“I’ve always been a very physically active person. I live for the feeling of pushing my body to its limit and the indescribable bliss that comes with exceeding goals and setting new personal records. I grew up as a gymnast, training for 20 hours per week alongside lengthy competitions on the weekends. In addition to gymnastics, I occasionally accompanied my dad on his morning runs before work. I fell in love with the meditative feeling of my feet hitting the pavement, the dewy morning breeze brushing over my skin, and the way the beat of my heart against the wall of my chest made me feel so alive. At this point in my journey, though, I didn’t really appreciate just how good running made me feel.
Eventually, because of a wrist injury, I had to quit gymnastics. The loss of this thing I had spent most of my life working at was devastating. For a while, I couldn’t find anything to fill the new and big, empty space. I didn’t know who I was or what to do with my more than 20 extra hours of time per week… and then I remembered my love of running. I began running regularly and on my own instead of just occasionally with my dad. I even continued the practice into college where I studied pre-nursing and maintained a part-time job. In 2015, I ran my first marathon, the Chicago Marathon, in support of the University of Iowa Dance Marathon. Running created space where I felt cramped in my life and became a valuable kind of therapy for me I may not have fully been able to appreciate had I not lost my ability to do gymnastics.
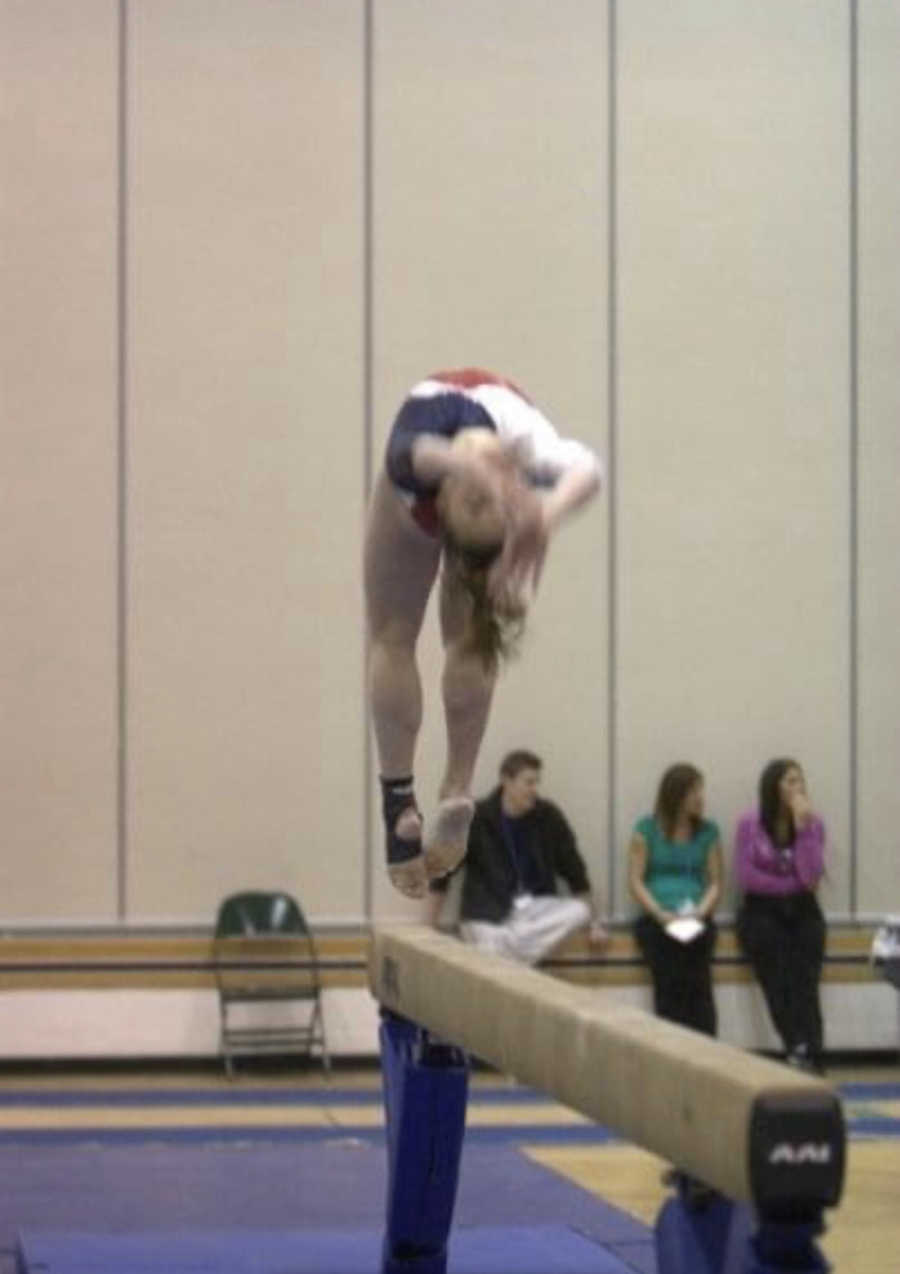
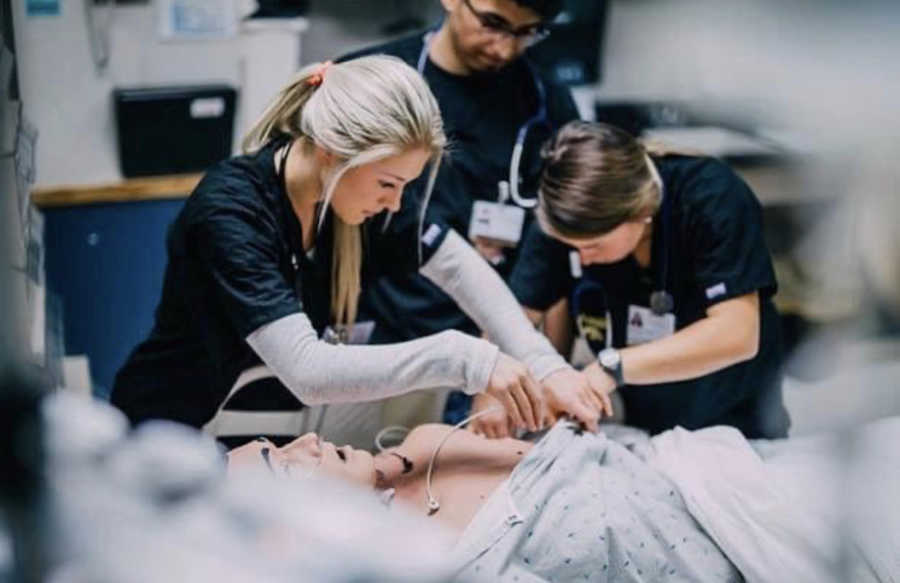
In 2018, all of my hard work in school paid off and I officially became a full-time, registered blood cancer/stem cell transplant nurse. I couldn’t wait to start being a small light in the midst of some people’s darkest, scariest days. I worked 12-hour shifts 3 days a week and continued to run and rely on my running practice as a meditative/therapeutic tool — especially during the exceptionally difficult transition that was going from student nurse to floor nurse.
