“My parents were in their mid-thirties when I was born. My oldest sister was sixteen, my older brother was ten, and then there was me. I was the baby of the family, the last born. Until, when I was four years old, my sister gave birth to a beautiful and healthy baby boy. It was the first baby I had ever seen or held; my first nephew, Brett.
I was an auntie for the first time, overwhelmed with new feelings and emotions. I fell in love with him the very first time I saw him, and I knew in that moment, I wanted to love him and protect him for the rest of my life. It was then, at four years old, I knew I wanted to be a mom.
I helped take care of Brett when he was a baby, and as we got older, he grew up with me as a little brother would. We played make believe, climbed trees, rode bikes, and got into mischief as all siblings do. We laughed, we cried, we screamed and yelled at each other, but we never stayed mad. He looked up to me, and I looked after him.

I watched him grow from a boy to a man; from braces with a squeaky voice, to girls, guitars, and graduations. He was my best friend when he was a boy, but as he got older, I stepped back to watch him grow. Our bond was special, and I loved that once little boy, now grown man, in a different way than I’ve ever loved anyone else.

On the morning of September 3rd, 2017, I got a phone call which changed my life. It was my mom screaming in my ear, ‘Brett’s dead, honey. He’s dead!’ My mind went blank. My body went numb. I yelled back, ‘MOM! WHAT HAPPENED?!’ My only reply was incoherent screams and sobs, so I hung up the phone. I hung up on my own mother, to try to understand what I couldn’t comprehend.
It was Sunday morning. I had just talked to Brett on Friday night. I frantically called my sister, all the while thinking it couldn’t be true. It had to be a mistake. My sister answered the phone, ‘ROOOOOOOSE!!!’ My middle name she always called me so lovingly, now tinged with the sound of pain. I heard her start sobbing as she dropped the phone, and I knew it was true. I knew in that moment, our little boy, now grown man, was gone forever. My heart sank as I hung up and fell to the floor, while all the strength left my body. My worst nightmare had just become my reality. It was later confirmed to be an accidental opiate overdose. He was only 23.

I almost lost myself that morning, drowning in a grief so intense I didn’t think I could ever recover. As I laid on the floor, I let myself sink into the mental darkness, wanting nothing more than to live there forever. My husband came to my side and scooped me up from the floor into his arms. He asked me what happened, but I couldn’t say it. ‘My boy…,’ I told him and trailed off. He looked at me, not understanding, while tears streamed down my face.
‘Brett,’ I said, ‘He’s dead.’ The realization of the words hit me as soon as they left my lips. I saw the sympathy in my husband’s eyes as he hugged me tighter, but in that moment, all I could think about was my sister. I thought about how she needed me. She needed me to be strong for her when she couldn’t be. She needed me to be there for her like she’d always been there for me. And just like that, with a strength I never knew existed, I pulled myself out of the darkness of my mind and got up off the floor.
That day was one of the worst days of my life, losing the first baby I’ve ever loved. But it was also a day that changed me forever. It showed me I can survive the darkness. It showed me how strong I can be when it comes to the people I love the most.
Before losing Brett that fall, my husband and I had decided to tell our family, in early summer, we were going to start trying to have a baby. I still wasn’t pregnant by the time we lost Brett, and I had started questioning if it was going to happen. After he passed away, it put me into an even deeper place of sadness about it. I would cry, talk out loud to Brett, and beg him to send me a baby. I would tell him, ‘Our family is hurting so badly. We need some happiness in our lives.’
As fate would have it, we conceived our daughter the weekend of Brett’s memorial benefit concert, only three weeks after his death. The pregnancy was confirmed just a week before his memorial service the following month. I knew for sure my guardian angel, Brett, had finally sent me the baby I had always wanted.

Everything was fine, until at 20 weeks, the ultrasound tech noticed an abnormality during a growth scan. After looking at the images, the doctor made the diagnosis of a ‘single umbilical artery’ in the umbilical cord. A typical umbilical cord contains two arteries and a vein, to transport nutrients and oxygen to, and remove waste from, the baby. With us, one of the arteries didn’t form properly and died early on, leaving our umbilical cord with only one artery, instead of two.
