“Oliver’s journey started way before birth. After years of trying and two miscarriages, we found out we were pregnant Labor Day weekend of 2019. We were hoping this third time would be the charm. Going into our first fetal imaging scan at 13 weeks, we were equal parts excited and apprehensive. We went through the scan and everything seemed to be going great until it didn’t.
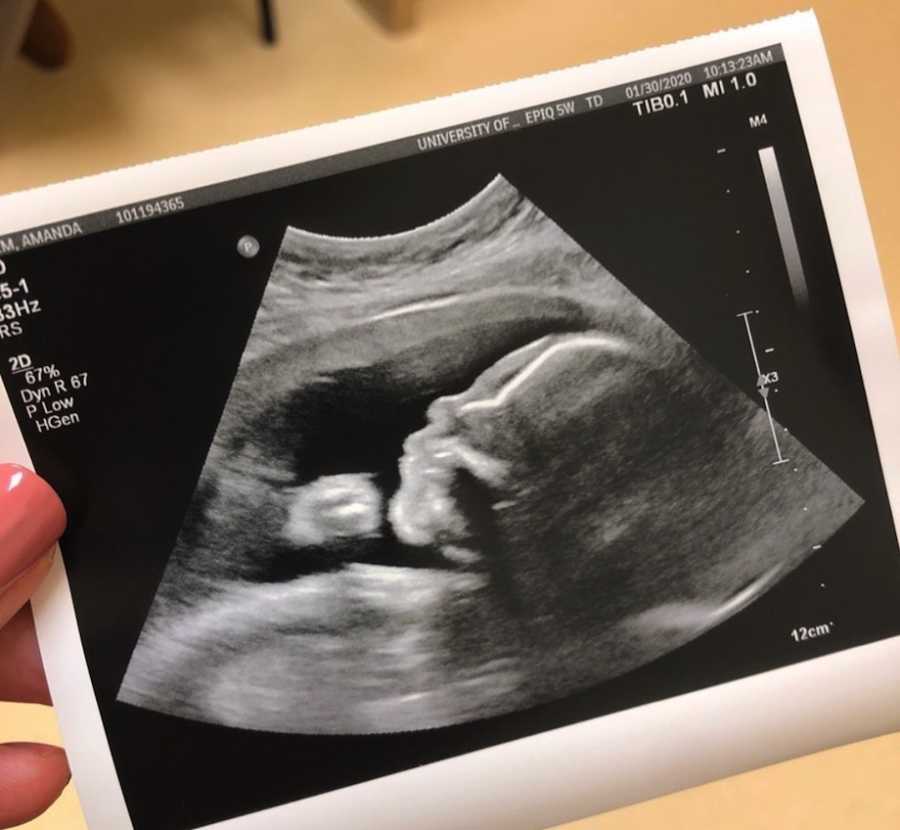
The sonographer must have had a great poker face, as we were shocked when they had our family visitors leave the room immediately after the scan. The doctor came in and painted a grim picture. We discussed things like congenital heart defects, genetics, and potential next steps. We waited for Oliver to continue to grow in order to know more about what his challenges might look like. We followed up with more imaging and more consultations. We were initially told his condition appeared to be hypoplastic left heart syndrome, which came with the likelihood of three or more open-heart procedures. We were scared, to say the least. We thought this was the worst news but little did we know, another issue would arise, changing the whole course of the pregnancy.

We came to the imaging scan as another bi-weekly follow up to see how the heart was progressing but also for a 20-week growth check. We were told there was fluid accumulating Oliver’s abdomen and this condition would more than likely progress to another condition called hydrops. The physician explained he truly believed Oliver’s current condition would worsen, and he would likely not survive. He quickly followed up with, ‘But miracles do happen.’ He continued to explain since we were at 20 weeks gestation, we ‘still had other options’ in Michigan. The physician reminded us ending the pregnancy might be the easiest road, since having a miscarriage or stillborn was likely. We were stunned. We were just coming to terms with the congenital heart defects and not prepared for yet another blow. We stood strong in our faith and wanted to give Oliver every chance possible, so we continued on and prayed and cried and prayed some more.

