“As a first-time mother in 2015, I knew I wanted to breastfeed, and my goal was to make it one full year nursing my son. Even taking a ‘Breastfeeding 101’ class at the hospital where I was due to give birth did not fully prepare me for the challenges and issues I would eventually face.
My older son was born in March 2015 after an emergency cesarean. I was induced the day prior and was only slowly progressing overnight and into the next day. My son did not respond well to the medication and increased contractions. I was given an oxygen mask as the nurses closely monitored his stats. Unfortunately, his heart rate dropped, and he went into fetal distress. My OB/GYN came rushing over from her office next to the hospital and explained I would need to have an immediate c-section. My baby’s heart rate had been too low for too long and needed to come out as soon as possible.

It was a rush and blur being wheeled into the operating room. Laying on the table staring up at the ceiling and the bright hospital lights waiting and praying was terrifying. I had a difficult time staying calm that my heart rate spiked high. The anesthesiologist kept having to remind me to take deep breaths to calm myself and bring my heart rate stable. Within the hour, I was in recovery holding my son in my arms. Luckily, he was perfectly healthy. Having a c-section caused my breastmilk to come in slower than normal, which is quite common. I was nursing my son every 2 hours or so, but he still was not getting enough milk, called colostrum, so we decided to supplement my milk with formula for a few feedings. Because he was born full-term, donor breastmilk was not available to him. After bringing him home from the hospital, the first 2 weeks of his life he struggled with weight gain.
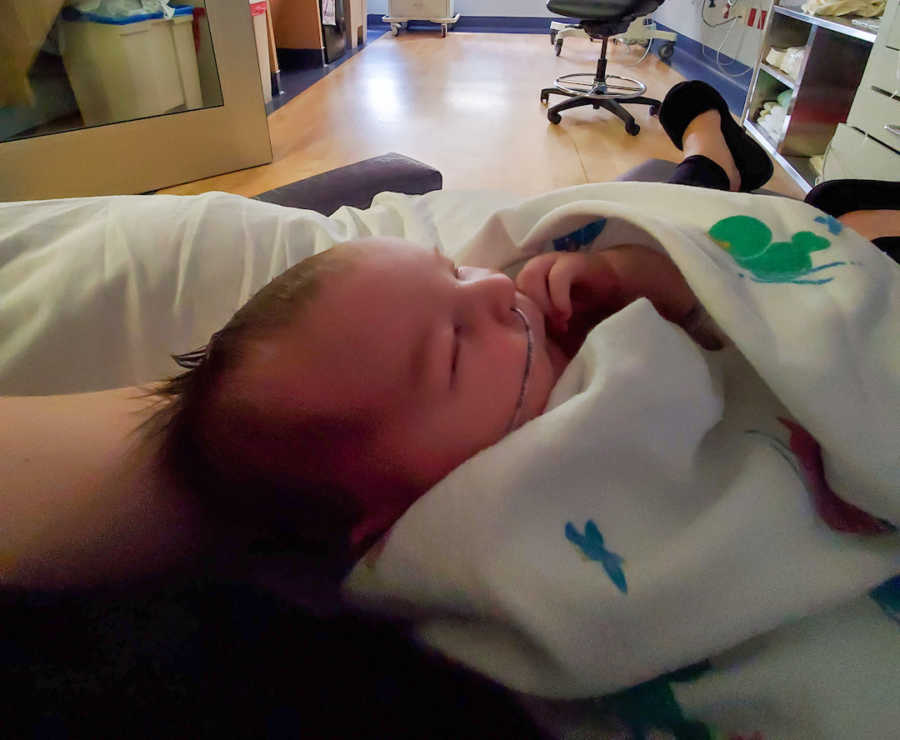
To ensure he was receiving enough milk at each feeding, I pumped in between nursing sessions, then used my pumped breastmilk in a supplemental nursing system (SNS) when feeding him. Essentially it was my milk in a bottle with a valve attached to a long, thin, tiny tube that taped to my breast at the nipple, so milk would come from my body and from the feeding tube. Usually, my husband held the bottle upright so the milk would flow down, providing additional milk to my son at every nursing session. My son eventually gained back all the weight without having to supplement with formula again. I had to continue with extra pumping to build up a supply of frozen milk for when my husband and I went out of town for 3 days when my son was 6 weeks old. I was exhausted taking care of a newborn on top of waking up at 3:00 or 4:00 a.m. to pump my milk to make sure he had enough milk for when we were gone. I did that for over a month straight.

I was blessed with an oversupply of milk and my son didn’t end up needing all the frozen milk. With him exclusively breastfeeding and not taking a bottle, I had a freezer full of milk I no longer needed or had room for. At the time, there were no milk banks in my area that collected human donor milk. I ended up donating to two local moms in one of my online breastfeeding support groups who both had a low supply and did not want to supplement their son and daughter with formula. I am proud to have met my goal and surpassed it by being able to nurse my older son to 21 months old but to also help a few local moms and their babies.

