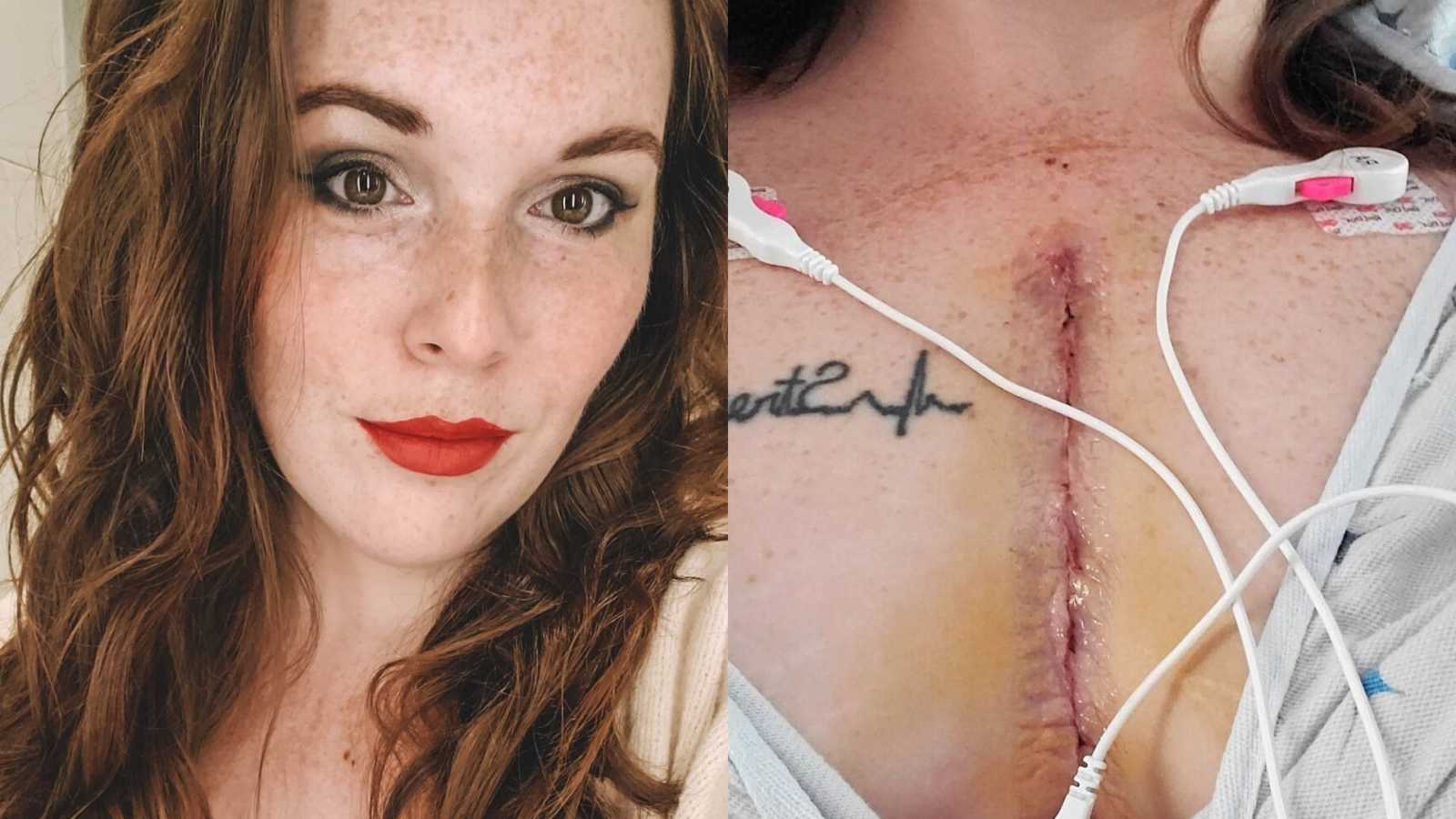
“‘Do you mind if I have someone else come take a listen?’ Little did I know how often I’d hear those words throughout my lifetime.
From the time I was really young and seeing a pediatrician, I’ve always been the patient that requires ‘extras.’ Extra nurses, extra labs, extra tests. Each time a doctor would listen to my heart through a stethoscope, I would watch their facial expressions turn. They’d listen, and then they’d always ask the same thing: ‘Do you mind if I have someone else come listen to this?’ I would always say, ‘Sure, I don’t mind.’ But I never understood why they wanted other people to listen. Honestly, it was embarrassing.
