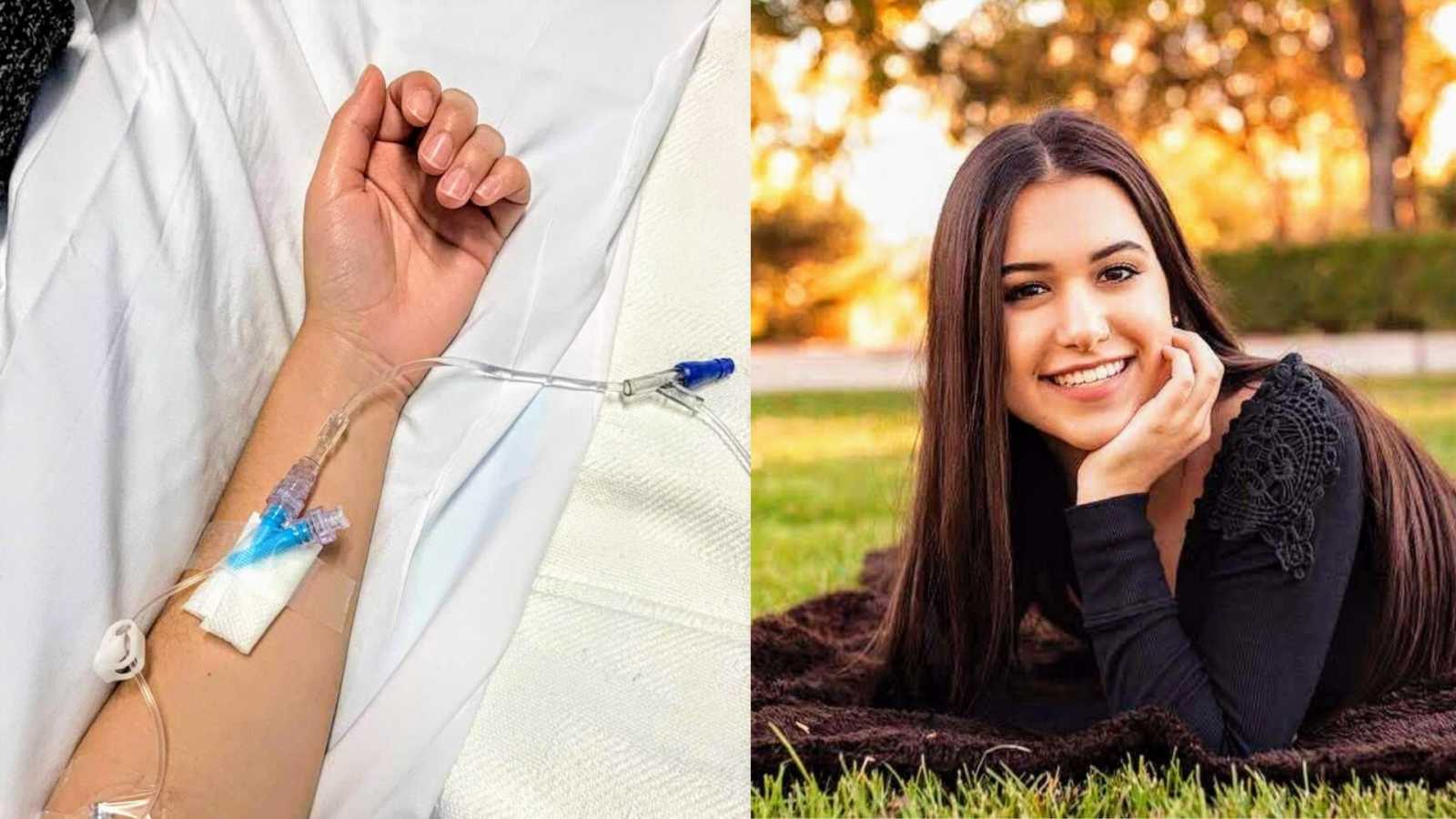
“I had traveled about 2,000 miles away from my home in Vegas to attend college with a full-ride academic scholarship. Last year, I was a sophomore and was taking my health and studies with sincereness. It was late October, and I was recovering from a long week. I decided to take it easy on Sunday and catch up on my rest. On Monday, I woke up and went to my 9 a.m. class. As the day went on, I started to realize something was wrong with my vision. Things seemed blurrier than usual and I couldn’t focus on anything far away. This was not normal, as I had always had 20/20 vision. I thought to myself, ‘Maybe this is just my blood sugar acting up – I didn’t eat very much yesterday.’ The next day, I started literally seeing double.
