“During the 9 months I was pregnant with my son, I thought I had prepared for everything: the painful birth, the sleepless nights, the difficult postpartum journey, etc. However, I wasn’t prepared for dying during his birth or for the miraculous story of survival that would follow. When I found out I was pregnant with my first child I was ecstatic. My pregnancy was uneventful overall, and I loved pretty much everything about being pregnant. The only issue was I felt like the baby was huge, but I continued to be reassured by my doctors I was measuring right on track.

At 40 weeks and two days, I went into the office and had 2 high blood pressure readings, which meant they had to send me to the hospital. It resolved itself when I arrived there because it was only anxiety related. However, since I was already overdue, they suggested I be induced. I reluctantly agreed, but was very nervous about an induction, especially at 0 cm. After two full days of labor requiring Cervadil, Pitocin, Foley Bulb, and an epidural (thankfully!), I woke up on the third morning at 7 cm and by 12 p.m. I was finally at 10 cm. At around 12:30 p.m. my OBGYN came in to check me and let me know I was 10 centimeters, ‘Ready to push!’ I was definitely nervous about not having enough energy to push after laboring for so long and barely sleeping, but I was so excited to meet my little boy. The doctor left the room and said she would be back shortly to deliver my baby.
I turned to the nurse to tell her I wasn’t feeling well, which she reassured me was normal during the transition stage of labor. As she went to go get me a bag, I continued to say I didn’t feel well, but there was growing concern in my voice. I then started to say something was wrong with my heart. The monitors weren’t registering anything, but I started shouting something was wrong with my heart. The monitors picked it up, started to alert and then I was out. I slumped over in my bed with my eyes open but nothing behind them. My husband started yelling in my face to get me to wake up and then he ran into the hallway shouting for a doctor. At the same time, my nurse hit the code blue alarm, an alarm that very rarely gets used in labor and delivery. People came flooding into the room, pushing my husband, Steve, into the corner. By sheer luck there happened to be a conference full of critical care personnel on the L&D floor that day. The quick (and lifesaving!) decision was made to take me right to the operating room. I was hurriedly disconnected from every wire and IV as they wheeled me down the hall, leaving Steve back in the room. There were nurses and techs in the hallway pointing the way to my OR so the necessary people could get there as quickly as possible.
