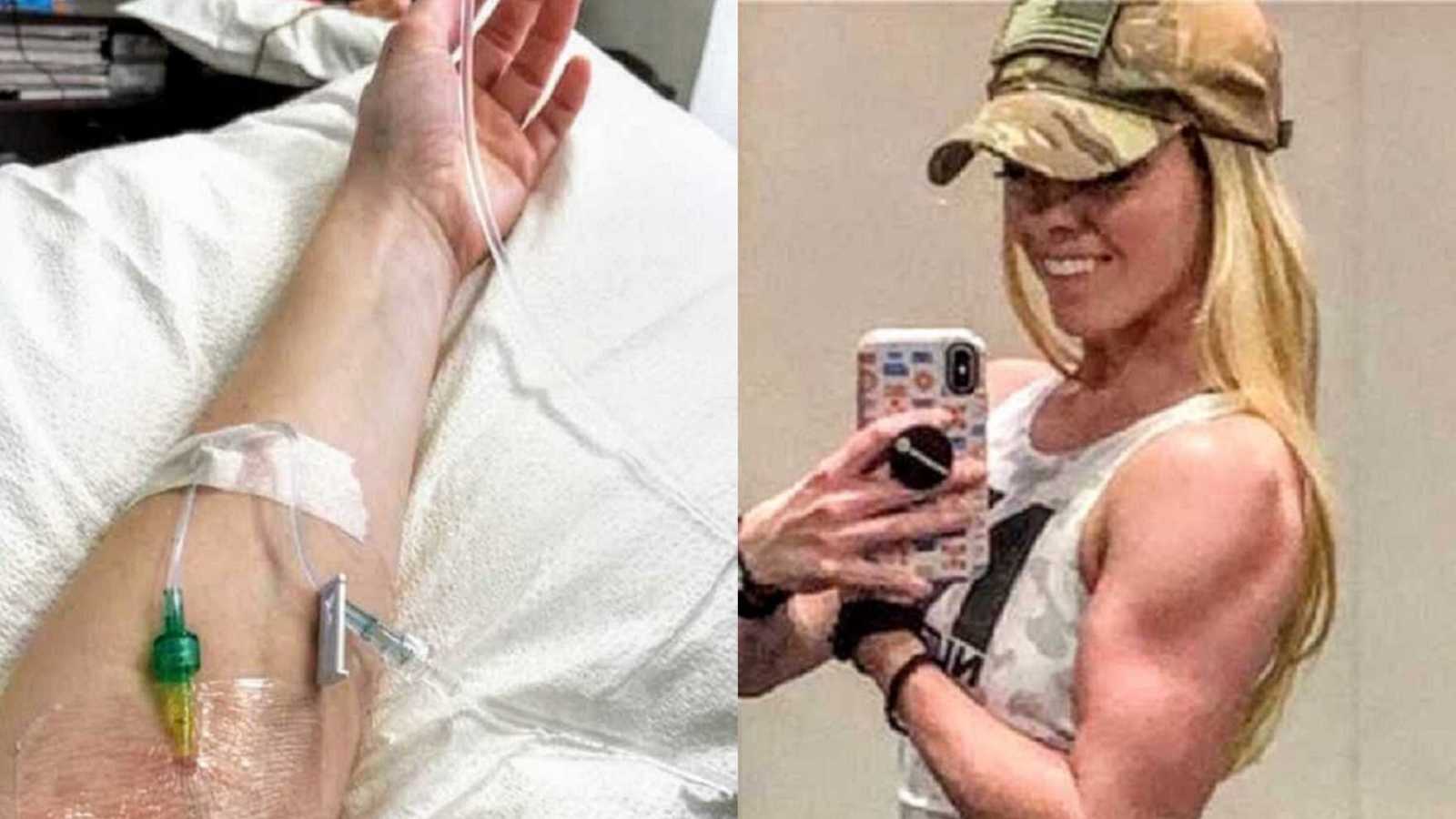
“In the beginning of 2013, I was 20 years old studying abroad in England, working out seven days a week, playing college soccer, and doing CrossFit. I was 130 pounds of muscle. Strong, healthy and in shape, which is the state I had been in my entire life.