We were then referred from our local hospital to the University of Michigan Mott Children’s Hospital. This turned out to be a blessing in disguise. Our first visit was on Christmas Eve, an appointment they barely got us squeezed in for. After a very tense, quiet heart scan, we were thinking the worst again. The physician surprised us by exclaiming she could see that Oliver did not have hypoplastic left heart syndrome but rather had a milder coarctation of the aorta and mitral valve stenosis (aka narrow aorta and smaller than average mitral valve). Most importantly, she believed this condition would require no immediate surgical intervention. She did, however, caution us she did not believe the congenital heart defects would cause the fluid buildup in the abdomen. We were, again, cautiously optimistic, and Oliver continued to grow but also continued to gain fluid.

With the referral to cardiology, also came a later referral to see additional Maternal-Fetal Medicine specialists at Mott. There, we learned the most about Oliver and came for bi-weekly scans and consultations. We continued to watch Oliver gain fluid and wondered what would be. At 25 weeks, we had come to a pivotal point. Our physician was concerned enough she suggested we do a paracentesis to remove the fluid building up in Oliver’s abdomen and lower areas. We agreed to the procedure, knowing the risks. Within a week, we were admitted to the hospital, due to our water breaking at just 26 weeks. The medical team informed us Oliver had about a 10% chance of survival. The hospital monitored us and we were able to postpone labor. While we were in the hospital, our medical team found a study at Jefferson