Trigger Warning: This story contains mention of child loss that may be triggering to some.
“My husband and I started trying to conceive almost 2 years ago in January of 2019. We were hopeful, excited, and thankful for our health. After 6 months of trying, we started to get nervous and I saw a doctor.
Within a few weeks, I was sitting in my RE’s office listening to him say, ‘You have two uteri (uteruses) and one tube. You will not be able to get pregnant naturally. Let’s talk about IVF!’ I had surgery on my tube, due to an ectopic rupture, but they had told us the tube remained open. However, my RE noted in the minute-by-minute surgery report, it specifically states the tube was closed. Doctors in the past had missed this. We were upset this mistake was made, but we were eager to move forward with IVF.
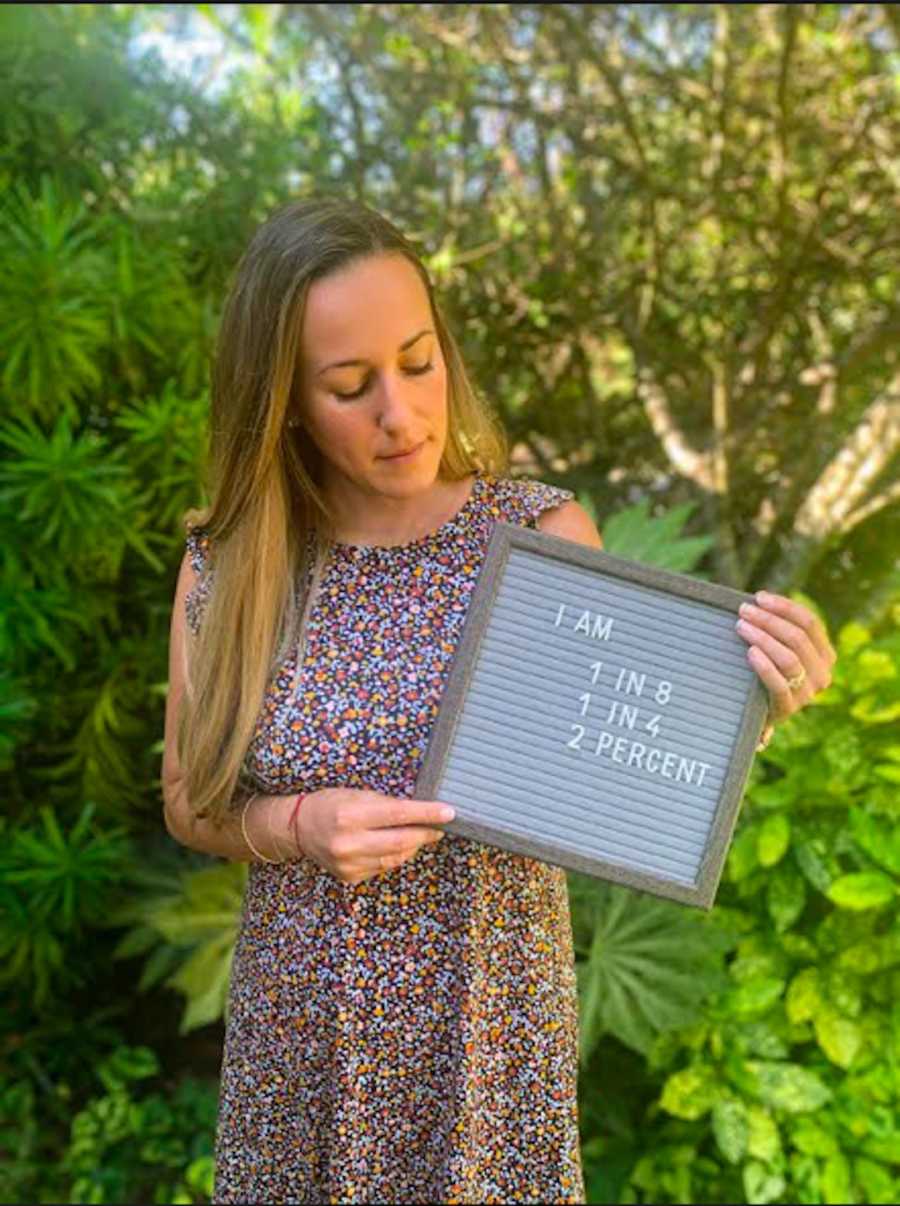

I was born with two uteri and the one attached to the working tube was not accessible. We didn’t ask many questions, just signed on the dotted line and thanked our RE. To be honest, we didn’t even grieve the loss of being able to conceive naturally. We started IVF right away and we were met with the amazing results of 12 PGS normal embryos! We let my body rest a month after the egg retrieval and then we transferred our strongest embryo in October of 2019. It worked!
I remember the fear that washed over me the first time I entered my RE’s office for my scan. I wondered, ‘Will the baby be in there? Will I hear the heartbeat?’ Thankfully, everything looked perfect. However, my RE reminded me, ‘This won’t be easy.’ With my anatomy, I was considered high risk. I felt robbed of any pregnancy innocence that one might have, ever after going through infertility treatments.