When I moved back to the United States in July 2013 to finish college, I started to cut back on the heavy physical activity because I began developing some minor aches and pains. What started out as shooting pain in my shoulder progressed into throbbing pain in my wrist, and swelling in my elbow to the point of not having full flexion or extension. At this point, I did what any other college student would do, and turned to WEB MD.
I called my Mom who is a nurse and told her I thought I might have something called fibromyalgia to which she responded with, ‘You need to stop working out so much. Take some Advil and rest and you’ll be fine.’ But a few months later in October of 2013, after taking Advil and shrugging it off, I was bartending and noticed it was a little colder in the bar than usual and when I couldn’t feel my hands, I looked down to see half of my fingers had turned completely white. I later found out this was known as ‘Raynaud’s Phenomenon.’ This time, there was no shrugging it off. My Mom knew I needed to see a Rheumatologist because something was clearly going on.

I didn’t have many medical issues growing up so seeing a specialist was new to me. I was excited to hopefully get some answers about these symptoms. Was the pain connected to my fingers going numb? Was this all in my head, or was I really coming down with something? The doctor had sent me for some blood work before my appointment and when she walked in I thought I was going to hear the spiel. ‘This is what’s wrong with you, this is how we are treating it, you’ll be good, etc.’
Unfortunately, the doctor walked in and sat down and said, ‘So Christine, you’re blood work is definitely not normal. I know you’re experiencing pain and swelling, your levels are off but I don’t know what’s wrong with you.’ The disappointment was unreal. I remember walking out and saying to my mother, ‘How can she not know what it is? She says it’s a rheumatology issue but can’t pinpoint it? Isn’t that her job?!’ I was defeated, but my Mother made an appointment with a specialist in Manhattan she went to years prior for a second opinion.
A few weeks later, with my blood work in hand, I met this new doctor with an open mind. At the end of the appointment, I finally had a diagnosis: Mixed Connective Tissue Disease. It is a disorder that contains symptoms of various other diseases such as lupus, scleroderma, myositis, and Raynaud’s phenomenon. Joint pain and swelling can also occur. The diagnosis fit like a glove and he prescribed me some medication to try to alleviate some of the symptoms. I continued with my normal schedule at school for my senior year of college, class, gym, study, sleep and everything seemed to be going well. The medication started making me nauseous so the doctor told me to switch to one pill a day.
Just a few short weeks later, I started to feel extremely sharp chest pains. Every time I took a breath, it was like someone placed an anvil on my chest and were squeezing my lungs as hard as they could. I called the doctor immediately and he said I had Pleurisy, a condition in which two large, thin layers of tissue that separate your lungs from your chest wall becomes inflamed causing extreme pain while breathing. Super convenient, right? Since we have to breathe to survive and all.
He prescribed me some medication and that subsided. A few months later at the end of May 2014, my health took a drastic turn for the worse. I went to being fairly healthy with manageable symptoms to constant pain, sleeping 16+ hours a day, eating twice a day, high fevers, and I could barely make it 200 feet from my parked car to the classroom without feeling like I was going to collapse. I would finish class and go straight to the hospital to get tests done at night only to return to school in the morning to try to finish my semester. My parents knew they needed to get me home, but I wanted to finish school. I managed to make it through the graduation ceremony, went out to lunch, and slept for the entire rest of the day and something just didn’t seem right. I knew I couldn’t keep living like this. The next day, my parents packed up my entire apartment and we went back to Long Island.