I was born with a congenital heart disease (CHD) called Aortic Stenosis. Unfortunately, it wasn’t until YEARS later we actually had a name to put with it. Until that point, I was always told I just had a murmur. When I was 14, I was referred to a cardiologist at Nationwide Children’s Hospital for an echocardiogram (echo, for short.) An echo is an ultrasound of the heart where doctors can more closely look at the inside of the heart including the chambers, valves, arteries, walls, etc. The average echo takes roughly an hour. Afterward, I met with my cardiologist to review the results. That’s when I was told I had Aortic Stenosis, a bicuspid aortic valve, as well as large amounts of regurgitation (blood flowing backward back into the heart.)
Aortic Stenosis is a condition where the aortic valve of the heart is narrowed. In a normal aortic valve, there are three flaps that open and close to allow oxygenated blood to travel from the heart, into the aorta, and into the rest of the body. Stenosis can be caused by calcification on the valve flaps, or by the flaps fusing together, which then would result in a bicuspid or unicuspid valve. In my case, I had both fused flaps and calcification. During fetal development, two of my three flaps had fused together, only allowing one to open and close.
For years, I struggled to participate in regular ‘kid’ activities. Running, playing, and sports were especially difficult, but I always blamed it on asthma. It felt like my lungs would just run out of air. The older I got, the worse it got, to where I would get winded just walking up a flight of steps. I was exceptionally tired all the time and was always very cold. The remainder of my teenage years were relatively ‘normal.’ I had friends I spent every possible moment with, I was involved in riding and showing horses, I graduated high school, and went to college.
In October of 2011, I was 18 years old and went back to the children’s hospital for my annual checkup. All of my results came back similar to the year prior and showed no major changes, so I was given the green light to come back for my next check-up in 2 years instead of one. At that time, I felt like everything was going well.
2 years later in December of 2013, I went back for my next checkup. Given my last one had gone so well, I really wasn’t concerned. I only had my echo that day and didn’t get to actually meet with the cardiologist. A few days later, I was at a restaurant having dinner with a friend when I got the call from my cardiologist to discuss my test results. The restaurant was loud and had terrible reception, so I stepped outside. I heard his voice, and the first word out of his mouth was, ‘Unfortunately…’ and suddenly I felt like I had been sucker-punched. At 20 years old, I was told I was going to have to endure open-heart surgery to fix my diseased valve. I had so many questions but was so shocked, I couldn’t even ask them. After I hung up the phone, I gave my friend the news and then went home to inform my family. My head was spinning, and I had no idea what came next.
I can’t remember how long it was after that phone call I had to return to the hospital for testing, but it was within a few weeks. I was scheduled for another echo, an EKG, and a stress test. I had no worries about the echo and EKG because I was so used to them. I had never had a stress test, though, so I wasn’t sure what it would consist of. I was hooked to a few monitors and asked to walk on a treadmill for some duration of time.
As I walked, the nurses would gradually increase speed and incline, and not long into it, I was jogging on the treadmill. The nurse told me to push myself, but to also stay aware of how I was feeling and to stop if I needed to. I could feel my lungs struggling to keep up, and my chest became tighter as I pushed myself. But I wouldn’t stop. I was so determined to prove to them, and to myself, I was strong. I was not willing to accept defeat. I pushed myself until they stopped the treadmill. I stumbled off the treadmill, face beat red, and so winded I couldn’t talk. I was dizzy and my lungs felt like they were on fire.
After I gathered my composure, I was off to meet with my cardiologist. We discussed all the technicalities of my heart such as the gradients, the blood flow, the overall function. He then told me even though there had been definite changes in my valve, I was still walking the line between ‘moderate’ and ‘severe’ stenosis. He then told me they will not operate until I am considered ‘severe,’ because insurance wouldn’t cover it otherwise.
I don’t remember exactly how I responded to those words, but I was so angry. Livid, actually. I had finally begun to make peace with the fact I was going to need this life-saving operation, and then I was basically told, ‘Oh sorry, you’re not sick enough yet.’ I was hurt, disappointed, stressed, angry, confused. I felt like a price tag had literally been put on my life.
‘So what’s next?’ I asked. ‘We wait and see how your valve progresses,’ was the answer I received.
We discussed options for surgery because I had the option to pick what type of valve replacement I received. The first option was to try and repair the valve. It would still be open-heart surgery, but it would (theoretically) be less difficult since they would be using my own valve tissue to repair it. However, this was a relatively new procedure and wasn’t around long enough to have any real statistics on its longevity. They weren’t sure if they’d be able to repair it, or even if it would last. The next option was to use a bioprosthetic valve or tissue valve. This option would consist of the surgeon cutting out my existing valve and replacing it with that of a pig or cow. This option was only guaranteed to last 5 to 7 years. The third option was what is called a Ross Procedure. In the Ross Procedure, the surgeon would remove my existing pulmonary valve and use it to replace my aortic valve, and then give me an artificial pulmonary valve. Lastly, was the mechanical valve. This valve is the most durable and would likely last me the rest of my life, but it would also require me to be on blood thinners for the rest of my life, therefore making any future pregnancies extremely dangerous.
