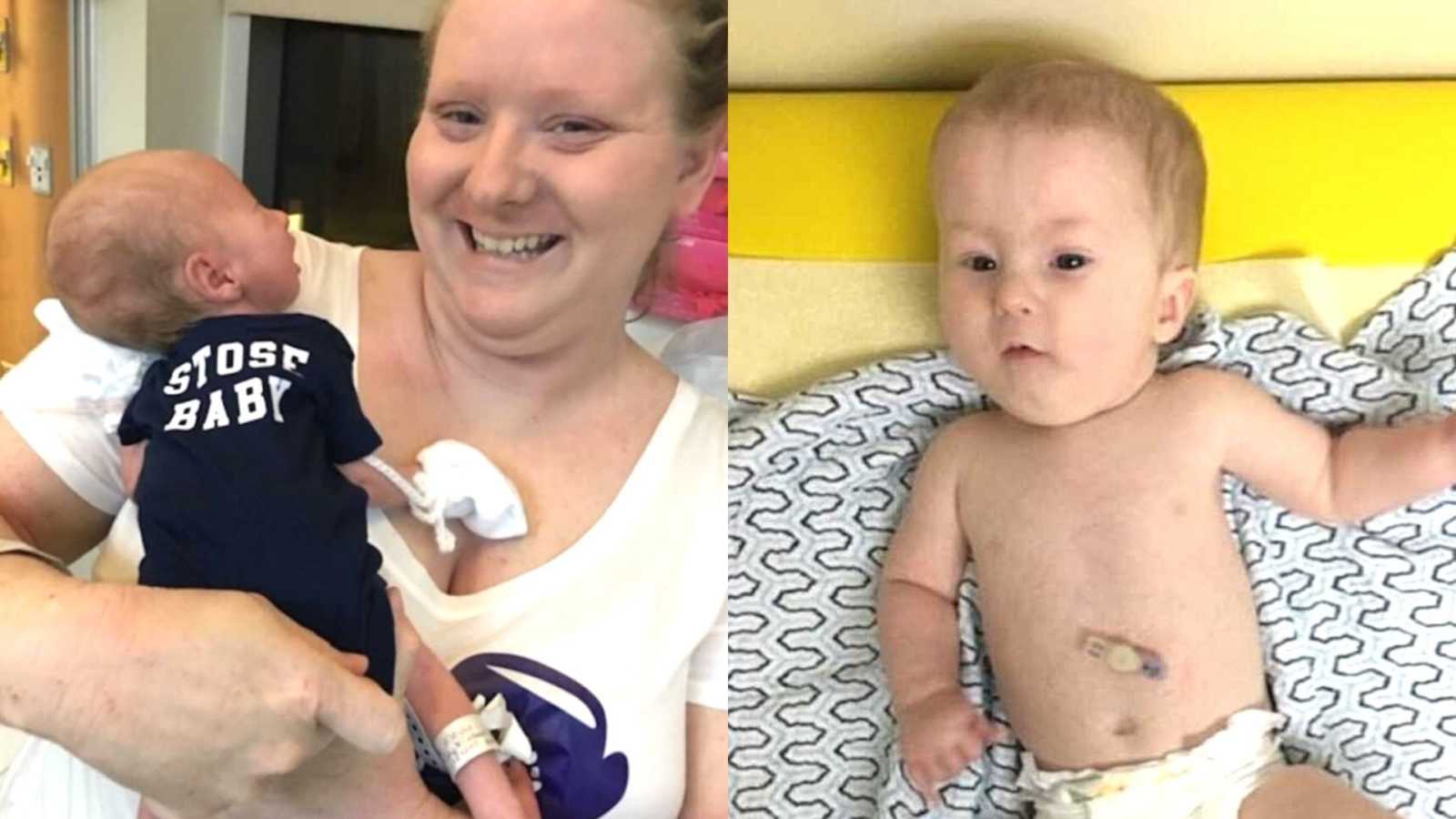
“I’ve wanted to be a mommy since I was two years old. I had baby dolls with outfits, bottles, strollers, and doll cribs. I walked around with my baby dolls under my shirt mimicking breastfeeding and I would put them in time-out when they misbehaved. As I grew up and made plans for what I thought life would look like I just assumed that I would get married, immediately have children, and live happily ever after.
It took me one year to get pregnant after I started trying. One year in the grand scheme of things isn’t actually that long but for me, it was filled with months and months of disappointments and negative tests. When I did actually receive a positive pregnancy test, I was absolutely ecstatic and a little overwhelmed. My time had finally come and I was expectant for a happy, healthy, and glowing pregnancy.