Once in the OR, CPR was initiated and they began an emergency c-section. The baby was out within 6 minutes of my code, which saved his life. It was a miracle he came out okay and was somehow unaffected by my collapse (side note, I was right, he was 10 lbs. 14 oz). Once the baby was out, the attention turned towards me. I was dying. They successfully resuscitated me after 7 minutes with no pulse, but I arrested again a few minutes later. After the second resuscitation, I began to bleed and A LOT. I went into what is called DIC, which is when your blood no longer clots. They inserted a balloon into my uterus to try to stem the bleeding from that location.
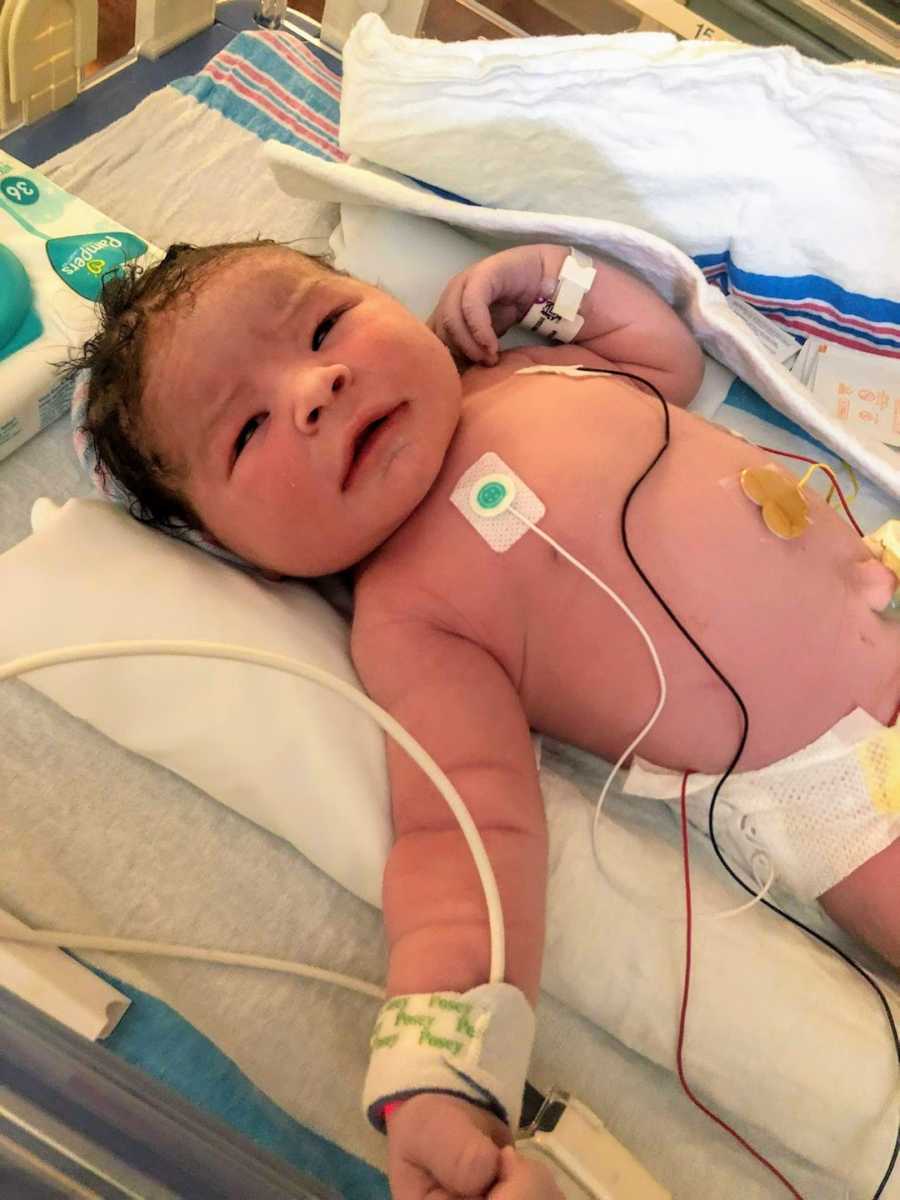
The timing of my collapse was unfortunate, as everyone was either already at the hospital or soon arriving to meet their new grandson/nephew. When I was 10 cm, my husband and I asked my mom to be in the room for the birth, which was not the original plan. She was so excited and went to tell my dad, who was in the waiting room. As she was about the leave the waiting room to walk back to my room, they both heard ‘Rapid Response Room 230.’ They knew it was my room and my mom began to panic, but my dad said it could be anything and not to worry yet. At the same time, my dad thought he heard Steve’s voice yell down the hall for a doctor. Then, ‘Code Blue, Room 230’ rang over the loudspeaker and chaos ensued. My mom tried to step out into the hallway to get to my room just as a herd of medical personnel ran by towards my room, but they wouldn’t let her back. She cried, ‘You don’t understand, that’s my baby girl!’
What felt like an eternity later, they let my mom back into my room where Steve was standing, saying over and over again, ‘Please just save my wife, please just save my wife.’ My dad stayed in the waiting room because he knew my brother- and sister-in-law were about to arrive. Then, my best friend arrived at the hospital, giddy with excitement to meet her new nephew. She spotted my dad in the corner of the waiting room, slumped over and crying. It took her a second to comprehend the emotions didn’t match up with the event or location. My dad went over and hugged her. All he could manage was ‘It’s not okay, it’s not okay, Kayleigh and the baby, we don’t know, we don’t know.’ She crumpled in a chair and started to cry. My dad went to be with my mom and husband. Then, my brother and his wife arrived, just as excited as my best friend had been to meet their new nephew. The scene repeated itself, she had to deliver the news I was not okay. My brother fell down into a chair, devastated.
