“Kristy and I both came to the same realization in the Summer of 2015. Our sons, Oliver and Micah, were 6 and 4 at the time, and we had maintained a ‘two was enough’ pact for quite some time, but our family felt incomplete. We agreed to try for one more child and a few months later, we were elated to learn of Kristy’s pregnancy.
As a labor and delivery nurse at a major hospital, Kristy kept tabs on her progression informally and I joined her at the first official ultrasound where we learned a baby girl was on her way. ‘Your 24 weeks, right?’ the ultrasound tech asked. ‘No, that’s not right, I’m 21 and 2 (L&D talk),’ Kristy affirmed. ‘That’s odd, the head is measuring 24.’ The tech figured it was an angle but called her supervisor in to measure as well. Kristy joked this little girl was going to have a big head like her brother Micah. We ended up getting referred to high-risk neonatology based on two findings: ventriculomegaly and echogenic bowel.
Things muddied quickly. The first doctor to scan Kristy struggled to find a kidney (which was there) and felt our daughter’s skull had an irregularity but couldn’t quite figure it out. He was very concerned and ordered a fetal MRI and amniocentesis. Our nerves had begun to mount. The doctor, a colleague my wife had known for years, shared a variation of, ‘God gives special babies to special people,’ in an effort to provide comfort, a platitude which I would hear and have since come to disdain.
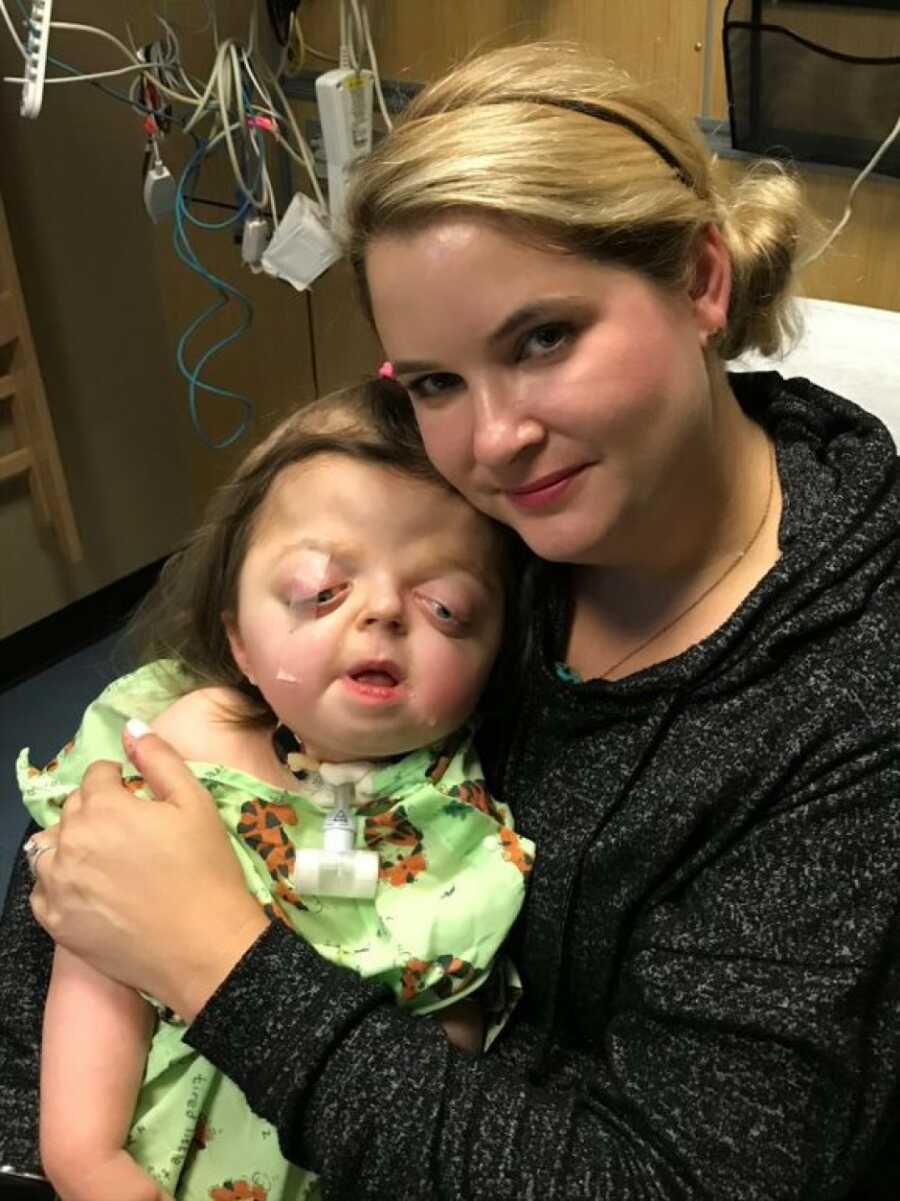
We ended up seeking a second opinion, a highly regarded physician, and due to an important multiday accreditation at work, I needed to miss the first appointment. Huge regret didn’t take long to set in. A panicked phone call from Kristy on my lunch break, coherence barely intact revealed, ‘Dr. H is 90% sure Hadley has syndromic craniosynostosis. Don’t google it.’ I excused myself from work and relayed to the lead accreditor I would not be in tomorrow. Hadley’s amnio would eventually come back to confirm Pfeiffer Syndrome, an FGFR2 mutation that causes premature fusing of plates in the skull. The doctor had been right.