When the doctors attempted to complete the first anatomy scan, they stated the baby was just too small for accurate results and we would try again later. The next anatomy scan was at my 32-week ultrasound appointment and it changed my world. My son, Gatlin, wasn’t measuring correctly for his growth. The doctor’s office repeatedly checked my dates but I was positive on his conception date. Gatlin’s head size was appropriate but his femur bones were measuring two weeks behind where they should be and his stomach was a month behind! ‘What does this mean? Why isn’t he growing right? Have I done something wrong?’ I was at that appointment alone. I hadn’t expected to need anyone with me. The doctor told me I would be coming twice a week and getting ultrasounds at each visit. Then my OB started discussing possible early delivery, being prepared, possible issues with my placenta’s blood flow, and the baby’s growth. I left the office feeling overwhelmed and unsure of anything, and with no answers as to why this was happening.

My next appointment was three days later. The doctor explained Gatlin had IUGR (intrauterine growth restriction), which meant my placental blood vessels were restricted and Gatlin wasn’t receiving the necessary amount of blood flow and nutrients. He had demonstrated all necessary movements on the ultrasound and as long as that stayed the same, our goal for delivery would be 37 weeks or later. The office told me to pack a bag for the hospital just in case. After that appointment, I was sent to the hospital to start steroid injections to aid in Gatlin’s lung development, in case early delivery was needed. I still felt there was plenty of time and found myself in complete denial an early birth would occur.
On November 2, 2018, I had just turned 34 weeks and went into my OB’s office for another ultrasound. This one felt different. The ultrasound was taking longer than expected, the tech wasn’t talking to me as much as usual, there was an air of uncertainty. After the ultrasound, I was moved to a room to talk to my OB and he told me for 30 minutes, Gatlin had not moved. He had a heartbeat but I was told to drive immediately to the hospital and they would start induction tonight. ‘What?! I don’t understand? No one is here with me! Why am I going to the hospital? It is too early! I can’t have my baby right now, he isn’t big enough! He isn’t supposed to come this early!’
My family came but they told me I needed to keep my visitation down. I couldn’t believe this was happening. By the first night, despite everything I started to get excited my baby was coming. I was still afraid, but I blocked those feelings. The next morning, the doctor broke my water and started me on medication to speed up my labor. Labor progressed very slowly. As the day progressed, I began having complications and that is when my OB decided it was time to go ahead and have a c-section. I was devastated and felt so overwhelmed because it didn’t seem like I was able to be in control of anything. I was rushed to the operating room to have surgery. During the c-section, it was discovered I had an additional complication of a Bandl’s ring on my uterus. A Bandl’s ring obstructs labor and contracts around the uterus preventing delivery. Once inside, they had difficulty getting Gatlin back out of my uterus because of the Bandl’s ring and the fact he had already started heading into the birth canal. It took three people to pull him out of me. After Gatlin was delivered and I heard the very faintest of cries, they took him away from me.
