“’You didn’t lose your baby, but there’s two in there.’ This was what I heard as I laid in a hospital bed thinking I was miscarrying our second child. My husband and I found out we were expecting in December, and by January I was having sharp pains in my abdomen every time I took a deep breath. Thinking the worst, I went to the ER after work on January 16, 2021. I explained I thought I was having a miscarriage or an ectopic pregnancy. I never imagined they would come into the room and tell me it was twins.
My husband had to stay in the car with our 2-year-old; I couldn’t wait to tell him, so I sent a simple text. ‘It’s not bad news.’ Jokingly he replied back saying, ‘Haha, TWINS??’ It was quite the shock when I sent back a simple ‘Yes.’
After that night, we were excited. No one on either side of our families had twins and it was so different and invigorating that we were going to have twins. Our love story has TWINS in it! We started brainstorming names and hoping they would be one of each, a boy and our first girl.
We went to our first prenatal appointment at 6 weeks, and even though the ER had sent over the medical records that stated they were unsure of what type of twins they were, my OBGYN brushed it off and only did a welcome exam with no ultrasound. They then scheduled me for our first ultrasound at 12 weeks. This was gut wrenching to me. Not only were we having twins, but my previous pregnancy had been high risk as well with medical complications such as gestational diabetes, thyroid problems and hypertension. Having to wait 6 more weeks felt like torture.
In addition to my original concerns, I had read online of the different types of twins and learned there were fraternal twins (di/di) who did not share a sac or a placenta, identical twins (mo/di) who shared a placenta but were separated by a membrane, and finally mo/mo twins, who share a placenta and aren’t separated by a membrane. The documents from the ER didn’t say if there was a membrane or not. This led me down a rabbit hole of worry that our OBGYN might miss this and by the time they figured it out, it could be too late and something bad would happen.
I showed up to our 12-week appointment, with my husband, to find out they had cancelled our ultrasound. My knees felt weak. I thought I was going to vomit all over the floor. I looked the receptionist in the eye and told her I would not be leaving without an ultrasound and we were having twins but did not know what type yet. Ironically, they were able to fit us in just fine. During the ultrasound we saw both babies, they looked great! However, the ultrasound tech could not locate the membrane. She called in another tech to do a double look and they thought they saw a glimpse of it but couldn’t be certain. It was still too early to tell.
When I met with the doctor, I was told due to this being a mo/di or mo/mo pregnancy, I had to be referred to a high risk doctor in addition to my normal OBGYN appointments. This was the moment I knew this was going to be a wild ride. Over the course of the next few weeks, we were monitored by both my OBGYN and the high risk doctor. They determined we were carrying mo/di twins, which meant they shared a placenta but were separated by a membrane. This allowed me to breathe a sigh of relief. The membrane ensures the babies won’t get wrapped around each other and cause problems with their umbilical cords.
We were then being monitored at the OBGYN office for fluid for each baby (this is to make sure each baby is getting the proper nutrients). At the high risk doctor’s office, they were monitoring for anatomy changes, such as a bladder disappearing. At 16 weeks we found out they were girls! I was so excited as I had been hoping for a girl this time.
At 18 weeks + 2 days, I went in to see my OBGYN for our routine ultrasound. The mood in the room was quiet and I could tell on the screen something wasn’t right. When the doctor came into the room, she told me she was going to send me to high risk as soon as possible because the babies looked like they were in danger of twin to twin transfusion syndrome.
Twin to twin transfusion syndrome, or TTTS, is where one twin is receiving more blood from the placenta than the other twin. This causes different sizes in the babies as well as the ‘donor’ twin to stop producing amniotic fluid. This can be fatal if not addressed quickly. Fear immediately set in. We had stayed reserved that we could lose one baby at any time during this pregnancy, but at 18 weeks we thought we had cleared the threshold of them both coming home alive.
At 18 weeks and 5 days, we saw the high risk doctor who determined it was more than likely not TTTS, but instead diagnosed Baby B with selective intrauterine growth restriction (SIUGR). SIUGR is when, in this case, one baby is not receiving the proper nutrients from the placenta. This did not mean Baby A was stealing the nutrients, it only meant the placenta was not supplying both babies with enough nutrients. We also learned Baby B had a marginal cord insertion, which meant her umbilical cord was inserted into the side of the placenta instead of the middle like a normal pregnancy.
