Changing Scripts
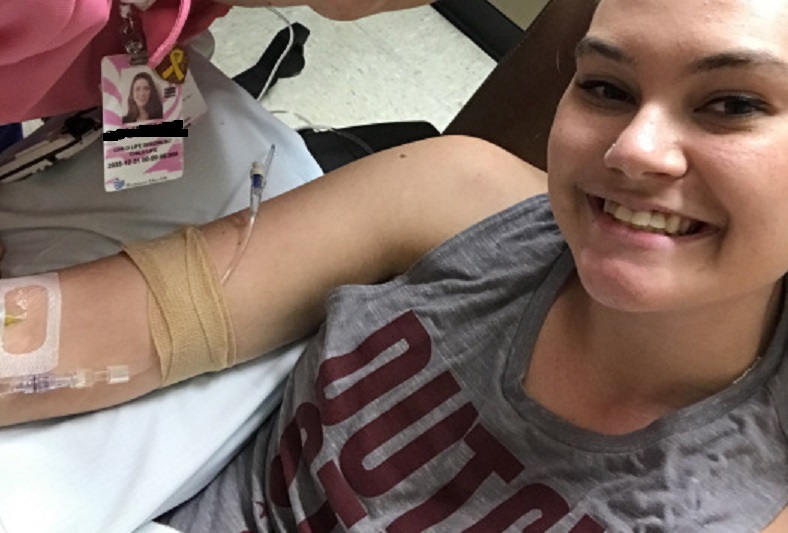
“I’m suddenly awakened by the beeping of the IV pump, and I quickly glance at my watch to see that it’s already 1:30. The nurse, having heard the pump, is already at my bedside and ready to flush and remove my IV. ‘Sorry friend, nap time is over and it’s time for work!,’ she jokes as I get out of the (somewhat comfortable) recliner. ‘See you Saturday!,’ I reply.
It’s time to switch gears to get ready to ‘go to work,’ though I’ve been here in the hospital all morning already. I walk back to my office, careful to remove the bandage from my arm so that no one asks where I’ve been. I slide my patient wristband off and drop it into my purse. It’s become such a normal routine I’m not even fully aware of the actions I take to maintain this ‘secret life.’ This morning, I was Sarah, a patient with chronic illness needing medical treatment and intervention; but now it’s time to transform into Sarah, the child life specialist and full-time pediatric ED employee. I quickly change clothes in my office, clip on my badge, and log in. It’s go time.

POTS Diagnosis
It’s been a little over a year since I received my POTS diagnosis, and the diagnosis of Ehlers Danlos followed quickly thereafter. POTS is short for postural orthostatic tachycardia syndrome, and is a failure of the autonomic nervous system to appropriately regulate heart rate and blood pressure. Ehlers Danlos is a connective tissue disorder that is responsible for frequent joint subluxations and hyper-mobile joints. Some clinicians believe the underlying connective tissue disorder actually causes the POTS, but this isn’t a well-studied or proven phenomenon.
To put it lightly, this diagnosis was hard to process, for many reasons. First and foremost, it was time to accept I was ‘chronically ill’ and this was not a transient problem I could grow out of or wish away. The nagging symptoms and scary near syncopal episodes finally had a name, and that name was not curable. It was comforting to have an answer, but terrifying to understand the potential lifelong implications and symptoms that may never go away.
Second, it completely rocked my world from the healthcare employee point of view. For longer than I’d like to admit, I was a part of the medical community who completely disregards ‘dysautonomic’ diagnoses. For far too long, and partly due to a lack of education on my part, I believed that ‘dysautonomia’ was a synonym for ‘psychosomatic.’ Yes, I, too, was skeptical until the conditions manifested themselves in my very own body, in a very real way. Aside from ‘anxiety’ induced palpitations, aside from feeling fatigued after a full night’s rest, aside from transient nausea and skipping meals, it quickly became clear there was systematic dysfunction; something I pushed from my mind for months before seeking medical help (denial is real). So the reality, as I’ve painfully learned, is that dysautonomia and psychosomatic are actually worlds apart.
Dysautonomia is a blanket term or diagnosis, yes, but it is caused by autonomic system dysfunction – not by a mental factor. It encompasses a lot of different disorders, syndromes, and diagnoses – but all with one common denominator – the failure of a person’s autonomic nervous system. For me, this means my body does not regulate heart rate and blood pressure changes as it should. Because it’s not my heart but my nervous system that is malfunctioning, I experience a whole constellation of symptoms: stomach pain, nausea, headaches, palpitations, hypotension, and tachycardia. Because the underlying problem is depleted blood volume and not necessarily dehydration, drinking upwards of 80 ounces of water a day doesn’t always do the trick. It feels wrong to liken this daily struggle to a hangover, but it’s sometimes the easiest way for others to understand it. I often wake up feeling dehydrated, nauseated, and with a gnarly headache.

