Disclaimer: This story includes descriptions of mental illness that may be triggering to some.
“I used to be ashamed to have bipolar disorder. In my mind, it was almost an expletive, used to describe people with extreme mood swings, the weather when it shifts suddenly from pleasant to stormy, and, when taken seriously, a mental illness that stamps ‘unstable’ on the bearer. When I was twenty-three, and the psychiatrist I was seeing first did an about-face from major depressive disorder to bipolar II (the form of bipolar disorder with less dangerous bouts of mania, called ‘hypomania’), I was both curious and ashamed.
Everybody knows someone who has depression, but the only person I had ever even been familiar with who had bipolar disorder was the daughter of an acquaintance of my parents. I got the impression that bipolar was something to be sad about. During that insightful doctor’s visit, I evaluated my bouts of depression that kept coming even though I was consistently medicated. I thought through the many activities I excelled at, the concern of professors or clergy who said I was taking on too much. Could it be? Could I be bipolar? If I evaluate my life honestly, I feel like I live within the eye of a hurricane, a paradox of the mentally ill. Today, at 37 years old, I am firmly convinced I do have bipolar disorder, and actually, I have the more dangerous kind, bipolar I.
I had always told people it started when I was 17 when I suddenly stopped feeling like part of the universe. I felt flat and ‘other’ and very much like Thomas Anderson in the Matrix movies when he had a strong feeling that reality was false. I used to secretly hit my hands on the edges of tables and walls just to test whether I was really here. At that point, my parents took me to a psychiatrist, and the pastor at my church tried patiently to understand the nonsense I was saying and to draw me closer to God. That was when I first started antidepressants with minimal success.
Although that has struck me as the first manifestation of my mental illness, in watching my oldest daughter, Shiloh, I recall bits and pieces of an extremely anxious childhood. Sleep has been the great demon of my life, and it started young. I used to obsessively try to force myself asleep before my Little Mermaid tape ran out, feeling the tightness of anxiety in my chest as I imagined strangers sneaking into my window and killing me. Every night, I compulsively prayed a list of scary things I was desperate not to dream about, and if I messed up the order, I had to start again.

I excelled at school, but if I didn’t receive perfect scores, I felt defeated and sure I had disappointed my parents. As I grew, my fears of not having perfect marks became more crystallized, focusing on how I would never get into the college of my dreams if I didn’t get that prized A-plus. I have a vivid memory of sitting alone in my geometry classroom, crying silently while trying to finish an exam over my lunch break, my teacher reminding me it was ‘just a test.’
Because I was a gifted student, I went into a program called the International Baccalaureate program (or I.B.) at a local public school. Academics had always been my wheelhouse, so I skated through the curriculum without much anxiety. Instead, what has now been identified as a formal anxiety disorder shifted to sports. I was a decent but not especially talented soccer player, but when I was promoted to varsity, I started to dread games, putting artificial pressure on my performance.
I started running track, and my coaches soon discovered that combining my speed and natural ability with the hurdles made me unstoppable. Looking back, I wish that time hadn’t been so colored by anxiety because I should have loved winning so often. Instead, I put the responsibility of winning unnecessarily on my shoulders. As soon as one meet was over, I relaxed until the next morning, then obsessively counted down the days until the next.

Thankfully, having strong friendships kept my head above the water of my anxiety, and later, depression. My core group of friends, and especially my best friend, Carly, gave me some incredible memories of carefree fun. I was able to shed the anxiety of school and sports when we were being ridiculous in our teenage silliness. It was really the first sign that relationships would anchor me going forward. At 17, feeling disassociated from reality, I timidly began to talk to my close friends about seeing a doctor. One good friend, Katharine, encouraged me, and we talked a lot about feeling sad.
Having someone else say, ‘Me too!’ was deeply therapeutic. On top of those friendships, I was quite tapped into my church’s youth group; and my faith, which was strong albeit youthfully naive, kept me buoyed above my budding depression. I had an especially close friendship with Kelsey, who was two years younger than me but wise beyond her years and one of the best listeners I’ve ever met. She was an emotional foothold throughout my twenties, and we served as maids/matrons of honor in each other’s weddings.
I went off to undergrad in San Antonio and began to have periodic, serious depressive episodes. I would suddenly have graphic images of dying or of seriously self-injuring myself. I sobbed in the dorm shower, leaving my suitemates and good friends, Kat and Katie, deeply concerned. I leaned on them through the ups and downs of depression, which, strangely, did not let up despite a multitude of drug trials over that year. Once again, friendship kept me from getting lost in deep despondency.

