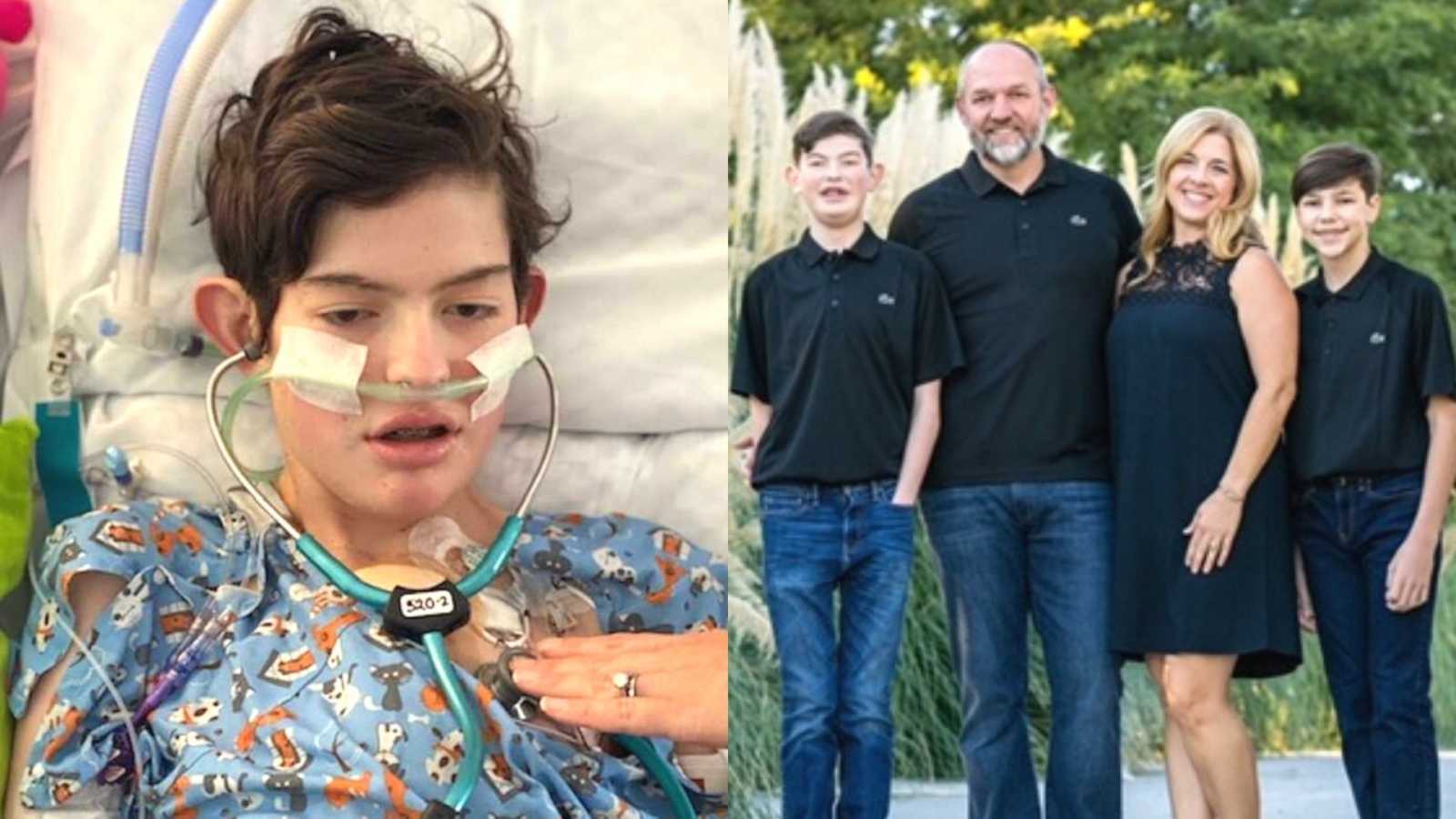
“When we learned we were being chosen to adopt our second baby boy in 13 months’ time, we had no idea how this little guy, number two, would keep us on our toes. I received the call from the adoption agency on Thursday night, asking me, ‘Can you come get a baby boy in the morning?’ Parker was a surprise from the beginning, and the surprises just kept coming.