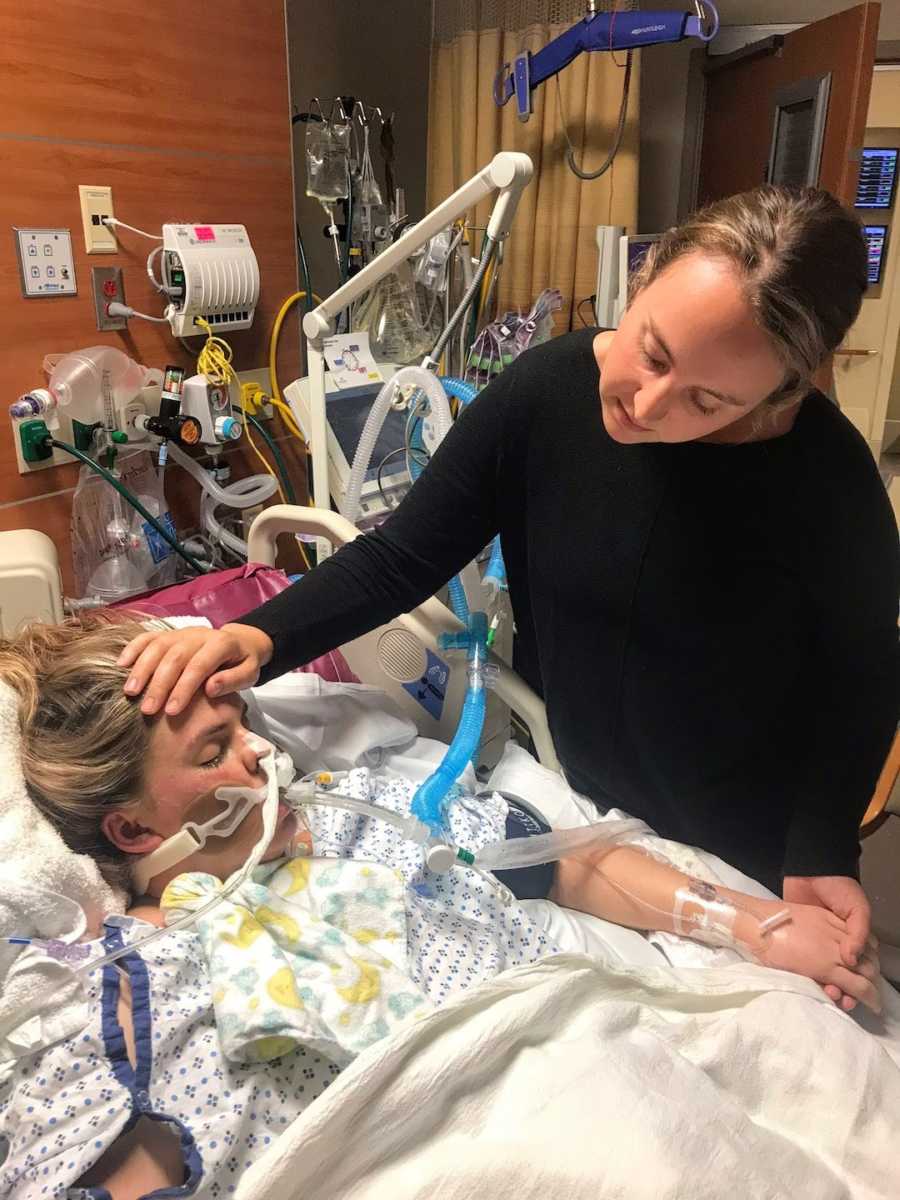
My OB came to update my family. She told them the baby was out and he was completely healthy, even though I had coded while he was still inside. She explained that I, unfortunately, was not okay; I had suffered an Amniotic Fluid Embolism, an extremely rare and often fatal obstetrical complication. Of the 4 million mothers who give birth in the U.S. each year, only 100 will suffer an AFE. She was hopeful they would be able to stabilize me soon.