We graduated from the fertility clinic and I started to see my OB and MFM at UCSF. The pregnancy was hard from the beginning. I was high risk and seen almost weekly. I was constantly worried about the baby and how my body was doing. I refused to even go for a long walk until 12 weeks. When it came time to talk about prenatal testing, we opted in for all the testing California offers, despite our embryo being PGS tested. We received uncertain first and second-trimester screener results, which completely threw us off. We thought we were just being cautious, but we were not prepared for the feat we were about to face.
Weeks 13 through 16 of pregnancy were a blur. I was constantly waiting for phone calls from my MFM team. Thankfully, with each call, I was met with positive news. It seemed like everything had been ruled out and it was just my placenta hormones that were off. However, after all those weeks of living in constant fear, we wanted a diagnostic test done to confirm the baby was okay. At 16 weeks, we decided to do an amnio.
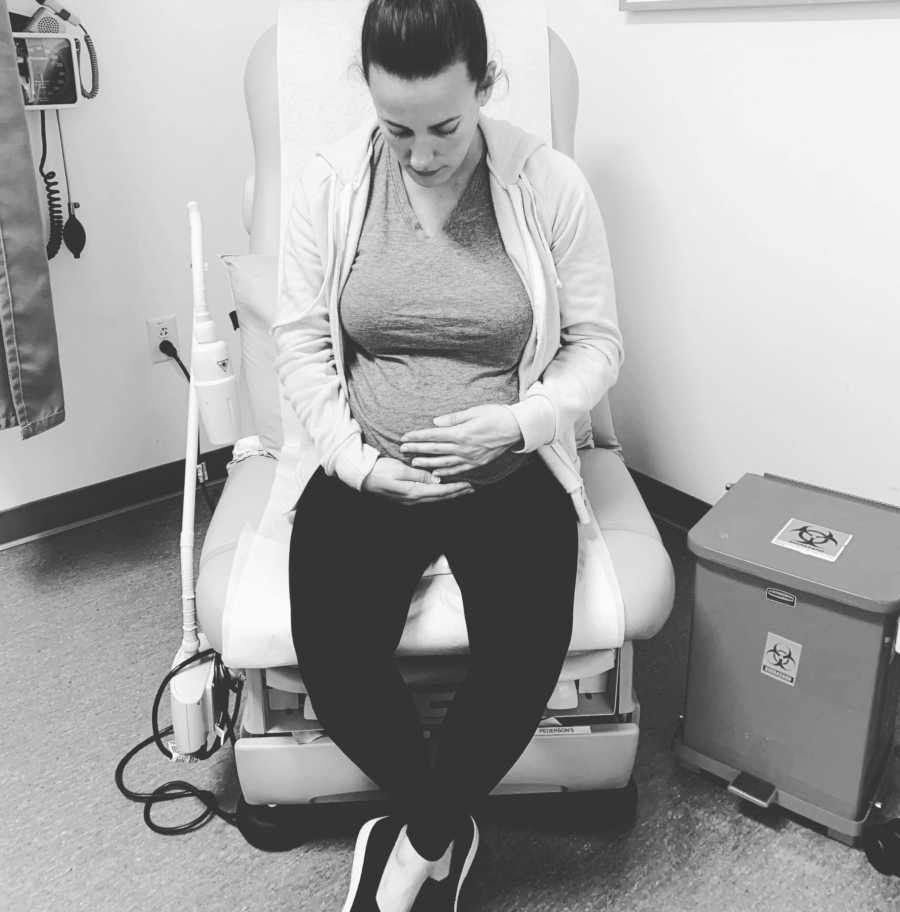
I was terrified. I remember sitting in the room and squeezing my husband’s hand as the needle went through my stomach and into my placenta. I was watching my baby on the screen the entire time, begging the doctor, ‘Please be careful!’ We got through it. Everything was okay, but that week of waiting for the results was one of the hardest times for me. Being able to feel your baby inside of you is a beautiful thing, but when you’re unsure if your baby is sick or not it becomes heartbreaking.
When I got the phone call that the amnio came back normal, I felt like I could finally breathe. We decided to announce our pregnancy on social media at 17 weeks and we were so excited. Until week 18 when I had an abnormal ultrasound. I went in, alone, for a cervical check. The tech started taking pictures and then got very quiet. She asked me, ‘Where is your partner?’ And then told me, ‘Please wait for the doctor.’
An hour later, the doctor came in and told me, ‘Your son is sick. We are going to run some more tests, but you should ask your husband to join you.’ My husband rushed right over from work and we began our 8-hour day at the hospital.
It will forever be one of the worst days of my life. I felt helpless. I could see my baby moving around on the screen, I could feel him inside of me, but I couldn’t help him. He seemed healthy to me. He was moving, but why wasn’t he growing the way we had hoped? From weeks 18 to 21, we did a variety of different tests. We did a fetal echocardiogram, a microarray, and an MRI. We met with a urologist, another MFM, the head of OB, and some more genetic counselors. By week 22, a Whole Exome Gene Sequencing test confirmed our worst nightmare. We would lose our baby boy, Cole, to a rare genetic defect.

