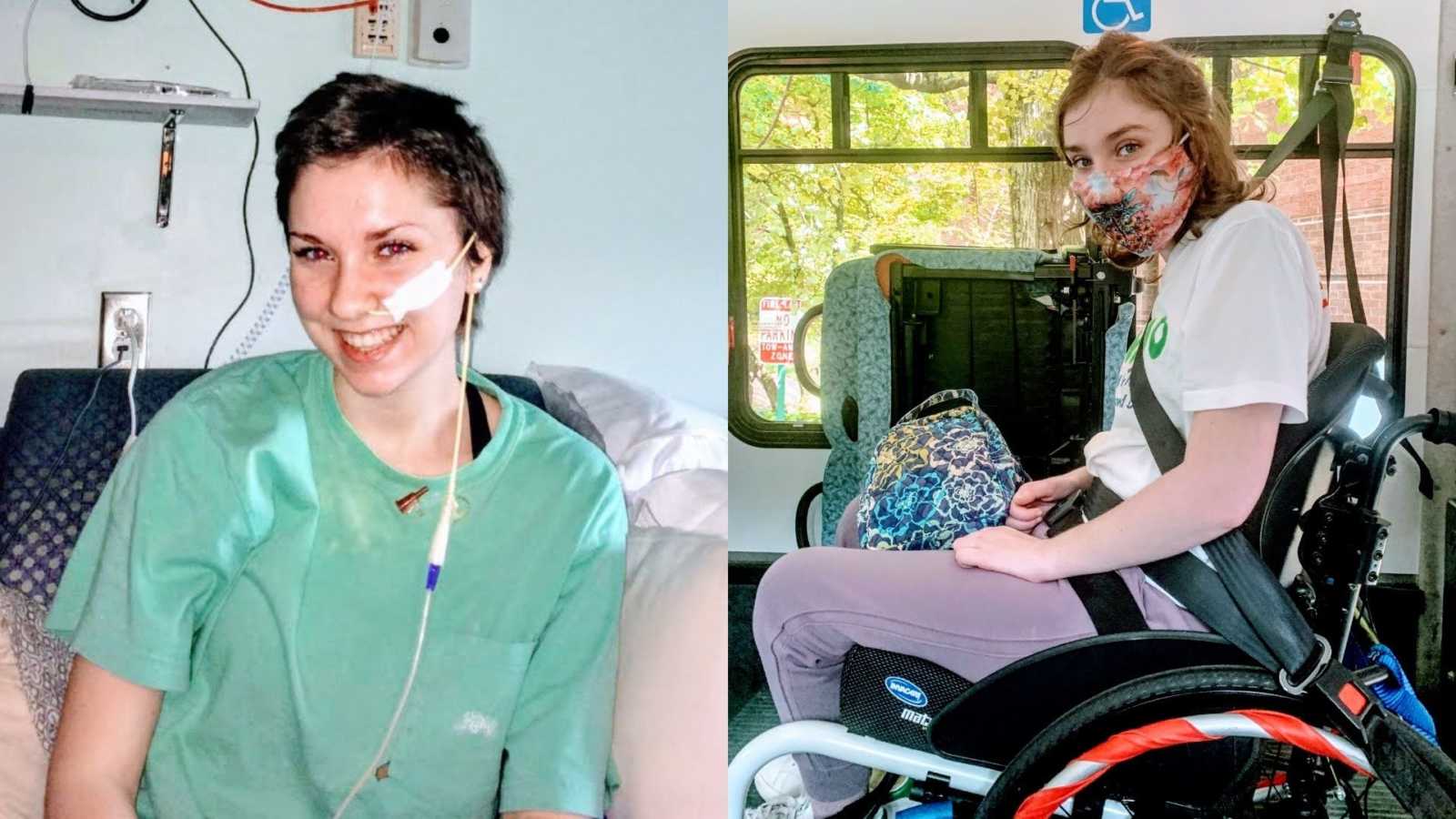
“It all started in 2017. I graduated from eighth grade, went on a trip to Germany, and even won an open water 10k swim race. Then everything changed. It started with not being able to breathe and passing out. Then it turned into the inability to eat and severe infections.

Between 2017 and 2019, I was formally diagnosed with Ehlers-Danlos Syndrome, Dysautonomia, Hashimoto’s, Alopecia (fancy word for hair loss), Gastroparesis, and a multitude of strange and unusual infections. During this time, I started seeing a Rheumatologist who said, ‘Something is brewing, but I just can’t put my finger on it.’ That summer, I had sepsis and went into septic shock twice. I was extremely weak from being intubated and sedated for so long as well as worsening of my EDS. I was prescribed a wheelchair, and began rigorous outpatient physical therapy.