They told us it occurs in 1 in 100 pregnancies, and usually, the babies are just delivered early so they can grow easier outside the womb than inside. Our high-risk specialist informed us a single umbilical artery can sometimes be an indicator of a genetic abnormality, but they usually see other issues along with it, if that were the case. Since they found no other issues, they did not deem it necessary to get an amniocentesis, and the decision was left up to us if we wanted to rule out the possibility of genetic problems. Since our routine blood work came back with a decreased risk of genetic issues, and our nuchal translucency tests came back normal, we chose not to do the amniocentesis.
Shortly after this, they noticed our daughter wasn’t growing at the rate she should. They diagnosed her as being intrauterine growth restricted and small for her gestational age. At her lowest, she dropped into the 2nd percentile for growth. The goal was to get to at least 32 weeks gestation before trying to deliver. This was because, at 32 weeks, she would have a higher survival rate if she had to be born early.

Beginning at 28 weeks, the high-risk specialist recommended we go in for non-stress tests twice a week, and weekly growth scans. They wanted to make sure she was still growing and progressing, otherwise they would need to deliver. We would routinely fail the non-stress tests and be sent to the hospital, where they would hook us up to a better doppler, get acceptable readings, and send us home. This happened every week.
Then, at 32 weeks, we failed another NST and got sent to the hospital again for better monitoring. But this time it was different. This time, they chose to keep us so they could monitor us overnight. The next morning, the doctor told me my daughter’s heart rate was dropping, and her time left in my womb was limited. They said if we didn’t deliver her soon, we could lose her. I was scared, but I knew it was the right decision.
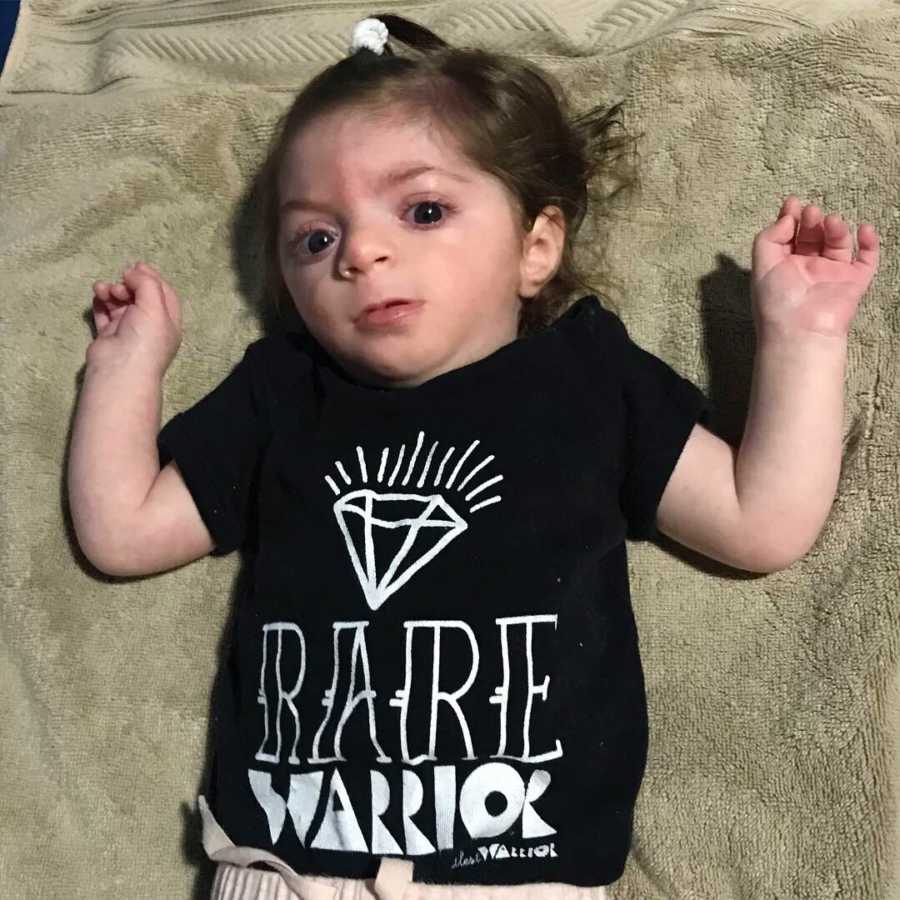
The next morning, our daughter Joplyn was born 8 weeks premature via C-section, weighing only 2lbs 15oz. She was in the NICU for a total of 92 days: 46 days at St. Joseph’s Hospital in Stockton and 46 days at UCSF Benioff Children’s Hospital in Oakland.