Upon returning home, we went to the ER and I told them my very long list of symptoms only to be met with, ‘You’re going to be fine, just go home and rest.’ I felt like I was a prisoner in my own body and these doctors and nurses were telling me I was fine. After a week of the continued agony of high fevers and pain, I remember sitting on the couch, looking at my Mom and saying, ‘Mom, I need help. I can’t do this anymore.’ She took me to Urgent Care, where they took my vitals. My temperature was 102 and my resting heart rate was 155 beats per minute (bpm). They told me they would call an ambulance to take me to the hospital right away.
So, there I was, back in the ER, sicker than the previous visit and they were still hesitant to admit me. Again, we were met with, ‘We think everything is okay, we can give you meds to make the fever go down.’ You name it, we heard it and it was beyond frustrating. Luckily, my family had friends who worked in the hospital and we had to PULL SOME STRINGS just to get me admitted. After sitting in the ER for close to 8 hours, I was finally placed in a room upstairs when I doctor came in and looked at my chart and said, ‘I really don’t know why you’re here, you’re fine.’ All I could do was close my eyes and cry into the pillow. Fine? How could he say I was fine? Every day new symptoms appeared and I felt like a helpless shell of who I once was.
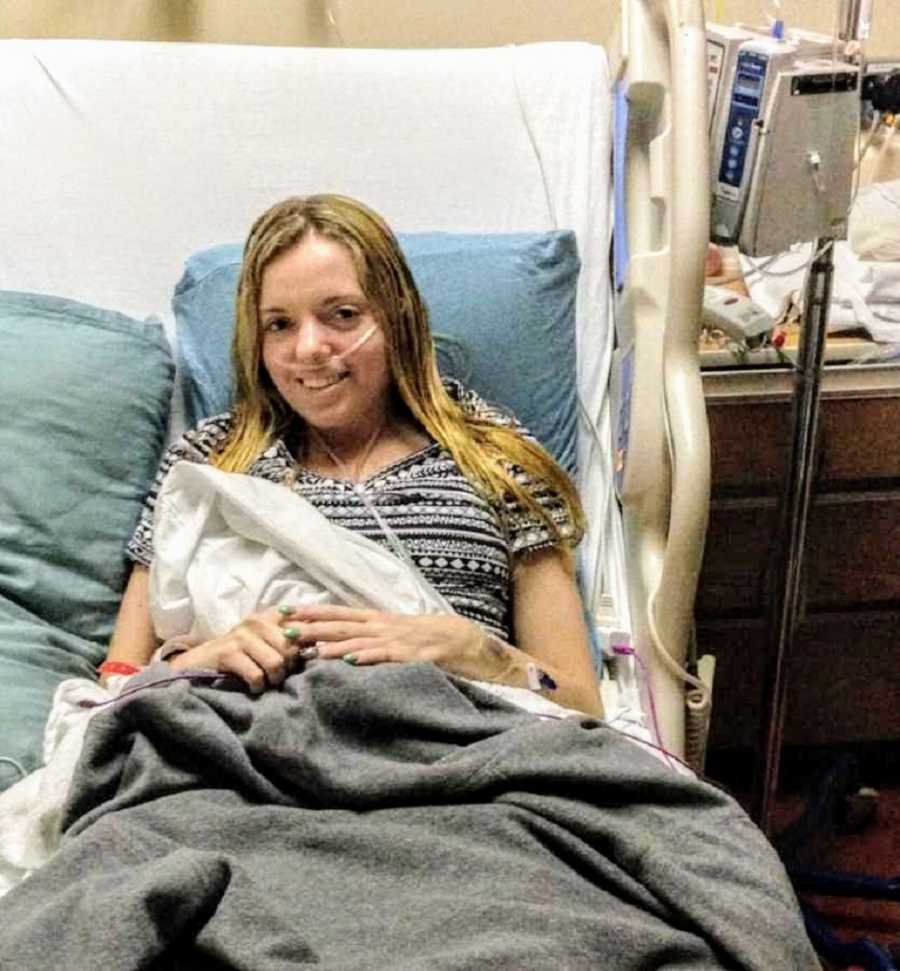
The next 10 days in the hospital were straight misery. The nurses drew so much blood I became anemic, my body retained all the saline they gave me to the point where my stomach was 40 inches around and I had to refuse the IV after day 7. I had moved so little that I could only lift my arms up to feed myself, I couldn’t get up or walk without assistance. I was still spiking fevers daily, and they sent me for every test under the sun with no diagnosis in sight. On day 9, we still had no answers.
I was depressed, sleep deprived, irritable, absolutely miserable, and I wanted to crawl into a hole and disappear forever. That afternoon, a group of doctors huddled at the end of my bed and I vividly remember overhearing them say, ‘She’s so incredibly sick, we just can’t figure out what’s wrong with her but she isn’t going to make it to the end of the summer.’ I remember sitting there thinking, ‘This is not possible, I just want to get over this and go back to living my life. I will not let whatever this is kill me.’ My parents knew something had to change if I was going to survive whatever was attacking my body. They managed to have me discharged and got in touch with my Rheumatologist who was at a conference overseas. He flew home on a red eye and opened his office early to see me the next morning (he’s the real MVP).
There I was, all 90 pounds of me sitting in the office in a wheelchair, high on a fever, so nauseous and dizzy I could barely see straight. After what felt like an eternity of the doctor flipping through my charts, he finally had an answer. ‘You have Lupus. It’s a fairly unusual case and it is affecting your muscles. Your muscle enzyme levels are close to 6500 and they should be between 26-100.’ I knew I had to have had a confused look on my face. Lupus? I really didn’t know anything about it other than that my previous diagnosis shared some symptoms. But at least we could move forward now. (Lupus is s a long-term autoimmune disease in which the body’s immune system becomes hyperactive and attacks normal, healthy tissue).

