out, but my cervix wasn’t dilated enough to deliver her head. It took two hours to fully deliver her. It was a quiet and sorrowful 2 hours. I leaned up at one point and could see her legs. She was lifeless. I’m positive that bathroom break was Hattie’s last movements and I hold onto those movements every day.
Hattie was born at 11:06 that night on April 22, 2015. She was a tiny 7.6 ounces and 8.5 inches long. She was whole and perfect, just tiny. She had long fingers, chubby thighs and the cutest little button nose. I held her for hours. I touched every single part of her little body, engraining that into my head so that I’d never forget how perfect my little girl was. I do have photos of her and with her, but I’m not ready to share those special moments quite yet. I look at them often. I have the blanket they wrapped her in, a bear they gave her, her tiny footprints and more. These items mean the world to me. I wasn’t ready to let her go, and honestly I’m still not.

We laid Hattie to rest in an area they call ‘babyland’ at our local cemetery. We visit her often. Kennedy talks about her a lot. I miss her daily. What would she have looked like? What would her personality be like? How would Kennedy and Hattie be together? Why didn’t she get a chance at this life? Why did MY body fail her? While I cannot answer these questions, I DO know that I am OKAY right now.
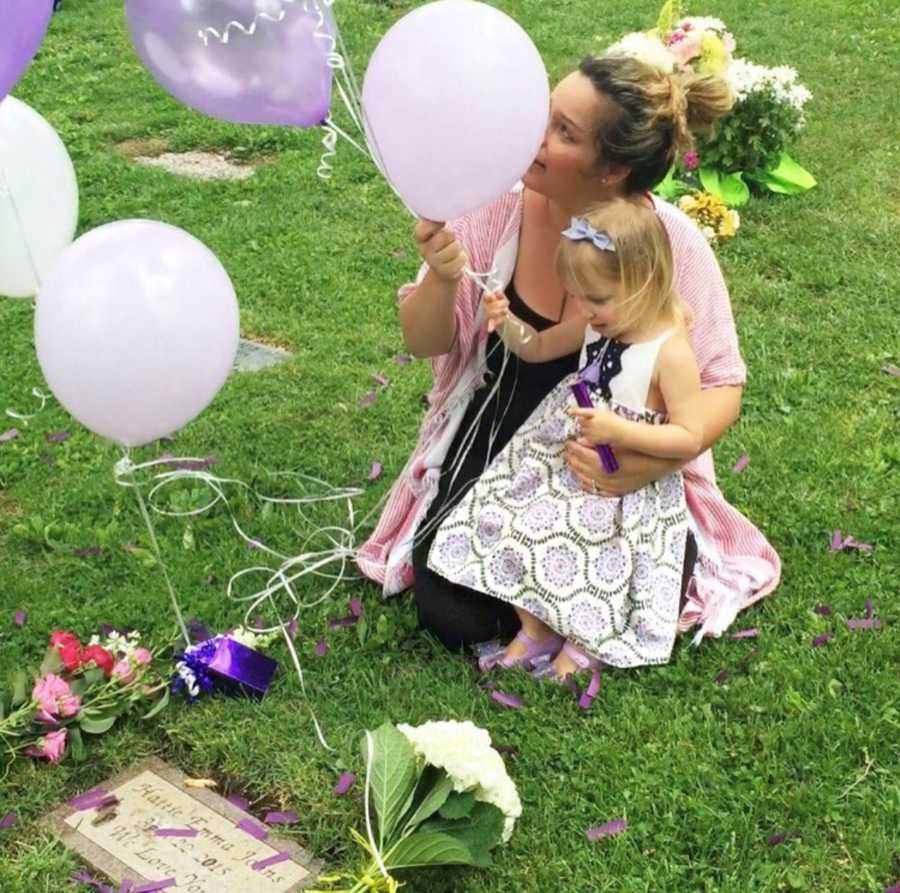
Grief isn’t an easy road; it’s a life-long process. I am sharing my story because I know I’m not alone. After losing Hattie, I read stories on other’s loss. In a way it helped me grieve knowing I’m not alone. I connected with other moms who have lost a child, joined Facebook groups, found Instagram’s with grieving mothers and more. I needed to feel a connection in some way at a time where I felt SO alone. If you have experienced loss, I encourage you to reach out. I’m happy to be a listening ear and friend, or find resources locally.
I may be 1 in 4 of a club I never asked to join, but I am here to break the silence.”



This story was submitted to Love What Matters by Kristyn Johns of Lexington, Kentucky. You can follow her journey on Instagram. Submit your own story here, and subscribe to our best stories in our free newsletter here.
Read more stories like this:
Please SHARE to help educate others about the grieving process, and the kind of support it takes to help heal.