When Parker was about 2 years old, we really began to question if there was something we were missing. He crawled late, he walked late, and he fell a lot. He fell so much I was worried I would be reported to child protective services. I mentioned it to his pediatrician and thankfully, she acted immediately. First, we took Parker for an eye exam and realized his eyesight was miserable. He was then fitted with the cutest little eyeglasses I have ever seen on a little guy. But she also sent him for an evaluation with muscle disease specialists, as she suspected that he had some sort of muscle disease.
Within the next year or so, we received a diagnosis. ‘Your son has Ulrich Congenital Muscular Dystrophy.’ We realized we had so much to learn. In the beginning, we didn’t notice a whole lot of difference between Parker and other kids his age, other than the fact he was weaker than other kids. Over the years, we remained hopeful he would defy the odds and be like every other healthy little boy.
When Parker was about 9, his new neurologist questioned his diagnosis. Things weren’t adding up, and she thought his diagnosis needed to be corrected. So, we were asked to travel to the National Institute of Health (NIH) in Washington, D.C. to get help correcting his diagnosis. We celebrated his 10th birthday in our nation’s capital at the beginning of the trip. After 3 days of intensive visits in the clinical center, Parker and I headed back to California. We really didn’t leave with many answers. They said, ‘We’ve narrowed his possible diagnosis down to two muscle diseases.’

By the time we returned to The NIH in April of 2019, they had corrected his diagnosis and found he actually had an even more rare muscle disease. Parker’s diagnosis was corrected to Desmin Myofibrillar Myopathy (recessive). There were only four other documented cases of recessive desminopathy. This trip had us in 2 more days of back-to-back appointments with specialty clinics. On the afternoon we were leaving, I got a phone call asking, ‘Please come back to the clinical center.’ When we arrived, they asked Parker to go into another room and watch TV while they continued to tell me, ‘Parker is in early heart failure. The muscle disease is attacking his heart.’
He was just days shy of his 12th birthday. My husband was home in California with our other son, and I just had a bomb dropped in my lap. I was panic-stricken, but I knew I had to keep it together so Parker wasn’t scared. I was terrified. We did end up meeting some friends in the area for dinner before we flew back to California the next morning. It was so hard to just put a smile on my face and pretend everything was okay for the rest of the night. After dinner, our friends dropped us back off at the Children’s Inn. I packed up our suitcases for an early flight and put Parker to bed. I went into the bathroom, turned on the bathtub, sat on the floor, and cried my eyes out for a good hour.
The flight back to California was the longest and most dreadful flight of my life. Parker could tell something was wrong. He was also scared. By the time we had landed, Parker already had follow-up appointments within the week with the heart failure team at Rady Children’s Hospital. And this became our regular life. The skeletal muscle part of his disease took a little bit of a back seat to this new heart failure diagnosis.

After a couple of months, we got used to the new routine and new medications. Then one day, at the end of June 2019, we were at Disneyland with some friends visiting from New Mexico, and I got a call from the cardiology clinic. I wasn’t in an area where I could take a call, so I made my way to an area that was quieter with better service to return their call, and they called again. I will admit it, I was all of a sudden worried they kept calling me. When I was finally able to take the call, Parker’s nurse practitioner was on the line asking, ‘Can you come to the hospital right away? We need to admit your son because he is having some dangerous heart rhythms.’ He had worn a halter monitor the week before, and they had just gotten the results.
I left our friends, and Parker and I headed straight to Rady Children’s hospital from Disneyland. When Parker and I arrived at the hospital, my husband was there to meet us. Everything went so fast. They were ready for him immediately. Parker was having episodes of ventricular tachycardia and they needed to get it under control. He was there for 2 weeks. We ended up having to cancel our family summer vacation because going on a cruise ship to Alaska was just too risky and too far from a pediatric heart center. So, again, we pivoted and made the best of our situation.

Once his team had a baseline, we were going to the clinic every other month for follow-up. I could little by little see Parker slowing down. He would get tired easier, but he never wanted to admit it. He never wanted me or my husband to notice. Our lives changed slowly over the course of the next year. We modified the things we did and the way we did them so Parker could live as normally as possible. By late winter of 2020, it was clear that Parker’s heart was running out of fight. He was no longer able to eat and digest a meal, and he was constantly tired. As a mom, it was heartbreaking to watch. Knowing I couldn’t do anything more for him was devastating.