The next day, Kristy’s dear friend Sarah joined us at the house. We sat stoically at the dining table, overwhelmed and trying to process based on the little research we had done. Trying to rally us, Sarah asserted, ‘Of all the couples I know, the two of you can handle this, and Hadley (we had settled on a name) will be so lucky to have you.’ I was struck with a sense of support and went into game mode. Kristy struggled through the remainder of the pregnancy, losing weight and experiencing extreme anxiety. This would start a cycle: When one of us starts to fall apart, the other grows strong, and we’ve been taking turns ever since.
We met with a local craniofacial team, who talked us through the likely surgical progression to address Hadley’s anticipated needs. Cranial vault reconstruction (CVR) and a frontal orbital advancement (FOA) were in here future. Eventually, a midface advancement and possibly jaw surgery would likely follow later in life. The road map was loose, but there, although the doctor shared there’s no exact algorithm as each child is different.
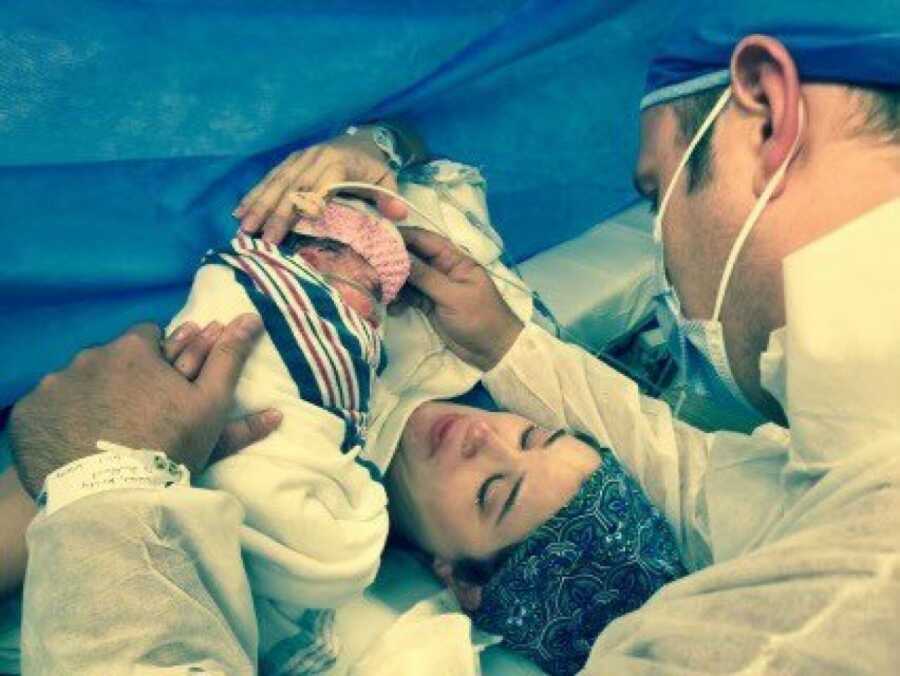
Hadley was born June 2, 2016, by scheduled C-Section as she had presented breech for the two weeks leading up to the delivery. Sarah and Alyssa, another close nurse friend, took care of Kristy that day, and after placing her foley Kristy asked Sarah if she was dilated. Sarah shot Kristy a look to confirm yes, adding, ‘And she’s head down.’ All the nurses laughed as this sort of thing is funny to them, while I on the other hand sucked a peppermint and fought an ominous sense of foreboding. The C-Section proceeded smoothly, and we met our little girl. She was precious, and fragile, but foreign all the same. And we loved her from second one.
