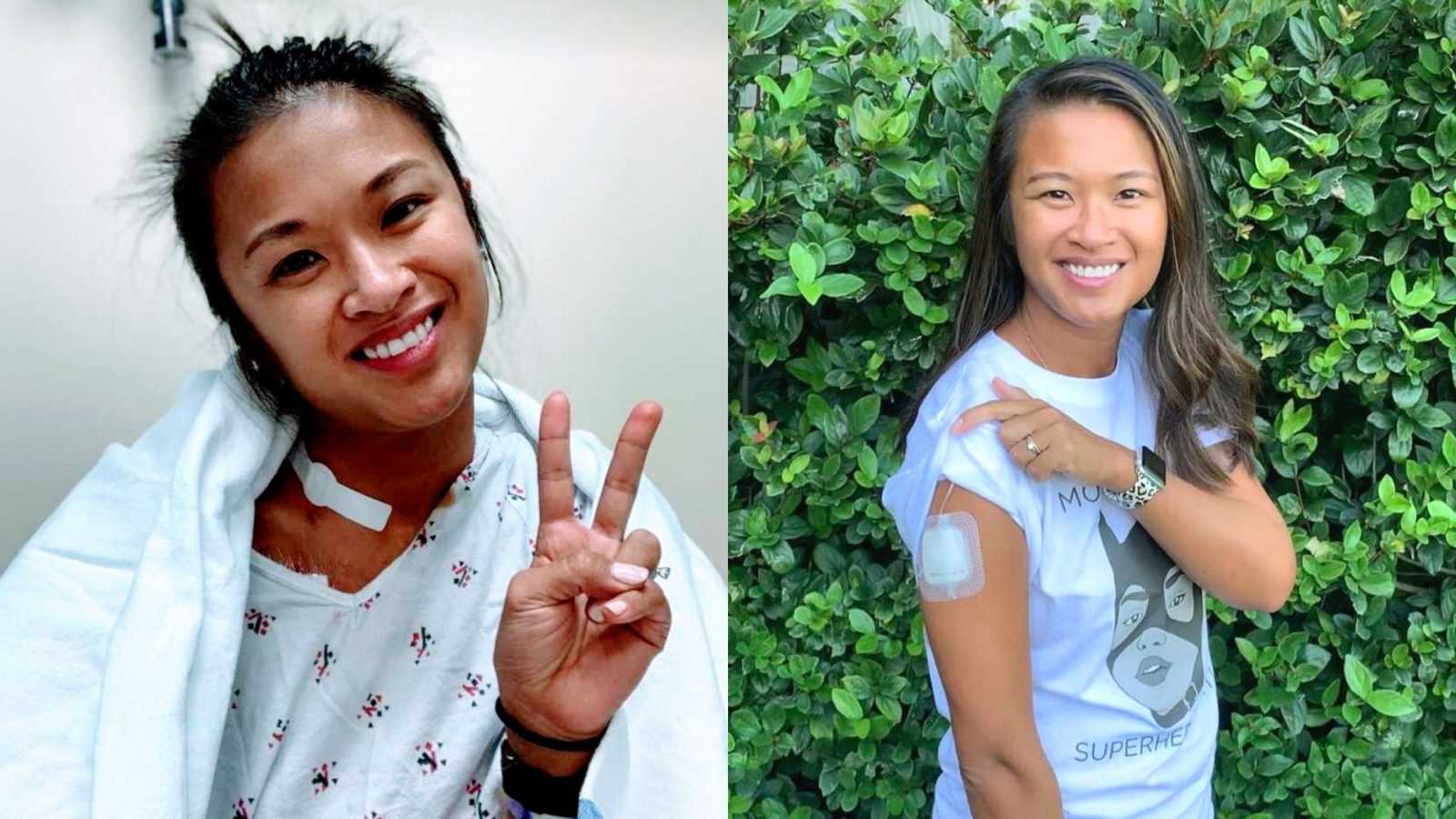“Growing up, I was always a pretty healthy kid. I played soccer year-round in high school, did CrossFit after college, and never had an issue staying in shape. I’ve always hated going to the doctor. I was pretty confident in my immune system and never found myself in any situation where I had to question my well-being.
My husband and I got married in 2015 and the first couple of years were uneventful health-wise. When we found out I was pregnant in January of 2017, it was a complete surprise and we had no idea what to expect. We learned we were pregnant with twin boys. I thought that was going to be the most pivotal moment of my life, and in some ways, it was.