University and we qualified. All of our bloodwork was sent over and we anxiously waited for the results. At 30 weeks, we went into labor. Our favorite physician happened to be on the schedule that day and had been expecting the results back from the exome sequence that was completed on Oliver’s DNA. Right after I received an epidural, our physician came in with news. She had heard from Jefferson University and they had found Oliver has a rare syndrome called Kabuki Syndrome. We were in active labor and did not have time to research or discuss this in-depth, as Oliver was soon to make his arrival.

A few short hours later, Oliver was here and admitted to the NICU. Oliver required a ventilator for oxygen support and multiple medications and tests but he was here and stable. We were able to meet with a genetic specialist right after delivery, who is very experienced in Kabuki Syndrome and would be following Oliver’s development.
By day 3 of life, Oliver was breathing on his own and enjoying snuggles when the surgeons agreed it was time for surgery. Oliver had fluid in his belly and there were concerns his intestines were going to twist. Oliver was again placed on a ventilator and faced his first surgery. The surgeons were able to rearrange his intestines and drain the fluid. Prior to the surgery, mom and dad baptized quickly, due to the medical team waiting outside to take him to the OR, in a very quick and sentimental ceremony that involved an empty glass dish from the hospital lunch tray.
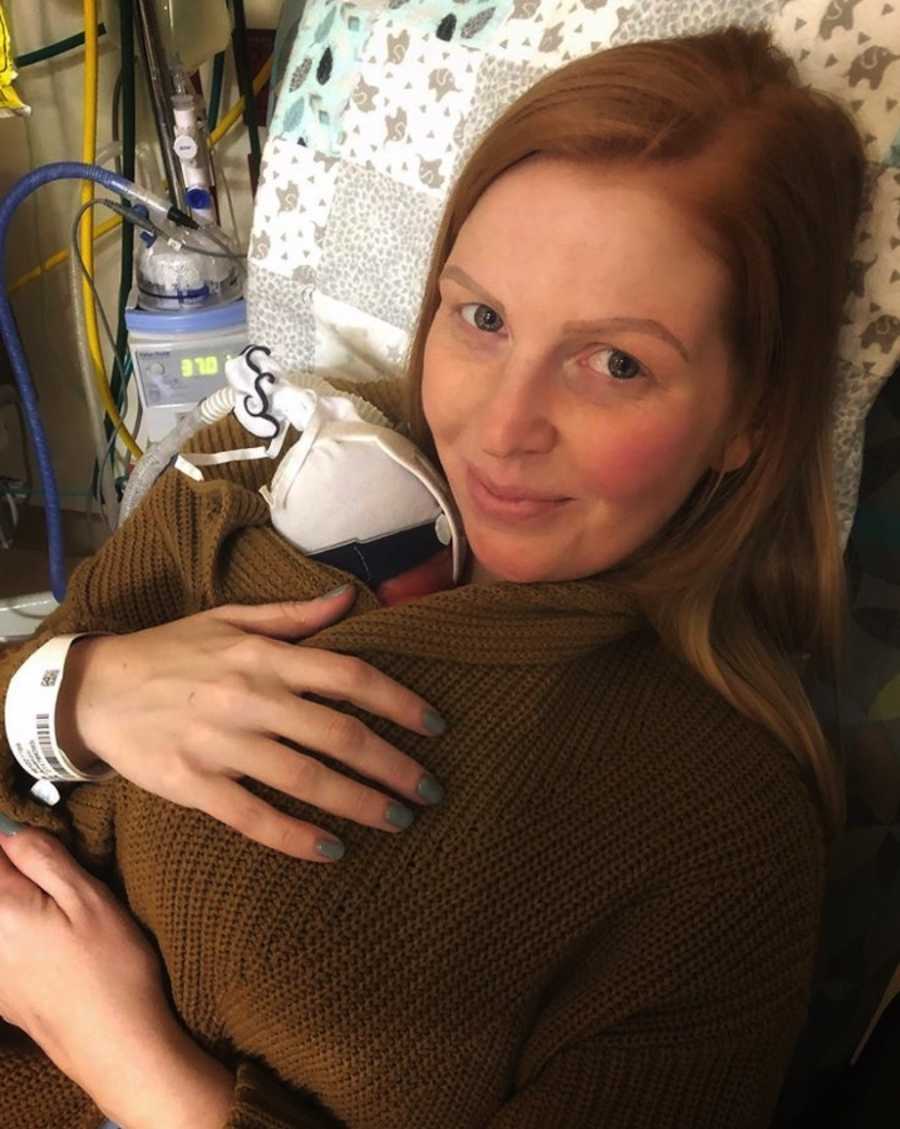