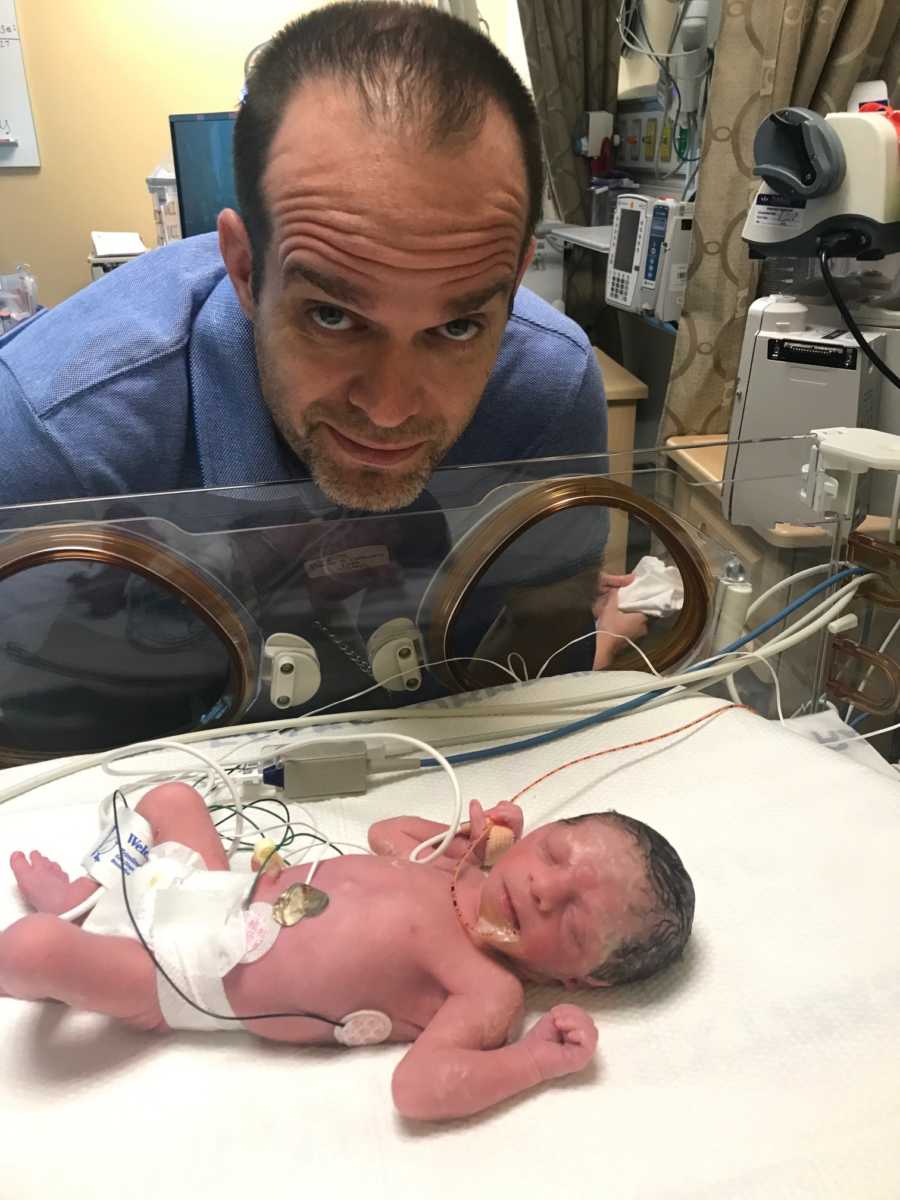

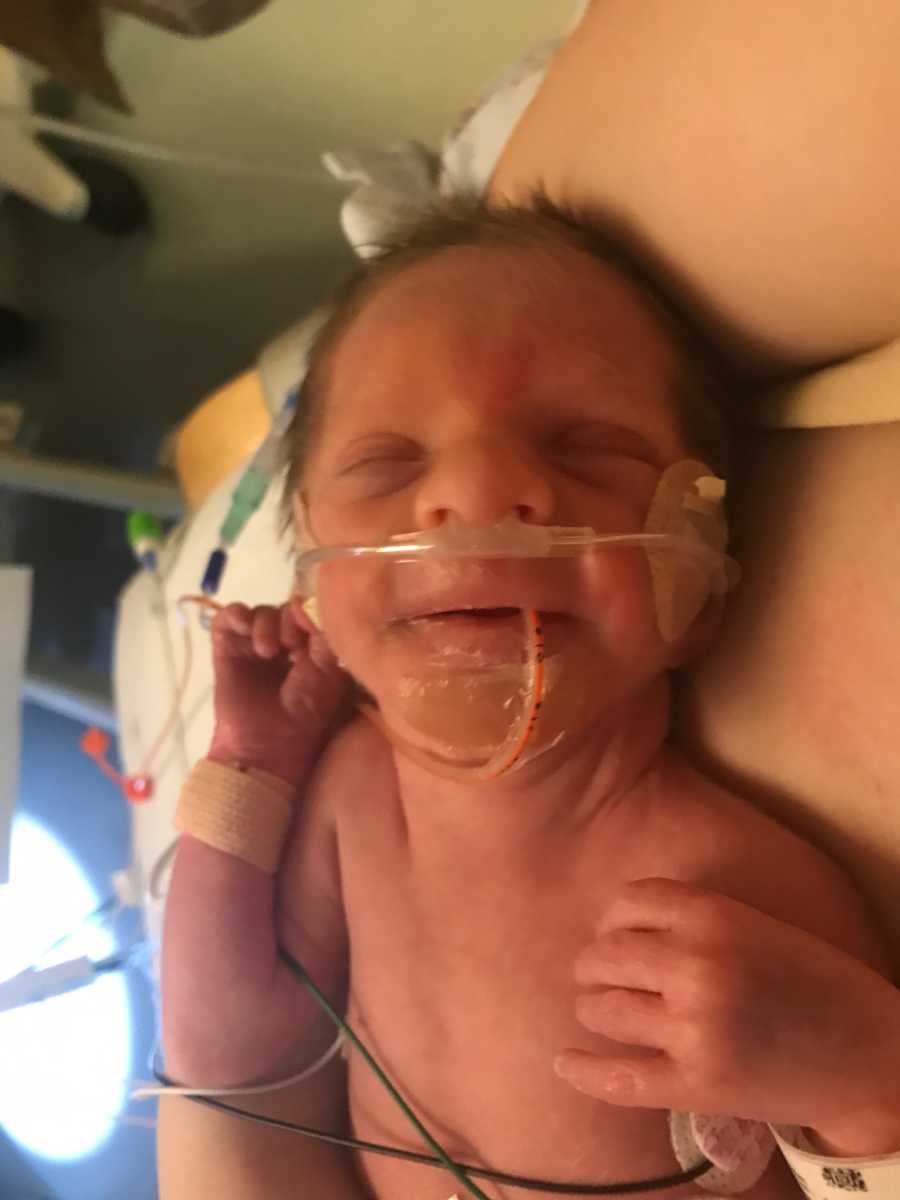
She was transferred to Oakland due to feeding issues, malabsorption, and insufficient weight gain. At this time, they performed a swallow study and determined she has ‘silent aspiration,’ meaning when she swallows, part of the liquid goes into her lungs instead of her stomach. It is dangerous because it can lead to respiratory issues such as pneumonia.
Shortly after arriving in Oakland, they recommended doing a genetic test to see if there were a genetic explanation for her compounding health issues. Two weeks later, we were called into a private family meeting where they gave us the news. At two months old, our daughter Joplyn was diagnosed with an extremely rare genetic condition called chromosome 17p duplication (11.2-13.3).