When I looked straight ahead, I could see fine. It was when I looked over to the right that I saw double. I was very troubled by this. I remember studying at my desk in my dorm, and looking over to my right to my roommate as she walked through the door. I literally saw two of her walk through the door, and that’s when I knew there was an issue.
Seeing double in my right peripheral vision lasted for eight consistent weeks, during most of which I had no idea what was going on. Eventually, I had to adjust and accept this as my new normal. My double vision was constant and didn’t go away. After about a week, I made an appointment at a local ophthalmologist. They scheduled me in with an optometrist, but thankfully she was a kind lady and promised to have the ophthalmologist look at my case as well. As I expected, I still had 20/20 vision. They took a few other tests. Everything came out completely normal.
The optometrist told me she suspected I may have something called myasthenia. She said I would need a blood test to check if I had it for sure, but that if I was experiencing any shortness of breath, I would need to check into the ER right away. This gave me some serious anxiety because I often did get short of breath at times. She also ordered me an ocular and brain MRI, just to be safe. In addition to this, she referred me to a neurologist’s practice she went to herself. When blood results came back normal, I almost canceled the MRI because I didn’t think I needed it. But, I went ahead and got it anyway to rule out anything else that might have caused the double vision.
I didn’t get in with the main neurologist at first. She was a nurse practitioner and did a neurological exam on me. Everything still came out normal. She suspected my eyes might need an alignment, but said that was the ophthalmologist’s expertise.
A little while later, I got a call early in the morning before class. It was the optometrist. My MRI results had come back, and things had taken an unexpected turn. She explained it looked like I had an 80% chance of having multiple sclerosis. ‘I know this must be a lot to take in,’ she said. I was shocked. I knew my double vision wasn’t ideal, but I wasn’t expecting a diagnosis to this extent. I didn’t even know that much about MS, but she said it affected my muscles and that a neurologist would better explain it.

I was ordered a lumbar puncture, better known as a spinal tap, to further investigate whether I had MS or not. During a spinal tap, a sample of cerebrospinal fluid is taken from your spinal canal. I looked up ‘what to expect during a spinal tap’ on YouTube, which was probably one of the worst things I’ve ever done. I read through the comments and people were commenting about how extremely painful the procedure was. This sent my anxiety up the wall.
I remember sitting in the waiting room with my dad, who had come in to support me, and trying to keep calm. I absolutely lost it when the doctor walked into the operating room. I lost all control of myself and burst into tears. The doctor read me the list of possible side effects while I was still crying, and I signed my name, still crying. The doctor left to give me a few minutes to gather myself before the procedure, and I remember laying on the table with the doctor’s assistant handing me a tissue. I had to hold still while the numbing shot went all the way into my lower back, and it was the weirdest feeling. But in no way was it ‘extremely painful.’ All I felt was a little pinch before I was completely numb. That just goes to show that you should never YouTube a procedure before you go in.
I was basically calming down from my anxiety attack during the whole procedure. I kept apologizing. ‘I never freak out like this,’ I told the doctor and his assistant about 15 times. They were both very kind, though. The doctor asked me, ‘So what’s the reason you’re having this procedure?’ I replied, ‘They think I have MS,’ to which he replied, ‘Well, I sure hope you don’t.’
Needless to say, I got out of the spinal tap procedure without an extreme amount of pain. In fact, the extreme amount of pain started after the procedure. Anyone who has a spinal tap also has the possibility of getting a spinal headache, which occurs when cerebrospinal fluid leaks through the puncture hole. If you have a spinal headache, every time you sit up, even an inch, you get an instant headache. Not a dull headache, but an extremely painful headache. I had to literally lay down flat for 4 days until I’d had enough and called the doctor. He told me to go to the emergency room and get a blood patch, so I ended up at the hospital, lying down in the ER’s waiting room while filling out the info sheet. I also almost puked from the pain, which I didn’t even know was possible.
In the emergency room, they gave me caffeine, Tylenol, ibuprofen, and an IV for hydration. It took my pain down from an 8 to a 4, but the pain was still there and I knew it would come back. Someone came to talk to me about the blood patch. It turns out there was a chance of getting another spinal headache from that procedure, and some other undesirable side effects. I decided to just wait it out since they assured me it wouldn’t last for longer than another few days. Thankfully, the pain went away within the next 3 days.
