Disclaimer: This story includes mentions of suicidal ideation that may be triggering to some.
“‘Some people are dealt some of the toughest hands of cards life has to offer, and, looking at your history, it looks like you’re definitely one of those people. But I have to say, you are pretty strong.’
A nurse named ‘Jim’ told me this in the emergency room on Valentine’s Day weekend in 2017, when I was back, yet again, for another exciting episode of ‘What’s Killing My Body Today?’ When he said this to me, I absolutely lost it. The tears came down, the emotions overflowed, and I couldn’t describe how deeply the statement he made resonated with me.
I’ll never forget what he said, his name, or the kindness he showed to me on what was supposed to be a romantic weekend. It was in the middle of a particularly rough spell in the grand scheme of my exceptionally complicated illness, but in that present moment, all I needed was for someone to acknowledge the hell I was going through and to tell me I was strong enough to make it to the other side.
Because what I have been dealt is one horrific hand of cards, but somehow I’ve managed to keep playing every single one.

I have never known what it was like to be ‘not sick’ (mentally or physically), but I can definitely divide the periods of my life into the ‘more healthy’ and ‘dying’ days, and damn did the ‘more healthy’ days feel good. My overwhelming diagnoses are interstitial cystitis (bladder pain syndrome), gastroparesis (paralysis of the stomach muscles), and colonic inertia (the colon is unable to move stool through the digestive tract), the latter of which resulted in me losing my colon and being given an ileostomy bag. While I was born with the last two, I was given the first after something went wrong during a routine endometrial ablation and my doctor permanently damaged my bladder and ruptured my uterus, causing a hysterectomy. Talk about bad luck.
While it seems like I like to play the game of ‘how many organs can my body live without?’ with a total of twenty-two lifetime surgeries as of 7/12/2021 (many resulting in partial or total organ removal), the reality is I would do anything to change my given situation. I would love to develop a time machine, go back to when I felt better, and appreciate every moment more, but I can’t. So, I’m left with memories and the will to fight every single day to survive in a body that won’t quite die, but won’t quite survive either as is the case for many of us with chronic illnesses.
Every year seems to be a bit more difficult: 2015 – total abdominal colectomy, 1-month hospital stay. I fight like hell to recover from this one, returning back to the strong, confident bodybuilder and law enforcement officer I was prior to the whole fiasco. 2016 – I get sicker and have to switch occupations as a result, giving up my dream of climbing the law enforcement ladder. 2017 – Ileostomy Bag Placement: what is meant to be a simple, routine surgery results in a near 3-month hospital stay, an additional surgery, and my body becoming completely dependent on opiates, having to complete the hardest withdrawal of my life. Thank God I learned so much from supervising former drug addicts in my former occupation, right? I had no idea at the time how important working with addicts would become later in my life.