Fast forward to July 2019 when I was pregnant with my second son. I knew I wanted more birth support because I wanted to try for a VBAC (vaginal birth after cesarean), so I hired a doula. She was the one who told me there was a milk bank for the area in case I needed to supplement again and did not wish to use formula. Mother’s Milk Bank of North Texas (MMBNT) is a non-profit organization that provides premature and critically ill infants human donor milk when their own mother’s milk is not available.
After making a call to the hospital I was due to deliver at, I discovered donor milk was only available to non-full-term babies. After about 4 days of prodromal labor, and a day of regular labor, I was able to achieve a VBAC with my second son. But my happiness ended there because while he was born full-term at 41 weeks, he suffered from severe meconium aspiration. He had inhaled his poop, for lack of better description, at some point during labor, and while that is not uncommon, what is uncommon is how sick he was. His infection was so severe he went immediately to the NICU where we waited for hours to see him.

He was on medications to help clear up the infection in his lungs, and ventilators to help him breathe. My colostrum started to come in that same night and by the next morning, I was able to start pumping my breastmilk since I was unable to nurse him. I was exhausted physically and mentally but determined to continue pumping for my son, so I did every 2-3 hours.
The second day after he was born was the worst day of our lives. The neonatologist came to us and described to us our son was not stabilizing. His heart was working so hard to keep up with the ventilator for his lungs she was worried there was a chance he would need ECMO surgery. Basically, a bypass for his heart and lungs, allowing them to rest and get better. The NICU there at the hospital he was born at did not have the capability for this surgery and machine, so the decision was made to transfer him to Medical City Dallas Children’s Hospital where they have the top level of NICU designation in our area.
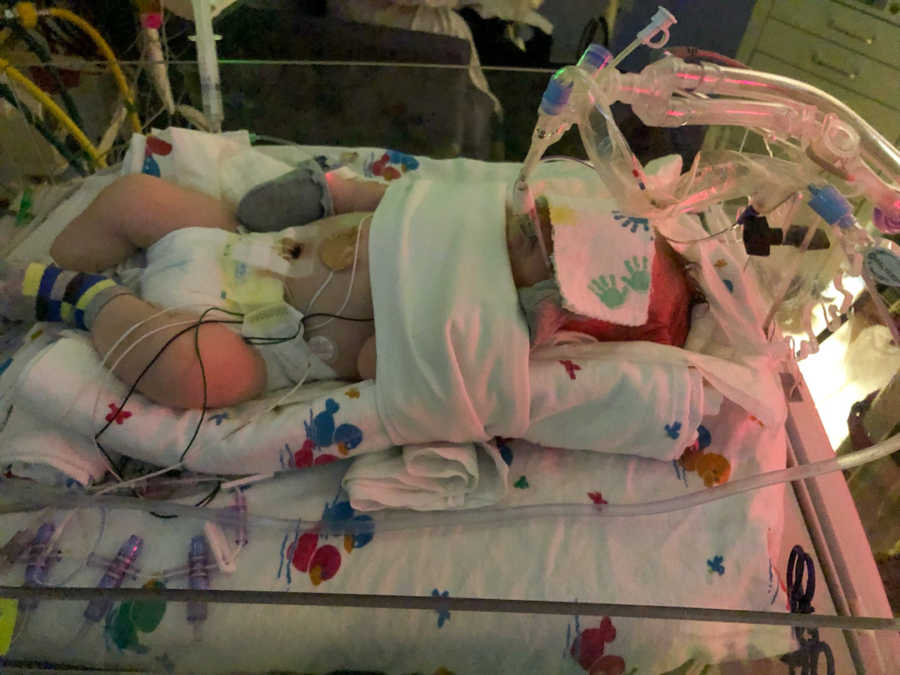
My son stabilized enough to be transferred by ambulance. I was able to be discharged early myself in order to be able to go with my husband to the Children’s Hospital. In the early hours of the morning before the sun rose, we raced to keep up with the ambulance carrying our child as he fought for his life. When we arrived, the nurses and staff showed us to the waiting room. And wait and wait we did. It was hours before the doctor found us and described our son’s condition and prognosis. He was not in the clear just yet, but on the long road to recovery and luckily did not require the ECMO machine or surgery. After scrubbing in to disinfect our hands, we were finally able to go back to see him. He was attached to so many wires and tubes it was difficult to touch him. We had to keep contact with him to a minimum at first because he was easily overstimulated causing his stats to go back up. The only thing I could do was rub his forehead and eyebrows and talk and sing to him for days.