Having so many options at such a young age was overwhelming. I wasn’t sure at the time if I wanted to have children, but I knew I wanted the option. The next several weeks were spent listing the pros and cons of each option. After careful thought, and consulting with my medical team, my family, and friends, I had decided to try for the repair and to do the mechanical as a backup if the repair wasn’t able to be done.
Not long after, my valve finally hit the ‘severe’ stage and we had a surgery date scheduled: December 4, 2014. The day finally rolled around, and I was a nervous wreck. Once my pre-op tasks were done, my surgeon came in to discuss the procedure. He confirmed he’d try to repair the valve and would use the mechanical as a backup if needed. I was then asked if I had any questions before we got started. I only had one: ‘What’s the probability I’ll die?’ His expression shifted and he was comforting as he told me the mortality rate was less than 3%.
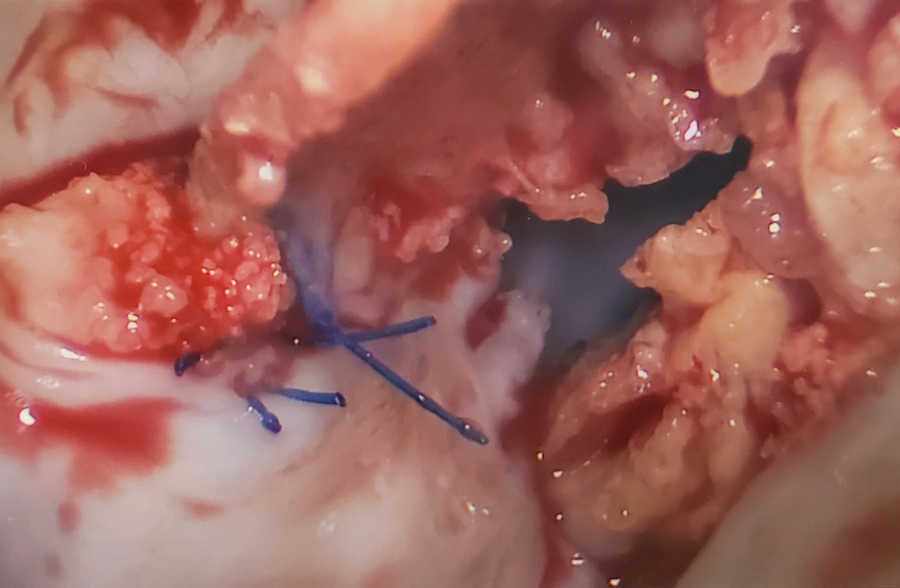
I was then wheeled back to the operating room. I woke up nearly 9 hours later in the Cardiac ICU. I remember looking at my family’s faces, the nurses, my feet, and thinking, ‘I’m alive. I made it.’ There were minor complications such as some blood pressure issues, but overall, the surgery went great. The repair was completed, with a little help from some cow tissue to replace the flaps that were too badly damaged.
