“I can’t help but smile as I picture myself drawing up my life plan as a teenager. I was going to finish college and grad school, travel the world, then meet the man of my dreams and be married by age 27, start having kids by age 30, and finish having 3 or 4 children by age 35. But, as luck would have it, I had 10 extra years to travel the world before I finally met the man of my dreams and married him at age 37. If I had to wait that long to get married, surely I wouldn’t have to wait that long to have children, right?

Wrong. So far, my husband and I have now been going through infertility for about 4½ years. What I didn’t know at the time, of course, was that not only would we never get pregnant on our own, but that our insurance would never cover the many expensive infertility treatments needed. We have gone through two failed intrauterine inseminations, five egg retrievals (three of which were failures), a clinic change, an apartment move to afford in-vitro fertilization (IVF), two failed frozen embryo transfers, a surgery to remove both blocked fallopian tubes (caught way too late), and a diagnosis that would take us to Mexico four times for reproductive autoimmune treatments.
I hadn’t realized at the beginning of this journey that infertility would be a full-time job on top of my already full-time job. Between researching the right reproductive endocrinologist (RE) and embryo lab (they aren’t all created equally), and finding the right medication protocol, supplements, tests, blood draws, procedures, appointments, consults, etc., I felt like I was getting another master’s degree in infertility (or a doctorate depending on the day), as there is just so much to learn and understand. Not to mention the fact that you’re asked to be your own doctor at home by ordering, preparing, mixing, and injecting your medications, usually with not much more than having seen an instructional video or pamphlet.
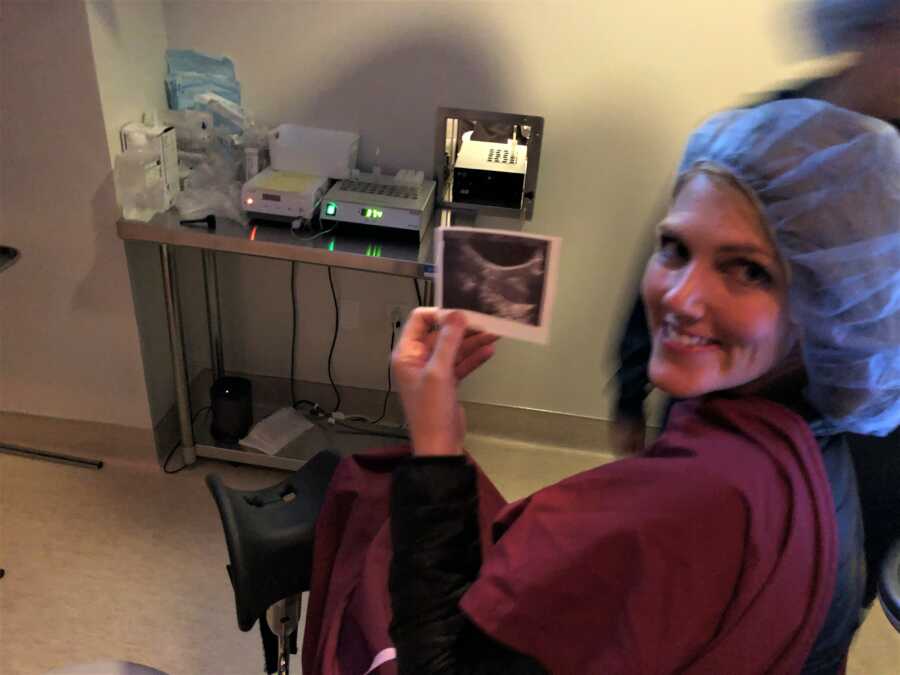
If I had to explain infertility in just a few words, they would be: exhausting, heart-wrenching, and grueling. My ‘vending machine theory’ is that, as a society, we expect to get out what we put in—you feed that vending machine your crispest dollar, push A2, and out comes your Tropical Skittles. With life, you finish college, you’re handed a diploma; you work out every day, you start to tone up; you save enough for your dream car, and soon you’re zipping around town feeling the wind in your hair. But the infertility vending machine is a different, brutal monster, one for which you put in tens of thousands of dollars, only to be handed back angst in just about every life category: emotionally, physically, spiritually, socially, sexually, professionally, and financially. You sacrifice everything and fight ferociously for a baby, with little control and no guarantees.
One in eight couples will experience infertility, and yet our society doesn’t openly discuss or educate on the topic. It’s a taboo subject, brushed under the infertility rug because it’s looked at as a ‘women’s issue.’ This is an ironic misconception, as men account for half of infertility problems. Even though the American Medical Association acknowledged infertility as a disease a few years ago, most insurance companies still won’t cover it in any meaningful way. Resolve.org works to promote the infertility-coverage movement and gives tools on how to go to your company to advocate for yourself. I did this at my last company, and my HR director declined the notion, saying, ‘We don’t have a need for that right now.’