In January 2018, 6 months after we had the boys, we moved from North Carolina to Colorado. Life in Colorado, across the country from our family and friends brought us many challenges. In our first couple of months, things were relatively normal. I had altitude sickness, and after being pregnant and not exercising, I found myself pretty out of shape. I began attributing my shortness of breath with being out of shape and my extreme fatigue to newfound motherhood.
Because of sleep training twins, adjusting to altitude and the lack of maintaining exercise in daily life, the symptoms that started to present were brushed under the rug and life went on. After about 6 months of being in Colorado, I was still finding it difficult to catch my breath and some days would have to stop for a break, just walking from the front door to the car. After a while, I started to question my well-being but always told myself it was probably just in my head.

In June, I started to develop a pretty severe dry cough. It sort of sounded like a smoker’s cough, but I didn’t smoke. I thought it was the Colorado allergies getting to me. I was taking ample amounts of antihistamines and Sudafed, but nothing seemed to help. I sought out the help of a local family doctor, who told me it was probably just allergies and I should take more Sudafed to dry up my mucus. I told her I didn’t have any mucus but she said it was probably just post-nasal drip and sent me on my way.
In July, we were exploring the local towns and while we were walking around, I found myself so dizzy and out of breath we had to stop about every 20 feet so I could catch my breath. I found walking any amount of distance was difficult, but I continued to think it must be because I was out of shape. One afternoon, we went with our friends out for a hike, and I didn’t make it through the parking lot before I was so dizzy I almost passed out and had to sit down. I should have known then there was something seriously wrong.
In August, my husband, who is in the military, left for 5 weeks and I was home alone with the boys. My friends from out of town visited and I started to notice my clothes were starting to fit a little snug. I asked them if they noticed I had gained weight, and they told me it wasn’t very noticeable. I told myself I should start working out more now the boys were a year old and I was no longer breastfeeding.

I took up yoga and started to work out but over the next month I noticed even with all of my efforts, I was still gaining weight, and quite rapidly. By the time my husband came home 5 weeks later, I had gained almost 15 pounds.
That September, we flew to North Carolina for a wedding and upon arrival, my dad asked me if I had noticed my feet were starting to swell. I started wondering if I may be pregnant. The symptoms made sense; weight gain, fatigue, shortness of breath, and now swelling. I made a doctors appointment for when we got back to Colorado for a follow up with a new doctor.
When I got back to the doctor in Colorado, she found my symptoms were pretty significant and she ran bloodwork. She thought maybe I had a thyroid problem, or possibly I was pregnant. She told me the bloodwork would take about 48 hours to come back and then we would know more once it came back. I didn’t make it the 48 hours. The next day I went to bed around 7 p.m., unable to shake how foggy and tired I was. I woke up and when I went to stand up, I almost fell down because my feet and legs were so swollen.
I was having some chest pain and I told my husband I needed to go to the emergency room. I hated going to the doctor, so when I told my husband I thought I needed to go to the ER, he was immediately concerned. Because of the boys, I felt it was easier if I drove myself, so I left him at home with the kids and drove myself to the emergency room.
Upon arrival, things began to happen quickly. The intake nurse took one look at me, and while I was explaining my symptoms, asked for another nurse to come run an EKG. She asked me if anyone had ever asked me about heart failure, and I will never forget the chill that ran up my spine. I said no, I was too young for heart failure. After getting the results of the EKG, I wasn’t even done filling out the paperwork before I was being taken to a room and doctors were coming in.