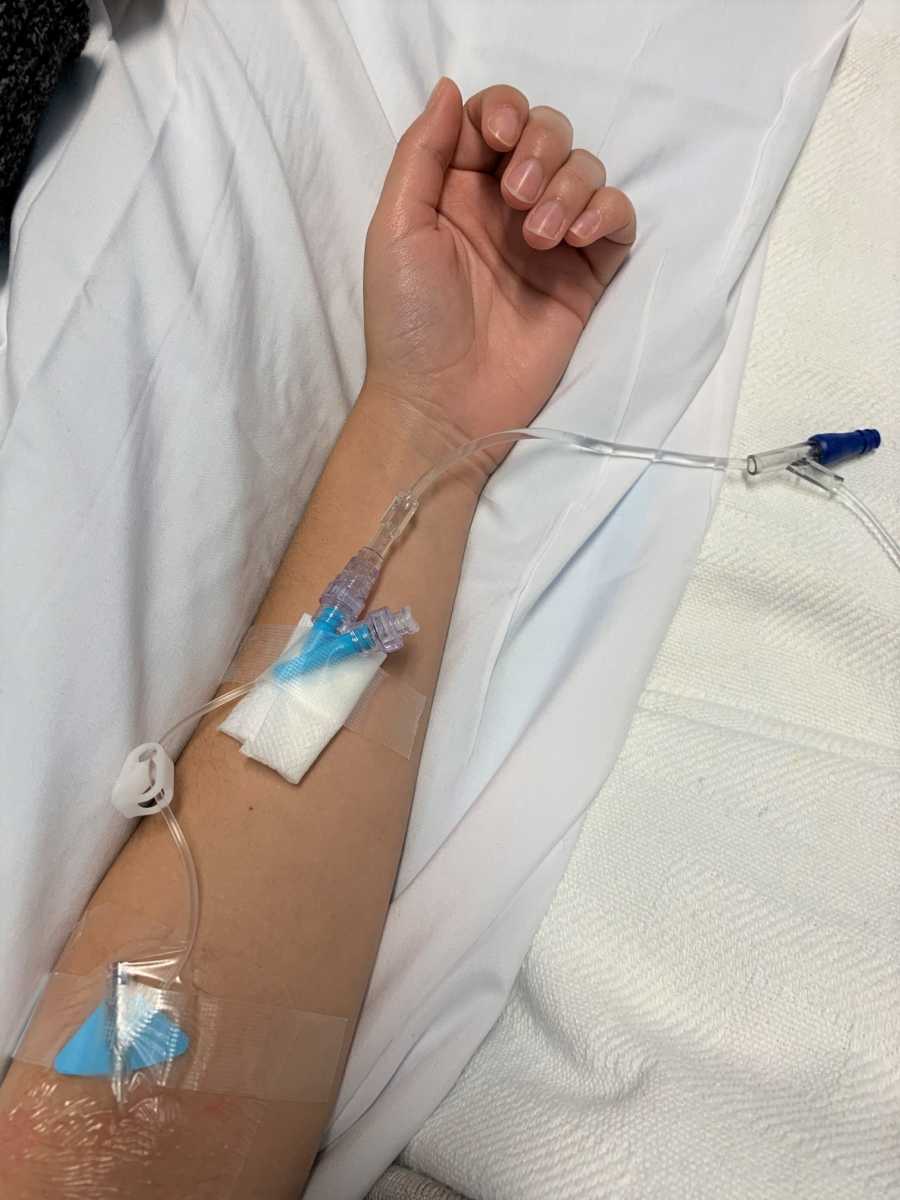
After that misery, I had a conversation on the phone with the nurse practitioner over at the neurologist’s practice. The neurologist wanted me to go on either a pill or IV medication for MS once I had the final diagnosis they were preparing me for. I hated needles at the time, so I chose the daily pill. I asked about potential side effects and she only said I might have some flushing and an upset stomach. I asked specifically if this would change anything else about me, and she said no. I wanted to see the actual neurologist right away but was told she refused to see me until I got another MRI of my cervical spine to be sure I had MS.
I saw the actual neurologist after my cervical spine MRI. She diagnosed me with MS officially, said I had a severe amount of lesions in my brain, and emphasized I would need to start aggressive treatment ASAP. I came in with my laptop that day because I had typed out a list of questions for her to answer. She couldn’t give me a number of MS patients that she treated. Hundreds? Less than that? ‘I couldn’t tell you,’ she said.