The following year, my depression became too much to handle, and I requested a leave of absence from the university, which, given my pride and my strong academic abilities, was pretty shameful in my eyes. When I returned the following semester, my incredible roommate, Susan, listened to me try to explain my nonsensical feelings of depression every night, helping me stabilize my emotions enough to feel just a little bit okay before I went to bed and woke up to start the whole cycle of sadness over again.
I had a good year and a half after that: my incredible and kind friends helped me enjoy college. As a senior, I approached my psychiatrist, who, listening to me explain my desire to come off medication, helped me wean off the antidepressants I was taking. Within 4 months, I was suicidal. I spent graduation with tears streaming down my face and was crying in every single joyful picture of me and my friends. I dejectedly went home for a month before I was scheduled to start my Master of Arts in Teaching. I had a minor psychotic episode and was put on an antipsychotic as well as beginning my antidepressant regime again.

To my parents, it was clear I was deeply depressed, but they, and my counselor, thought having some structure and support while I engaged in something I loved (learning to be a teacher) would be good for me. A few weeks into the program, I found myself sitting anxiously on my bed, and suddenly, impulsively, I grabbed a bottle of antipsychotics sitting on my nightstand, swallowed them one-by-one, and topped it off with a handful of Tylenol. It was a bizarre and obviously tragic choice, and I couldn’t even explain why I did it until I was appropriately diagnosed with bipolar II.
This diagnosis is one of the most dangerous ones for young people because it manifests with periods of major depression then periods of high but not worrisome levels of energy and accomplishment. Because people with bipolar II are often misdiagnosed with depression, they are put on antidepressants without a mood stabilizer. Then, when they go through a depressive episode, the lack of mood stability makes them very impulsive. Many misdiagnosed young people with bipolar II commit suicide without actually wanting to die. That was me.
After an ICU stay, I went back to be with my parents. My doctor prescribed a high dose of antipsychotics and antidepressants (I still was not properly diagnosed), and I stabilized. Though I was ashamed everyone knew I attempted suicide, I was too proud to walk away from my commitment to the MAT program, so, once I was ‘back to myself,’ I started working at home, then returned to graduate. A dear colleague said she cried when I was hooded, thinking, ‘She actually did it.’ It was a profoundly humiliating experience, but I was proud of my perseverance.

I then tried to be a teacher on a military base, but still, on the wrong medications, I continued to cycle through bouts of high mood and depression. I confided in a fellow teacher that I had attempted suicide, and our relationship immediately changed. She became hyper-vigilant about my behavior. One day, when I called her to ask for help with the computers, she could hear me choking up with frustration. She began what felt like a campaign to discredit me. Ultimately, the principal offered me a choice between probation and resignation, and despondently, I resigned.
Amidst all this, I was working at a camp for children with special needs. My first camper, Bertha, went on to be a client of mine as I began a string of long-term personal attendant positions, and she, and the other women I worked with, taught me about disabilities, inclusion, gratefulness for the gifts I do have. In addition to Bertha, I met my husband, Edward, and my best friend, Mary, at Camp C.A.M.P., as well as many other lifelong friends. My relationships with Mary and Edward have probably been those that have kept me from losing my footing with my mental illness. With their empathetic support and my parents’ unconditional love and encouragement, I have bounced back from each depressive, and later, manic and psychotic, episode.