After a quick chat, my doctor sent me a few blocks away to an Oncology office to start treatment that day. Every day for three days, I would receive 1000mg of IV steroids and on the third day, I would also receive a chemotherapy infusion of a medication called Rituxan. Although the word chemotherapy scared the life out of me, I was down to try anything to feel the slightest bit better. The steroid and chemo treatment went well and besides a little pain in my chest on and off, it was bearable. Or so I thought.
Six hours after returning home, I experienced the worst pain I had ever felt in my entire life. I spiked a 104 fever and was on the couch writhing in pain, grunting, and moaning, begging for it to stop. I felt like someone had grabbed a hold of each arm and leg and tried to rip my limbs off while having a giant weight crush my body at the same time. Even after some Tylenol to kill the fever and a cold shower, the pain lasted for twelve hours. I hoped this would only be a one-time occurrence, but after my second chemo treatment in the middle of July, it was hell all over again. Luckily, I didn’t need to get another infusion after that for six more months and that one was a more pleasant experience.
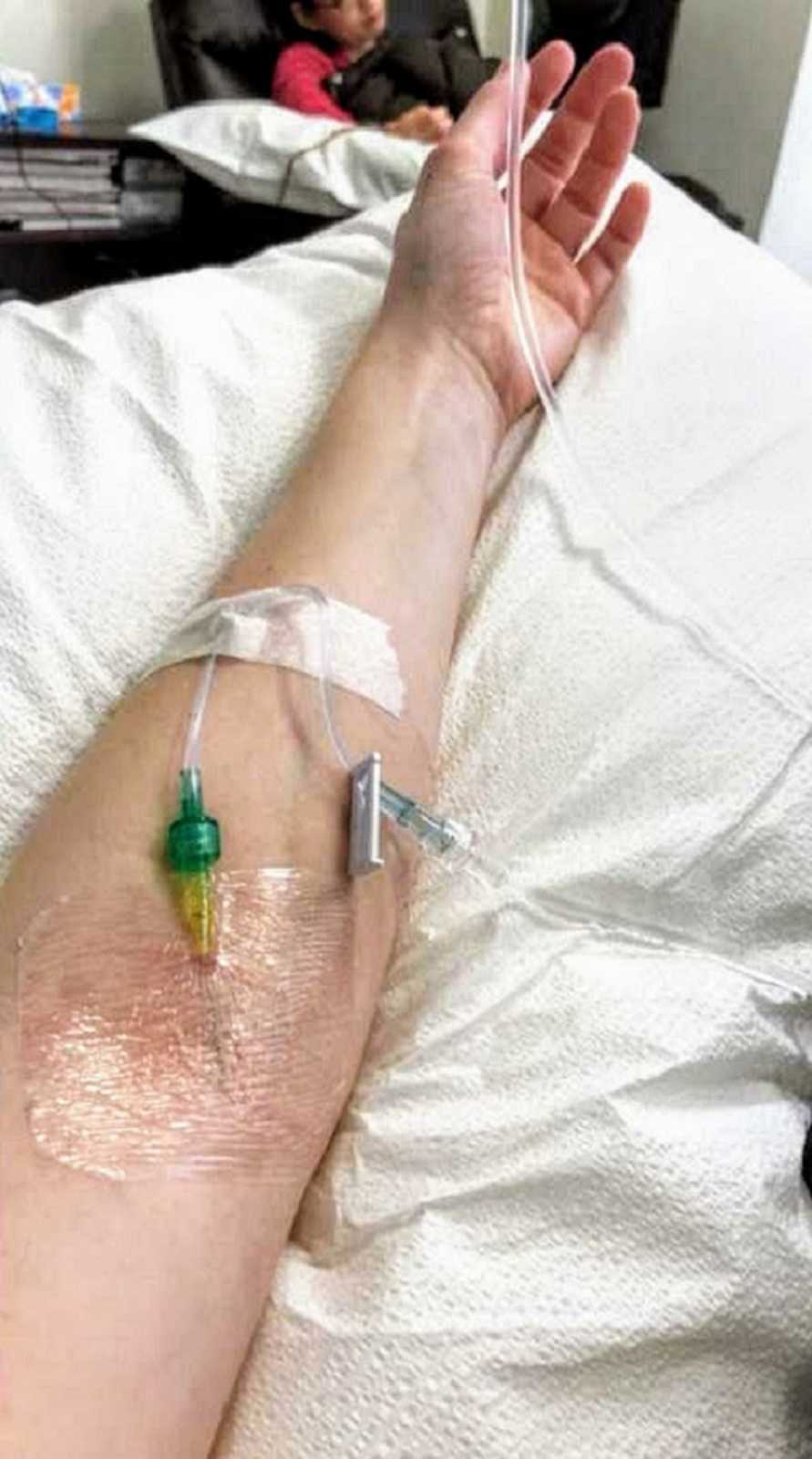
From the middle of July to October, I spent a lot of time researching Lupus and takings steps on the road to recovery. I was unable to do very much on my own but with some PT and help from my family, I slowly started getting into the swing of things. I was able to walk on my own, wash my own hair, and put my clothes on without help and it felt amazing. Unfortunately, because of the trauma my body went through, I lost all my hair and had to shave my head. As someone who has always had long hair this was a huge blow to my self-esteem. But hey, Brad Pitt and I had the same haircut for a little bit!