With the SIUGR diagnosis, we knew there was nothing they could do. There was no surgery that could correct it, there were no options but to wait and hope Baby B made it. The weeks following were spent on the couch trying to comply with the semi-bed rest order I was given. I spent most of the time during the day prodding at my stomach, trying to make both babies move so I knew they were both still alive.

At this point our OBGYN had stopped doing ultrasounds and we rarely were seen at their office. Our high risk doctor was having us in for routine ultrasounds every 2 weeks to check growth on Baby B. At our 20-week anatomy scan, everything looked great! Baby B was measuring about a week behind in growth but there was nothing concerning. I was told to keep doing what I was doing with the semi-bed rest.
Two weeks later, on a Friday, we went in for our 22-week check. This is where things took a turn. Baby B’s bladder was gone. It was not showing on the ultrasound at all. She also barely had any fluid left in her amniotic sac. The doctor was extremely concerned this was in fact TTTS and not just SIUGR. We were immediately referred to Cincinnati Children’s Hospital in Ohio. Our appointment was scheduled for the following Tuesday. We had almost a full day of tests to do there. They did another anatomy scan which took roughly 1.5 hours to complete, we did an Echocardiogram which took 2 hours to complete, and after we were able to speak to the doctor on staff to determine what needed to be done. There are surgeries available to aid in TTTS and separate the blood vessels which in turn stops TTTS from happening. It is a risky surgery, however, and sometimes either one or both twins still pass afterwards.
When we were finally able to speak to the doctor, it was determined we did not need surgery that day and TTTS truly was not present at the time. Baby B’s bladder was able to be seen during their anatomy scan and the Echo showed both babies’ hearts were working 100% normally and there was no trace of extra blood flow in either baby. This was a relief to hear but also scary, because if it wasn’t TTTS, then why did Baby B lose their bladder and have no fluid?
I expressed this concern to the doctor, who tried to explain the best she could there were multiple reasons this could be happening. The one that stood out to me though, was gestational diabetes. I was already at risk of having it again and knowing it has a history of causing excess, or not enough, amniotic fluid drove me to realize. This was part of the issue. Once we returned home from Cincinnati, I drove to Walmart, purchased a glucose meter and test strips, and started testing my blood sugar 4x a day. Sure enough, it was high after my meals and in the morning after I woke up. I immediately changed my diet and controlled my sugar numbers the best I could. Once I was able to see my endocrinologist, I was then placed on insulin to keep everything controlled.
Two weeks later at 24 weeks, we were back in the High risk office. This time we were diagnosed with absent end diastolic flow in Baby B’s umbilical cord. This meant there were moments where there was no blood flow in her umbilical cord. I felt sick hearing this. I was doing everything in my power to keep this baby safe, and alive, and this was another blow to the gut. I could do everything in the world to keep this baby safe and I was still at risk of losing her. This was the moment where I was told I would be hospitalized at some point in my pregnancy.
At 25 weeks, I went in praying for good news, and was told there was no change. Neither good nor bad. I was told to just continue bed rest and take it easy. At 26 weeks and 4 days, I went in for another routine ultrasound only to be told I was being admitted that day. I was scared, I knew this was coming, but I was SCARED. This was the point I knew it was coming to be life or death for this baby. My sweet Baby B was at risk of dying. They gave me my first round of steroids and admitted me to a hospital with a level 4 NICU in case they were delivered prior to 28 weeks.
I stayed in the hospital for 4 days. It was agonizing. I felt like I was in jail. Due to COVID restrictions, I couldn’t leave the room, I couldn’t walk the halls or go to the cafeteria. Even though I had tested negative for COVID, I still had to wear a mask when someone came into my room. Twice a day they performed Non Stress Tests, this monitored the twins’ heart rates and looked for any abnormalities that showed they were struggling. They passed every NST with flying colors. They did a mobile ultrasound once daily to check Baby B’s cord flow, sometimes it showed AEDF and sometimes it was completely normal.
After 4 days, they discharged me to go home and follow up with my high risk doctor two days later. I had one day of freedom before I had another appointment. At 27 weeks and 3 days, I went back to the high risk doctor who performed another ultrasound and readmitted me to their hospital this time. I am fairly certain this was to prevent me from being discharged again. I cried. Having to be hospitalized for an unknown amount of time was scary, it was upsetting; I just missed my home, my husband, my son, my dogs! I missed my shower, my bed, I missed being able to have all my belongings and clothes at my grasp instead of miles away from me. I knew I had to suck it up though, my babies needed me to stay strong and push through the mental roadblock.