When the pandemic hit, I was quietly thankful for time to be at home with my kids. I was thankful to not have a schedule to adhere to. I was thankful. Both of my parents became sick with the virus, and sadly my dad didn’t make it. He passed on Parker’s 13th birthday in May. By the time July rolled around, Parker was really not doing well, and we ended up back at Rady Children’s hospital for a 15-day stay. He started his 8th-grade year virtually, from the cardiovascular intensive care unit (CVICU). We knew he was very sick, and during this stay, they talked to us about LVADs and heart transplant.
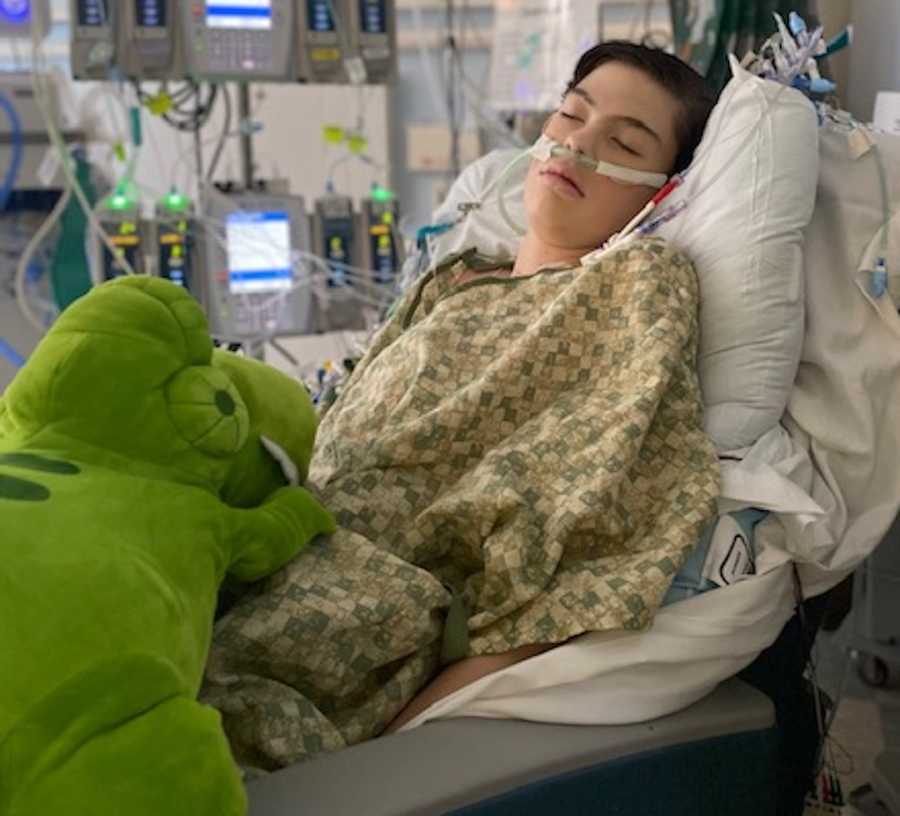
He got well enough to go home mid-August, but that didn’t last long. For the next 2 weeks, Parker would do his virtual schooling until around noon and then sleep until dinner time. He had no energy and still could not eat. I was scared. On the afternoon of September 1, Parker mentioned to me, ‘Something just doesn’t feel right.’ But he couldn’t tell me what was wrong. I told him, ‘Just rest and if it gets worse, we will go to the hospital. If it doesn’t get better, I will call your heart failure team in the morning.’ Well, I didn’t call them, they called me.
At exactly 9 a.m., his electrophysiology team called because they had been alerted of an irregular rhythm by his implanted heart monitor. They asked, ‘Can you come right in?’ And they warned us we could be there a few hours or we could be there overnight. I decided to err on the side of caution and pack a bag, and of course, we needed it. My own heart sunk when I found out Parker was in atrial fibrillation.
That day, Parker had cardioversion, which is where they have to shock his heart back into a normal rhythm. We decided to let the doctors start working him up for a heart transplant. Due to his underlying muscle disease, we weren’t even sure if Parker would be a candidate for transplant, so we were really aiming towards having the LVAD surgery while we tried to find out his candidacy. On September 8, we decided to go forward with LVAD, and surgery was scheduled for September 11. On September 9, we had a really rough night. Some of the medications Parker was on were making him sick, and we ended up being up all night throwing up that night.