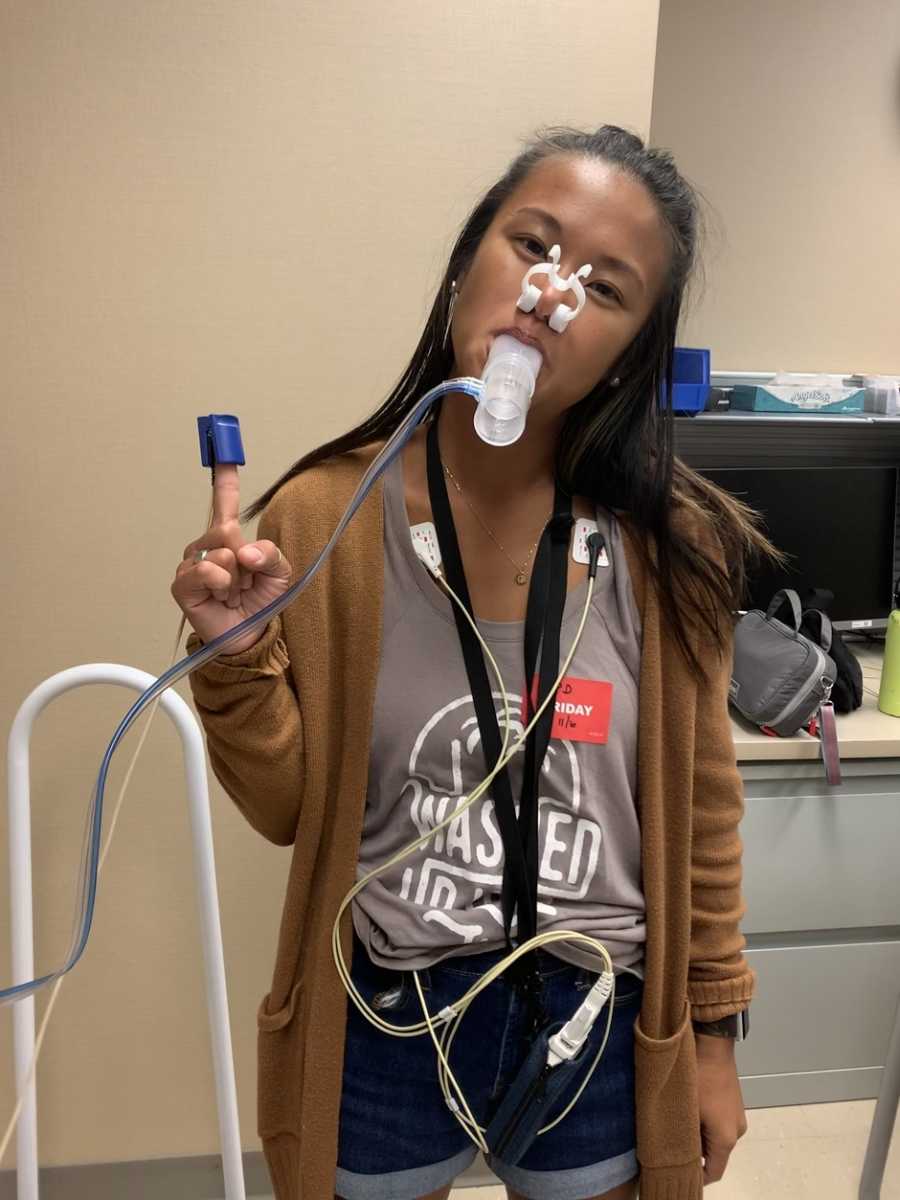
The doctors and physicians were asking me all sorts of questions. When did my symptoms start? Did I do drugs? How severe was the chest pain? They started running tests, echocardiograms, CT scans, X-rays, bloodwork, another EKG, and then the doctor came in and asked me if I had ever had heart disease.
I texted my husband that the doctors were asking some pretty serious questions and I was unsure what was happening. I was scared, and I don’t scare easily. Then the doctor came in again, and he told me I was in severe heart failure and now they were trying to figure out why. They had specialists working on my case and going forward I was going to be admitted to the hospital until they could figure it out.
After about 48 more hours worth of tests and a right heart catheterization, I was diagnosed with mild Idiopathic Pulmonary Arterial Hypertension (IPAH) and congestive heart failure. I was referred to a specialist in Denver. Once I saw the specialists in Denver, they suggested I would be admitted to their hospital so they could run their own tests.
Idiopathic Pulmonary Arterial Hypertension is a rare progressive, chronic lung disease that affects the pressures in the pulmonary arteries. Idiopathic meaning the reason for the condition is unknown. And there is no cure.