Suicide is another big theme this year. 2018 – I have a surprise pregnancy, which is an absolute nightmare. I have two emergency abdominal surgeries to keep my baby alive. 2020 – God, 2020. That botched surgery occurs, where everyone thinks I’m a drug seeker and faking my pain when it turns out my insides were rotting the entire time. I spend 4 months contemplating suicide, and I honestly can’t believe I’m still here today. 2021…
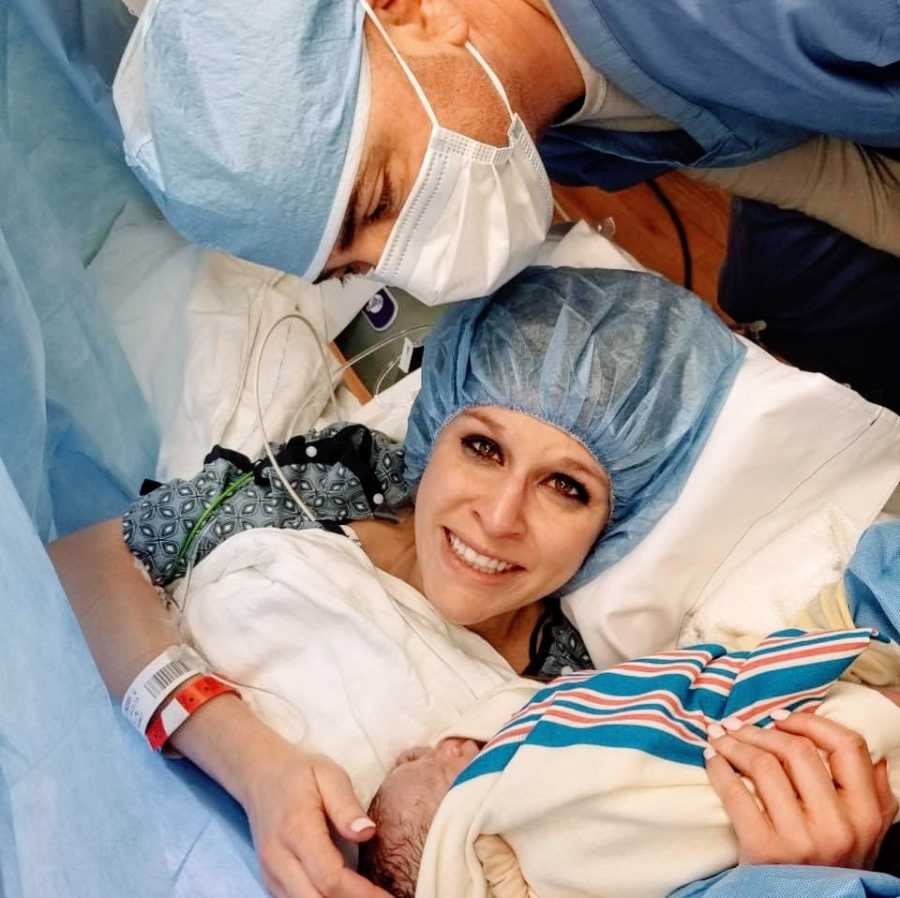
Ahh, what do I say about 2021?
It began as the year of hope. I closed out 2020 arguably at the healthiest (and happiest) I had been in four years. For the first time since my colectomy, my ileostomy placement, my hysterectomy, and my interstitial cystitis diagnosis, I felt a weird feeling—hope. I felt I could finally do it all; I’d be able to manage my condition, the pain would be able to be held at bay, and this period of remission I was feeling would last. I could finally be a wife, a mother, a friend—all of these roles I wanted to fulfill would be able to be achieved.

There was truly nothing in the world that could have ever been more wrong than those feelings and goals.
Shortly after the year began, my interstitial cystitis reared its ugly head again, and I had to repeat the hydrodistention surgery. Although I felt down about that, it would be the easiest part; I had no idea what would begin to happen as I was recovering from this.
I began noticing food was impossibly difficult to consume as I recovered from my bladder surgery. I simply couldn’t eat; any time any solid, or liquid for that matter, entered my body, a paralyzing, torturous pain akin to someone stabbing a knife in the middle of my abdomen would occur to the point where I could not eat food to sustain myself. Shortly after it began, the affliction became persistent, regardless of whether or not I was attempting to eat, and that’s when I knew it was time to get it addressed.
It may seem odd I waited so dreadfully long to get my issues seen about by healthcare professionals. ‘Why would you not simply run to an emergency room at the first sign of trouble?’ one may ask. The answer is an easy one—I have long been discriminated against, not been taken seriously, and been ignored as a woman. I have severe anxiety and post-traumatic stress disorder when it comes to being treated by an emergency room, and I always wait until the last possible second to go. If I thought I suffered from being unheard before, I had no idea what would be waiting for me this year.
While I eventually caved and went to an emergency room, I was chastised by the nurse when I told her information relating directly to my diagnosis, and eventually told I couldn’t be helped by that location. I then went to another emergency room at one of the most ‘prestigious’ hospitals in Georgia, the location where I had a surgeon who was in charge of my gastrointestinal care, where I was horrifically ignored. I was told my pain ‘wasn’t serious,’ ‘didn’t matter,’ that ‘other people are in pain, and you are wasting a bed,’ along with, ‘You’re putting yourself at risk for COVID by being here. You don’t want COVID, do you?’ and finally, ‘You’re not an emergency.’ I wish I was kidding.
After two weeks of literally being on the verge of death, it was discovered my intestine had, quite literally, turned itself in a knot. But I’m not an emergency, right?