After the multiple septic episodes, I was placed on a ‘fever rule.’ Any time I had a fever over 100.4, I had to be admitted to the hospital for prophylactic antibiotics and 72-hour blood cultures. Between July of 2019 and December 2019, I was admitted at least five times for this exact reason/treatment plan. I have always run pretty neutropenic, so fevers are nothing to mess around with for me.
Due to the severity of my GI issues, I was placed on a nasal-jejunal feeding tube through my nose for almost a year. In October of 2019, I finally underwent a gastro-jejunostomy feeding tube surgery which essentially failed. That December, I was placed on total parenteral nutrition through a PICC line. I went through so many surgeries trying to get the tube right again, but nothing ever worked. It was probably one of the most devastating times of my life.
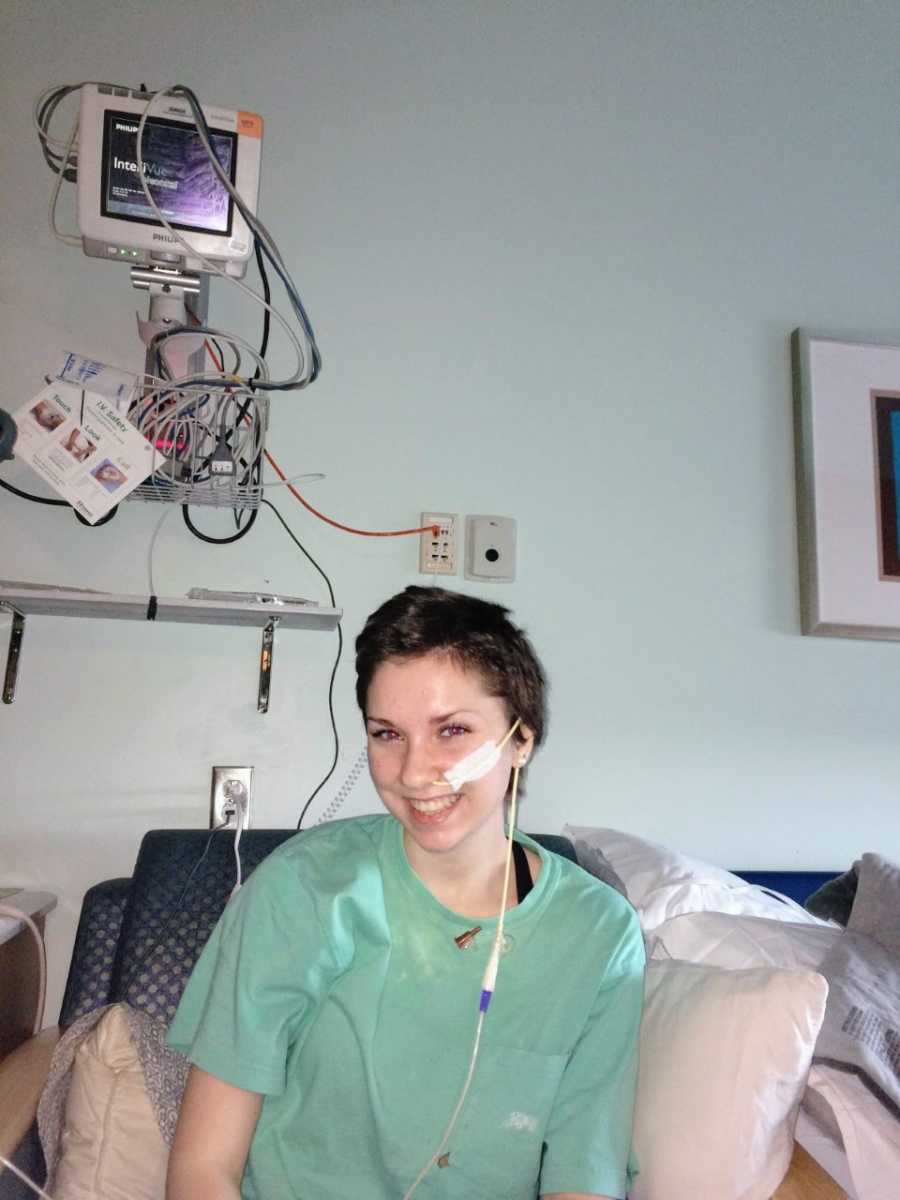
Eventually, in May 2020, I had surgery done to place a Roux-En-Y Jejunostomy, giving us access directly to my small intestine while leaving my G-tube in to give me access to my stomach as well. Surgery was complicated. I had excessive post-op bleeding, and the pain was nothing like I’ve ever felt. I was so scared and so out of it. The complications were explained to me over and over again, but I felt like nobody was listening to me. But I made it through what I thought had been the worst time of my life (except for sepsis in 2019). I thought it couldn’t get any harder. What I went through in the coming weeks and months put everything I had already been through into a humbling perspective.