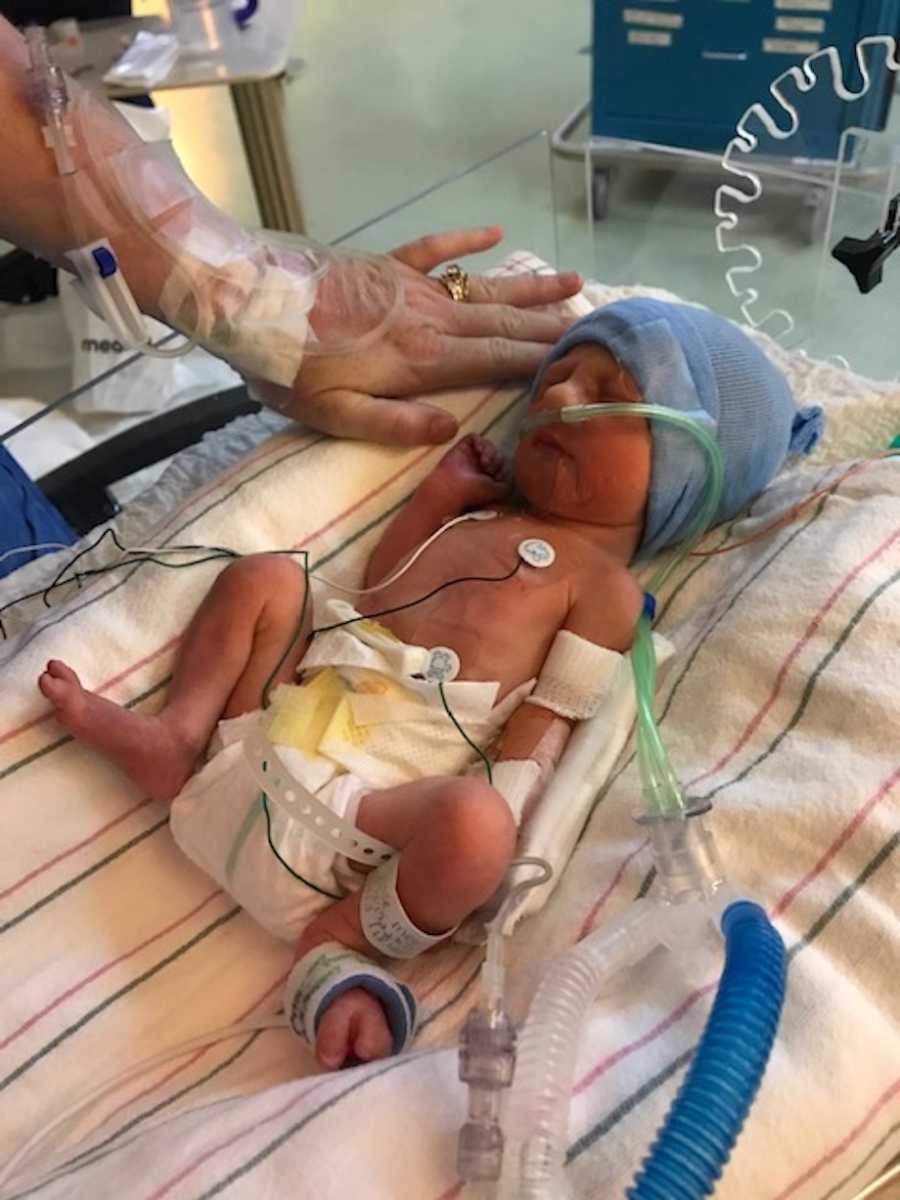
Once released from recovery, they wheeled me to the NICU to see him. I had never seen a baby so small. He looked strange to me because he was unlike any other baby I had ever seen. He weighed only 3 pounds and was 7 inches long. He had tubes all over his body and when they put him on my chest, I barely felt the weight of him. It’s an emotionally overwhelming and painful experience.

I spent as much time in the NICU as possible but was constantly being prompted to return to my room for meds and rest. I found this the most difficult because I NEEDED to be with my child. Once officially discharged, I spent all day every day in the NICU and only took breaks to eat or take care of necessities. I snuggled with Gatlin, sent pictures to family and friends, sang to him, and just listened to the commotion around me. Breastfeeding was on the top of my priority list because if nothing else, I knew this was something I could give to my baby. Although the lactation consultants worked with me diligently, Gatlin wasn’t sucking and my milk didn’t come in as I had hoped. I painstakingly pumped and tried to nurse with limited success. Gatlin ended up needing to have his milk fortified because of his need for increased calories to properly grow.

The more time I spent in the NICU, the more I learned. I made it a point to be there for rounds so I could hear what the doctors, nurses, and therapists had to say about my son. I learned despite being born 6 weeks early and despite having IUGR during pregnancy, Gatlin still seemed to be delayed in reflexes. He had significantly low tone, wasn’t demonstrating appropriate reflexes, his testicles hadn’t descended, and with little-to-no suck, he wasn’t thriving. The doctors decided to run genetic testing stating they believed these tests would come back with a diagnosis.
At about three weeks old, Gatlin was diagnosed with a rare, genetic disorder called Prader Willi Syndrome. PWS happens in about one out of 15,000 births and is the most common cause of life-threatening childhood obesity. Basically, there is a chromosomal abnormality that causes a variety of symptoms that change over time. The abnormal growth during pregnancy, the weak cry at birth, the lack of suck for feeding, as well as the floppy and weak muscle tone are all symptoms of Prader Willi Syndrome. I was faced with a baby that was labeled as ‘Failure to Thrive’ and presented with literature that painted a bleak and miserable life ahead for my son. I was told he would have an insatiable hunger, become extremely obese, and have a significant intellectual disability. Prader Willi Syndrome affects the endocrine organ in the brain called the hypothalamus. This organ regulates temperature and pain, it regulates satiety and hunger, as well as the wake and sleep cycle, fluid balance, fertility, and emotions. Basically, the part of the brain which controls all of these vital bodily functions is abnormal.