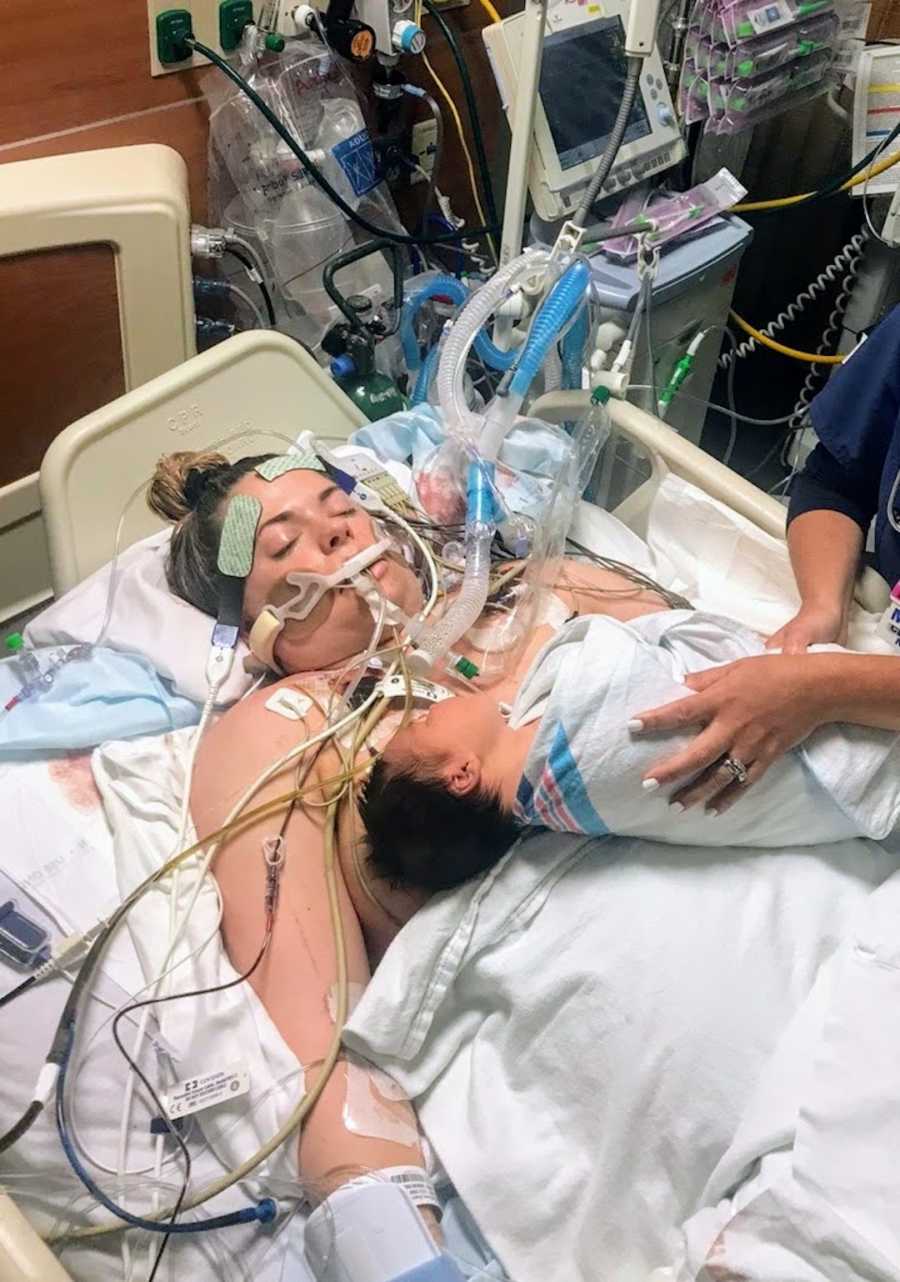
Twenty minutes later things took a turn for the worst. My OB updated it was extremely critical because they could no longer stop the bleeding and asked my family to please pray. At this point my family began to prepare for the worst. They were pretty sure I wasn’t going to make it and they were going to have to say goodbye to me as they met my son for the first time. I was bleeding from everywhere and there was no way to stop it. Massive transfusion protocol had been initiated, but the blood was pouring out as fast as it was going in (I ended up with a total of 143 units of blood product transfused by the end of this ordeal). More than 5 liters of blood were collected through the catheter attached to the balloon that was attempting to stop the bleeding from my uterus. I was also struggling with oxygenation because my heart and lungs weren’t working at full capacity. The decision was made to put me on ECMO, a form of life support.