There was a lactation room there in the NICU that provided breast pumps and supplies for the mothers. I was grateful for a place to sit and pump and decompress for 20 minutes after the stress of everything going on with our son. Besides pumping at the hospital, I continued pumping at home every 2-3 hours. I would bring my breastmilk I pumped at home to the hospital and my son was fed with it through a feeding tube. There was always milk leftover because I was pumping more than my son was being fed, so I was able to keep my milk in a small refrigerator in his room for the nurses to use the breastmilk as they needed for his scheduled feedings. We were traveling back and forth from the hospital to our house every day, about an hour drive each way since the NICU did not have the room for me to stay in-room with my son.

We are grateful my husband’s parents, and then my mom, were able to stay at our house for a few weeks to help care for our older son while we were traveling back and forth to the hospital. Eventually, he got well enough to be disconnected from some of the machines, ventilators, and oscillators. After weeks, we were finally able to hold our son in our arms and I will never forget the pure joy I felt after not being able to hold him directly after his birth. It was an adjustment holding him while he was still connected to his feeding tube and pulse oximeter. The constant beeping and sounds his machines made were nerve-wracking.
Day by day, he got better and better. I was able to try to nurse him after about 2 weeks, but that did not go so well as he had to learn how to breathe and eat properly so as not to inhale milk into his lungs. Soon after, he was discharged from the critical unit of the NICU to another floor for babies that were doing well. There he was still given milk in his feeding tube every 3 hours, but we were given the go-ahead to try bottle feeding him with my milk to see how he did. Gradually, he took a bottle but was still not too successful at it.

The doctors were concerned they did not want to take his feeding tube out until he was competent with bottle-feeding or breastfeeding. I got approval from the doctor and OT to try nursing again. Fortunately, he got better and better at nursing, so whenever I was there at the hospital and he was due for a feeding, I was able to nurse him. The time finally came where his feeding tube was able to be removed. For him to be discharged to go home, the doctors wanted him to gain a certain number of ounces from nursing him at every feeding. In order to accomplish this, I stayed overnight at the hospital for two nights, almost three, with feedings every 3 hours or on cue whenever he was showing signs of hunger. Sleeping and staying at the hospital day and night was arduous. Between waking up for feedings, the sound of the beeps and machines, people and staff walking past the room, and nursing coming in for rounds and assessments, I barely got any sleep. I was glad to do it because it was the first time I was able to continuously care for my baby without having to leave him every night.

My efforts were rewarded, and with the help of the nurses and lactation consultants, my son was able to be discharged as fully recovered as an exclusively breastfeed full-term NICU graduate. That is extremely rare and almost unheard of for NICU babies. Going home, I brought the unused breastmilk home with me to add it to my already growing collection in my home freezer. It was one of the absolute best days of my life to finally bring our son home and bring together our family of four. He continued nursing, and I continued pumping when needed to relieve any discomfort. Eventually, our freezer was full of breastmilk and my son was not eating it since he did not take a bottle, so I had to find something to do with it. I made the call to Mother’s Milk Bank of North Texas and began the application process of becoming a milk donor. I completed the health questionnaire and was given an order to have my blood drawn at no cost as the final step. A couple of weeks later, I was notified I was approved as a donor and could begin donating at any time. Even though there are numerous drop-off locations or milk depots as some are called, none were close to me.

After some months, I was able to bring all my frozen milk at the time to the hospital where my son was born. It was surreal being there where I delivered him and seeing it from a different perspective. Another few weeks later in April 2020, I received a certificate of appreciation from MMBNT for donating 787 ounces of my breastmilk. Since I never counted how many ounces I was happily surprised by the amount—that is a little more than six gallons of milk in my first donation. I was not sure if I was going to continue donating, but I still was pumping as needed and saving my breastmilk.
In April of this year, I saw I had quite a bit of frozen breastmilk in my freezer. Knowing my son was not ever going to use it, I decided to make a final donation. My wonderful husband drove me and both our sons over an hour away to Fort Worth, Texas to the MMBNT is located. Because of covid-19 protocols, I was not allowed inside to tour the facility, but I was just as happy to capture a few pictures outside to commemorate the occasion.
A few days before Mother’s Day I received an email thanking me for my final donation of 227 ounces, another almost two gallons. That brings my total donation to 1,014 ounces, just shy of eight gallons of my breastmilk going to feed fragile babies. Writing this now, I am getting emotional thinking of all the hurdles and obstacles I had to overcome with both of my boys in order to breastfeed them, something that seemingly should come as natural. My sons will continue to be my greatest accomplishments in my life but being able to donate as much milk as I did and help so many babies and families is just as high up on my list. If you are a mother reading this and have extra breastmilk or wish to pump extra to donate, I urge you to consider donating to a milk bank in your area. And if you are local to Texas and wish to donate, please reach out to texasmilkbank.org!”

This story was submitted to Love What Matters by Stacey Edwards from McKinney, Texas . You can follow her journey on Instagram. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more amazing stories about motherhood here:
Please SHARE this story on Facebook and Instagram to encourage others to cherish every moment and love what matters most.