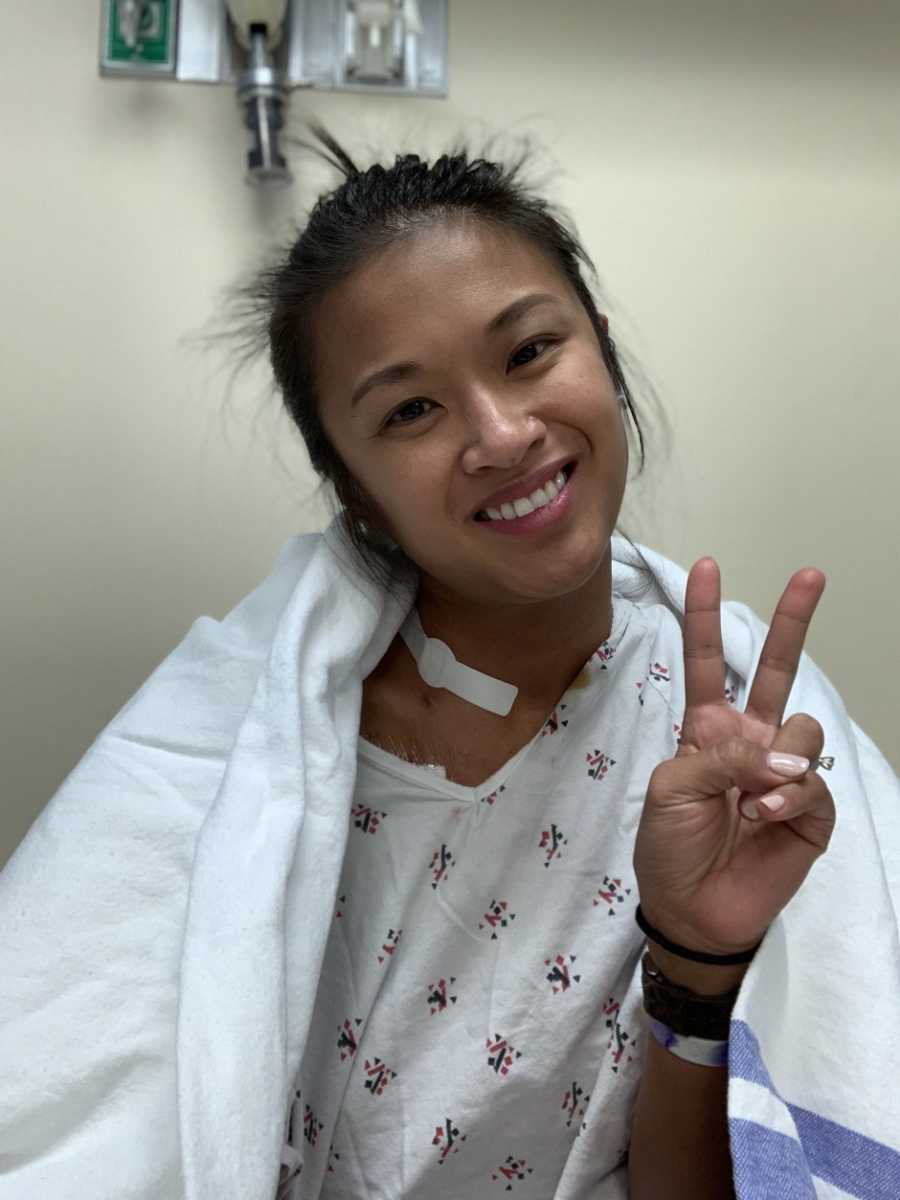
After being admitted in Denver, the tests came back and the team realized my pulmonary hypertension was actually much more severe than the other hospital realized. I actually needed to start medication immediately or I would die. I called my husband and I cried. I called all of my friends, and I sobbed. I begged God to spare me, for my kids’ sake. I remember distinctly feeling God telling me, ‘Gerry, I’m bigger than this.’ I took a deep breath, I got it together, and dug my heels in. We started treatment immediately. They placed a central line to my heart and started me on IV Remodulin for the PH and heart failure.

3 weeks later, we moved from Colorado to Alabama because of my husband’s job. I started at a new hospital and over the course of a year, my condition improved tremendously. My heart went from severe failure to almost completely normal. Unfortunately, I was having numerous issues with skin infections that led to central line infections and almost sepsis so my Alabama team decided that I should try oral medication.
They took me off the pump and started me on an oral medication, in addition to the other two oral medications I had taken on that year. And for a while, I felt like I was on cloud nine, and the oral medication was actually working. However, after about 6 months, I started to feel a little more tired than usual and a little more short of breath than I had been in previous months.
But soon after we moved away from Alabama to Florida in March 2020, my new doctors realized my oral medication was actually not working and my heart was back in severe heart failure. My Florida team told me, ‘For longevity, we have to try something different,’ and that really sobered me. It brought me back down to Earth and we decided we needed to be aggressive in treatment and start back on the pump, but this time a subcutaneous Remodulin pump instead of an IV.
I started subcutaneous Remodulin in August of 2020 and so far the numbers look like they are improving. Slowly but surely. We also recently changed one of my oral medications and it looks like both moves were the right one for me. This treatment could give me many added years to my life, and I’ll take anything I can get!

The subcutaneous pump is similar to an insulin pump that runs 24/7, 365 days a year. I self inject the sites and change them myself. I also change the cartridge out every 3 days and refill it with new medication. The biggest difference between the subcutaneous and IV is my sites are not permanent and they can be used on any part of my body that has subcutaneous fat. It reduces the risk for blood infections I was having issues with on the IV pump.