The next morning, the CVICU attending decided they needed to take over his breathing, as they were afraid he would aspirate vomit in his bi-pap mask while he was sleeping. I was scared, and to be very honest, I was so mad at the attending for suggesting this. My dad died on a ventilator just 4 months prior to this from COVID-19. But deep down, I knew she was right. I was up with Parker all night the night before, and it was terrifying to watch. So, we consented, and they intubated my baby. All the while, plans continued for surgery the next day.
The night before, they drew labs and prepped him for surgery, the first case of the day. We were scared and hopeful at the same time, as medicine was failing our son and we were losing him. While we were in Parker’s room on the morning of surgery, they called off the surgery at 6:30 a.m. His labs showed signs of infection. He had, in fact, aspirated on his own vomit the night before last, and he had developed pneumonia. It was too risky to send this already very sick child into surgery after developing pneumonia.
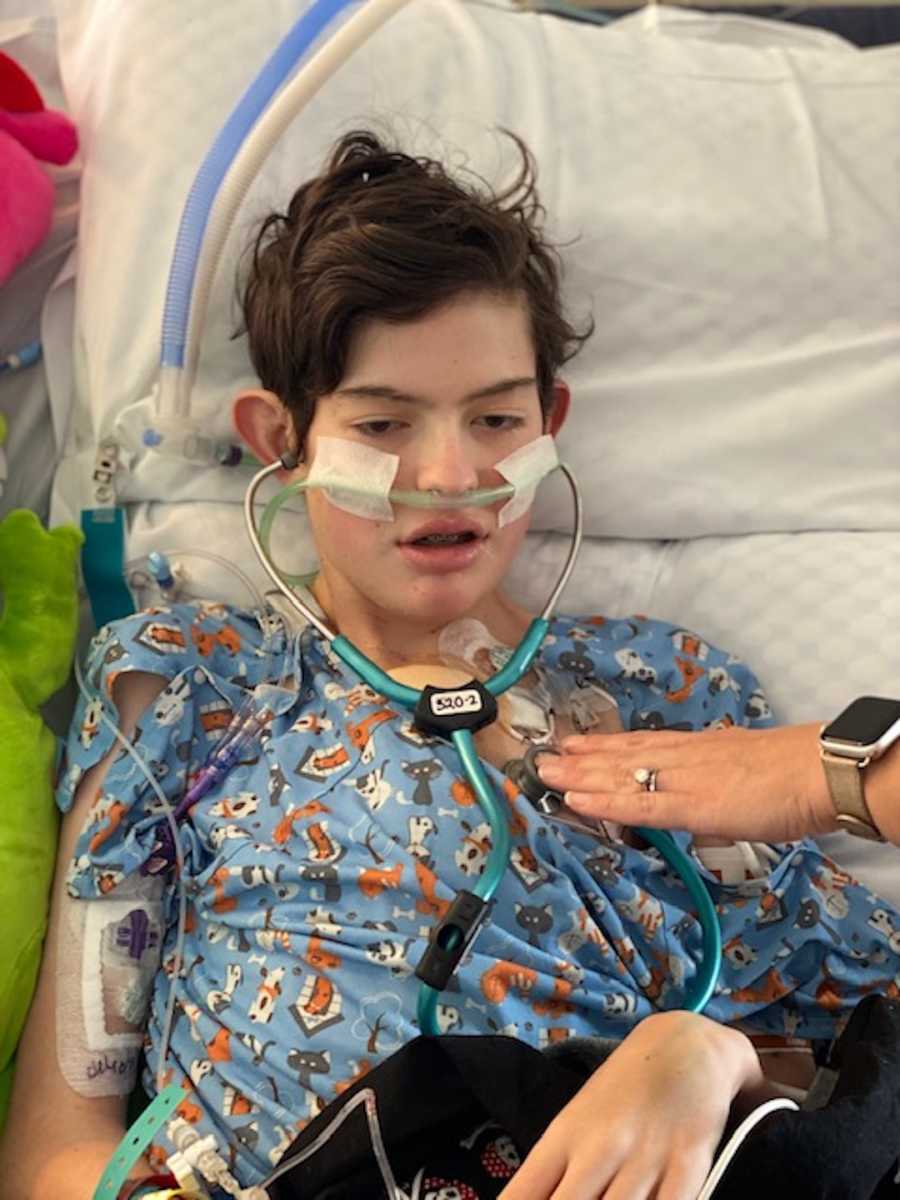
After a very long week and a very heavy round of antibiotics, surgery was rescheduled for Friday, September 18. It was the longest week of my life, and I was terrified every minute of every day. Parker was sedated, but he could still communicate with us a little. He was able to motion when he wanted his mouth moistened, and he was able to ask us what time and day it was. And when he realized surgery didn’t happen, he cried. I felt so helpless.