May 29, 2020 is a day I will never, ever forget. I woke up that morning, exactly a week after being discharged from the hospital, with the worst headache and chest pain in my entire life. According to my Mom, I looked septic, but never had a fever. I tried to take a shower to help with the pain, we left the house and drove quickly and erratically to the ER. Covid was still new at this point, so the Hospital’s Emergency Room was almost empty. I potentially wouldn’t have survived if I didn’t get back as fast as I did.
A doctor thought I had a migraine and decided to start the Raskins Protocol. I remember disconnecting from my feeding tube because I was throwing up so much. And that’s the last coherent thing I remember for the next two months. My vitals became severely erratic, and I was rushed to a trauma room. I was in severe cardiogenic shock and multisystem organ failure.
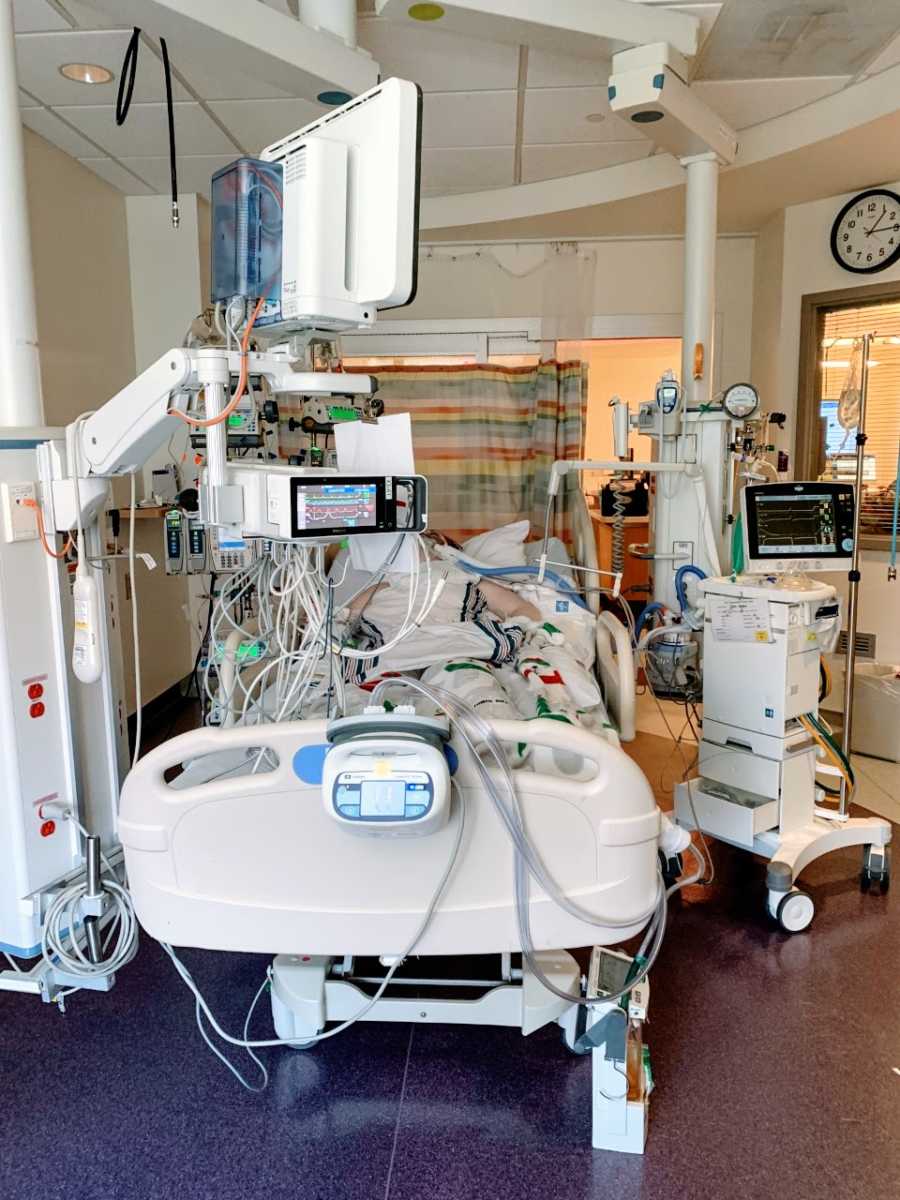
I was moved up to the Pediatric Intensive Care Unit (PICU) and was intubated quickly due to respiratory failure. Within 24 hours, my heart failure escalated, and I was taken in the Pediatric Critical Care ambulance to a hospital with more advanced life support to be started on ECMO (heart-lung bypass).