Oliver continued to grow and heal but that all changed on March 25. While we were staying at the Ronald McDonald House, we received a call in the middle of the night from one of Oliver’s doctors. Oliver had been diagnosed with Necrotizing enterocolitis (NEC). Due to COVID-19, only one parent was allowed in his room at a time but we could take turns every other day. The doctors prepared us for the worst. They immediately stopped all feeds, started antibiotics, and ordered X-rays every 8 hours. Dad took Wednesday at the hospital with Oliver and talked to multiple doctors, surgeons, and medical teams as they checked in on Oliver and watched for any signs of perforation. A few days later, the hospital policies changed again and only one primary parent was allowed; there was no switching. Due to the restrictions, we moved back home, which is about an hour’s drive each way.
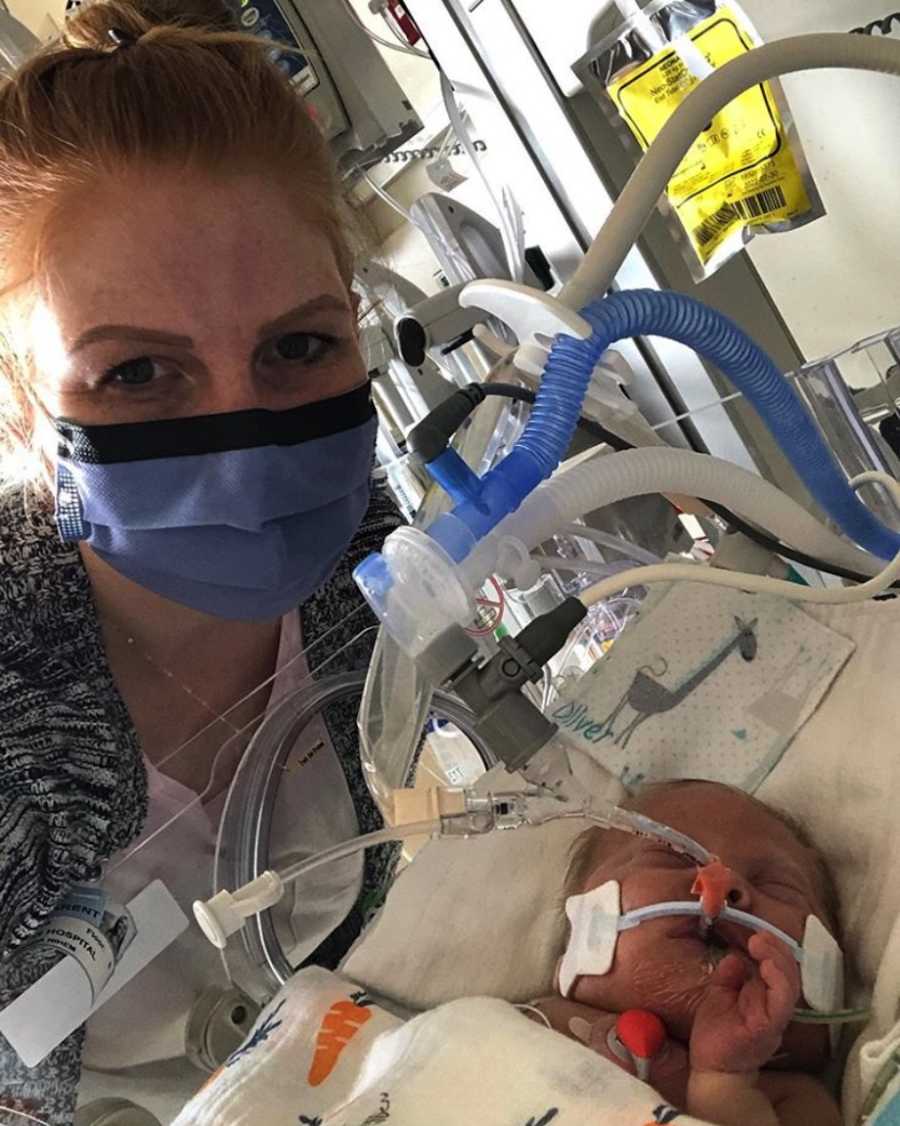
Then everything got worse and Oliver was in critical condition. The hospital approved an exception to have both parents present, due to Oliver’s state. Oliver was intubated and placed on an oscillator. Two drains were inserted into Oliver’s chest to drain the excess fluid that was building up. The medical team sat down with us and talked about how worried they were for Oliver. At this point, Oliver was close to the highest settings on his ventilator and they were not recommending any sort of bypass or life support based on his age and needs. This was a very dark conversation, but without more answers as to why this is all happening, the medical team was stuck. Right after this conversation, the Chaplin called us without knowing the details of the day. She prayed with us over the phone. Dad was only allowed in the hospital for 24 hours, then had to leave due to the restrictions.