Surgery finally happened and he did well. He tolerated anesthesia, and it was so wonderful to see him awake and feel his warm hands and feet because he finally had adequate blood flow to his body. From here, the hard work started. He was fragile and weak, and he had to be rehabilitated. He had to re-learn how to chew, swallow, and walk again. From being so ill for so long, my 5’6 child had whittled away to 77 pounds. You could see every bone in his frail little body. So, we immediately started working on getting his weight back and getting him moving again. Parker’s work ethic not only amazed Dan and me, but it impressed his nurses as well. He did everything they asked because he wanted so badly to get better and go home. He missed his brother and his dogs.
The days and weeks were long, and every day we woke up at the Ronald McDonald House felt like Groundhog Day, the movie. We were all so tired and emotionally taxed, and yet we had such a long road ahead of us. We set a personal goal to be discharged to Ronald McDonald House by the first week of November, and home a few days after that. Parker wanted, we all wanted, to spend the holidays at home. We knew a transplant was still in our future, but for right now, we were ready to be home, and be together as a family. And we were almost there, but then Parker started to go into atrial fibrillation repeatedly again. And finally, he had had enough and told me, ‘Mom, I cannot keep coming back here to be shocked into rhythm again every week. Let’s just list me for transplant, I can’t take this anymore.’

So, on Monday, October 26, Parker was listed for transplant. The team had advised us it could happen fast based on Parker’s match information and we hoped they were right. I started getting hopeful he could have a new heart by Christmas, even though I knew people usually waited months for a heart. We had resigned ourselves to spending however long we had to in the hospital, as much as we wanted to be home. We missed our other son and it had been weeks since we had seen him. This pandemic complicated everything.
On the morning of Friday, October 31, one of Parker’s transplant coordinators came bursting into his room and 7:45 a.m., way earlier than we had ever seen Emily before. Parker immediately threw off his bi-pap mask as if he was a catcher throwing off his mask to catch a pop fly. Emily said, ‘Parker, we received a really good offer this morning, and think you should really consider taking it.’ I couldn’t believe what I was hearing! Parker looked at his dad and me, and then looked to Emily with a smile and nodded his head yes. She confirmed, ‘So, you are saying yes, that you want to take the heart?’ Parker replied firmly, ‘Yes.’
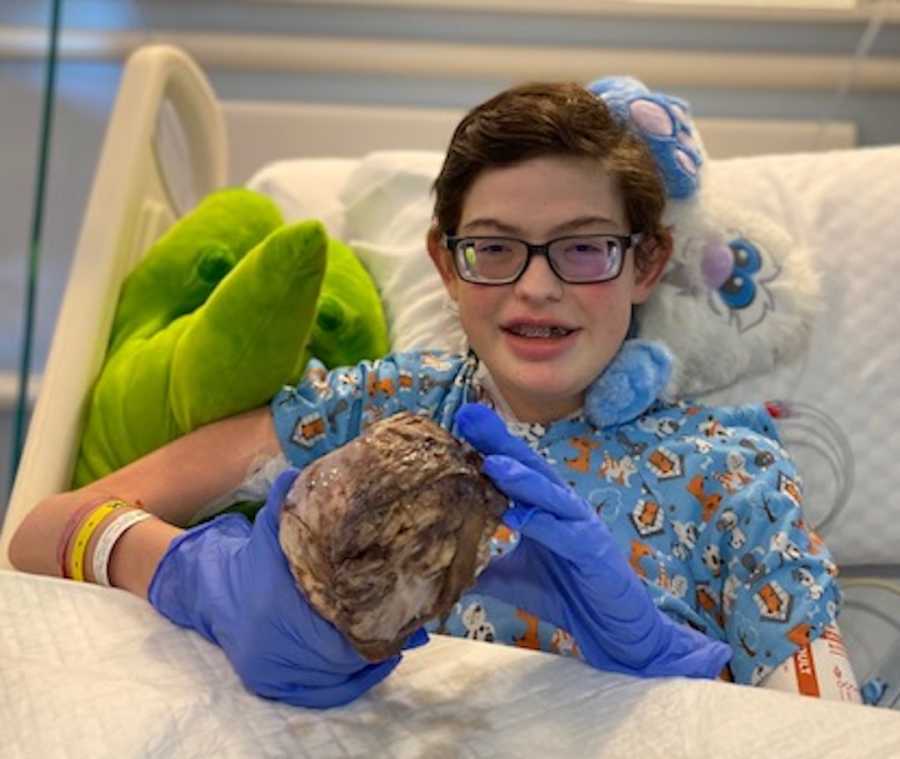
We were in shock and such disbelief, but oh man, were we ever grateful. I could not stop the tears from flowing. They explained to us it was going to be a long day, but the schedule had Parker going into surgery around 5:30 p.m. In the meantime, we had a lot of nothing to do. It was probably the single longest day of my life. We sat around watching TV. We were all hungry. Parker couldn’t eat because of surgery, and there was no way we were going to eat in front of him. The minutes ticked by so slowly. That afternoon, Dan had taken a call outside of the hospital. He saw one of Parker’s heart surgeons, and one of his transplant coordinators, get into an SUV that said something about organ transport on the side of it. He was pretty sure they were headed to get his heart.