While in the PICU, I had blood, urine, and lung cultures pulled countless times. They were clean every single time. With my presentation and history of sepsis, this was incredibly confusing. Several days later I spiked a fever of 108 degrees. I was literally stripped naked, covered with cold cloths and had cold fans blasting at my body. We now know most of what happened early on in my hospitalization was most likely due to a severe autoimmune crisis that wrecked my body in too many ways to count.
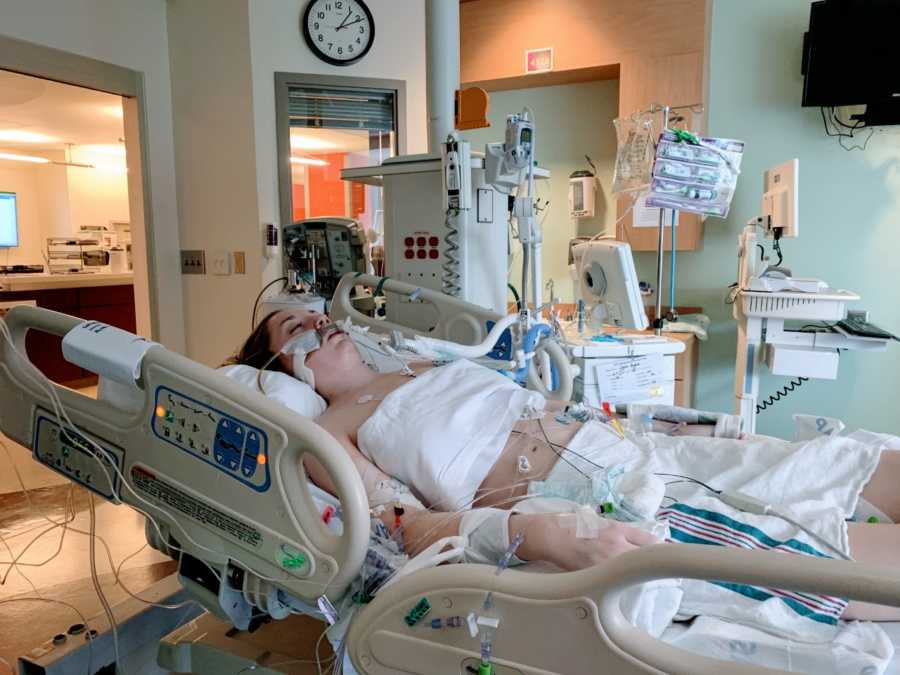
Several days later, I had my breathing tube removed. I have been extubated before, but it was never like this. Upon coming off the ventilator, I went between catatonic and psychotic. The things I was saying made no sense. It was the most terrifying time in my life. Things as simple as the movie The Blind Side or Miss Congeniality would push me over the edge and into a lake of terror. During this time, the ICU Psychiatry doctors were giving me strong antipsychotics, which eventually caused me to have seizures.
I never thought I would be thankful for seizures, but these lead the doctors to find what was wrong with me. After convulsing, the medical team ordered a CT scan of my head. The scan found two small strokes in my cerebellum. These happened while already on blood thinners, which prompted my fantastic hematologist to run a set of antibody tests. They were positive, and 3 months later I was officially diagnosed with Antiphospholipid Syndrome, an autoimmune blood clotting disorder.
After my Rheumatologist found out about the APLS, she ran another antibody panel which was positive. It turned out I wasn’t crazy, the psychosis was from a disease called Autoimmune Encephalomyelitis. I quickly began undergoing chemotherapy treatments to suppress my immune system and IVIG to fill my body with healthy antibodies. These helped, but I still sustained a Brain Injury from the Encephalitis.
But the punches didn’t stop with the TBI. Around July 14th, I completely stopped moving. The speech, physical, and occupational therapists as well as my nurse and mother all knew something was wrong, but the doctors in the ICU were convinced my lack of movement was due to heart failure. A week later, I had a spinal tap, which showed severe inflammation in my spinal fluid, a nerve conduction test, which showed no nerve function anywhere below the neck, and a spinal MRI, which showed severe inflammation in the bottom segment of my spinal cord. I was diagnosed with severe Guillain-Barre Syndrome, flaccid quadriplegia, and mixed sensory-motor polyneuropathy. Essentially, I now had severe peripheral nerve, spinal cord, and brain damage. The night of my nerve test I had a femoral vas-cath implanted and was started on Plasmapheresis, a procedure that filters the blood of bad antibodies. I received PLEX five times. The rest of my time in PICU was focused on Spinal Cord and Brain Injury rehabilitation.