The fact that most insurances dismiss infertility as a medical condition worthy of coverage just like any other medical condition only perpetuates the silence and shame women often feel around the subject. Assisted reproductive therapies, like IVF, are not elective treatments. They are often the only means by which people can start their families. And almost half of individuals who need these treatments don’t have access to them, either because their insurance won’t cover it or they can’t afford it out of pocket. This is a human rights issue. And to those who say, ‘You should just adopt,’ well, private adoption is often even more expensive than IVF.
These financial stressors only contribute to the pool of other stressors. My husband and I both happen to be therapists. Initially, I thought that being a therapist might give me some sort of upper hand with the emotional turmoil of infertility, but of course it’s easier to provide the guidance than to receive it when you’re in the raging storm. I was stuck in the emotional pitfalls the infertility process brings, despite all my learned coping skills. I felt all the common feelings of hopelessness, depression, and anxiety, as well as jealousy and resentment toward those for whom pregnancy seemed to come easy. Eventually, I sought therapy and infertility support groups to help me cope with all the loss and trauma infertility had brought over the years.

At the beginning, like many, I assumed our first IVF egg retrieval would be our last. We had four embryos that made it through the 5-day post-fertilization watch period and would then be sent out for preimplantation genetic testing. Such testing is recommended for women over 35, as there is a higher rate of chromosomal abnormality. If the embryos come back abnormal, it means they would have more than likely miscarried. All four of our embryos came back abnormal. I was devastated. Originally our diagnosis was male-factor infertility (which later resolved through supplementation), but I was starting to realize that egg quality was probably a key player too. I worried we’d never have a chance at having our own children.
For our second egg retrieval, we had five embryos sent out for testing. Thankfully, one came back normal, which gave us hope. But at this point, we were ‘banking’ embryos, meaning we would keep doing egg retrievals until we had at least four normal ones. We wanted at least two children, and they say you need at least two embryos for every one child you want, to account for the possibility of the embryo not implanting.
On our third cycle, we only had three embryos go out to genetic testing, and all came back abnormal. More devastation. At this rate, it would take us years to bank four normal embryos, so for our fourth egg retrieval, we decided it was time to switch things up, starting with a new clinic, a new medication protocol, a diet geared toward helping with egg quality, and the addition of acupuncture and extra human growth hormone (HGH) which can help with egg quality. I also cut out all beauty and household products with parabens, fragrances, BPA, etc. (which I’d read can impact egg quality). For 3 months, I eliminated sugar and all processed foods. I drank hot Chinese herbs that tasted like gardening soil and waved a burning moxibustion stick over my meridian points twice a day to increase antioxidant defenses. My acupuncturist told me not to eat or drink anything cold or raw like salads as they would take more blood to digest, stealing it away from my ovaries where it was needed the most.
Those three months of prep were during the summer when it was too hot to be drinking room-temperature water (which I did anyways and which could never fully quench my thirst). One day at work, I forgot my water bottle and had to use a cup with the ice-cold cooler water. I would swish the water around in my mouth first to warm it before swallowing (making me feel like I was at a dental cleaning). In my purse, I would always carry my own mini fragrance-free hand soap. When we did our taxes, I used latex gloves so I wouldn’t expose my hands to the BPA in the receipts. Infertility can make you feel and act a bit paranoid. I felt like every little thing I did or didn’t do would somehow impact our future family. It was a lot of pressure and stress, but I also knew for me, emotionally, I needed to do everything within my control so I could walk away with no regrets.