I remained hospitalized with multiple NST’s a day and a daily ultrasound at my high risk doctor. The weekend of June 19th and 20th was my only break from ultrasounds; they weren’t open on the weekends to do them, even for inpatients. During an NST, Baby B’s heart rate did not look good and they called in the on-call OBGYN to look. She talked to me and said she wasn’t going to deliver me that day and it looked stable enough to wait through the weekend. I honestly think they were waiting because I had to be at least 28 weeks for my babies to be delivered at this hospital as their NICU is only a level 3.
Monday rolls around and I was 28 weeks and 1 day. They took me up for our daily ultrasound at 7 a.m. Baby B was having reversed blood flow and needed to be delivered ASAP. I had already eaten some of my breakfast, but they said it didn’t matter and they would risk the surgery even though I had food in my system.
My husband had enough time to get there and at 11:10 a.m. and 11:11 a.m. both babies entered the world via emergency C-Section. The C-Section went flawlessly, even though it had been emergent the doctor’s involved were very thorough and it was a calm procedure. The babies were whisked away to the NICU and my husband was allowed to follow. They were both stable and doing well. I was able to see them later that day for the first time.
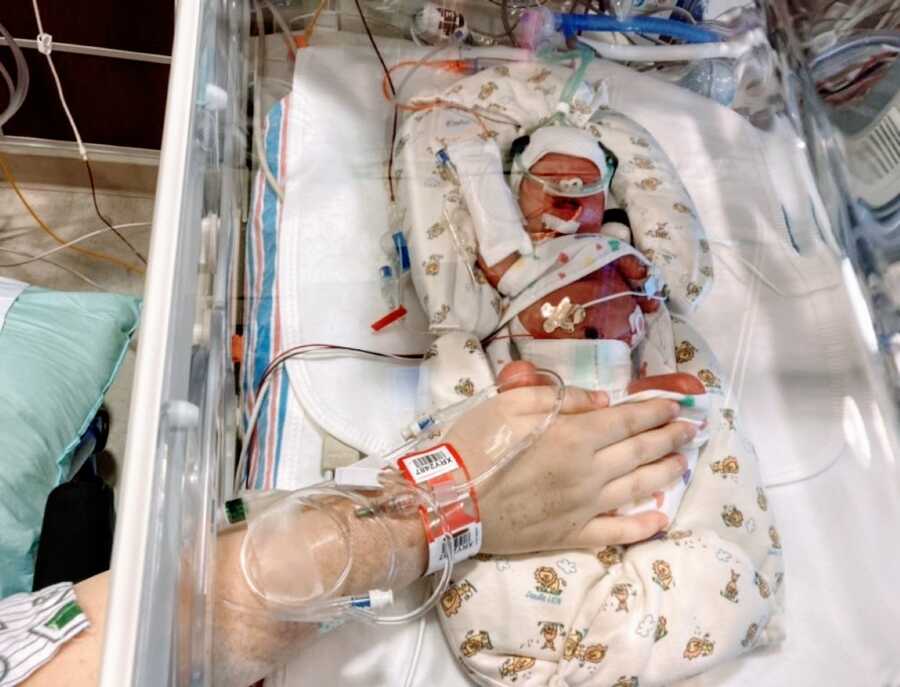
Baby A, Eliza Clarke, was born weighing 2 Pounds 8 Ounces. They had difficulty with her umbilical cord being used for her IV insertion and it ultimately cut off circulation to her foot. It turned shades of purple and black and all that ran through my mind was it would need to be amputated and I would have a one-footed baby. Thankfully they were able to move the IV to her arm, and over the course of a week, her foot healed and turned out just fine. Baby B, Octavia Marie, was born weighing 1 pound 14 ounces. She had no complications when they stabilized her. Unlike Eliza, she was able to have her IV through her umbilical cord without issue.