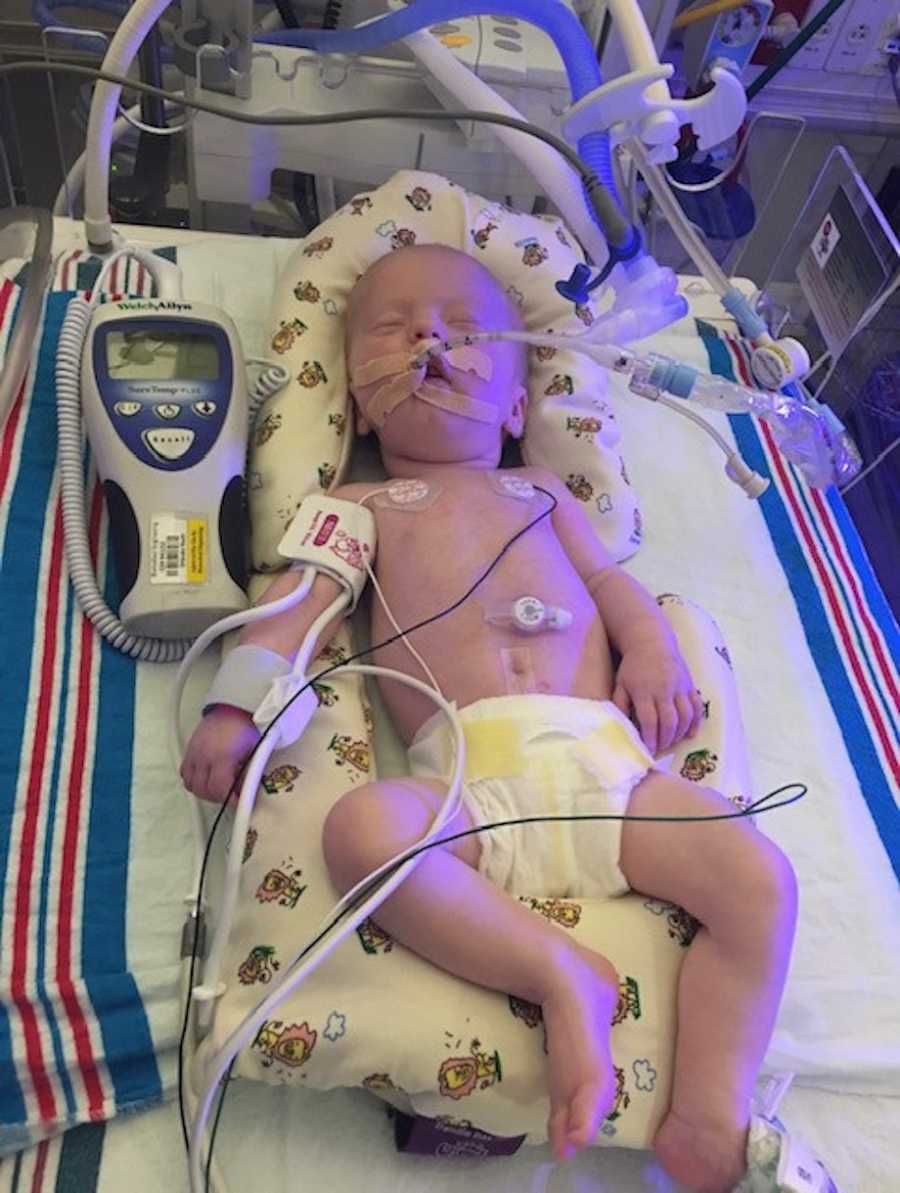
I was devastated. The news was horrific and all-consuming and seemed like an impossible journey with detrimental side effects for my little boy. I was wrought with dismay and anger and uncertainty. Why me? Why my family? I had waited for so long to be a mom and now this? Can I do this? What do I tell people? Who will understand? Will my son have friends? Will he get to go to school?
I decided to have Gatlin moved to another NICU at a children’s hospital about 2 hours away from home that was better equipped to handle the needs of Gatlin. He was taken by ambulance to the children’s hospital where we met another team of doctors, nurses, therapists, and specialists to care for him. We spent the first few days being observed and allowing the team to make their own assessments. I was now even further away from my family and friends but I knew this was the best place for Gatlin. It was here I was able to be alone with my child for the first time.

Gatlin still wasn’t able to nurse from me or suck from a bottle. It was determined he needed a g-tube inserted into his stomach in order to provide him with nutrition and fluids. Surgery was required for the tube to be placed. I thought that we had already gone through the hard parts but it turned out that surgery was even worse. Gatlin had difficulty waking from surgery. He took longer than expected to come off of the breathing vent. He did finally wake up and get off that ventilator and I re-learned how to care for him. I learned how to use and clean his g-tube site and how to work a pump I would program and use to pump milk into him for nutrition. I had to demonstrate my ability and willingness to appropriately care for my child before discharge would even be discussed. We had already missed Thanksgiving and I was begging to please let us home for Christmas. 51 days after birth, PRAISE GOD, Gatlin was discharged and went home two days before Christmas.

Once home, the first few weeks were a whirlwind of learning how to adapt. At that point, I lived-in three-hour increments trying to nurse, then pump and hooking him up for slow tube feedings that lasted for an hour. It was exhausting and I felt like a failure those first couple weeks. Eventually, I got the hang of everything and we began to find our routine together.