I remember we were getting close to starting the 10-day stimulation medications for our fourth egg retrieval and I was counting down the days until I could finally eat what I wanted, put ice in my drinks, and use my old beauty products again. As I walked into my weekly acupuncture appointment, I got an email saying our overseas infertility meds (which should be arriving any day) were held up in customs in England for at least two more weeks, which meant our cycle would be delayed another month.
The acupuncturist placed the needles and then left me in the dark for the next 45 minutes. As I laid there on my back, a human porcupine, being perfectly still as to not jostle the needles, I allowed myself to absorb the impact of this news. Another month without sugar, or McDonald’s? Another month of daily HGH injections, acupuncture, moxa, and swishing cold water in my mouth? Another month without a baby. It was another setback. Another loss. Another infertility hit.
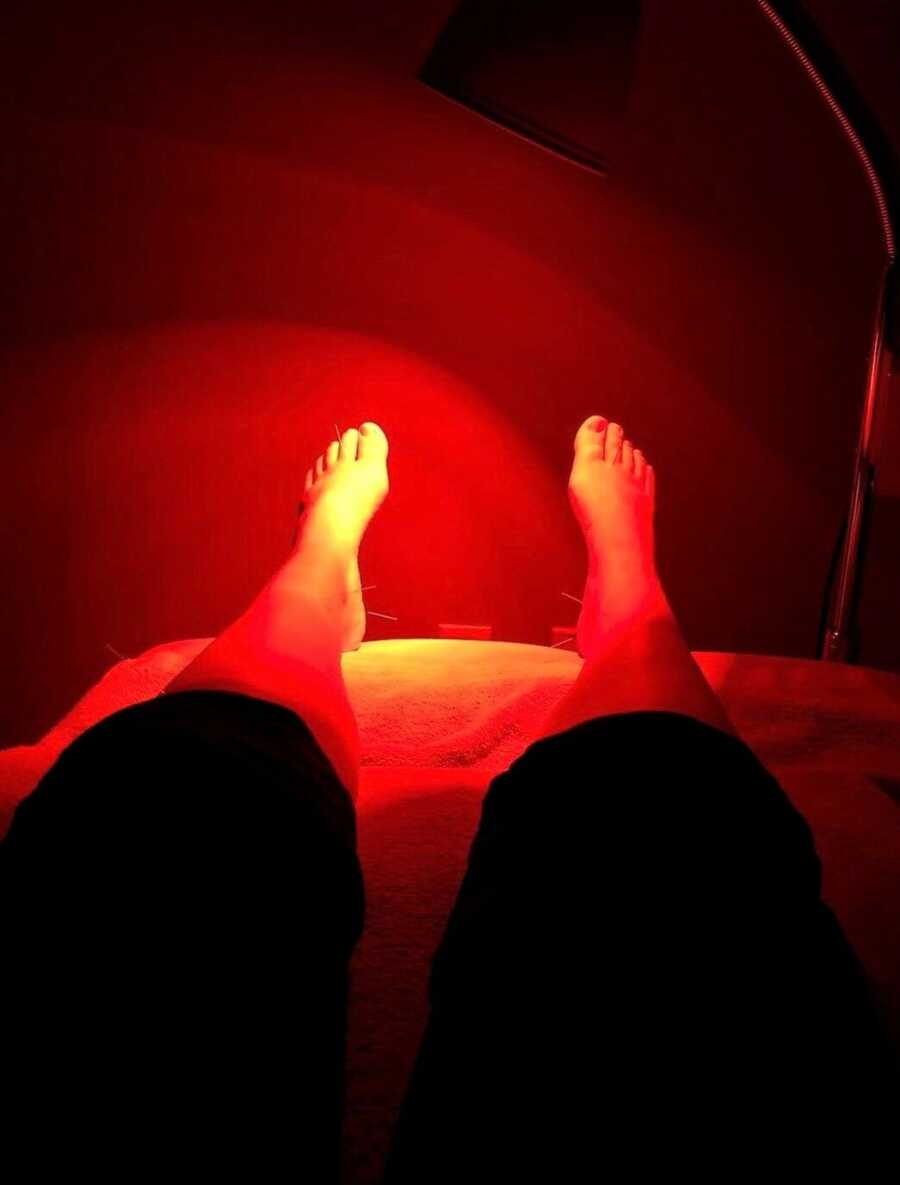
I couldn’t stop the tears from pouring down the sides of my face. The worst part was that I couldn’t move my hands to wipe the tears, as I had needles sticking out between my thumb and index finger. My tears had nowhere to go but to pool into my ears, making them tickle like crazy. I was sniffling so hard I could barely breath out of my nose. I couldn’t breathe, itch my ears, wipe my tears, blow my nose, or move my body. I had lost control of everything in my life, and I felt completely helpless and defeated. The only way I could really compose myself was to acknowledge the truth: for whatever reason, we weren’t supposed to do an IVF cycle that month. I just had to grieve it, let it go, and move forward.
But that extra month of prep may have paid off, as miraculously we had seven embryos go out for testing, of which three came back genetically normal! Presumably, all the changes I had made had worked, and we were now home free to finally move forward with a transfer!
A few months later we transferred our first embryo and it failed to implant. I took some time to emotionally heal before we tried again. A couple of weeks after our second embryo transfer, we were sitting on the bed when we got the final-result call. We were officially not pregnant. I felt completely shocked and shattered. I was convinced this couldn’t happen to us again, and yet here we were with two back-to-back miscarriages. We’d just lost two of the four embryos we’d worked so hard to bank over the past 3 years. To me, we’d just lost half of what our family could’ve been.