Around the same time I began my career as a nurse, I joined a gym called Orange Theory Fitness (OTF). OTF is a group fitness studio that combines 30 minutes of cardio (treadmill/rower) with 30 minutes of weight floor exercises. The group aspect of the studio gave me a ton of new and beautiful friendships and made me feel part of something bigger than myself. I always had someone cheering me on and pushing me to beat my own personal bests and vice versa. When work was exceptionally difficult, (i.e. a patient passing away or another getting devastating news, or even just your everyday stressors of working in a fast-paced hospital setting) the treadmill at OTF was always right there waiting for me to let out my frustrations.
In May of 2019, I ran my fastest mile time of 5 minutes and 42 seconds. I was elated and just radiating so much happiness. I remember telling my closest friends how much I wanted to reach a 5 minutes and 30-second mile. That was my ultimate goal and I couldn’t wait to train. Unfortunately, in June of 2019, things changed. Over the course of about a month, I noticed my hips start to ache while I ran. I sometimes also noticed morning stiffness that would hang around until I got moving for the day. I tried not to pay too much attention to either of these things and instead started scheduling my workouts in the afternoons as opposed to mornings.
At the start of my symptoms, I visited my PCP who referred me to physical therapy thinking I had just overdone it at the gym. It makes sense when someone tells you they just ran a sub-6-minute mile a few months before starting to experience symptoms of pain and stiffness! In my head though, I knew this was something different.