I questioned her about the side effects of the drugs she recommended because only after my own personal research did I actually find out what the serious side effects were. The side effects of the MS medications out there were troubling. PML (a brain disease that causes severe disability or death) being the scariest, but also hair loss, a suppressed immune system, liver problems, and the list goes on. She then said I could ‘choose whatever medication I wanted’ as long as it was for relapsing-remitting MS. She said for my next appointment she could ‘fit me in in a 5-minute window’ the next week to tell her the kind of medicine I wanted, and that would be it.
It was during that time which I felt the most denial. What if the diagnosis was wrong? It felt wrong. I didn’t in any way feel like I had MS. Looking up the common symptoms, I didn’t have even half of them. I read stories online about people who thought they had MS but actually had something else, like heavy metal poisoning. I also felt a lot of anger – why did this have to happen to me? I just wanted to opt-out of this, but there was no way. I was stuck with this for the rest of my life, and there was no way out. It took a couple of long months to finally accept my diagnosis and begin moving on with my life.
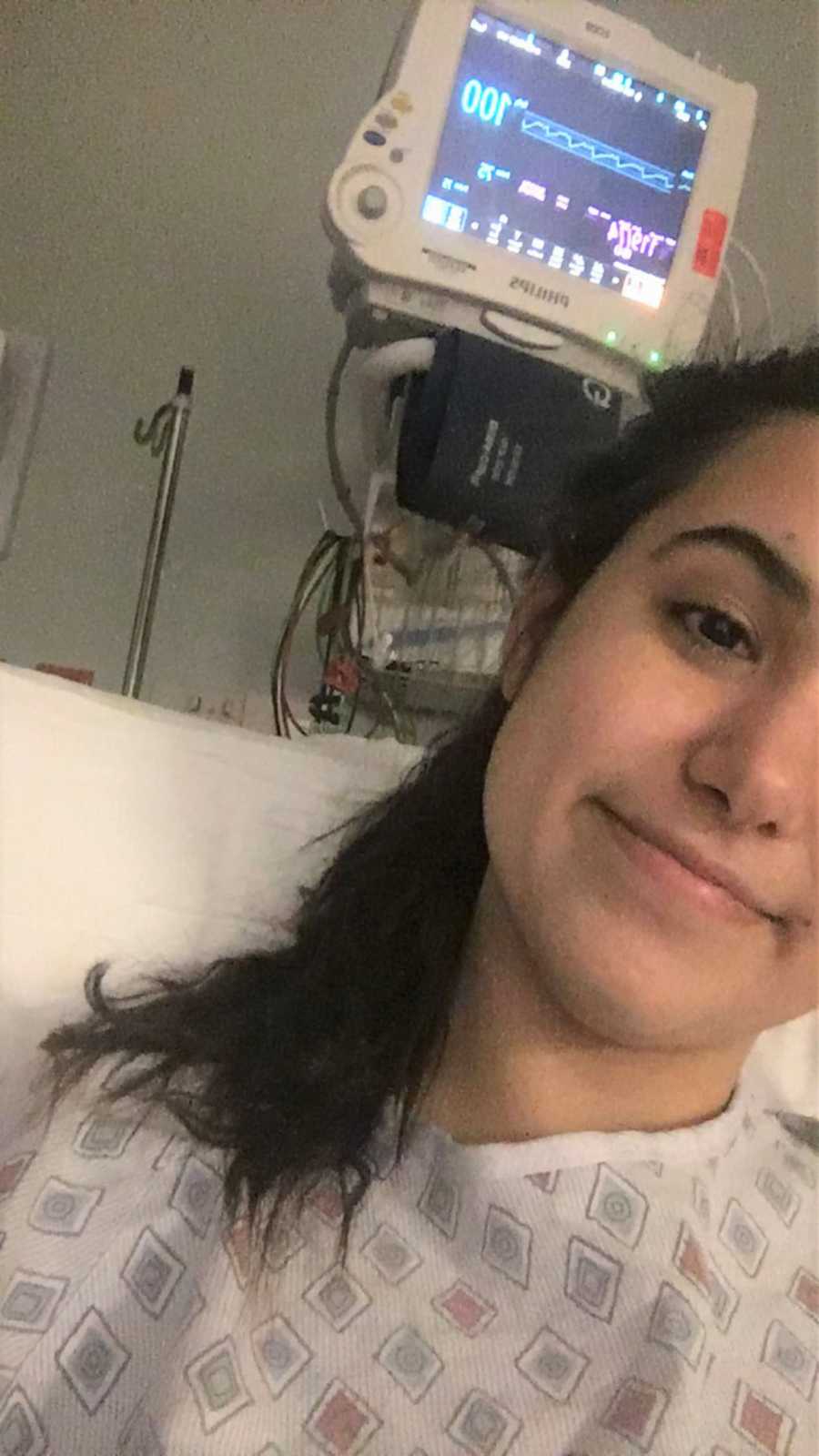
But things started to turn around. I decided to get a second opinion back home in Vegas. The care I got there versus the care I got in my college town was night and day. The new neurologist specialized in multiple sclerosis. Everything finally added up when we went over the symptoms I’ve had throughout my life.