Despite what that emergency room doctor stated, I did have emergency surgery to repair this problem.
On the road to recovery, I was feeling good again. I could start living life. Three short weeks later, I landed back where I began, and it was discovered that—you guessed it—my intestine had decided to curl back in another knot. My colorectal surgeon, a man I have dubbed my personal Jesus, having saved two lives at this point with my son’s as well, suited up to operate on me once more. ‘Alright,’ I thought, ‘I can do this.’ It’s just another setback, but we can get back to normal at this point.

Do I need to say once more I was wrong?
I thought all that was ahead of me was a simple bladder surgery on June 2. I repeat these every 2-3 months for my interstitial cystitis, as this helps to protect my bladder from the pain. I complete them, no problem. On June 3, I had an ER visit because my stomach had shut down. I tell next to no one because I’m embarrassed as hell. How many times do I have to inform people, ‘Yep, I’m in the hospital again.’ It’s just humiliating at a certain point. We assume my stomach shut down due to the anesthesia from my bladder surgery—cool; I don’t get better.
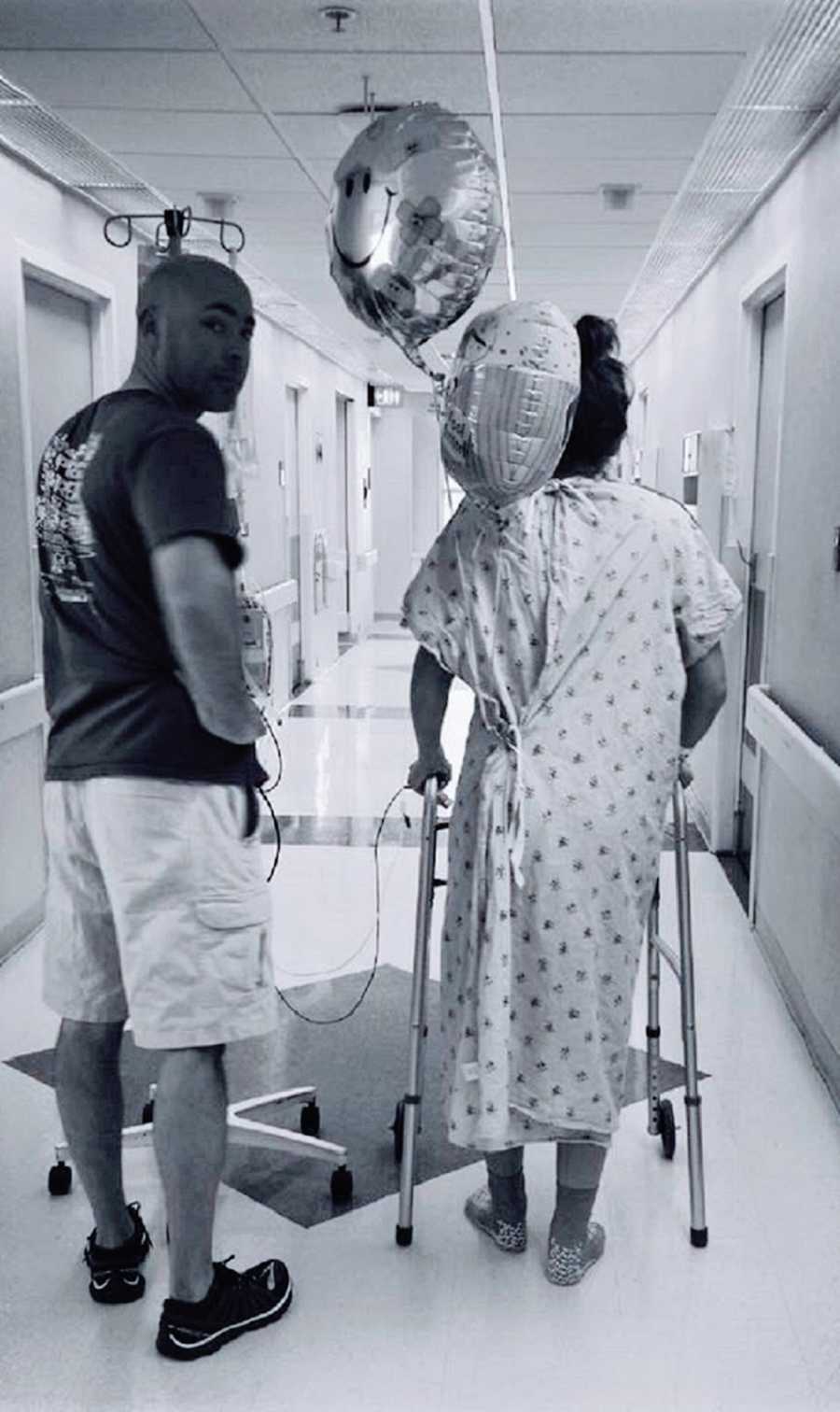
On June 8, my husband is out of town, and I am on the struggle bus. My dad, my best friend in the entire world, is up to assist me. Before I say anything next, let me say I was always okay with having an ostomy bag. Yeah, I struggle with confidence issues because of it from time to time, but pre-surgery and post-surgery, no part of me was not okay with not having the bag. I understand this is a battle for many, and I’m thankful I did not have to go through the mental gymnastics of grappling with a sh*t bag for the rest of my life.