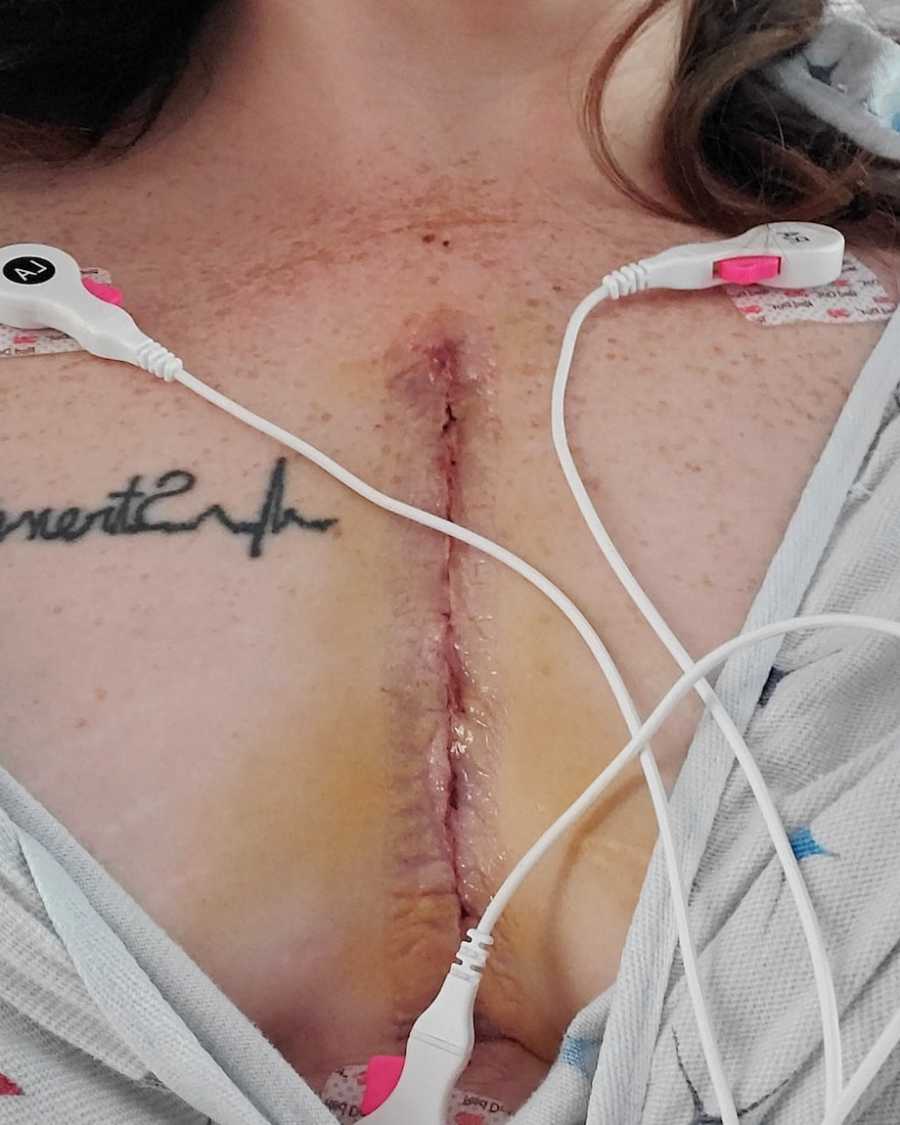
While my surgeon was inside my heart, he discovered I actually had a unicuspid valve instead of the bicuspid valve we thought I had all along. I spent the next 4 days being the BEST heart patient I could be. I was up walking, showering, moving, eating – everything I was supposed to do before I could go home. I was finally released on day four.
My recovery went incredibly well and I was back to work at 7 weeks post-op. The next few years were life-changing. I had energy I had never felt before. I was able to run, play, jump and move in ways I never thought I’d be able to. At each follow-up visit, I was consistently told how great my results were and if they could, they’d have my results in every one of their patients.
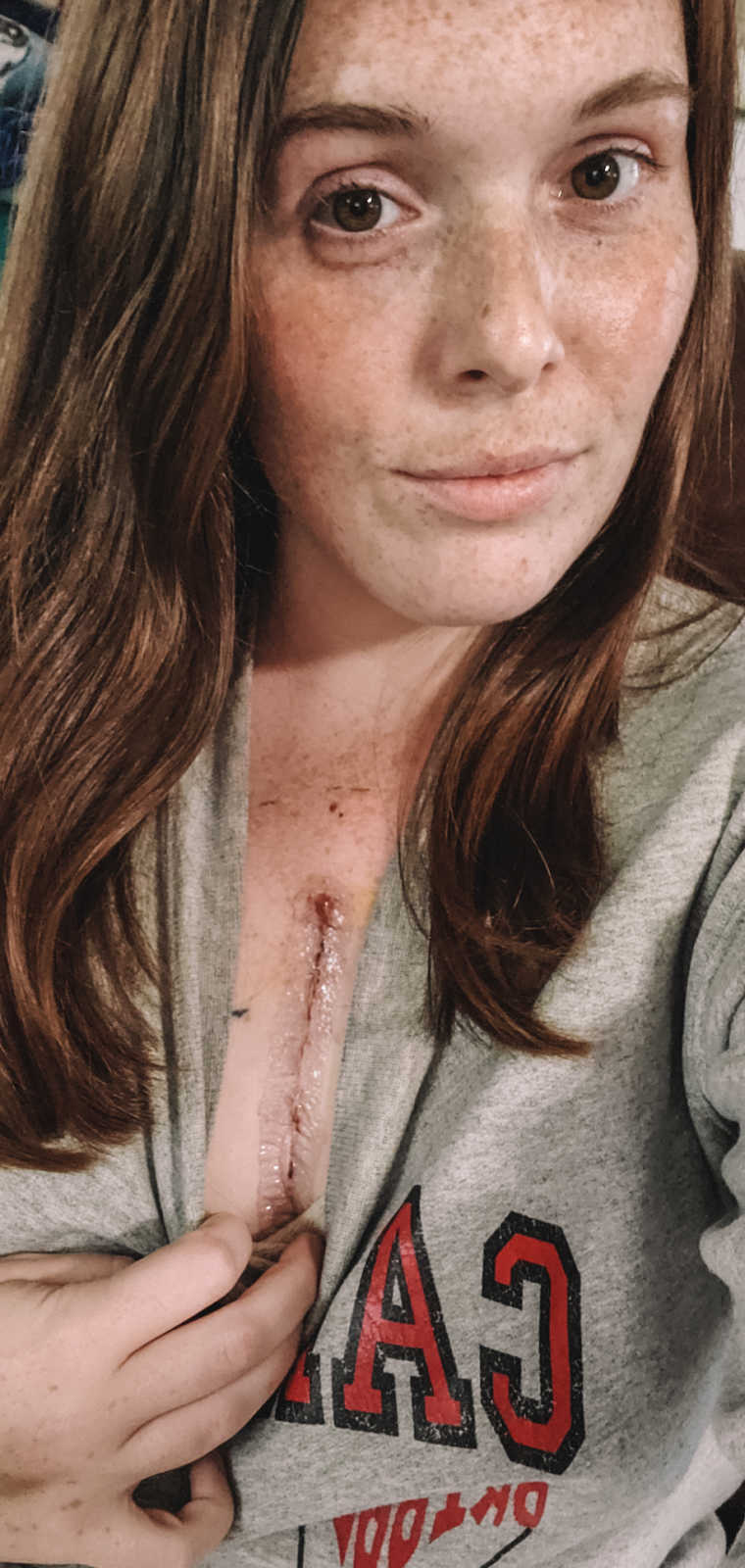
Roughly 2 years after surgery, I got pregnant with my first child. It was a rough, high-risk pregnancy due to my heart. Pregnancy puts so much stress on the heart, I was very closely monitored. It wasn’t a pleasant experience for me and at 35 weeks pregnant, I ended up with pre-eclampsia. I was induced at 37 weeks because my body was retaining so much fluid, and in August of 2017, my husband and I welcome our sweet 5-pound, 13.5-ounce baby girl into the world.
Fast forward. In May of 2019, I went back to the cardiologist for my annual checkup expecting to receive the same glowing results I always had since my surgery. So when I was told my valve had started to calcify again pretty badly, it hit me like a ton of bricks. This was not the news I was expecting. And suddenly, every scenario of my daughter growing up without a mother went flashing through my mind. I had to have another surgery, but again, we had to wait until I was even sicker.
I walked to my car in the parking garage and I cried. I sobbed, actually. I was 26 years old, and now having to undergo my second open-heart surgery. It was far scarier this time because I had someone who depends on me to come home to. Over the next year, I went for more testing and monitoring, watching for when the time was right. I was given the same surgery options as before, minus the repair. My surgeon felt a repair was not an option again this time. I chose the mechanical valve, as I had decided I did not want a third surgery as far as I could prevent it.