In late 2015, I became pregnant with my daughter, Shiloh. Edward and I prepped for a bout of postpartum depression (PPD), as it seemed likely given my history of depressive episodes. I took several medications deemed as safe as possible for fetal development. I spoke frequently with the psychiatric nurse handling my mental healthcare. While she knew a lot about PPD, she had no training in the more likely postpartum outcome for a bipolar woman: postpartum psychosis (PPP). When you hear about mothers going crazy and killing their infants or themselves, it is probably PPP they were experiencing.
48 hours before I gave birth to Shiloh, I began having painful contractions. We went to labor and delivery 3 times before they admitted me. I hadn’t slept the whole time. I had a safe and easy birth, and we were transferred to recovery. As soon as Shiloh was delivered, I felt the natural high that mothers who have unmedicated births describe, despite my having an epidural. I felt like a superhero, not at all tired, and so proud of the amazing feat I just accomplished. I still did not sleep. We went home, and for 3 more nights, I continued not to sleep, waking my newborn to breastfeed her when she didn’t want it, watching her, and obsessively singing her lullabies.
On the sixth night of not sleeping a wink, I sat in the living room, rocking back and forth in a recliner with Shiloh on my breast. Suddenly, I began to hallucinate. I felt my whole body buzzing, and my brain began a delusion that my milk was causing Shiloh to grow at an enormous pace. As she grew, my body shriveled as I gave up my life force to her. I was convinced I was having an out-of-body experience, where, in the real world, I was lying in a hospital, near death in a coma, while mentally, I was trapped in my mind in my living room. I screamed for my husband. He ran to the living room, and I shoved Shiloh into his arms before violently jumping up and down and screaming, ‘I’m not going to die!’ over and over.

The next morning, Eddie supported me as I, half-crazy, admitted myself to a psychiatric facility. Then, he went back to our newborn by himself, without paternity leave. In the hospital, the medical staff made some serious mistakes, reducing my antipsychotic and increasing my antidepressant. The out-of-control levels of serotonin and dopamine both from my PPP and the changes in my medication propelled me into a nightmare world. I was mostly restricted to my room with a one-on-one staff member because I was volatile, screaming, and saying nonsensical things to other patients.
Most of the day, I lay in a bed, watched closely while my brain swam with delusions that I was in Hell, that I had killed Shiloh, that I was the victim of a school shooting and then the shooter, and that various family members had died or were ghosts. My incredible husband worked, took care of Shiloh, and still brought her to see me every day. I was hardly able to change her diaper, let alone hold her, but they kept up the routine to help me try to bond with her. After an incredibly traumatic 29 days, I was downgraded to a partial hospital program for 10 additional days, and then I was back to my home, where my role was suddenly the mother of a newborn.
Over the first 9 months of Shiloh’s life, I struggled hard with motherhood. I missed the precious newborn period, so the deep connection forged between mother and baby through hormones and closeness and breastfeeding was lost. I felt like a terrible mother, Shiloh didn’t seem to take to me, and I hardly knew what to do with myself when we were alone together. I’m pretty sure I developed postpartum depression during this time, but I was on such a heavy-hitting cocktail of mood stabilizers and antipsychotics that my new psychiatrist was not willing to treat me for depression. I went back to work shortly after I came home, but I felt like I was drowning.