A little after 4 p.m., one of Parker’s cardiologists, Dr. Chau, had come in to tell us the team that went to get visualization on the heart had landed. ‘We’ve had visualization and it is a go!’ At this point, Parker was already prepped for surgery, so we had him get onto his gurney and we rolled him down to the operating room. We left him in the competent hands of his team at 5:48 p.m. The doors to the operating room closed, and all of a sudden, I started to panic, and I felt like I couldn’t breathe. It had just dawned on me the timeline. They were prepping him for surgery, explanting his LVAD, and putting him on bypass to remove his heart, but the new heart wasn’t here yet. It was such a frightening thought. So, my husband and I went to grab a bite to eat, and then we decided to take a walk to keep our minds and bodies busy while we were waiting for an update.

We walked loops around the hospital campus, nearly 7 miles worth before we decided to go get a shower and into some comfortable clothes because we knew it would be a long night. The next time we heard from the team was 9:40 p.m., and they called to tell us, ‘Parker is on bypass and the heart is almost here.’ Shortly after that, sometime after 10 p.m., I got a call telling us they were suturing the new heart in. The next call was at 11:36 p.m., telling us they had removed the cross-clamp and his new heart was beating in his chest!
I don’t remember a lot of what happened over the next few hours, but I know we ended up back at the hospital, sitting outside of the CVICU waiting to see them roll Parker by from the operating room back to his room. We saw his transplant surgeon first, and he said, ‘Everything went well and I really need to get off of my feet.’ This was probably about 2:00 a.m. Then, around 2:45 a.m., we saw him! The team was wheeling him back to his ICU room and we got a fist pump from his anesthesiologist. He said, ‘He did great!’ We both fell asleep in the waiting room for a bit after that, and we were finally allowed to see him. He was doing so well! We had a Halloween heart transplant, Parker’s favorite holiday! Today, I’m still in shock he got a heart after waiting just 4 days.

It took a few days to bounce back, but once he did, he was on the road to recovery quickly. Parker developed two donor-specific antibodies that required a few rounds of plasmapheresis, and it set us back about a week, but we were determined. We set a goal to be home by November 24, just 4 days before Thanksgiving. We vocalized these goals to his team and his wonderful nurses went to action advocating for Parker’s healing and ultimately discharge. He worked hard every day. On Friday the 13, his transplant coordinator told us, ‘My goal is to have him home by next Friday, 4 days ahead of schedule.’ We tried not to get our hopes up, but it was hard. But we worked hard and did all of the things that were required of us. On the morning of the 20th, his echo looked good, and his surgeon gave his blessing by removing Parker’s transthoracic line. We were on our way home!
We’ve been home almost four weeks now and we’ve never been happier to be on stay-at-home orders. It’s true when they say there’s no place like home. There really isn’t. I celebrated the best Thanksgiving of my whole life this year and I couldn’t be happier. We are looking forward to a quiet Christmas at home and starting our letter to Parker’s donor family. Parker is doing great and he has more energy than he’s had in 2 years.
In spite of all of the terrible and trying things life has thrown at most everyone this year, we remain thankful and positive. There is always something to be thankful for. Always. We got our son back.”

This story was submitted to Love What Matters by Melissa Mayorgas. You can follow their journey on Instagram. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Provide hope for someone struggling. SHARE this story on Facebook with family and friends.