Part of her genetic duplication causes a disease called YUHAL Syndrome, which combines the features of Charcot Marie Tooth Disease 1A + Potocki-Lupski Syndrome. If you google the occurrence rate of YUHAL Syndrome, the Genetics Home Reference government website states, ‘The prevalence of YUHAL syndrome is unknown. More than 20 people with the condition have been described in medical literature.’ After her diagnosis, the geneticist also told us if they had found her chromosome duplication while I was pregnant, they would have recommended termination. There is not enough research about the disease, and it would be ‘no quality of life.’
The doctors still don’t know what to tell us, because of the limited research available. But they say the worst-case is she will never learn to walk, talk, or eat. We are told to expect damage to occur to her peripheral nerves, leading to loss of sensation and wasting away of the muscles in her legs before the age of 5, as well as a degree of intellectual disability and global developmental delay. So far, she has also been diagnosed with spastic cerebral palsy, and a brain malformation termed ‘Dysgenesis of the Corpus Callosum.’

Ever since her diagnosis of silent aspiration, she has had many types of feeding tubes — including an O-G tube, N-G tube, G-tube, N-J tube, and she now has a G-J tube. She cannot tolerate feeds solely through the G-tube, so she receives formula through the J-tube and medicine through the G-tube. She takes medication daily for GI bleeds, severe reflux, nausea, and spasticity.
Since she was released from the NICU, she has returned as an inpatient to the hospital twelve times. But we are hoping our frequent hospital stays decrease as she gets older. Currently, we receive many types of developmental services for her developmental delays — including physical therapy, occupational therapy, oral therapy, vision therapy, and speech therapy. She also wears ankle-foot orthotics to help correct her clubfeet.
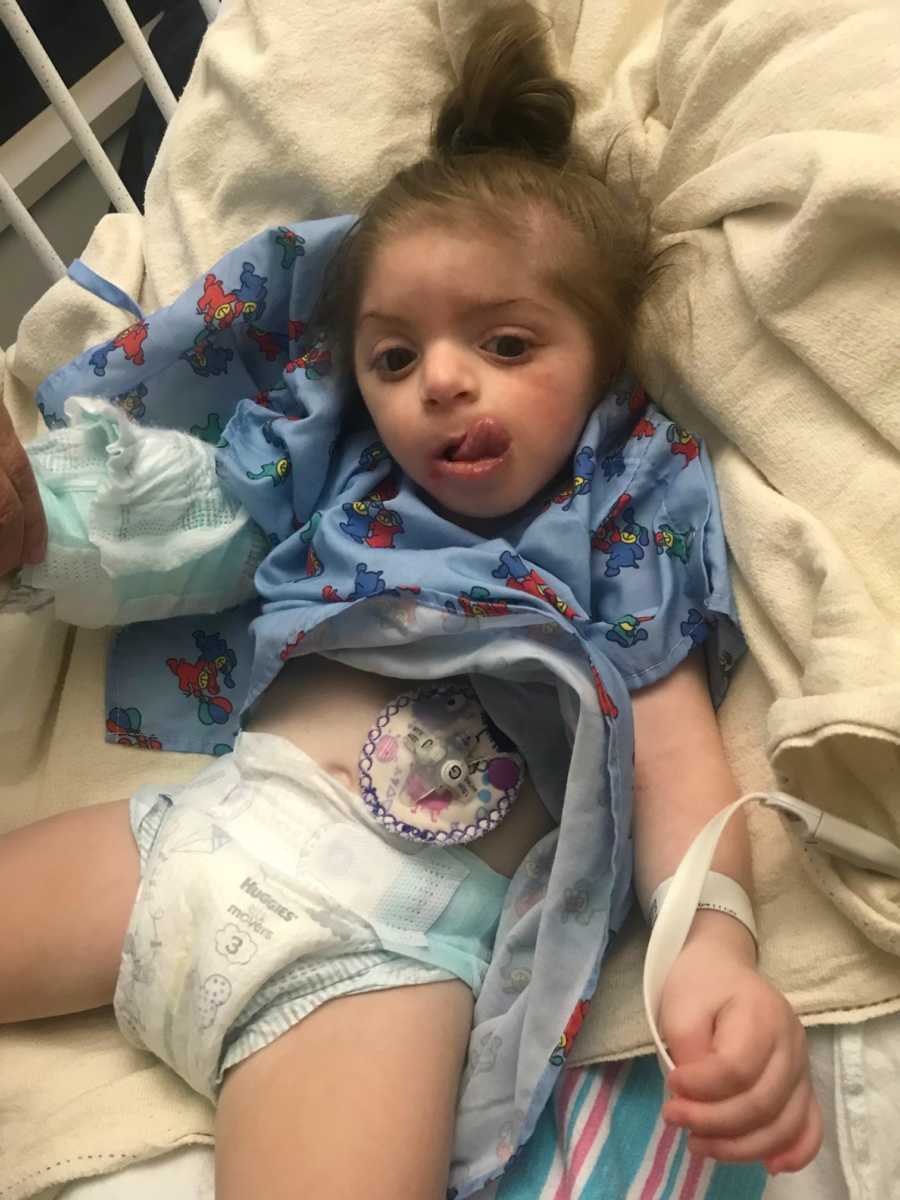
Aside from the mental stress, her rare disease has impacted our family in the sense we do not live the typical life. Our days and weeks are based around doctor’s appointments and therapy sessions. Her frequent vomiting and feeding intolerance issues make it difficult for us to travel places with her. Additionally, it is hard to find babysitters or ask family members to watch her, because many are not comfortable using her feeding tubes.