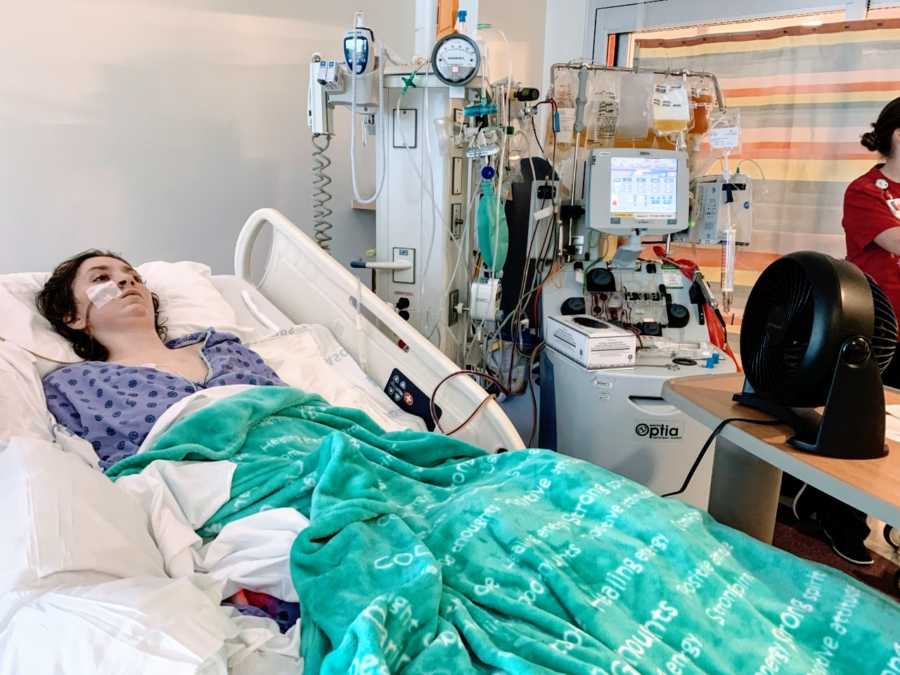
I have a hard time writing emotionally about this chapter of my story. People call me strong and a fighter, but I don’t feel like either of those things. I feel scared, weak, lonely – like nobody in the world could ever even begin to understand my experience. I don’t feel like I fought anything; I didn’t have a choice. I don’t remember anything, and the little bit I do recall are terrifying hallucinations. I would be set off by the littlest things. Watching a video my friends sent or hearing an unfamiliar voice would send me into a storm.
I usually remember everything that happens in the hospital. But this time, I don’t. The few memories I have are warped versions of my reality, and pain. So. much. pain. I remember watching HGTV and being sent into a full blown panic. Everything scared me and everything had a twisted meaning.
Finally, after seven weeks in the ICU, I was transferred back to the original hospital’s inpatient rehabilitation unit. I spent the first 2 or 3 weeks there on suicide watch. Even though I couldn’t move my body, I could feel it and I could speak. And the pain of feeling your nerves literally die is unlike anything I had ever imagined. I would scream how I wanted to die all day long. If anyone touched my legs, I would scream uncontrollably. Eventually, the psychosis started to subside, and I was allowed to attend therapies outside of my room. During this time, my upper body strength began to recover greatly. It took more work than I ever could’ve imagined.