My husband held me as I sobbed so hard that I could barely breathe at some points. Then I’d just lie there, exhausted, and let my mind go numb. Then the wave of grief would hit me all over again. It was like I was treading water in the cold, black ocean, barely able to keep afloat when another 20-foot wave of realization pounded over me. No words were spoken between us. There was nothing to say.
I looked across the room at the bulletin board propped up on my dresser. I had typed up positive mantras, affirmations, and faith-promoting quotes to read over the past few months—a daily reminder of what I wanted and what I felt I could have with enough faith. I calmly walked over and picked it up. I opened the sliding balcony door, and with all my might, flung it over the balcony and listened as it crashed to the ground of the backyard below. My husband’s eyes got wide, probably wondering if I’d finally lost it. But it felt great to let some of that aggression out.
Those next few days I didn’t want to do anything. I was mad at God and the world. Every second, another woman was discovering an ‘oopsie pregnancy,’ while it felt like I had done nothing short of learn Olympic-level aerial gymnastics to get pregnant—and it still didn’t matter. We had spent $4,000 on an endometrial receptivity biopsy to take the extra precaution of checking when my uterus was most receptive in the month, and it still didn’t matter. A doctor had carefully placed a catheter with an already-formed, genetically normal embryo directly inside my uterus (eliminating dozens of lead-up steps where something could’ve gone wrong), and it still didn’t matter.

A few months later we did a last-ditch, fifth egg retrieval to try and salvage our lost embryos, but of the three embryos we got, all came back abnormal, despite doing the same preparation and protocol as before. It was one unfair blow after another, and the build-up of losses was starting to feel suffocating.
Thankfully, our very attentive RE suggested more tests and then a laparoscopic surgery, which found both my tubes to be blocked. Despite prior tests which showed my tubes to be clear, they in fact weren’t, and this was more than likely the cause of the failed embryo transfers.
With my tubes removed and no way to get pregnant naturally, no more money to do another egg retrieval, and only two embryos left, we were leaving no embryo unturned, so to speak. We consulted with a reproductive immunologist and discovered autoimmune issues that could have also contributed to the miscarriages. It was recommended that we do a specific autoimmune therapy which is only available internationally, so we traveled across the border to Mexico on four different occasions (thankfully, we don’t live too far from where we needed to go). I think our family was really questioning our sanity at this point (and I don’t blame them). But we did our homework and talked to enough people who’d had the procedure done safely and with success. The process consists of taking anywhere from 10-20 vials of my husband’s blood and then extracting the white blood cells and injecting them into my forearms (similar to TB injections), with the hope that my body would ‘acclimatize’ to his cells and not reject an embryo.

With the barriers of blocked tubes removed and autoimmune issues leveled out, we are cautiously optimistic for the next transfer. This process has taught me not to compare our story to others, because each story is unique. I’m working on enjoying the moment and appreciating what we do have. I’m continuing to learn that there are no guarantees in life and to be more open. I feel confident we will be parents even if it’s not in the original way we’d hoped. It’s an ongoing process, but I’m learning to trust, allow, and let go of the things that I can’t control.”

This story was submitted to Love What Matters by Emily Blank. You can follow her journey on Instagram. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this here:
Do you know someone who could benefit from reading this? SHARE this story on Facebook with family and friends.