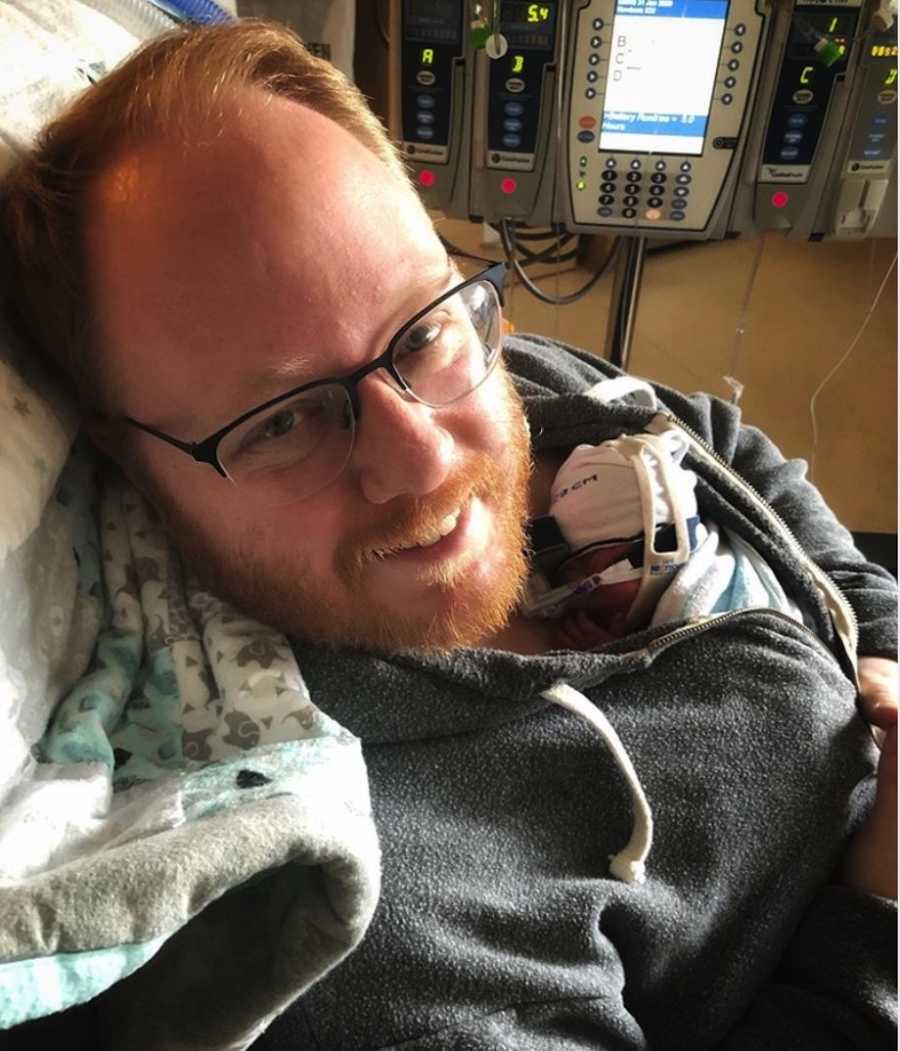
Following this, Oliver had fluid pulled off his belly, as the ascites that appeared to be pocketed and thickening. The fluid was tested and Oliver’s diagnosis of NEC from last week appeared to have made its way out into the belly. Oliver was on multiple antibiotics to fight infections. Oliver remained on the ventilator with chest draining fluid and on antibiotics for 15 days. He had to be sedated the whole time and I was unable to hold him throughout this period. Finally, Oliver pulled through and the chest drains were pulled. The oxygen support slowly became less and less.
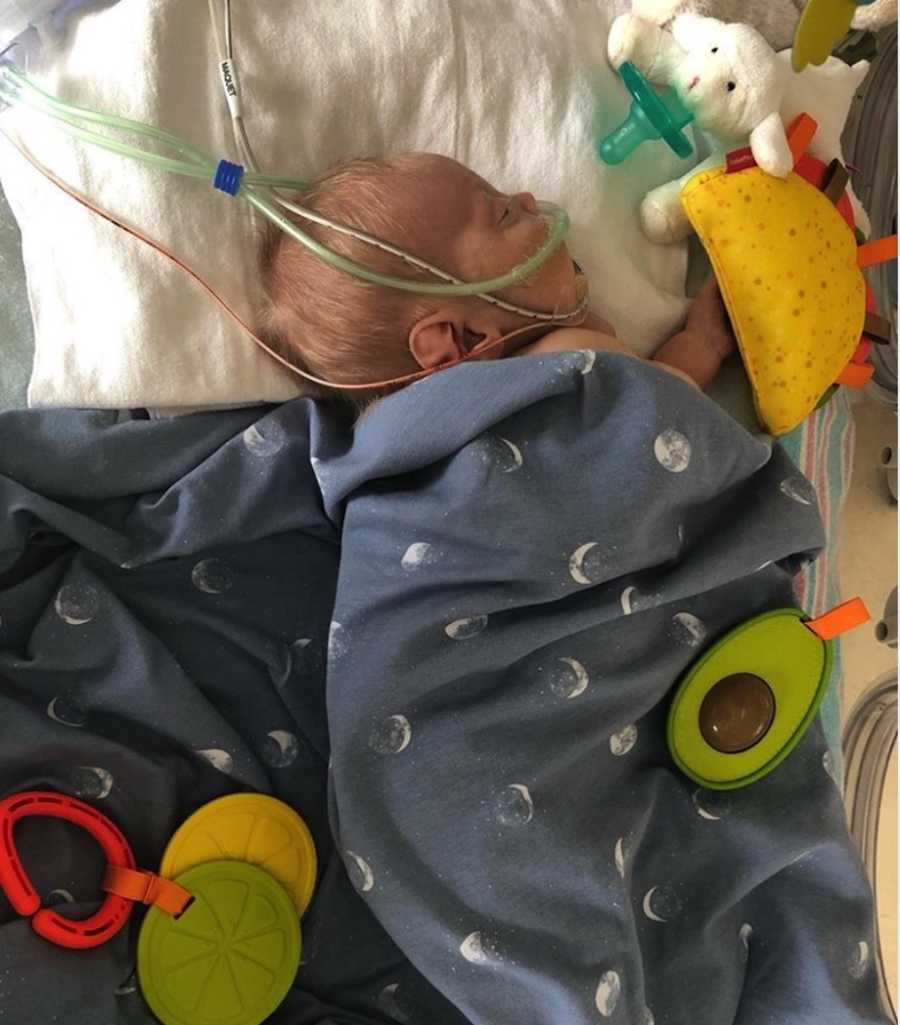
By the end of April, I needed to switch out. The hospital allowed a 7-day switch so his dad became the primary parent. Oliver continued to be on high oxygen support and required a heart catheter procedure, due to having severe pulmonary hypertension, causing Oliver to have very labored breathing. We requested to have both parents there but were denied, even though Oliver had to be intubated again. As of right now, Oliver does not need correction or intervention for his congenital heart defects. The cardiac cath suggests the lungs could be the main cause of pulmonary hypertension rather than the heart. Oliver’s preemie lungs have been damaged by the pressure of the ventilator systems he was on. The care team is suggesting new medications and hoping Oliver could possibly grow out of this condition as his lungs mature.