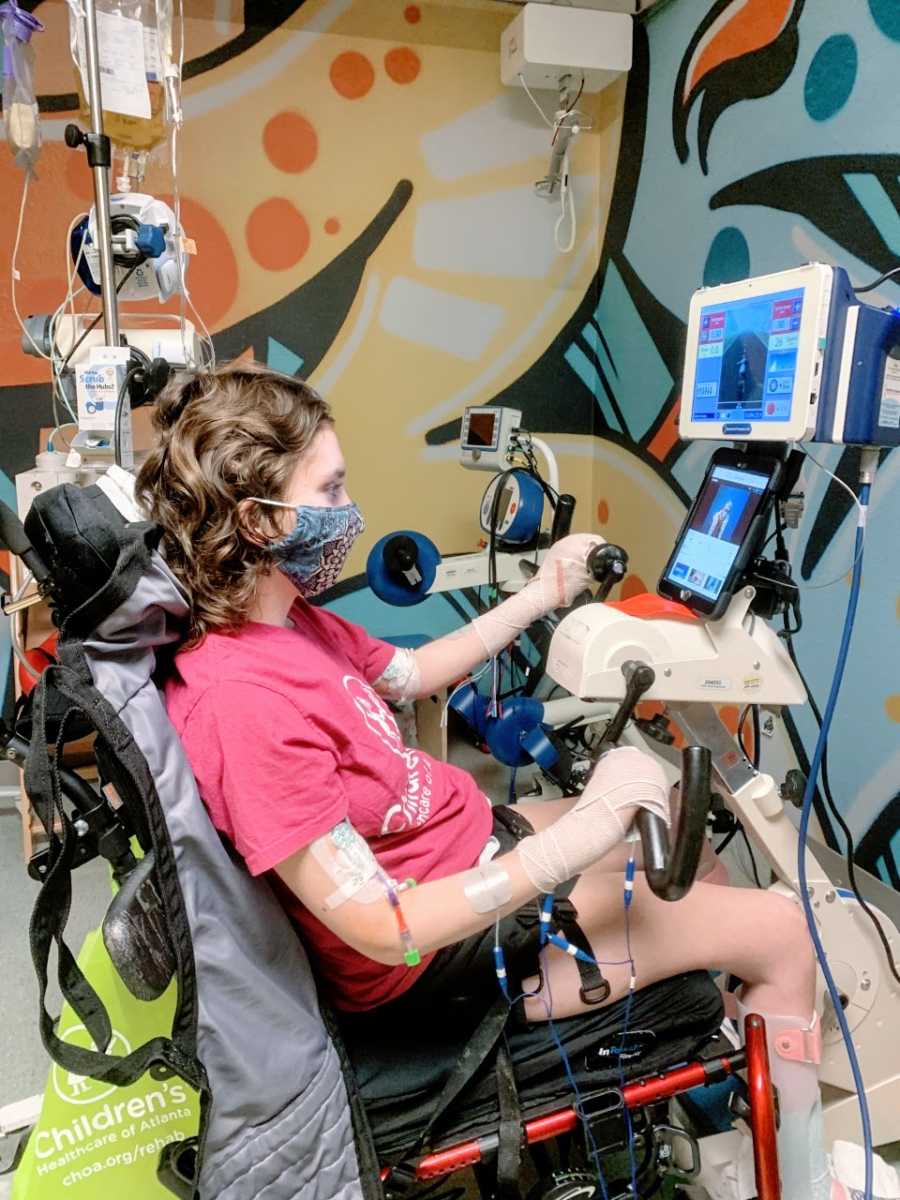
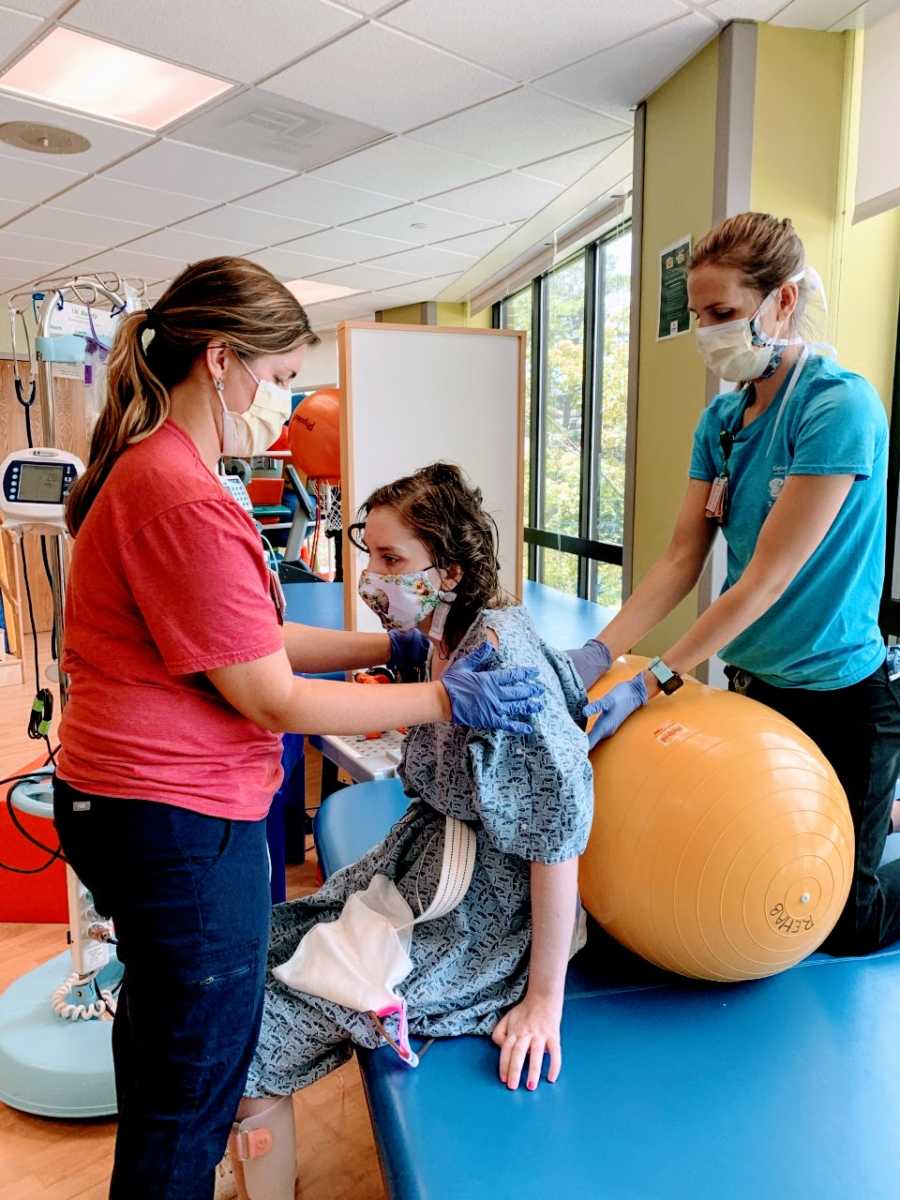
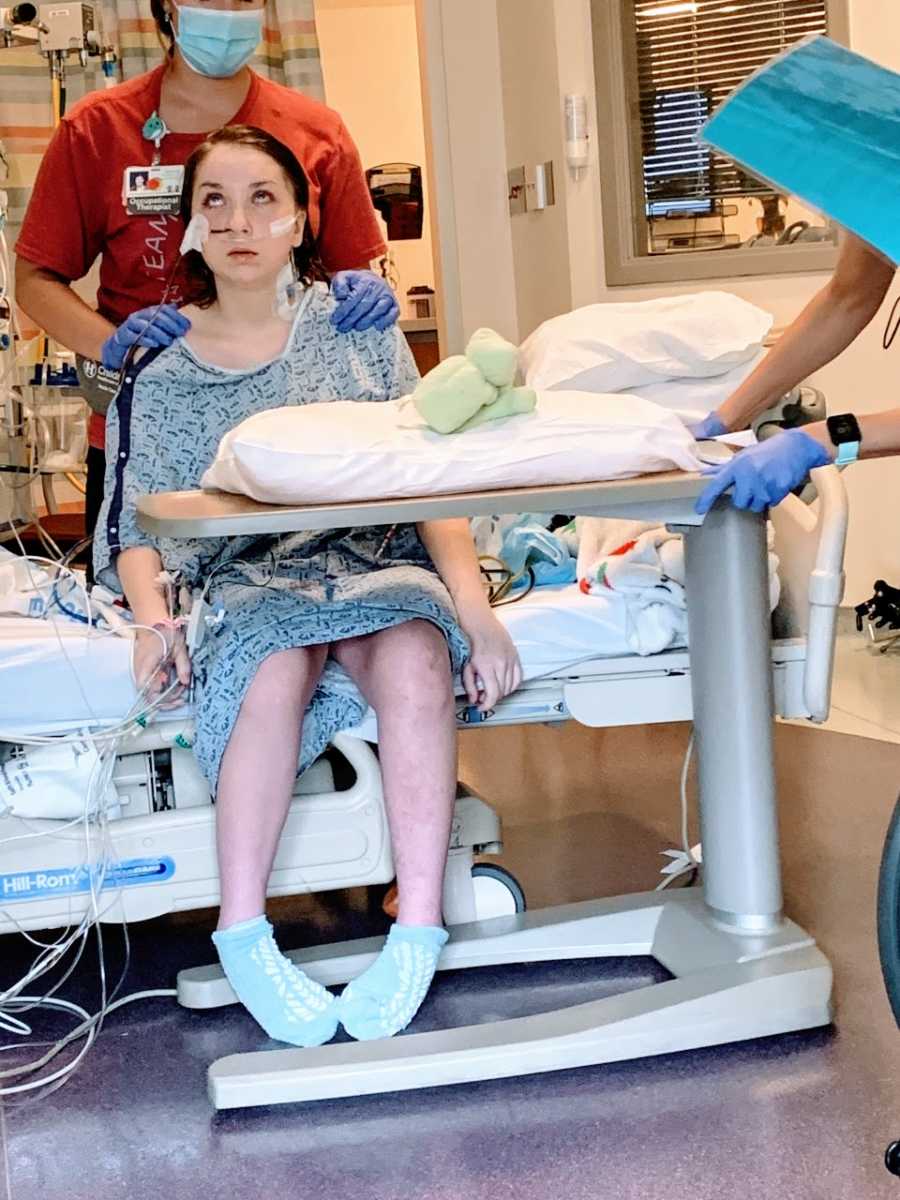
Towards the end of my stay in rehab, I stopped using the big tilt-in-space wheelchair and was able to start using my manual wheelchair again. Days later, I was discharged from the hospital, and sent home to a world I never imagined: I had to sleep in a hospital bed and use an electric lift to get into bed.