Because they were unable to stop the bleeding, they were forced to perform an emergency hysterectomy, leaving me with one ovary. They left me partially open because they knew they would have to go back in several more times to clean up my abdomen. I was then prepped to be transferred to another hospital that had the capability to maintain the ECMO circuit.
During these hours of waiting, my family realized Steve needed to go see the baby. He was reluctant to leave the conference room where he could be closest to me, but he knew I’d want him to go see our son. It still breaks my heart to think during his first five hours of life no one from our family was with him. As soon as Steve held him, he broke down crying. The day’s events caught up with him. He was terrified he was going to have to do this alone, without me.

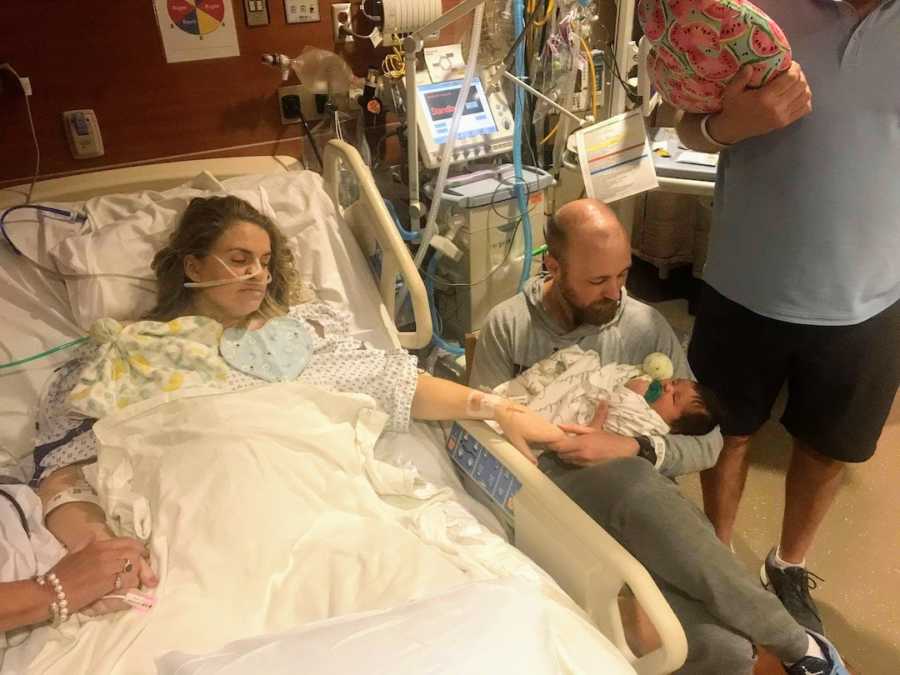
The trauma team updated my family. They still weren’t sure if I would survive this or what my functioning would look like if I did, but they were able to get me stable enough to transfer. They told my family they could see me before I was transferred. After waiting for about an hour while the 20 or so medical professionals readied me to travel, my family saw me for the first time since I had collapsed. It was difficult to see my face because of all the tubes coming from my nose and mouth. Steve was the first one to see me. He walked right up to the gurney, which was surrounded by about 20 nurses and doctors. Steve told me what a good job I had done keeping Cal safe. He let me know how big he was and that he was doing so well up in the NICU. My family told me there wasn’t a dry eye around the gurney when Steve was telling me about Cal. The rest of my family told me how much they loved me and to keep fighting. I was put on the ambulance and transferred to the CTICU at Lankenau Medical Center.