I am a full-time stay-at-home mom right now, to take care of her until she is old enough to attend a special needs school. This also impacts our family, because I am not able to work or bring in any income. All her specialists are located an hour and a half from where we live. So, we usually must travel at least once a week for appointments, which is mentally and financially taxing on us as well. To cope with the stress, I meditate, run, and workout. I think it is important as an extra needs parent, to find something you do for yourself, and make time out of each day to do it.

After Joplyn’s diagnosis, it was recommended my husband and I also get our genetic tests done, to determine if her genetic abnormality came from one of us or just randomly happened. It turns out, my husband has a genetic abnormality with two of his chromosomes. The tip of one of his copies of chromosome 17, and the tip of one of his copies of chromosome 14, both broke off and switched places with each other. He is not affected because he still has the normal number of genes he should have in his body; they are just switched around.
With Joplyn, she inherited one of my normal copies of chromosome 17, my husband’s only normal copy of chromosome 17, one of my normal copies of chromosome 14, and my husband’s abnormal copy of chromosome 14 with the extra chromosome 17 material at the tip, giving her the extra genes that cause her genetic duplication. Due to my husband’s genetic abnormality, we have a higher risk of having more affected children.
According to the report from our geneticist, ‘the risk for miscarriage, given a recognized pregnancy, is 32%. The chance a live born child would have an unbalanced translocation is 12.5-20%.’ In other words, we had a higher chance of miscarrying our daughter (32%) than bringing her to live birth (12.5-20%). We were very frightened by this news because, not only is Joplyn the only one we know of with her exact chromosome duplication, but we also run the risk of having more affected children with a similar rare disease. Our most realistic option for having another child would be through IVF, which could guarantee a genetically typical child, but is more expensive than we can afford.
Ever since my nephew was born, I knew I wanted to be a mom. After he passed away, I asked him to send me a baby, and genetic condition or not, I got my baby. According to doctors, she was never even supposed to be here. That’s how I know he sent her to me. He protected her like I protected him, and now I’m a mom and she’s my miracle. Even if we are never able to have a typical child, I don’t feel like we’ve missed out on anything, because I feel lucky to have her.