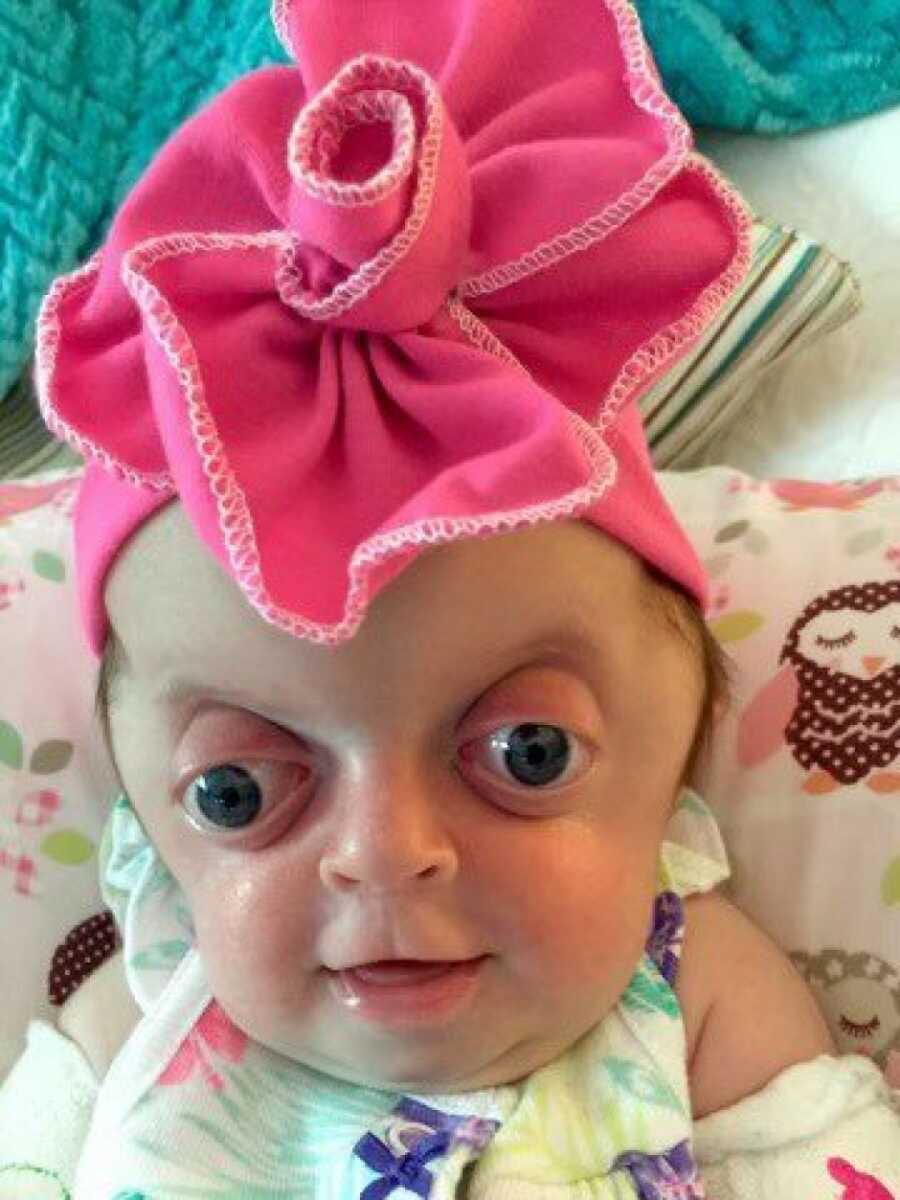
Her skull shape was domed due to the sagittal and coronal sutures closing, clinically described as brachycephaly. Apart from that, her vitals were strong, she was cute as could be, and after 4 days in the NICU for consults and to be cautious, we went home. A honeymoon period ensued and we enjoyed getting to know our girl. It wasn’t until the middle of July her eye bulged for the first time.