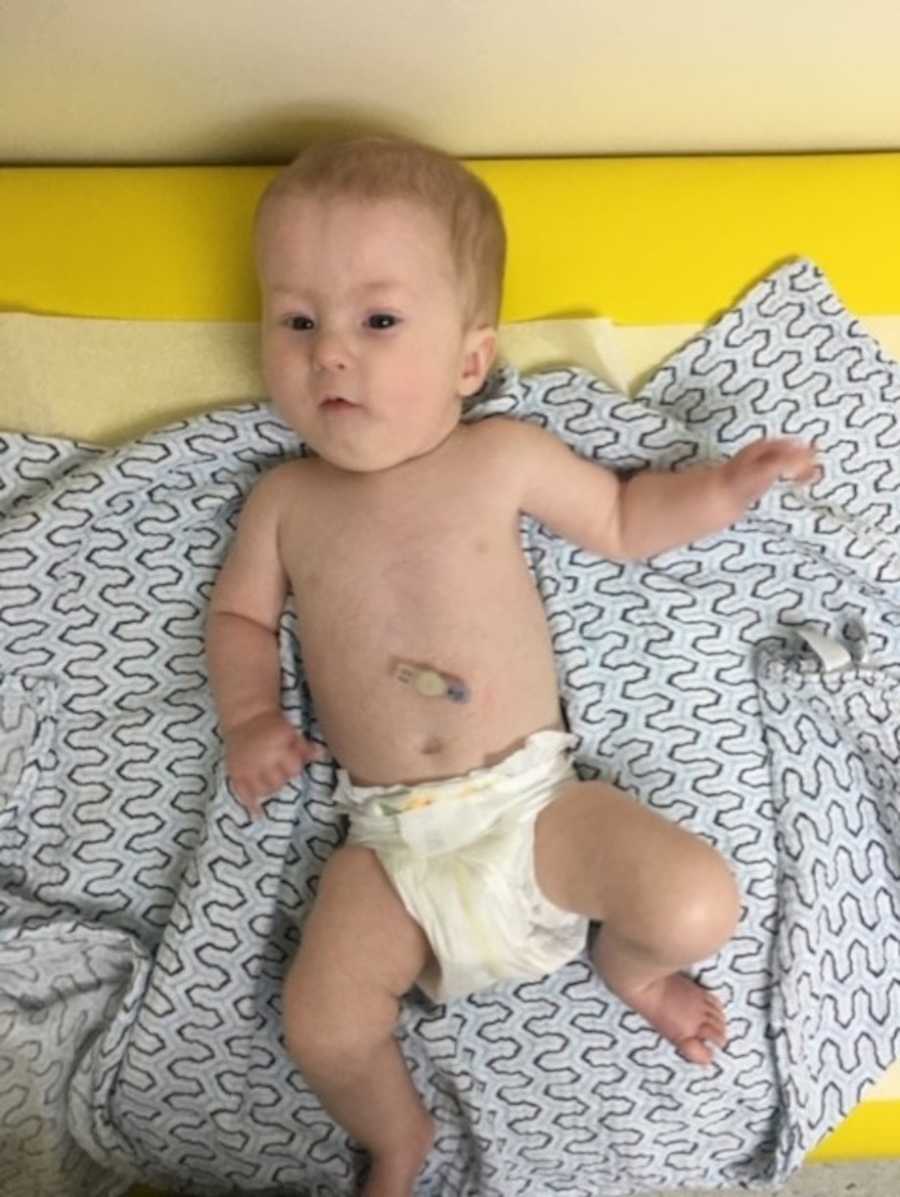
I took the time to start researching Prader Willi Syndrome and figuring out what was our next step. I found out the world-renowned Prader Willi Syndrome Specialist and Pediatric Endocrinologist, Dr. Jennifer Miller, practiced only a few hours from us and so I set up an appointment to meet her. In the meantime, we met with other specialists all over the state. I pushed for Gatlin to begin therapy. I found support groups online where I met other parents with infants and children also diagnosed with Prader Willi Syndrome. I started to feel hope for my future.

Dr. Miller changed my whole perspective on what our life would be like. She explained Gatlin will live a full and happy life and there were treatment options. She painted a new picture of a sweet, loving, and happy little boy who could do all things as long as he worked for him. His journey would be more of a struggle and he would have to put more effort in than his friends but he had the ability and potential to be everything he and we hoped he would be.

I came back from my appointment with her feeling refreshed, empowered, and capable. Life slowly evolved and I found myself as a single parent. I had never returned to work due to the significant amount of time and care necessary for Gatlin. I decided to turn my crafting hobby into a business and utilized social media in order to support us financially. I also use my business to bring awareness apparel to rare disorders like PWS. Life is different than I planned but much more beautiful than I could’ve imagined.