Over the next few months, my pain and stiffness continued to get worse. I went from running five times a week to avoiding the gym altogether. When I woke up first thing in the mornings, I would wince at just the thought of my feet hitting the floor. On top of my hip pain, I had started noticing a throbbing sensation in a few of my toes along with swelling and redness. It hurt so much to take those first few steps of the day that a lot of the time I had to hold back tears. I began limping for the first few hours (sometimes even the whole first half) of my day and my 12-hour shifts as a nurse started feeling impossible to muster through. I constantly worried something bad would happen at work (i.e. a code blue or some other type of emergency) and I wouldn’t be able to move fast enough to help. Walking was almost out of the question so running wasn’t even on the table. At my worst, I couldn’t even jog across the street to avoid an oncoming car. This was definitely something more than an injury from overuse and I knew exactly what it was.

At 12 years old, I was diagnosed with plaque psoriasis. The areas that are primarily affected are my scalp, my elbows, and occasionally my knees. Sometimes it pops up in random places, but generally, I would consider my case pretty mild compared to some. When I was diagnosed with psoriasis and at every clinic visit thereafter, my dermatologist warned me of the risk of psoriatic arthritis (PsA) and told me I needed to call right away if I experienced any joint pain. She would usually then attempt to reassure me by explaining while there is a risk, the majority of people with psoriasis don’t develop PsA. So, even though I knew the pain and stiffness I was experiencing could be PsA, I didn’t want to accept it. It was one of those things that ‘only happens to other people with psoriasis’… it had to be.

Unfortunately, it wasn’t. In November of 2019, at the age of 26, after a few more months of denial, I saw a rheumatologist who diagnosed me with what she described as ‘a textbook case of psoriatic arthritis.’ I remember the very first wave of grief (there would be many, many more) I felt as I sat on the cool, paper-lined exam table and watched my new rheumatologist examine my joints for damage. This would be forever. Part of me knew all along, but a bigger part of me had been holding onto the hope that it was still just a bad injury; something that could be cured.
My psoriatic arthritis diagnosis flipped my world upside-down. Seemingly overnight, I went from being an oncology nurse to a rheumatology patient and from being a runner to someone who could barely walk a mile. It felt like in a matter of months, my body had aged from 26 to 83 and instead of deciding which race to run next, I was now deciding which medications to try and which direction I would go if the first-line therapy didn’t work. It felt so isolating at first because none of my friends could really relate to what I was going through. When I told people in my life about my diagnosis the most common response was, ‘but you’re too young to have arthritis.’ This got to be frustrating over time because I always felt like I needed to explain myself or my diagnosis or both and I remember thinking so many times, ‘Clearly, I’m not too young because here I am… I have it.’ Eventually, I just started smiling and nodding in response.

The stresses of work continued on top of the stress of this new diagnosis and not long after that, a global pandemic ensued. My usual coping mechanism, running, wasn’t an option anymore and because of this, I felt trapped. I felt like my world was spinning out of control and all I could do was sit there and try not to throw up. Around the time the pandemic started, my doctor also urged me to switch to immunosuppressant medication since my first-line therapy wasn’t working. I couldn’t believe she wanted me to start medication that would suppress my immune system when we had just entered a pandemic. It felt so counterintuitive and I was scared to death. Luckily, I have a very patient and understanding doctor who listened to all of my concerns and sat with me for more than an hour so we could comb through my fears together and ultimately get me going in the direction that would be best for me… which ended up being starting the immunosuppressive medication.
I struggled a lot with depression during the early days of my diagnosis. I just felt so stuck in my body and all I wanted to do was unzip my skin and climb out. The medications I started would make me feel fatigued for days on end after taking them. I barely had any energy on top of still having joint pain and I cried a lot, but never in front of anyone. Eventually, I even ran out of tears. I felt like my spirit no longer matched my body or what it could do and there was very little I could do about it. I craved that feeling of my feet hitting the pavement, the breeze brushing over my skin, and the beat of my heart against the wall of my chest, but my body could no longer give me that. I also experienced intense guilt for feeling sad about my loss of ability. As a blood cancer/stem cell transplant nurse, I’m often present for some of the worst days of other people’s lives. Because of this, I felt guilty for grieving my loss of mobility, when other people were grieving the fact that they now had to fight for their lives.