Children with Pfieffer Syndrome and related syndromes are born with a sunken midface, resulting in proptosis. With her eye having less bone to protect it, a strain or a cough can cause the eye to move forward past the lid. We battled this pattern for several months of her eye essentially popping out, but always managed to guide her eyelid back over. We had begun to discuss Hadley’s first round of surgery, but when her right froze past her eyelid on September 16th, we were forced into an emergency situation. Hadley’s always called her own shots. Somewhere between birth and 3 months, Hadley had developed severe hydrocephalus and needed immediate surgery to expand her skull and relieve intracranial pressure. Over the course of 9 hours on a quiet Saturday morning, Hadley would have a CVR, her first FOA, and a shunt placed while Kristy and I sat alone in our first surgical waiting room.
The surgery, by all measures, was a success. Her skull looked amazing. However, two days into recovery Hadley’s eye would develop a pseudomonas infection that would result in her first, long hospitalization (10 days), and ultimately result in the enucleation of her right eye when she was four months old. It was a brutal experience. While we had prepared, embraced, and welcomed life raising a child with Hadley’s diagnosis, this was not in the script. The physicians felt terrible at the loss of Hadley’s eye. Our plastics doctor said in over 800 cases he had worked on, this had never happened before. This didn’t provide comfort and I can tell you being a statistical outlier to an already rare diagnosis (1 in 102,000 births) is a frustrating place to end up.
As a family unit, we began to adapt to Hadley’s increasing care needs. The balance of parenting our two boys and serving as both a parent and caretaker for Hadley was an adjustment that took time to figure out. We are fortunate to have the support of my parents locally for all three of our children, and they always manage to fill in the gaps. Shortly after her first birthday, a crummy sleep study, and an increased dependence on oxygen, Kristy and I agreed Hadley would benefit from a tracheostomy. Our boys spent the summer with my parents in Minnesota while Hadley healed and we learned a new set of skills.

At the tail end of the following summer, we would begin working with Boston Children’s Hospital for Hadley’s neurosurgery needs. Traveling with a child with machinery is stressful, leaving me to feel like a pack mule that everyone stares at. Medically pre-boarding a plane with a child in a stroller also tends to draw gawkers who question why you get to enter before them ‘just because you have a child,’ scrutiny I have grown stone-cold indifferent to over the years. We need that extra time. On that flight, our DME-issued oxygen concentrator ran out of battery 15 minutes before landing, Hadley’s oxygen saturation tanked, and we flagged down a flight attendant for the green oxygen tank. I had to rip off the connected mask and MacGyver the tubing so Hadley could breathe the remainder of the flight. I realized we had learned to function on ingenuity and instincts, but we always found a way.
Hadley needed a Chiari decompression to alleviate crowding at the base of her brain stem and we hoped it would help in her global development. The surgery was successful and about two days after, something remarkable happened. Hadley started to breathe room air and maintain her oxygen levels without support. The level of gratification and quality of life this provide was immense and a glimmer of hope.