In the new year, I was 1000% determined to get right back to where I used to be because I knew Lupus was only a minor setback. At my checkup in December, my doctor was absolutely amazed with my bloodwork results. For as sick as I was, he could see zero residual damage from my life-threatening lupus flare. There was one major factor that played a role in my outcome with this disease. He said, ‘If you weren’t as fit and muscular when you came into this battle, there is no way you would have made it out alive the way that you have.’ That small statement lit a fire in me. I knew my next step was to become the strongest version of myself possible.
After being cleared to go back to the gym in January of 2015 I slowly started to attempt to build my strength by lifting very light weights and walking on the treadmill. In April 2015, a few short months after returning to the gym, I ran my first Obstacle Course Race ever which was the Spartan Beast at Mountain Creek NJ. I had signed up to volunteer to see what Spartan Race was all about, but after my shift ended at 2 p.m., I decided that I would regret if I didn’t at least try to attempt it. I was unprepared, dehydrated, and not properly dressed for a 13-mile race through the mountains, but I knew I wanted to prove it to myself that Lupus would not hold me back.


I crossed the finish line bruised, bleeding, exhausted, and hysterical. Since then, I have run 50+ Obstacle Course Races including the OCR World Championships. Over the years, I rejoined CrossFit and regularly run and lift weights at the gym. As a result of my hard work and dedication, I was able to fulfill one of my life long dreams. In 2018, I became a New York City Police Officer and was one of the fittest women in my academy class. I can proudly say, I am the strongest I have ever been and I don’t plan on stopping any time soon.


After my Lupus battle, I was only 90 pounds of skin and bones and I couldn’t look at myself in the mirror without breaking down. I just keep repeating to myself, ‘This isn’t permanent, you will get through this.’ A little over five years later, I am 125 pounds of muscle and I can hold my high with confidence and be proud of everything I have accomplished. Today, my Lupus is much more manageable with small flares here and there. I am the strongest I have ever been and I believe the stars are the limit as to what I can achieve.

Often, I think back to the day when the doctors said I wouldn’t last much longer in the hospital and I feel blessed to be where I am today. For those of you out there battling Lupus, I know it is not easy. We all have days where we feel like we are alone and we have no one to turn to. We feel as though things will never get better because no one understands how we feel or our medications are just not working the way that they should. Do not give in to this disease and its symptoms. It will be an uphill battle but I promise you, you are capable of crushing every obstacle it places in your path.
Please, please, please do not lose hope. I am here for you and you have friends, family, and thousands of Lupus warriors across the world on social media who can be a shoulder to lean on and your own personal cheering squad. No matter what, stay positive and remember, you are in control of your life and this disease. Also, if you are reading this and you know someone battling Lupus, please reach out and let them know you are thinking of them. The smallest gesture can go a long way to brighten someone’s day. Although every battle is different, it is something no one should ever have to fight alone.”

This story was submitted to Love What Matters by Christine Galgano of Kings Park, New York. You can follow her journey on Instagram. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more about chronic illness:
Do you know someone who could benefit from reading this? SHARE this story on Facebook with family and friends.