By Mother’s Day, Oliver appeared to be recovering and growing. Feeds were started and due to blood being found in his stool, he was moved to a very gentle formula. Oliver was able to come off all oxygen support and continued to remain on room air throughout the week! However, he started to vomit a few days later so the medical team stopped Oliver’s formula feeds and went back to IV nutrition. Oliver had an upper GI study, which takes all day and requires a bunch of X-rays. Oliver returned to his room and immediately projectile vomited. We had to restart again, however, this time the doctors requested Oliver remained upright in between the X-ray to avoid more vomit. Oliver had an X-ray every couple of hours and remained mostly held upright. However, he continued to vomit.
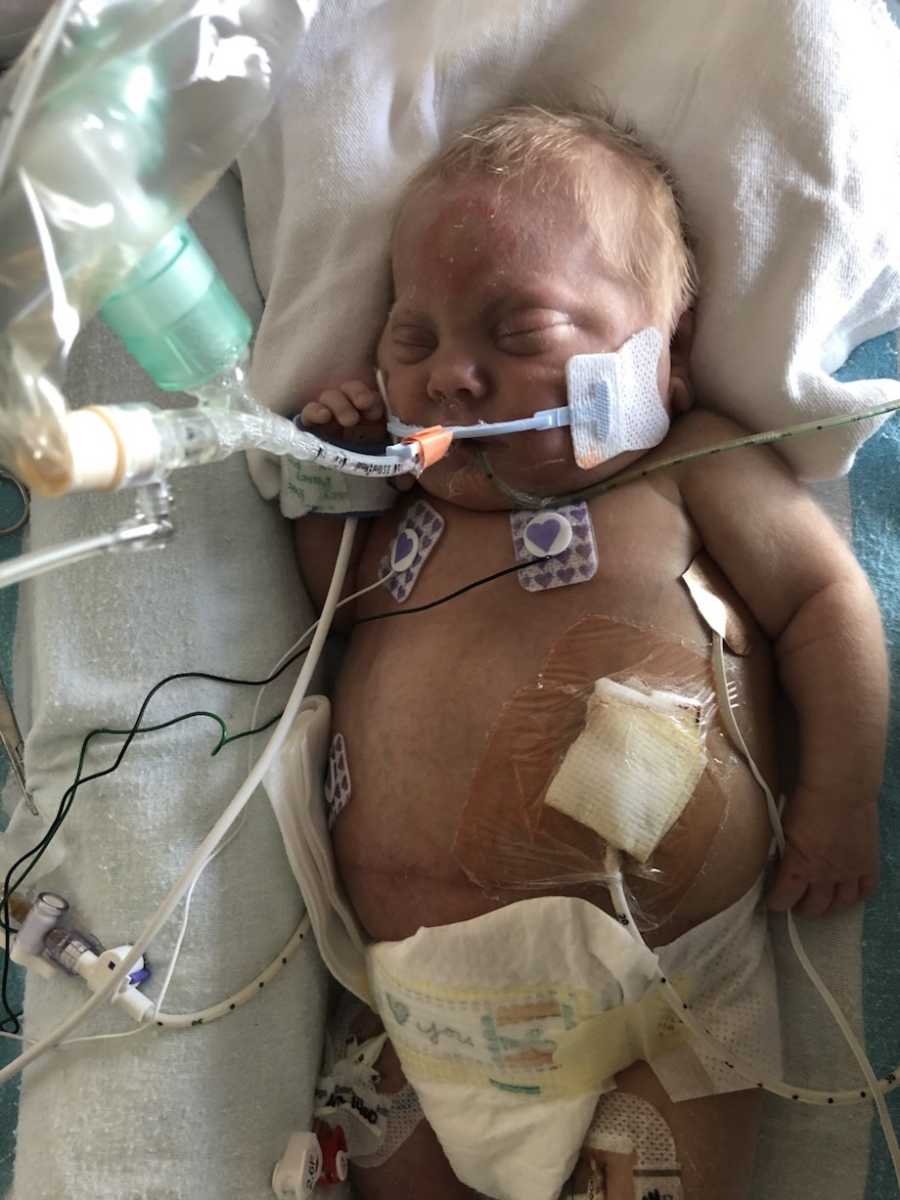
By the next day, the doctors agreed on surgery, as there seemed to be some sort of block or narrowing in his bowels. Oliver had exploratory surgery and the surgeons found a narrowing in the intestine from scar tissue build up. They were able to remove the damaged intestine and placed a g-tube in for future feeds.

After Oliver’s intestine healed, he was able to start feeds again. He started tolerating more and more breastmilk and continued to grow! By the first week of June, both parents were allowed back in the hospital together. We spent time learning how to feed and care for Oliver. Due to his extended hospital stay, he had blood clots caused by the PICC lines and required shots twice a day. We were finally discharged after 105 days!

The NICU is not for the weak. There are minute to minute changes, ups and downs, and curveballs all around. We are so thankful for the medical team and all of our family and friends who supported us. Oliver has over ten specialists we follow up with and this is only the beginning of Oliver’s story.

Kabuki Syndrome is a rare syndrome that affects about 1 in 32,000. We were in disbelief and completely blindsided. We were told common symptoms of Kabuki include unique facial characteristics, mild to moderate delays, heart defects, and a list of other concerns. The fact that there happens to be a genetic doctor in our healthcare system that is familiar with Kabuki Syndrome was fate. Once Oliver was born, we began to look and piece together what might be caused by his syndrome. This information was very difficult to process just hours before meeting Oliver and I often wonder if it stole my joy. However, with the small 10% survival rate, we were overcome with joy the moment we heard his first cry and continue to fall in love more and more every day, if that is even possible.”


This story was submitted to Love What Matters by Amanda Nihem. You can follow their journey on Instagram. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more amazing stories about babies beating the odds here:
Please SHARE this story on Facebook and Instagram to encourage other parents to cherish these little moments.