Looking back, I had many symptoms of MS in my life, I just didn’t realize that was what they were. I had experienced nerve pain in my fingers for a few years. Chronic fatigue had always had a presence in my life, even starting in middle school. Brain fog as well. There was also a time not so long ago that I felt numbness in my arm for two weeks, which was triggered after I got blood work done. During my freshman year of college, when running, I would experience numbness in my legs. Another complication of MS is heat sensitivity. I used to do hot yoga/hot pilates quite regularly before my diagnosis. I was in great shape, but as soon as the heat eventually got to be too much for me I would all of a sudden feel an overwhelming urge to collapse and have to leave the room. Afterward, I would be extremely tired and would knock out on the couch when I got home, sometimes even having a hard time staying awake while driving home. I always blamed this on myself and thought I just needed to be more physically fit to defeat this. I later learned that in MS, heat can actually mimic a relapse in the body. That was what I was experiencing all of that time. These were all things leading up to my eventual diagnosis.
The new neurologist saw the number of lesions in my brain as moderate, and not severe as I was originally told. She strongly recommended aggressive IV medication for me. I was still wary about going on such harsh medication. I have always favored natural/holistic approaches to modern medicine, but I felt very pressured to pick a treatment right then and there to start tackling MS. I told the neurologist I felt fine. ‘It will catch up with you,’ she said in complete seriousness. I felt like I could trust her more than the last. She did have a lot more expertise than the first neurologist I saw. The medication couldn’t cure me, but it was promised to delay the progression of the disease – so I made the difficult decision to start on it.

I remember telling some of the people I knew and trusted at the time that I had been diagnosed with MS, and a lot of them treated me as if I had just been given a death sentence. I was confused by their reactions because I felt fine. I ate healthily and worked out often. I felt better than I ever had. In all honesty, I think they were just very worried about me. Some people even asked me if my frequent yoga practice and fitness routine was what caused my MS. But both neurologists I saw theorized that my healthy lifestyle was why I was so asymptomatic, compared to the number of lesions that showed up on my MRI.
I felt powerless in a sense like I HAD to be on this medication with terrible side effects for the rest of my life if I ever wanted a chance at a good life. Now I’ve been on MS medication for about a year, and it’s been over a year since my diagnosis in November of 2018. I do think MS medication is useful to delay the progression of the disease. When I first started Tysabri, my IV medication, I had one fatigue relapse early on before it really started working. I would sleep for most hours of the day because I absolutely could not do anything else. The hours I was awake, which were very odd hours of the day, I would have to work on schoolwork because that was my biggest responsibility. After the 6-month mark, I had an MRI to make sure the medication was working. Two new lesions showed up, though they weren’t in ‘problem areas,’ and they were inactive thanks to the medication. I’m now due for another MRI to make sure my condition is still stable.
I’ve realized it is entirely my choice if I want to stay on medication for the rest of my life. If I wanted to choose another route of treatment tomorrow, then I would. It is my life, and I think everyone should have the choice to manage their health the way they think is best for them. I know people that are thriving with MS on no medication and people that are thriving with MS on medication. Everyone with MS is different; the disease is specific to each person.
It’s been over a year since my diagnosis now. I have come to terms with my disease, but it doesn’t define the person I am. I haven’t let this hold me back from anything I enjoy. Since my diagnosis, I have still done plenty of traveling, hiking, and physical activity. I don’t plan on that changing. I also try to maintain a positive attitude because I am so grateful to be doing so well. I still have challenges from time to time, but that doesn’t stop me from making a great life for myself, and hopefully being able to empower others.

This story was submitted to Love What Matters by Chloe Maddison. You can follow her journey on Instagram. Submit your story here, and be sure to subscribe to our free email newsletter for our best stories.
Read more beautiful stories of those living positively while battling chronic illness:
Provide hope for someone struggling. SHARE this story on Facebook and Instagram to let them know a community of support is available.