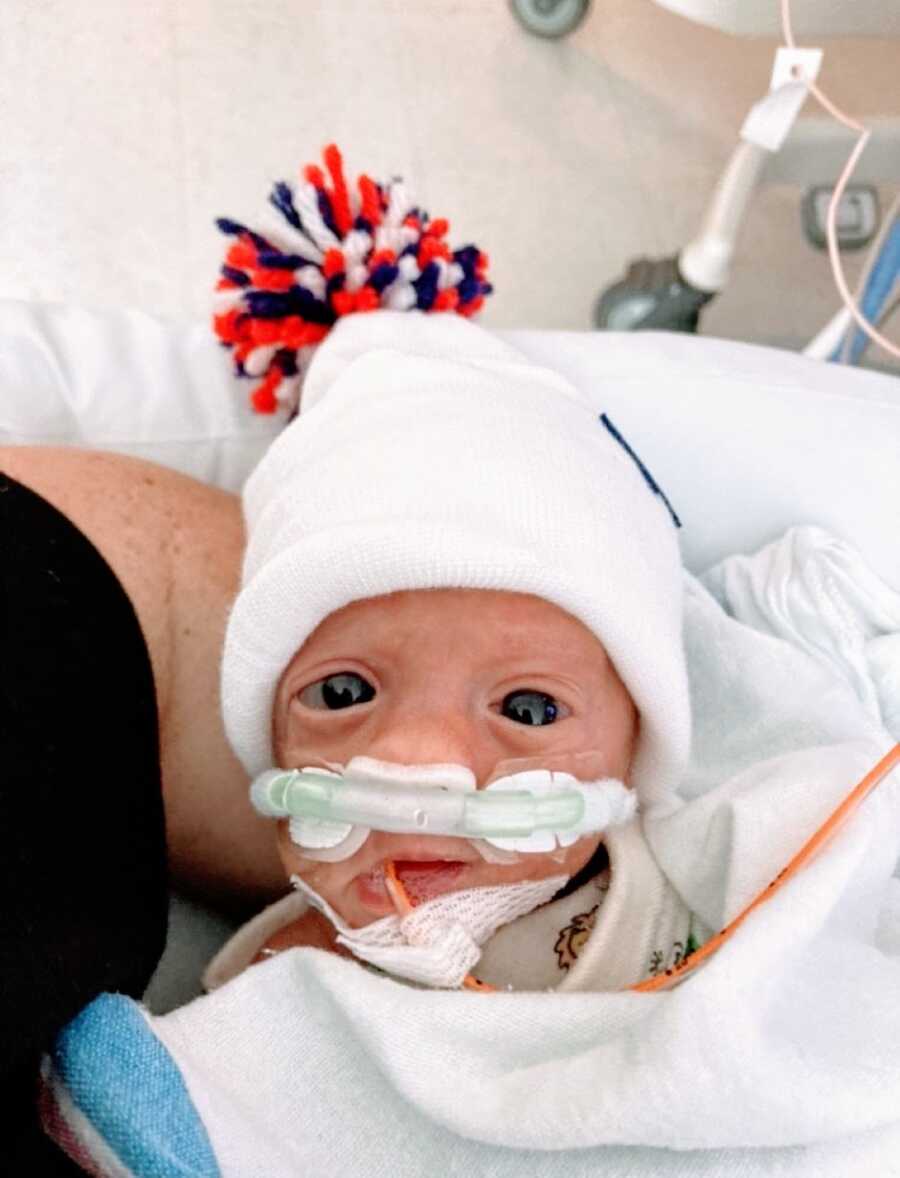
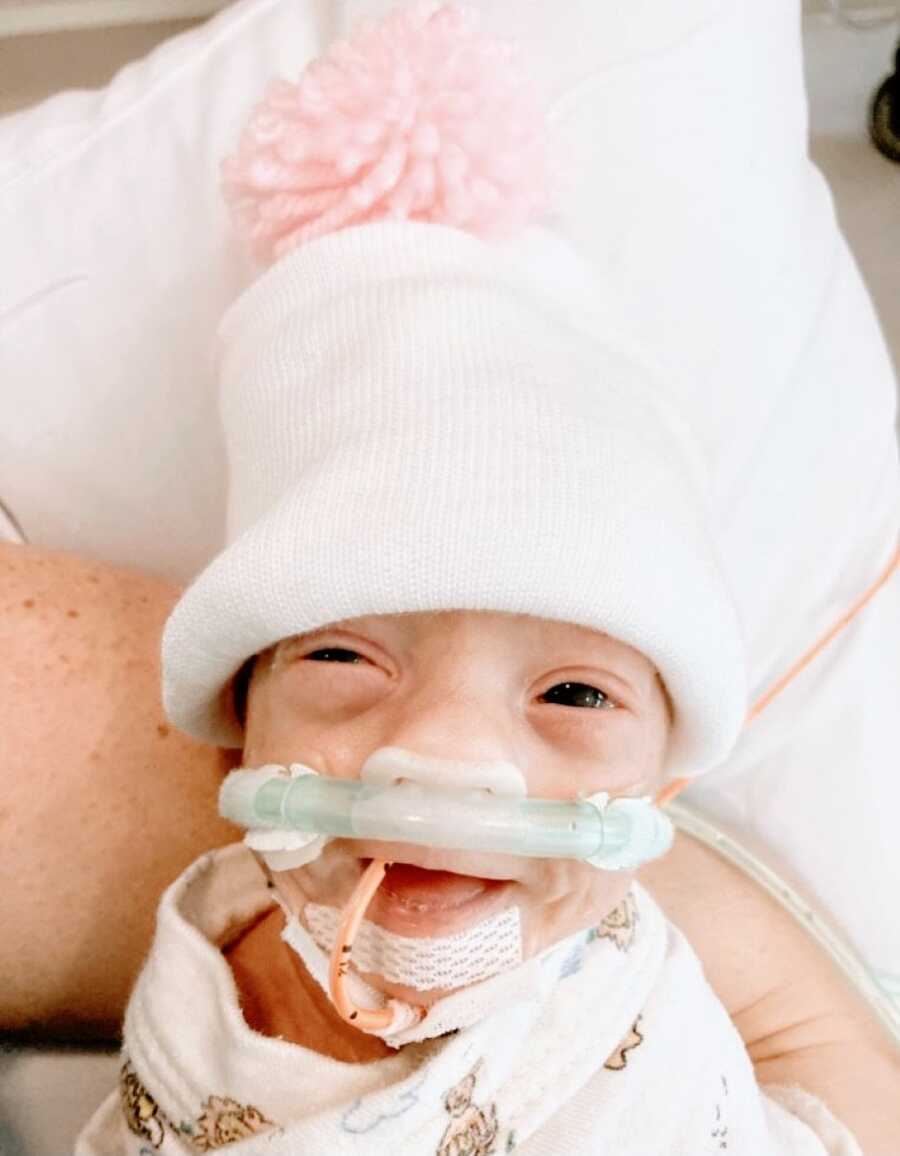
They were both placed on CPAP with room air for oxygen. This meant they needed the pressure from the CPAP machine but no additional oxygen required. After 72 hours, their IV’s were removed and neither one needed an IV again after that. It was daunting having them be born so early and knowing the complications they were at risk of developing. Each day I waited for a phone call from the NICU telling me to come immediately. Thankfully it never happened. We never received a call like that.
I went home after 2 days in the hospital and my husband returned to work. We were going to the NICU every night to see the girls, even if it was only for 15 minutes. They were not stable enough yet to be held, so there wasn’t much we could do while there besides look at them and talk to them. They continued to make great progress, we were clear of infections, never needed to move up on oxygen, and at 12 days old their primary nurse let us hold them for the first time. My husband and I felt like we were on cloud 9. They were so small. It felt so wonderful to finally have our babies on our chests.

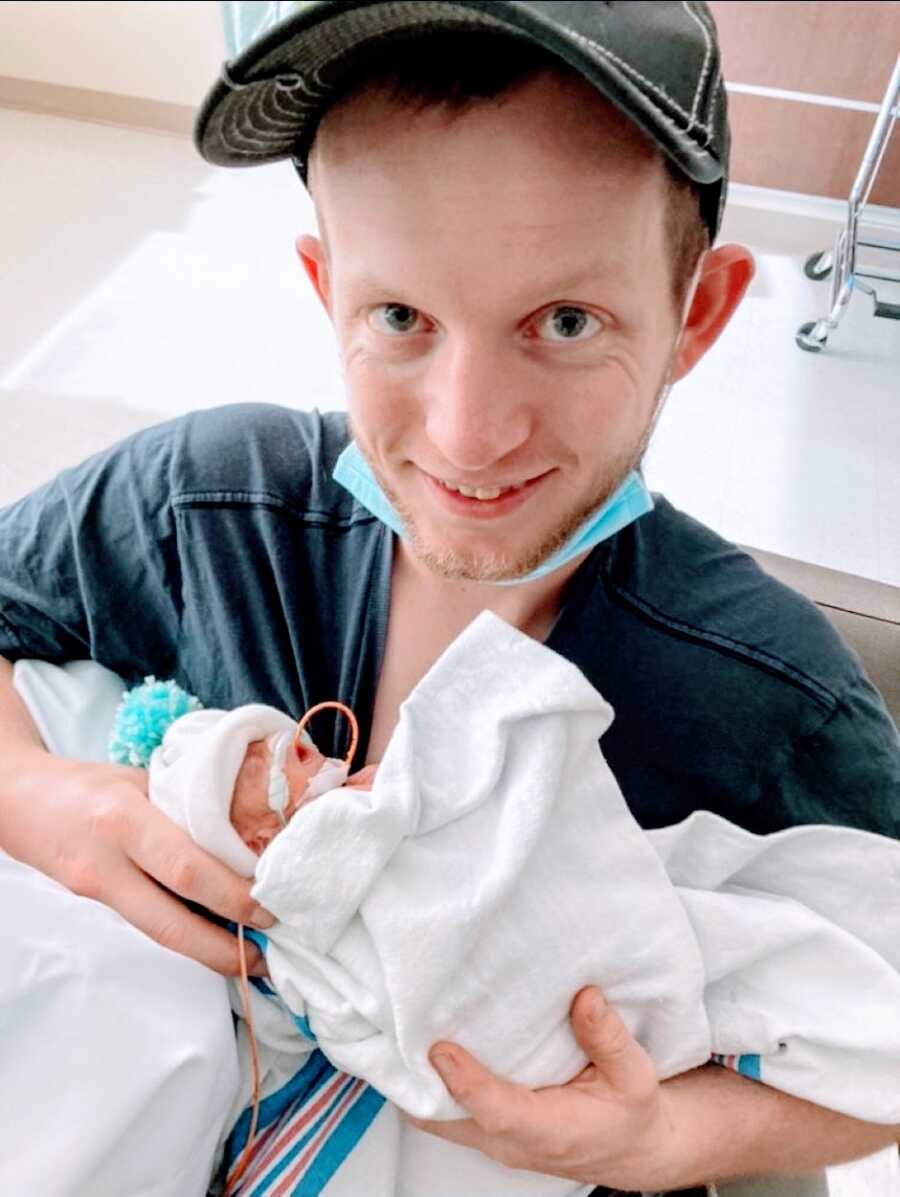