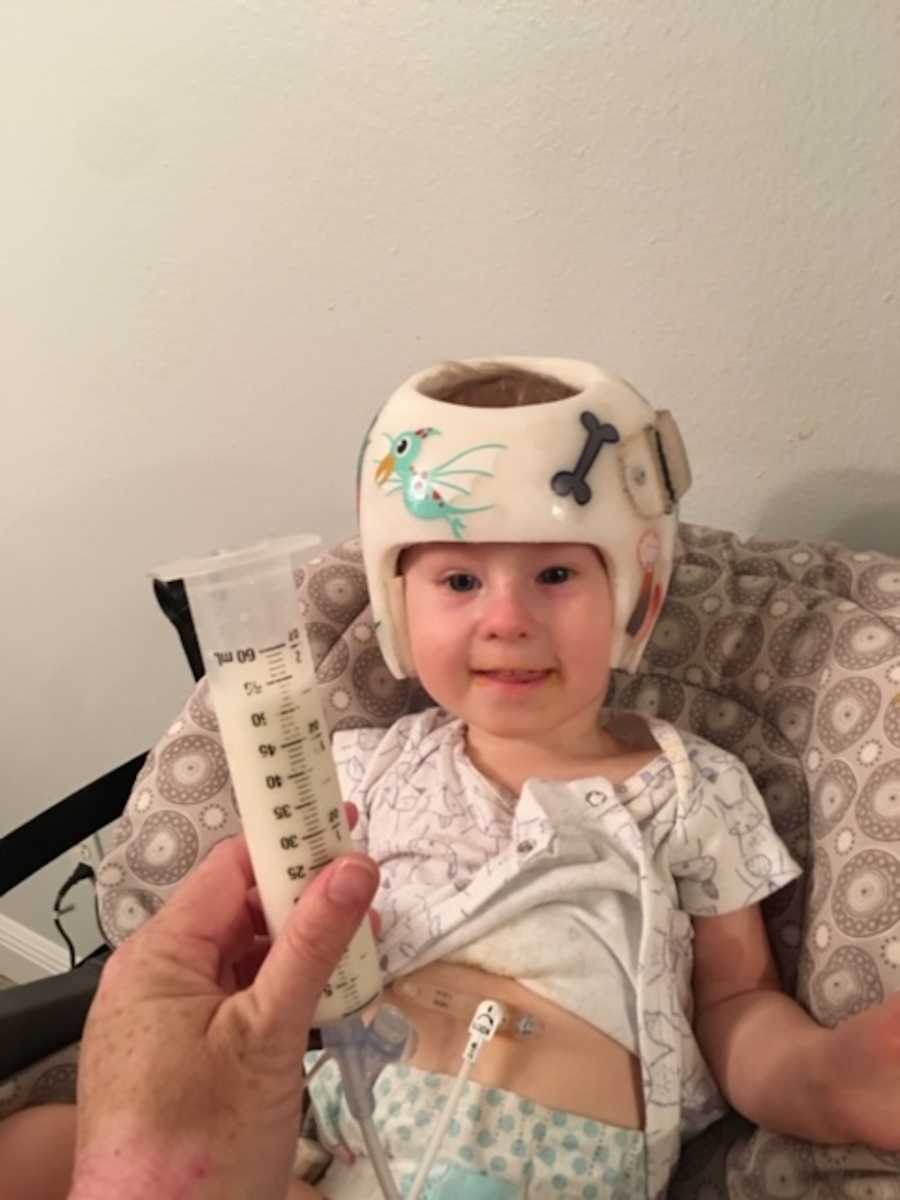
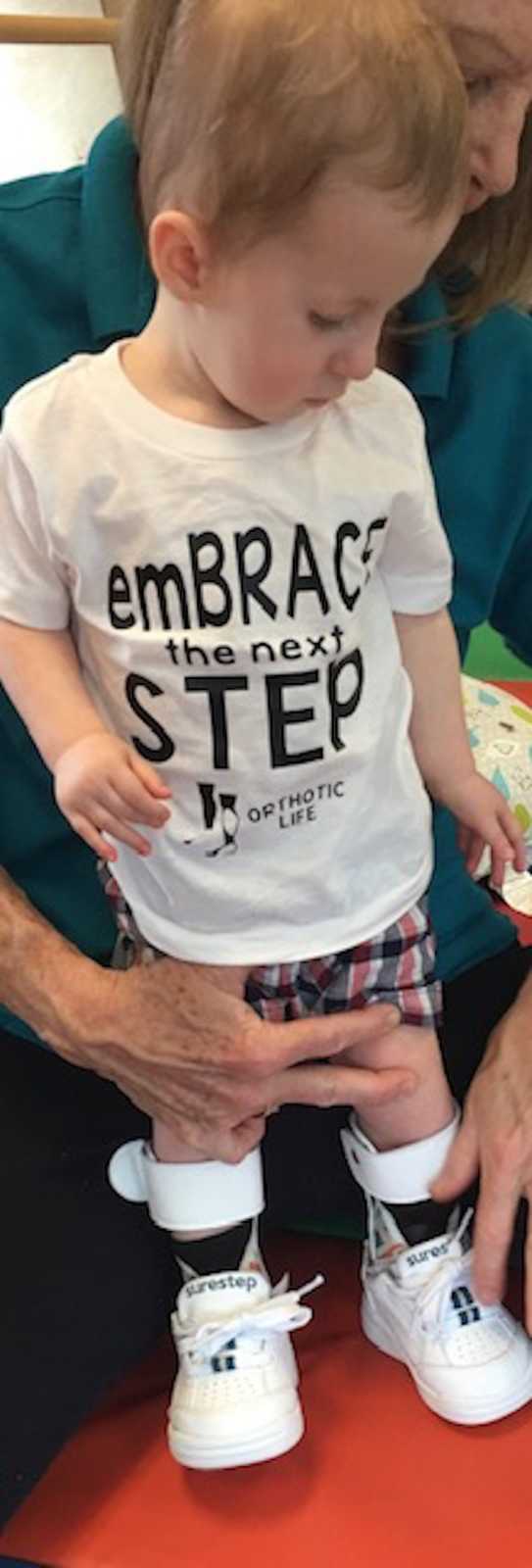
I began to advocate for what Gatlin needed and got him started in early interventions. Currently, he sees Physical Therapy, Occupational Therapy, and Speech Therapy each twice a week. He also has begun Aqua-therapy as well. His g-tube is still necessary for supplementing his nutrition and fluids. He is working on swallowing thin liquids and learning to eat semi-solid foods. Physically, he is delayed but I am constantly looking for ways to adapt and improve life for him. He is 20 months old right now and still weighs less than 20 pounds but is finally starting to get on the growth chart. He learned how to finally sit up on his own about two months ago and we are now teaching him how to crawl. His speech is delayed but he is making more and more verbal sounds, following directions, and working on mouthing words in order to produce increased language. He requires some oxygen at night for sleep apnea and uses a pulse-ox machine to monitor him while asleep but it reassures me he is breathing normally.