Thankfully, Edward supported my dream to move to where my parents lived, a possibility that gave me hope. I found a job as a clinical supervisor, achieved my state license quickly, and worked for almost two years. Over that time, we began co-sleeping with Shiloh, mostly out of desperation to sleep, which helped me start to bond with her. Things were really looking up.
Unfortunately, it was not meant to last. After being forced up against a deadline on a project, I had a few nights of insomnia. I panicked and asked Edward to take me to a local psychiatric hospital so I could stabilize quickly. I was concerned about driving my daughter in my car when I wasn’t sleeping and about making irresponsible decisions at my job. I work with autistic children so I was desperate not to make a misstep that would harm them, my reputation, or my company. I was diagnosed with true mania (rather than hypomania), due to tactile, auditory, and visual hallucinations and a wide variety of delusions.
When I was released, it was difficult to get the paperwork for FMLA for several weeks, and, unfortunately, I sent an unprofessional email while still unwell. Those occurrences signed my fate, and I was fired. During that time, I leaned on my good friend Courteney, a fellow clinical supervisor. She came to visit me at the height of my mania and listened to me ramble on about how the Matrix was real and the Purge (from the movie) was actively going on in our neighborhood. She even smudged my house with sage for me, an act of helping me feel safe. Once again, a relationship helped me to keep going.
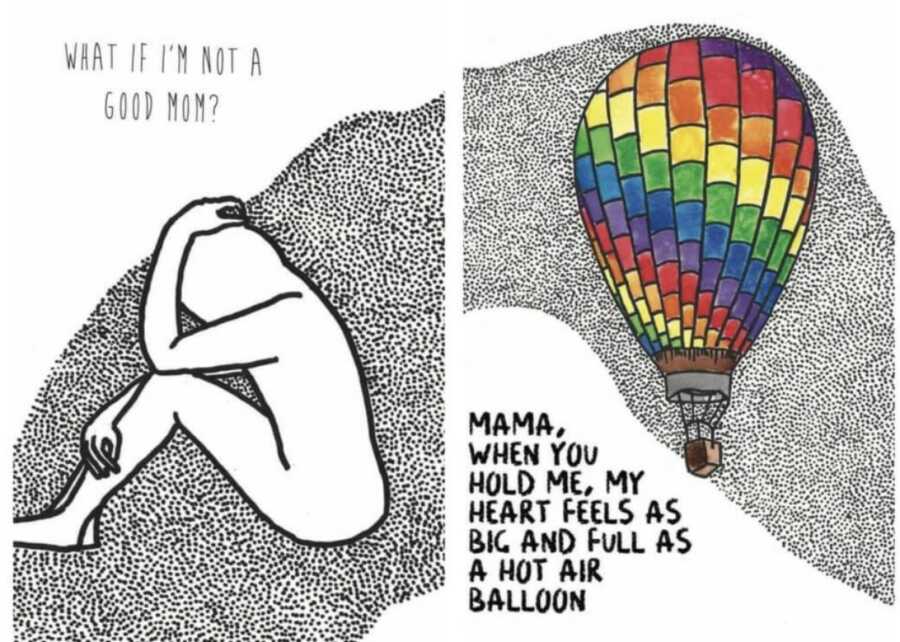
After stabilizing again, I wrote and illustrated a postpartum picture book for new mothers called, ‘You’re Doing a Great Job, Mama’ that juxtaposes new mothers’ deep feelings of shame and inadequacy with babies’ profound and unconditional love for their mamas. While not a commercial success, it gave me a sense of peace about my experience with Shiloh and the ultimate achievement of a strong mother/child bond. I also blogged openly about my, and other people’s, mental illness. Processing my painful experiences and educating others about different variations in the spectrum of mental health was deeply validating. I felt I was getting over my experience of PPP as I began gaining more comfort talking about the experience.
For a few years, I was terrified I would accidentally get pregnant and get lost in the nightmare of PPP again. It was too risky to experience another episode and potentially lose my ability to be a mother to Shiloh. I swore I would not have more kids, and though we both longed for Shiloh to have a sibling, it seemed she would be an only child. Then, when Shiloh was four, Mary got pregnant with her first child, a girl! The excitement of her pregnancy changed something in me, and I started asking my doctors how risky it would be to try again. My psychiatrist said we could likely avoid another episode if I was on the proper meds and protected my sleep after birth. I finally brought it up to my husband, and 7 months later, I was pregnant with another little girl.
19 weeks into my pregnancy, I switched OBs: my new OB saw I was deeply traumatized by my PPP episode and later said she could see and hear the depth of PTSD when I explained my situation. She and my psychiatrist met with me frequently, making titrations in my medications, checking on the development of the baby, and reassuring me I would be ‘wrapped in a cocoon of support’ after I gave birth. My parents, friends, husband, and I prepared for the worst while hoping for the best. We decided Edward would take night duties for the first 2-3 weeks when the risk of PPP would be greatest. We scheduled multiple appointments for those first weeks postpartum, and I was required to meet with the psychiatric team before I left the hospital.