Even without the added grief I was experiencing relating to my job, arthritis is a tricky thing to grieve because sometimes you barely get to finish grieving one thing before another loss pops up. Even with medication on board, my body became unpredictable. I never knew which body I was going to be waking up to in the morning. Some days I could barely walk from the bed to the couch and then the very next day I could jog a whole mile completely pain-free. It had to be as confusing for other people as it was for me. Luckily, right around the time I was diagnosed, I found an incredible therapist who helped (and continues to help) me through these confusing and unpredictable days.

In May of 2020, I created an Instagram account. I was tired of feeling alone and wanted to connect with other people closer to my age who were experiencing what I was experiencing. Little did I know at the time, this Instagram account would be a saving grace time and time again through some of my worst days. Almost instantly, after sharing my first post, I was welcomed into a huge community of people who with a wide range of chronic illnesses who just ‘got it,’ people who didn’t tell me I was too young to have arthritis, but who instead listened and held space for me to navigate the journey. I shared and continue to share my heart in long Instagram captions, which provides me with an outlet – similar to the way running had, just without the runners high. I share everything from my fears of asking for accommodations at work and in life to my experience with grief and chronic pain to the ways I’ve been able to modify exercises to stay healthy and active. Similar to my reason for wanting to be a nurse, my goal in creating this new account was to be a sort of lighthouse for those newly diagnosed; to make their journey a little smoother and a little less lonely and dark than mine. Very quickly though, this community became a lighthouse for me too.

Currently, my heart is bursting with happiness because finally, after a year and a half of trial and error, I’m on a medication regimen that is working. I still experience fatigue from my medications, but I’ve actually been able to get back to running recently, which for a while I thought would never happen. I now have very little to no pain at work and no longer fear I’ll have to quit doing what I love. I’ve also recently teamed up with Healthline, a health and wellness company, and have had the privilege of serving as the guide for their new app called PSA Healthline. Through this app, I’ve been able to hold space for others as they navigate their PsA journey and share their stories, trials, and triumphs in a space outside of Instagram.

To anyone who has just been newly diagnosed with PsA, I want you to know even when it feels like things will never get better, I promise they will. Even if your joints don’t get mend the way you wanted them to, or your pain hangs around longer than you hoped it would, YOU get stronger, more resilient, better. The process is slow, but I promise you’re not alone even on those days when you feel like nobody in the world ‘gets it.’ You’re not alone when your pain is wearing you down or when your fatigue is making it hard to even get up off the couch. I want you to also know it’s completely okay for you to feel how you feel right now. You don’t have to try to find the silver lining to your diagnosis or attempt to reason through how it has made you a better person. It’s okay for you to just be how you are in this moment and to feel how you feel – even if the feels aren’t great.

Finally, I want to gently remind you the moment you’re born your worth is established. It’s completely static and totally priceless. Your PSA diagnosis doesn’t change your worth. The way your body changes in response to your diagnosis and your change in mobility doesn’t change your worth. Your need for help and/or accommodations doesn’t change your worth. We are all just as worthy with our PsA diagnoses as we and are… or were… without. And most importantly, your story matters – so don’t be afraid to share it.”

This story was submitted to Love What Matters by Jenny Parker from Iowa City, Iowa. You can follow their journey on Instagram. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more touching stories like this here:
Provide hope for someone struggling. SHARE this story on Facebook to let them know a community of support is available.