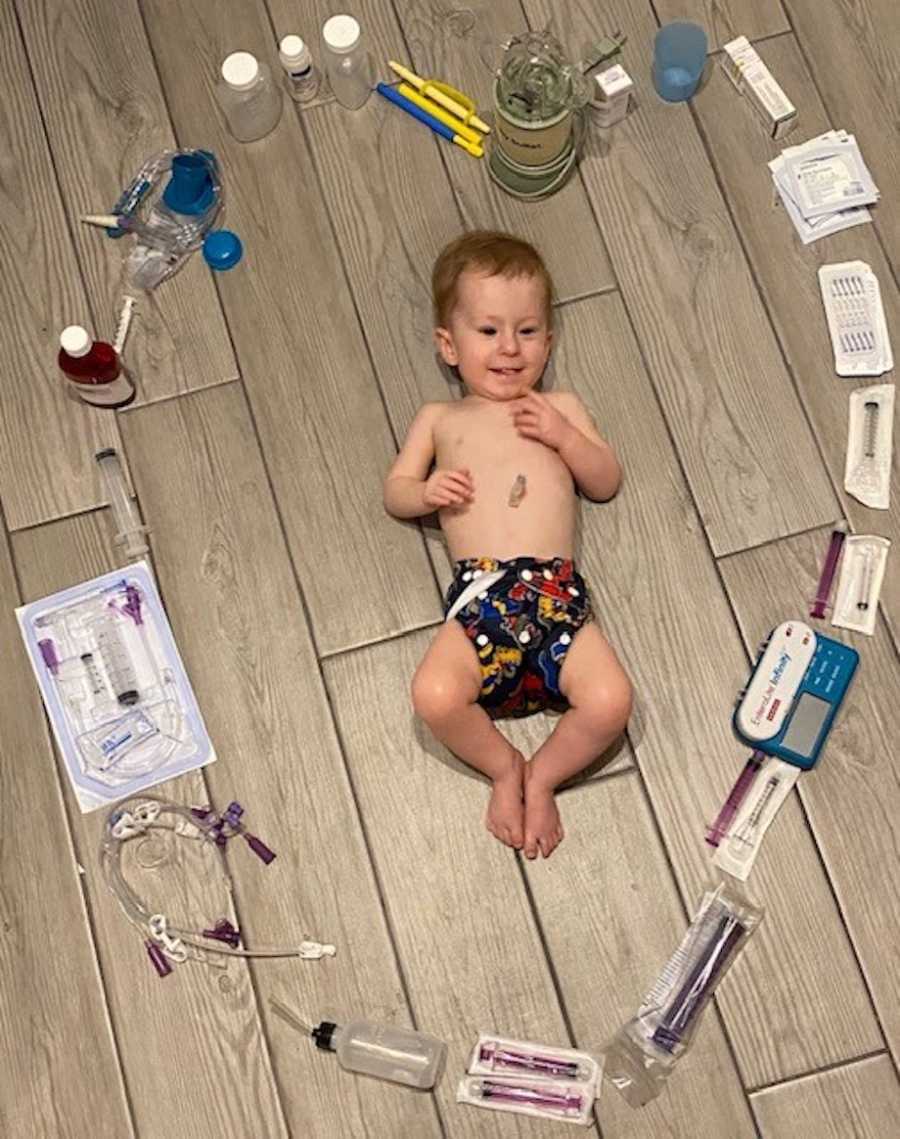

I still find it difficult not to compare him with other children his age but I know I am blessed beyond measure. Obviously, we are still in the beginning stages of PWS and have not reached a point yet where excessive hunger, obesity, or behavior have come into play. It’s hard to imagine those things but I can’t fear the future. All we can do is take one step at a time. Prader Willi Syndrome is a part of Gatlin’s story but I refuse to let it define him.