My second daughter’s birth was an induction because, at 36, I was an ‘older’ mother. Vida was born around 4 p.m., and after the exhaustion of the birth, I slept 4 hours the first night. I breathed a sigh of relief: I had slept! Maybe I would escape another episode! On the second day, I was hopeful and excited about going home but needed to spend another night in the hospital to be monitored and perhaps medicated. As Edward nodded off, insomnia crept in like some nefarious creature and curled up in my brain as I tried desperately to sleep. I had a panic attack in my hospital bed, and a nice nurse gave me a dose of Ambien, so I slept another 3-4 hours. We were released to spend our first night at home with Vida.
By that evening, I should have been exhausted. At first, I felt a little tired and thought I could sleep on just my normal medications. But the delusional thoughts began as I lay in the dark with my family. I thought God was singing in my brain and felt a bit delirious. I told Edward I couldn’t fall asleep because Vida’s crying was keeping me up, retreated to Shiloh’s room, and tried to fall asleep. Almost immediately, I had an intense panic attack. For 4 hours, I tried to control my breathing, with the heavy press of anxiety that sufferers of panic attacks feel in their chest. Finally, I woke Edward up and told him I thought it was starting again. He immediately emailed my psychiatrist, even though it was 4 a.m. Two hours later, she called us back and suggested it was probably some normal, postpartum anxiety and PTSD from my first episode.

My psychiatrist prescribed an incredibly powerful dose of an antipsychotic and 3 anti-anxiety meds to make me sleep and prevent panic attacks. I had desperately wanted to breastfeed Vida because that opportunity was lost with Shiloh, but while I was on Valium, it wasn’t safe. However, after I was successful at titrating off the Valium, breastfeeding would again be a possibility. Those early days of panic attacks transformed into a relatively moderate manic episode. I was irritable, sometimes verbally aggressive with loved ones, and I spent far too much money on items for the family. It was frustrating for my loved ones, but they marched alongside me, holding me up and allowing me to bond with Vida. They knew how much I grieved the loss of my early days with Shiloh, so they did everything they could to give me the gift of a healthy newborn period.
As I stabilized, I realized how important preparation and support were in keeping me safe from another PPP episode. Without knowing bipolar women have an almost 50% chance of going through a psychotic episode in the perinatal period, I wouldn’t have prepared a lifeline with my psychiatrist and wouldn’t have known how critical my sleep would be. Without a trauma-informed OB, I wouldn’t have been treated with gentle compassion while pregnant, assured that I would be safe and supported, and monitored closely while in the hospital. My traumatic experience taught me so much about what a woman with my diagnosis needs in her corner to have a safe pregnancy and postpartum period. I knew what needed to happen to protect women like me, and I decided it was my responsibility to spread that knowledge.
I began to post on social media about maternal mental health and reinvented my blog to focus on mental health and motherhood. I reached out to women who experienced a perinatal mood disorder, and they got me tapped into national and international groups focused on education, emotional and physical support, and national policy for new motherhood. With a friend’s help, I created Kindle and print editions of my postpartum book, available at booksellers worldwide.
I am devoted to making sure that other bipolar women won’t give birth without preparing for PPP, that mothers know that it is okay to prioritize their mental health over nursing when struggling and that perinatal mood disorders are a spectrum far wider than just depression. I will not stop talking about my mental illness, learning about the mental illness of others, and educating the public about how mental illness can be managed successfully.
As I said above, I often feel I am in the eye of a hurricane, caught between being able to clearly evaluate and share my own mental illness and the roaring winds of mania or depression. I am committed to being an open book about my mental illness. If just one other person feels less alone, less ashamed, because of reading my writings, then my difficult journey has been worth it. Mental health is a spectrum, and every single person falls somewhere between perfect health and deep illness. Just because you don’t have a diagnosis, it doesn’t mean you don’t deserve to be able to care for your mental health and talk about your feelings, struggles, or fears. The stigma of mental health is a weight hanging on our shoulders that has no reason to be there.
Prioritize your mental health. Learn about mental illness. Get help when you need it. End the stigma. You are worth it.”


This story was submitted to Love What Matters by Dr. Heather K. Gonzales from Phoenix, AZ. You can follow her journey on Instagram, LinkedIn, blog, and her Amazon book. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Do you know someone who could benefit from reading this? SHARE this story on Facebook with family and friends.