Invisible Illness Struggles
Throughout the day, I may experience palpitations, lightheaded and shakiness, and chest tightness or pressure. Anything that involves standing still is likely to trigger some amount of symptoms: at its worst, I become diaphoretic, dizzy, and my vision and hearing will black out— it’s my body’s way of telling me to find a place to sit – ASAP. These symptoms will be especially prevalent if dehydrated or if I spend time out in the heat (hello, I live in Phoenix… yikes) Luckily, due to the treatments I’ve started and continue with, these days are slowly getting fewer and farther between and I’m so, so thankful. The problem with POTS is there is not a clear treatment that works for everyone; it’s been described to me as a constantly moving puzzle, trying to fit the pieces in the right places.
So, my current puzzle pieces: 5 oral medication doses a day, 1-2 IV infusions per week, and at least 3-4 days of ‘cardiac rehab’ to retrain my nervous system. I’m on a doctor-ordered high sodium diet and I drink at least 80-100 ounces of water each day.
That’s what life looks like for me right now. I’m thankful for the treatment and its positive effects but I often feel like I spend more time in doctor’s offices and hospitals than I do spending time doing fun things with my friends; I spend more time on the phone with doctor’s offices, pharmacies, and hospitals than I do talking to my family. Not exactly the life this 24-year-old dreamed of.
Even with all I’ve done to work on appearing and acting normal, I’m still hesitant to share this struggle with friends, coworkers, and peers. I dispose of all ‘evidence’ of my IV infusion before heading to work. I would be lying if I said I hadn’t considered covering the bruises as well. I take the oral medications before and after I’ve left work. I don’t why I try so hard to maintain this ‘secret.’
Maybe it’s because I am in denial that I am ‘sick’ and not healthy like my coworkers and best friends. Maybe it’s because I stood by as a doctor at work told her resident, ‘anytime you see POTS, you know the patient is crazy before you go in the room. It’s made up.’ Maybe it’s because I wish I could live, love, and laugh with all my friends without needing medical treatment first. Maybe it’s because I overheard a nurse who I had confided in tell another nurse, ‘she just doesn’t know how to drink enough water.’ Maybe it’s because I don’t want anyone to feel bad for me or treat me differently, or tell me I should go home and rest (not knowing this is actually a daily occurrence for me). I want to be tough. I want to be the girl who can handle anything and stay strong. I want to be seen as ‘normal,’ just like everyone else.
I want to feel like I’m on top of the world and can conquer whatever is thrown my way. Or maybe it’s because I’m afraid the medical professionals I respect and love so much will have a changed opinion of me when they learn of the diagnoses I carry; the chronic illness I live with. Maybe it all comes down to this: my desire to be popular and to be liked and supported outweighs my desire to be fully and humbly honest. I’m afraid if I let people see this ‘other side’ of me they will draw back. They will run away, quickly realizing I’m far from healthy, far from ‘normal.’
By the time I clock out and leave here tonight, I will have been in the building for 14 hours. 3 as a patient, and 11 as an employee. This is invisible illness. This is dysautonomia.”
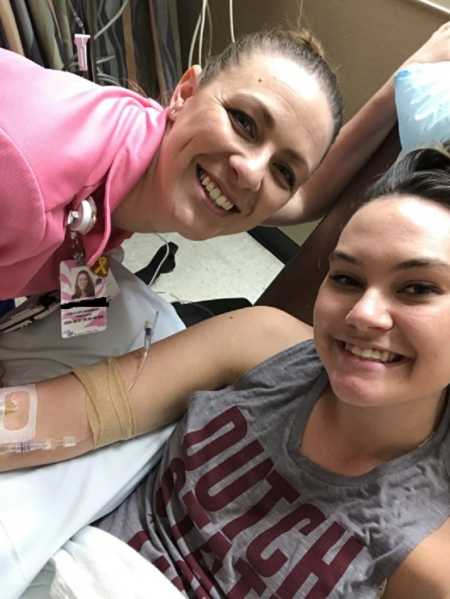
This story was submitted to Love What Matters by Sarah H of Arizona. You can follow her work on her blog. Submit your own story here, and subscribe to our best stories in our free newsletter here.
Do you know someone who could benefit from this story? SHARE on Facebook to let them know a community of support is available.