I am overwhelmingly grateful for the support I have from family, friends, and those who surround us. I know we have so many people here to pray for us and lend a helping hand. I have started telling Gatlin’s story and have met so many other families with the same diagnosis or who simply understand what it is like to have a child with a rare disease.
When we were first diagnosed and I sat alone in that NICU simply holding my baby, I did a lot of research and found information on PWS and what to expect was very limited. I found some resources eventually but the general search is scary and negative. I couldn’t find any awareness apparel like you can for a well-known disability. I couldn’t any find positive stories on the kids who are thriving today versus adults who have suffered for their whole life. Now I have survived the pregnancy, come out on the other side of a traumatic birth, lived through what most others will never understand, and become secure and confident in our journey — I have found a new desire to advocate not only for Gatlin but his diagnosis as well.

Advocating for Gatlin and detailing his journey with Prader-Willi Syndrome has become a mission for me. I want Gatlin to be surrounded with acceptance and support for the challenges he faces in life but I also want him to be included for who he is and not what diagnosis he may have. He is the biggest blessing of my life. I know he has and will touch the lives of every individual he meets.”
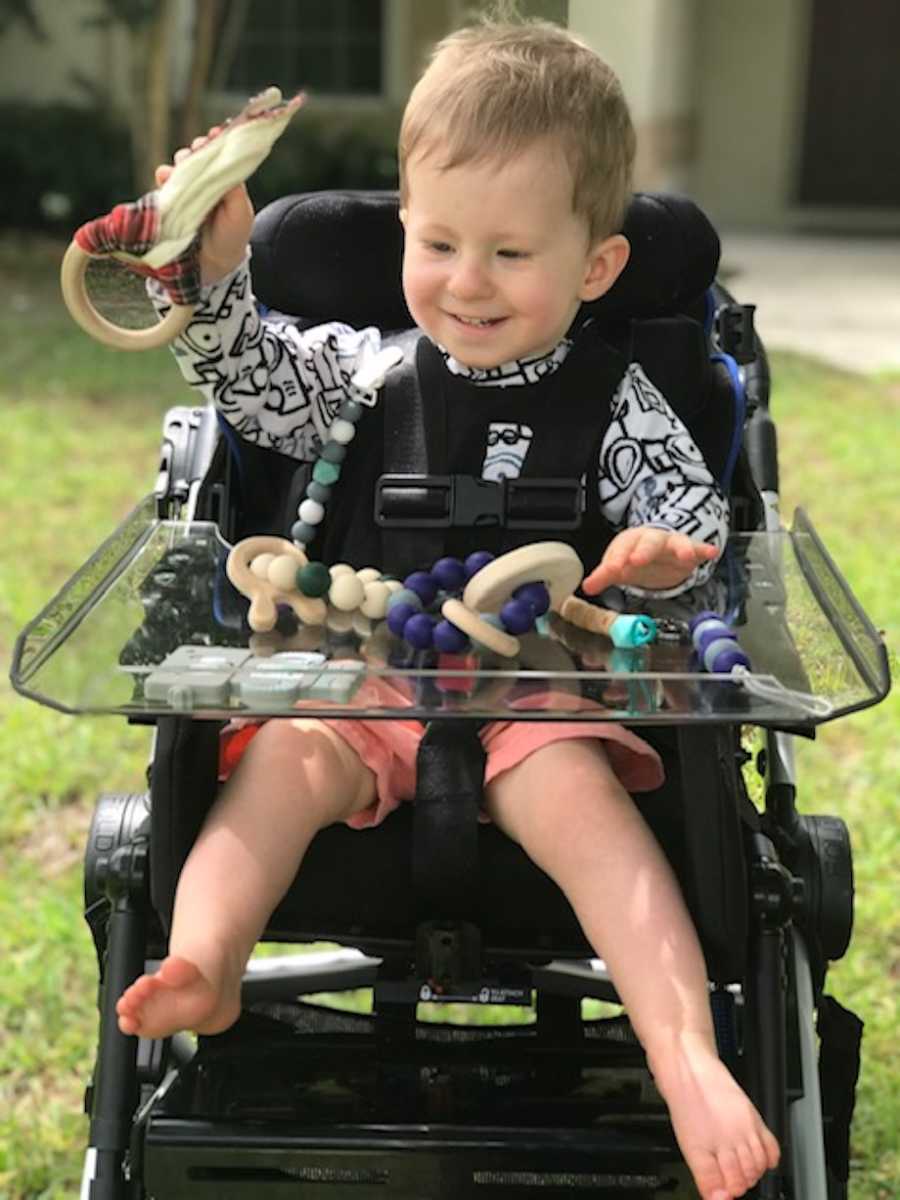
This story was submitted to Love What Matters by Megan Dempsey Stose from Palm Coast, FL. You can follow their journey on Instagram and Facebook. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more touching stories like this:
Provide beauty and strength for others. SHARE this story on Facebook with your friends and family.