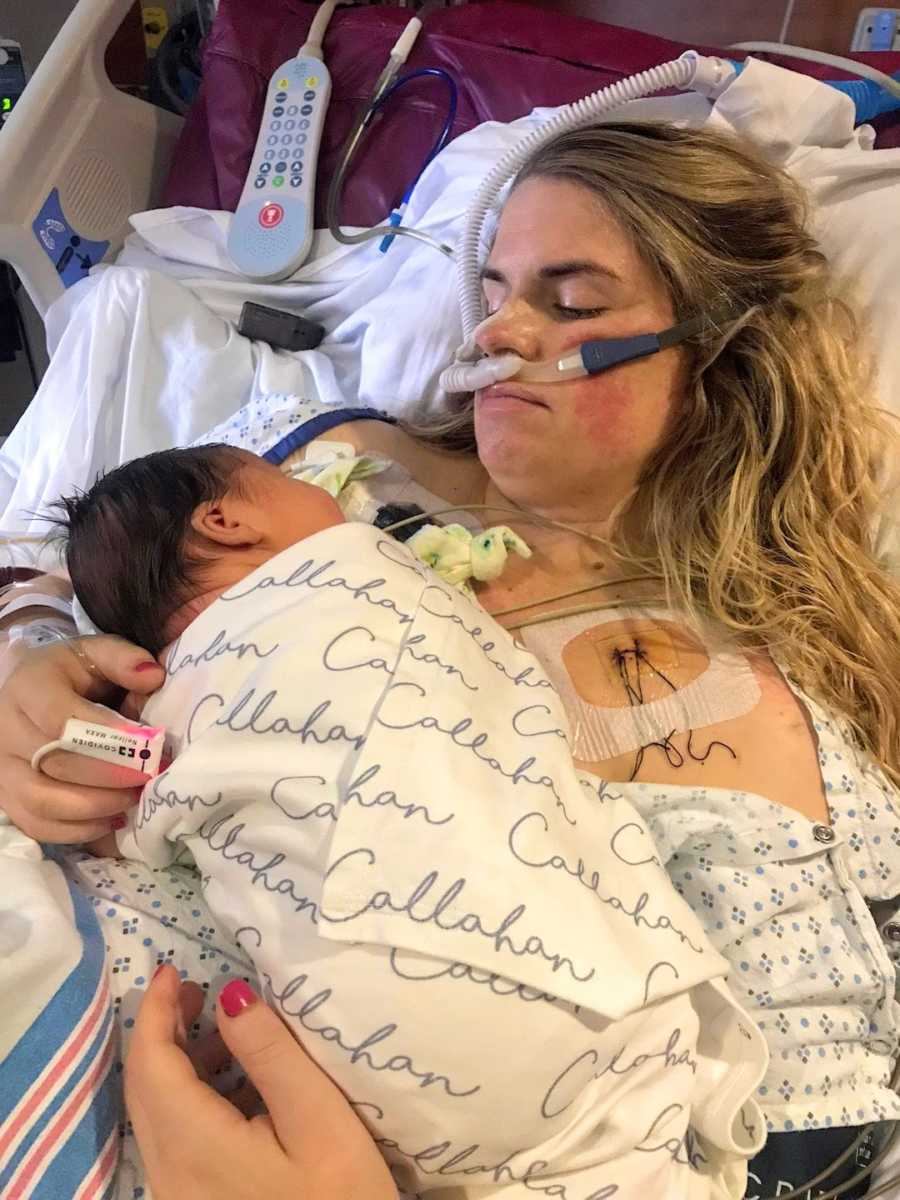
I don’t remember meeting my son for the first time, 5 days after his birth. The first memory I have is from day 6 when my OB and anesthesiologist came to my hospital to explain what happened to me. I remember just nodding my head and taking in each thing they said until they told me that despite their efforts, they still had to perform a hysterectomy. Tears streamed down my face. I would never carry another baby.
Once I was conscious and aware in the ICU, I was absolutely miserable. I wanted out of the hospital as soon as possible. I wasn’t sleeping and my anxiety was sky high, which meant either my mom or husband had to sleep in the hospital with me each night. I was determined to do everything in my power to get home. Over the next week all of my lines were removed. Then, I started standing, transferring to the chair, and then walking. After 14 days in the ICU, I was able to finish my recovery at home.
Now, a little over a year later my son and I are doing well and are so grateful to be alive. There have been many physical and emotional hurdles, but I am recovering each day and in awe I get to be here to watch my son grow up. We are forever grateful to our amazing medial team at Paoli Hospital in PA. Amniotic Fluid Embolism is an extremely rare obstetrical emergency that is unfortunately unpredictable, unpreventable, and often fatal. If you’d like to learn more about AFE please check out afesupport.org.”


This story was submitted to Love What Matters by Kayleigh Summers. You can follow her on Instagram. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Have you or a friend experienced labor complications? Please SHARE on Facebook to make them aware there is a community of support available.