Day Rehab was every week day from 9 a.m. to 3 p.m. Being there helped me to gain more independence with transfers, clothes management, and going to the bathroom. After that month, I was discharged back to outpatient therapies. This is where I truly began to grow and be challenged. I started standing here while supported. I’ll never forget the day I intentionally locked my knees out while standing. The tears were flowing.
Today I am doing physical and occupational therapy most weekdays. My arms and legs are continuing to recover and I am becoming more and more independent. I still receive IVIG every two weeks, take an immunosuppressive medication every day, and receive another one every few months. I will be on blood thinners for the rest of my life.
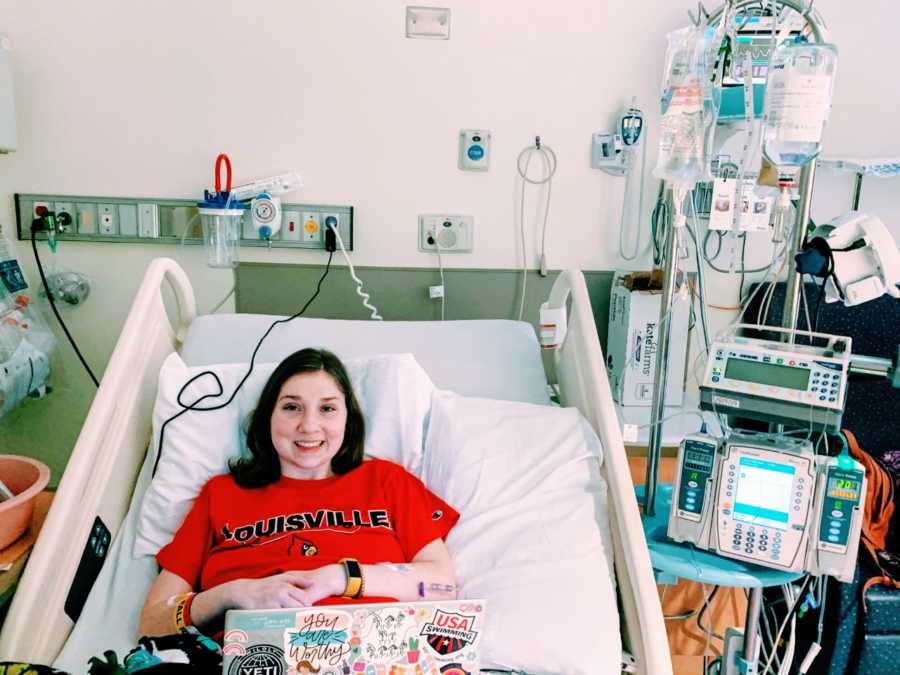
A lot of people pity me, but living with a disability isn’t always bad. Adjusting to life in a wheelchair has been harder than I ever could’ve imagined. I have spent a lot of time grieving the life I once had and accepting this bumpy new one. I will never take for granted something as simple as moving my body or life in itself. Others often are surprised at how positive I am despite everything I have gone through. The truth is I’m not always positive and happy with my situation. I cry and yell and get so angry and frustrated with my life. One of my favorite sayings is, ‘Grow through what you go through.’ I have chosen to live my life that way: always taking the worst and letting it inspire the good in me. Likewise, I choose to practice kindness and empathy. Being kind is incredibly rewarding.
I hope if you take one thing from my story it is to always, always be kind. As Ian Maclaren said, ‘Always be kind, for everyone you meet is fighting a battle you know nothing about.’ And I have learned to love what truly matters: the gift of life.”


This story was submitted to Love What Matters by Ceara Hughes. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Do you know someone who could benefit from this story? Please SHARE on Facebook to let them know a community of support is available.