Our diagnosis was given on a Thursday in March 2020. We confirmed delivery for the following week. It was the very first week of lockdown here in SF for the Coronavirus and, because of that, they couldn’t confirm my husband would be allowed in the room with me. That Saturday, before Cole’s delivery, I ended up in the Labor and Delivery emergency room. My anxiety had gotten to a point where I could no longer control it and I was diagnosed with adjustment disorder and heavily medicated. I honestly don’t know how I made it through. I could feel my baby inside of me and it was heartbreaking. Why was the universe doing this to us? We had fought so hard for our son. So many years filled with procedures, surgeries, shots, medications, and hope.
On Friday, March 20th, 2020, one week into the pandemic SIP, we lost our son at 23 weeks. It was a multiple day process. My husband was able to be by my side the entire time, but we had to fight for it. Hours spent on the phone with some of the top hospital admin trying to navigate how to make it possible. This pandemic was new for everyone and no one knew what to do. We were scared, overridden with grief, and in complete shock. My medical team dilated me on Wednesday using a spinal tap and laminaria sticks. We went home that evening and enjoyed the last few kicks of our baby boy. My husband had just started to feel him move.

On Friday morning, we went into Labor and Delivery. After some time, I was put to sleep due to my body being in danger. I had a septum that was making it hard for me to deliver. My baby boy and I went to sleep at the same time and I woke up without him inside of me. We had about an hour with Cole before we had to say goodbye. It will forever remain the most heartbreakingly beautiful moment of my life. We held him in our arms and cried. He will forever be our firstborn.
The weeks following the loss are still a blur. I could barely get out of bed. It’s hard to try and navigate how to deal with postpartum without your baby, while also grieving his loss and being stuck at home during a pandemic. It wasn’t until my first postpartum period came 9 weeks later I started to feel myself again. I started to gain hope.

We did PGD testing for the single gene defect on the remaining 11 embryos and we were left with sven healthy embryos. Hope. We had SO much hope. This is what kept us going. Losing our baby was hard. It was probably the hardest thing we will ever have to go through as a couple. I just remember thinking, ‘I am SO grateful for science and technology.’ Without it, we wouldn’t have been able to identify Cole’s defect. We wouldn’t have been able to test our remaining embryos to ensure we, and our future children, didn’t have to suffer a loss like that again. We wouldn’t be where we are today, which is one step closer to a healthy pregnancy and baby.
Since our March loss, I have been through three more transfers. Our transfers in June and November of 2020 resulted in negative betas. I remember being so hopeful our first time trying after the loss. Our first transfer worked, so why wouldn’t our second? Well, I was quickly sobered by the reality of a failed beta. After weeks of nightly shots and lots of hope, we got confirmation we lost our boy embryo. We were heartbroken but reminded this happens. It wasn’t anything to be too alarmed by.
Our doctor remained hopeful and advised me to take some time to rest. We then ran a few tests and did an HSC procedure to ensure everything was looking okay. A late loss can be very traumatic for the uterus so it was important for us to be safe, even if it meant more waiting. After a few more months we decided to move forward with another transfer. In November of this year, we transferred another embryo. Weeks of hormone injections, fear, anxiety, and hope lead us to our final beta day. Once again it was confirmed we had lost another boy embryo.
At this point, I decided I wasn’t willing to wait any longer. I wanted to dive right into another transfer. And that is what we did! My tests and procedures showed everything looked okay, so I continued the shots. I am currently in my fourth 2-week wait after transferring another beautiful embryo just 4 days ago. My body is tired, but we’re so hopeful. I am feeling hopeful, jaded, excited, and numb. After three losses and two failed transfers, it’s hard to imagine things working out. The truth is, I’m not terrified of it not working. I know how that feels. I know I can get through it. I am terrified of it working.


I don’t know what it feels like to go through a normal pregnancy. I don’t know what it feels like for things to work out. We have four embryos left and our hearts are still full of hope. My body, and our hearts, have been through the wringer. However, we’re still full of hope and gratitude. I feel it’s so important to keep pushing forward, keep reminding yourself that this fight will be worth it. And that, without IVF, many of us wouldn’t even be able to make it this far.
I’m hopeful that this next transfer will give us our rainbow baby. However, if it doesn’t, we have a plan. And that is what is keeping me pushing forward. That and this amazing community I have found. I have leaned on my fellow infertility warriors from the very beginning. It truly is the worst club with the best members. They have reminded me that this fight is worth it. IVF is hard, loss is crippling, and dealing with all during a pandemic is debilitating, but I won’t give up.”

This story was submitted to Love What Matters by Alyssa and Steven from San Francisco, CA. You can follow their journey on Instagram and Facebook. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Spread the love and SHARE this story on Facebook with family and friends.