It’s important to say this nurse, along with one other, I give 100% gratitude to. I believe they are the main reason our girls did so well in the NICU. Without these two nurses, I believe our stay would have been drastically different. As our stay continued on, it stayed uneventful. The girls were flying through their NICU stay with no issues popping up at all. There were moments where we thought they would have a set back and then they didn’t. It was a miracle.
After 53 days in the NICU, Eliza Clarke was able to come home. We settled into a routine with Eliza home and it felt like bringing home a normal singleton baby. Things were going great at home! In the NICU, however, things took a turn. Octavia was moved from the twin room to a normal room; this brought us new nurses who did not know her. Our primary nurse wasn’t allowed to be on her service because they had her on the other side of the unit.

The new nurses, while they were wonderful people, did not know Octavia and all her quirks. She’s a very hardheaded and strong-willed baby, so when it came to eating she would often stop, hold her breath and then wait until she was ready to finish her bottle. The nurses were so unfamiliar with her, they kept saying she wasn’t ready and was having too many destats, which were caused by the breath holding. Once again I felt like the world was against me. I KNEW my baby was fine, I knew this was something even a newborn infant not hooked to a monitor would do.
I felt like the world was ending, I just wanted both my babies home. After 59 days, I was exhausted. I walked in on a Friday night to see our night nurse from the night the girls were born and I could have leapt into that woman’s arms. I was so happy to see her. I knew she would get Octavia’s stats back on track for the doctor’s to see she was fine to come home!
I was correct, Octavia returned to finishing her bottles, the nurse was giving her the appropriate amount of breaks she needed to finish and she had stopped her destats on the monitor. The doctor’s were fine with this new trend and 10 Days after Eliza, at 63 days, Octavia Marie was able to come home.

Our pregnancy and NICU stay will forever be engraved in my memory. This was a really testing time of our lives and I am forever in debt to the nurses who advocated for them both in the NICU and ultimately helped them come home so soon. These NICU nurses deserve the world for helping ensure our girls received the proper care. We have had both girls home for a few weeks now and it has been the best time of our lives. We’re tired, but we are so fulfilled and happy.”


This story was submitted to Love What Matters by Caytlin Dyan of Lexington, KY. You can follow her journey on Instagram and TikTok. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this here:
Spread beauty and strength for others. SHARE this story on Facebook with family and friends.