On September 10, 2020, I had my second open heart surgery at 27 years old and received a mechanical aortic valve. The day before, I recorded a video for my daughter, to let her know she was the greatest thing to ever happen to me and I loved her more than life itself, in case I didn’t make it home. Recording that video was so hard because I knew the gravity of the situation. I could feel it suffocating me.

I woke up from surgery again in the Cardiac ICU and felt a wave of relief rush over me. I made it, again, and I was going to make it home to see my daughter. At that moment, the world felt okay again. Due to covid-19, I was only allowed to have two visitors for the entire duration of my hospital stay and no children were allowed. I video chatted with my girl every day for 5 days until I was able to come home. And when I walked in the door and saw her sweet face, I was overcome with emotion. I bawled. I was so grateful.

I completed 12 weeks of cardiac rehab and since have joined the gym to ensure I am taking the best care of myself I possibly can. Not only for myself, but for my friends and family, too. My entire mindset and outlook on life have changed so drastically in the last 6 years. I’ve learned life is so fragile, and there is no time to spend even a day of it unhappy. I never thought I’d have to have my heart stopped and restarted twice to make me appreciate life, but I did. I am on life #3, and every day I wake up grateful to get to celebrate it with the ones who make it worth living.”

This story was submitted to Love What Matters by Megan Cauley from Champaign County, Ohio. You can follow their journey on Instagram and their blog. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribeto our free email newsletter for our best stories, and YouTubefor our best videos.
Read more touching stories like this here:
Do you know someone who could benefit from this story? Please SHARE on Facebook or Twitter