Facing my own mortality over the last 2 years has been exhausting and also exhilarating at the same time. It’s made me realize there is so much more to this life than the things I was concerned about 2 years ago. Things have been less than easy over the last couple of years and finding doctors I trust have been pivotal in my journey. When things have gotten tough, it’s been incredibly important to stand strong in my faith and belief God uses everything for His good. It also has saved my life to have people who stood by me, even after the diagnosis. The friends and family who have stepped up and shown up have been more important than they probably know.

When I started sharing my story, it was really the easiest way to keep friends and family up to date with current information because things were changing so quickly. But sharing my story on Instagram has brought me such a great community of people across the world, and their stories have fueled the fire of why I continue to share my journey. I have found so much hope and so much comfort in their stories, but I also have people reach out to me who have found comfort in mine.
My word of advice for newly diagnosed chronic illness warriors out there, share your story. There is strength in showing up and being vulnerable. Step out on faith and open up. At first it might seem scary, but there is someone out there looking for a story just like yours.”
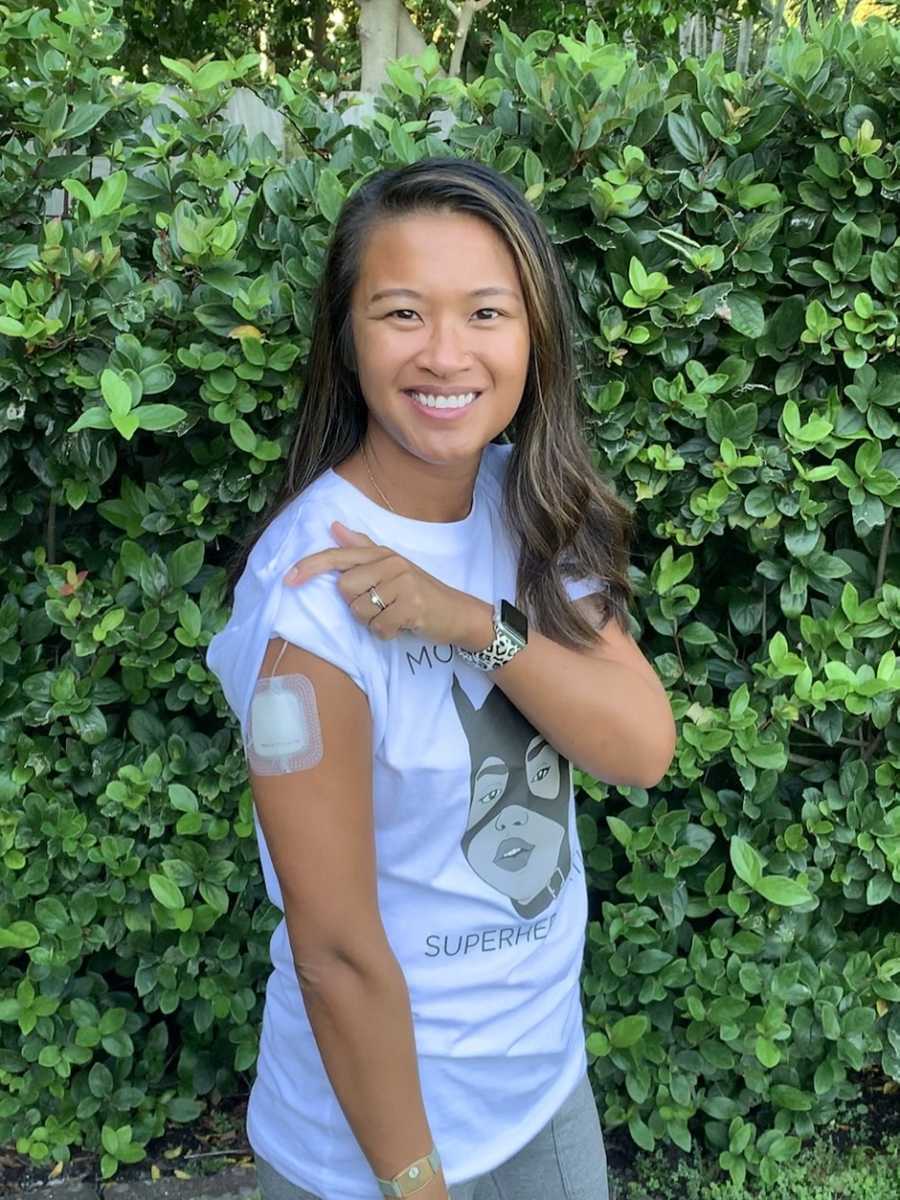
This story was submitted to Love What Matters by Gerry Langan of St. Petersburg, Florida. You can follow her journey on Instagram and her website. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
SHARE on Facebook with family and Friends.