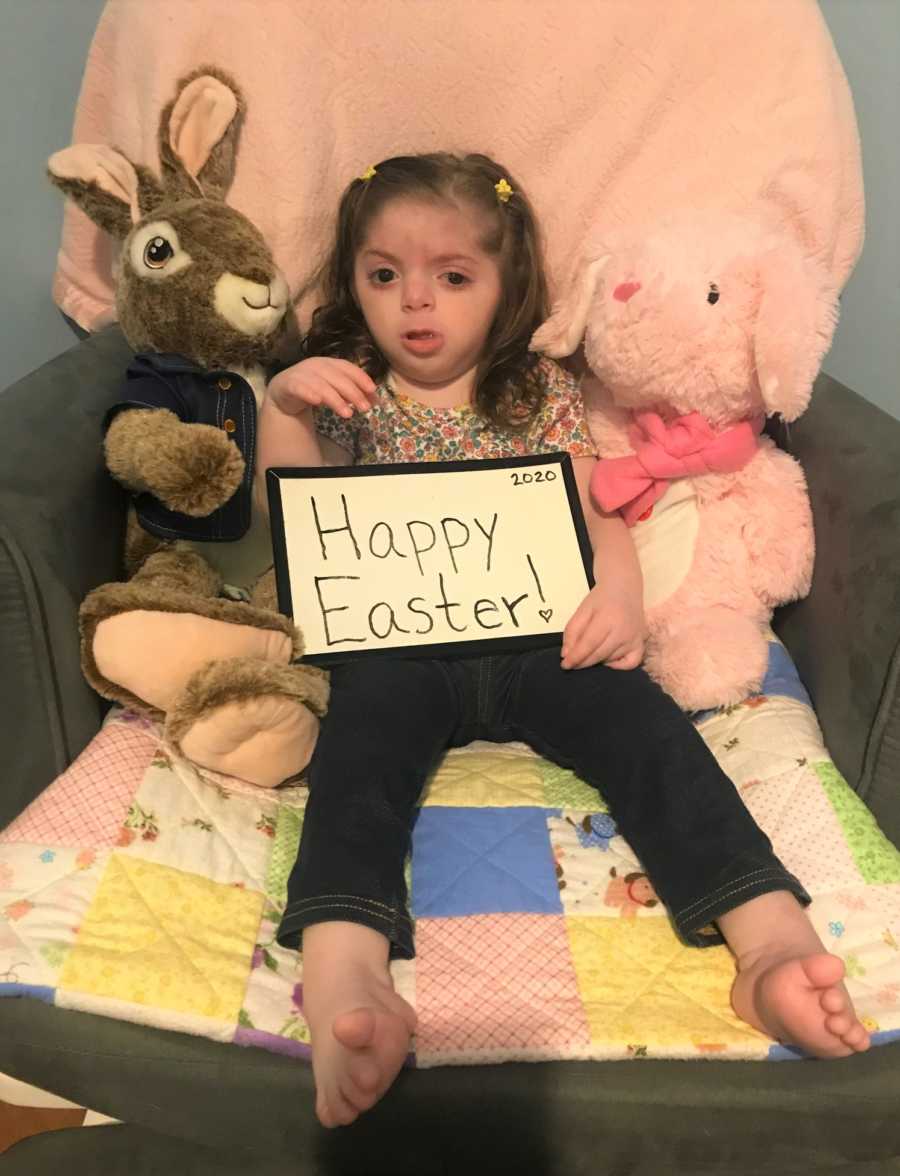
As a woman, sure there are things I wish I could have experienced: a normal labor and delivery, breastfeeding, going home together from the hospital, playing with toys, solid foods, crawling, walking, talking. There are so many things that haven’t happened yet, or may not ever happen. But it’s OK. I understand and have accepted this is the path we are meant to walk. We are people with a lot of love to give, and not every special needs family can give unconditional love and deal with overwhelming stress at the same time. It tears most families apart, but it has made our family stronger.
We overcome challenges as a team, with a large tribe of people by our side, who love and support us through every step of this journey. And we couldn’t do this without them. To other special needs parents I would say, keep your head up, breathe, and focus on all the blessings you have. Find your tribe. I know this life seems crazy and impossible at times, but I promise it is worth it all. Now that I have my daughter, I couldn’t imagine my life without her.”


This story was submitted to Love What Matters by Heather Norris of Stockton, CA. You can follow their journey on Instagram and Facebook. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories.
Read more stories like this:
Provide beauty and strength for others. SHARE this story on Facebook with your friends and family.