The next felt months felt like progress. Hadley grew stronger. She needed air from time to time, but not with consistency. She was using a passe Muir valve. Then came the Saturday morning of the garage sale. Kristy was outside cutting deals on secondhand clothes and gently used toys, and I was hanging out with Hadley when she stopped breathing. With her pulse oximeter reading in the 40s, I decided to change her trach as suctioning hadn’t worked. A fresh trach and a steady flow of oxygen helped her recover a little but her numbers still weren’t great. Then she dipped again, this time into the teens. I yelled for Micah, ‘Go get Mom. Now!’ Kristy rushed in, I gave her the Cliff Notes version and she went to stimulating and the Ambu bag while I found an oxygen tank with a higher regulator flow. A few frantic minutes and Hadley recovered enough for us to jump in the car, send the boys next door, and rush to the ER.

Hadley kept it together for the car ride but as were waiting for intake at the desk, Kristy asserted, ‘We need to be seen immediately,’ and walked directly into the unit. By the time I got back to the room, a nurse was working on vitals when we saw Hadley’s leg begin to twitch. The full seizure quaked moments behind, and for the next 30 minutes, I’m not really sure how long, we stood in the corner as we watched a team of medical professionals attend to our coding daughter. Powerless, hopeful and shocked, they eventually stabilized Hadley.
It turns out Hadley’s body had been retaining CO2, resulting in low energy levels and diminished hypoxic drive. With a little calculation and chemistry, Hadley bounced back and looked as good as ever, but she was sent home with a ventilator to use at night. Our pulmonologist sought out a vented model that could monitor her gas levels which kept us in the hospital a few extra days to secure, but well worth it. ‘If she has to have a vent, it might as well be sexy,’ I told Kristy over the phone during rounds one day, which the attendee doctor couldn’t help but laugh at. Humor, sometimes dark, sustained us that day, and many. As Kristy often says, ‘Laugh or cry. Right?’
The introduction of the ventilator into Hadley’s regimen completed our bionic little girl. Life became stable, imperfect, and ours. Hadley’s global development is at a snail’s pace, but it’s there. Neurology added cerebral palsy to her list of diagnoses along the way, likely acquired, but it’s just another asterisk to her story. No condition defines her.

Our marriage has strained but strengthened through the past five years. I love my teammate, and while the first year of Hadley’s life was incredibly stressful on our relationship, we stumbled through it and ended up in a better place than where we started. Our sons love their sister to no end and have functioned with maturity and effusive love both in support of Hadley and also in watching their parents struggle to cope with a difficult diagnosis, grieve idealizations, and welcome the wonder that is Hadley into our family. I’m so thankful for Oliver and Micah and their resilience.

We have made lifelong friendships sparked by common circumstances and solidified by the human connection that were born on Facebook. The level of community available online and bolstered through organizations such as the Children’s Craniofacial Association are powerful tools of support. Social media has also proven a means for me to share my perspective on life, raising Hadley. While I have an amazing group of friends, the guys aren’t always the right outlet to share about the ins and outs of Hadley. I’d rather talk football and indulge in a little escapism. When we started Hadley’s Facebook page several years ago, it was a means to keep friends and family up to speed while sharing some of my feelings at the same time. As we moved on to Instagram, the audience reach is vastly larger, so my intent has shifted slightly. On IG, I’m seeking to normalize families with medically complex kids and reinforce that all children are worthy and should be celebrated. I like making videos that strike a balance between sentimental, emotionally raw, and funny to reflect our life. It’s a purposeful way I can spend time with Hadley, and she makes a great comedic foil for her goofy Dad.
Hadley’s life isn’t what Kristy and I envisioned when we decided our family was missing something years ago. But it turns out she’s just what we needed. We continue to maximize Hadley’s experience and development but wouldn’t trade her for the world. Our daughter exudes happiness, makes us think, and talk and feel, and provides focus and meaning to our lives. She is perfectly imperfect and her life has value. If I could change anything, I think back to that one doctor’s appointment I missed. I made it to the next 100 before I finally stopped counting. You can’t always fix mistakes, but you can always show up for the ones you love.”


This story was submitted to Love What Matters by Andrew Lund. You can follow his journey on Instagram and Facebook. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this here:
Provide hope for someone struggling. SHARE this story on Facebook and Instagram to let them know a community of support is available.