No part of me ever thought I’d get a G/J (gastro-jejunal) tube, and furthermore, if I had to get one, no part of me was okay with it. That’s where I draw the line, that’s where the confidence wears off.
As we reported together to my colorectal surgeon’s office on June 8 for my emergency appointment, I barely listened as he told me to report to the emergency room immediately and was casually told it was time for G/J tube; there was no other option. ‘Say what?’ I thought. He told me, but I swear to God, the words didn’t sink in.
We went home to get my hospital bag I had packed for a short three-day stay (I have this ready to go at this point), I took a shower (y’all don’t know how precious these are without an IV), and we texted all those who needed to know. ‘Yeah, that’s what he says,’ I told my mom, my husband, my mother-in-law; but I swear to you, I didn’t believe it. I thought I’d get admitted, and they’d decide to do something else.
Due to COVID precautions and ERs being the way they are, I waited for four and a half hours alone in the St. Mary’s Waiting Room in a pain-wasted delirium. By the time they took me back, I can’t even tell you what was going on or who my doctor was, which I always remember. I just recall hearing the sentence at some point again, ‘Yep, we were told you’ll be getting the G/J tube.’
My dad, loyal as they come, waited with me until 11 p.m. when I finally received a room. The next day, they said I would not be totally put under for the procedure but would be given a high dose of pain medicine and twilight, which wouldn’t allow me to remember or feel anything. I told them what a high tolerance I have for both as a chronic illness patient. They laugh me off and say trust me, you won’t feel a thing.

I woke up multiple times during the surgery and felt it all. Trust me, it felt maddeningly, horrifically, awful. When we were done, the guy said he never had anyone wake up like that. I warned him, but I digress…
They hook me up to a Dilaudid pain pump, my drug of choice and typically the only thing that works for me. I will state once again; I am fine taking this drug for a short period of time—after extended periods, I am not. However, when you are in severe pain like myself and many chronic illness patients are, you absolutely need this drug to survive, and often, it does not cover it all. You’ll still want to sit there and die because of how much you simply just hurt. I didn’t look at my stomach for quite some time because I just could not. I’ve got a crap sack there; fine—I don’t want to see the tube. I’m still not mentally ready for the tube.
For two days, it all seems fine, until day three arrives and everything shuts off. My tube is clogged, and they can’t get it to work. My surgeon says he’s done tons of these in four years and this has only happened to me—he has no idea what’s going on. If it’s going to happen to anybody, it’s me right?
Meanwhile, those who operated on my stomach (which is still sitting in my pelvis, where it shouldn’t be), tell my surgeon unlike typical gastroparesis patients, who have some stomach motility, I have none. My muscles are 100% dead, rendering my stomach useless. Guess what that means? It’s finally time to address and either partially or totally remove my stomach; but I can’t even begin to comprehend this yet.
I am just about as depressed as I’ve ever been. It’s been a hell of year, I’m sick of being in the hospital away from my son, I’ve got a new tube sticking out of my stomach that doesn’t work, and you’re telling me you now have to remove my stomach and my body is now fully addicted to opiates after being on IV opiates for two weeks?
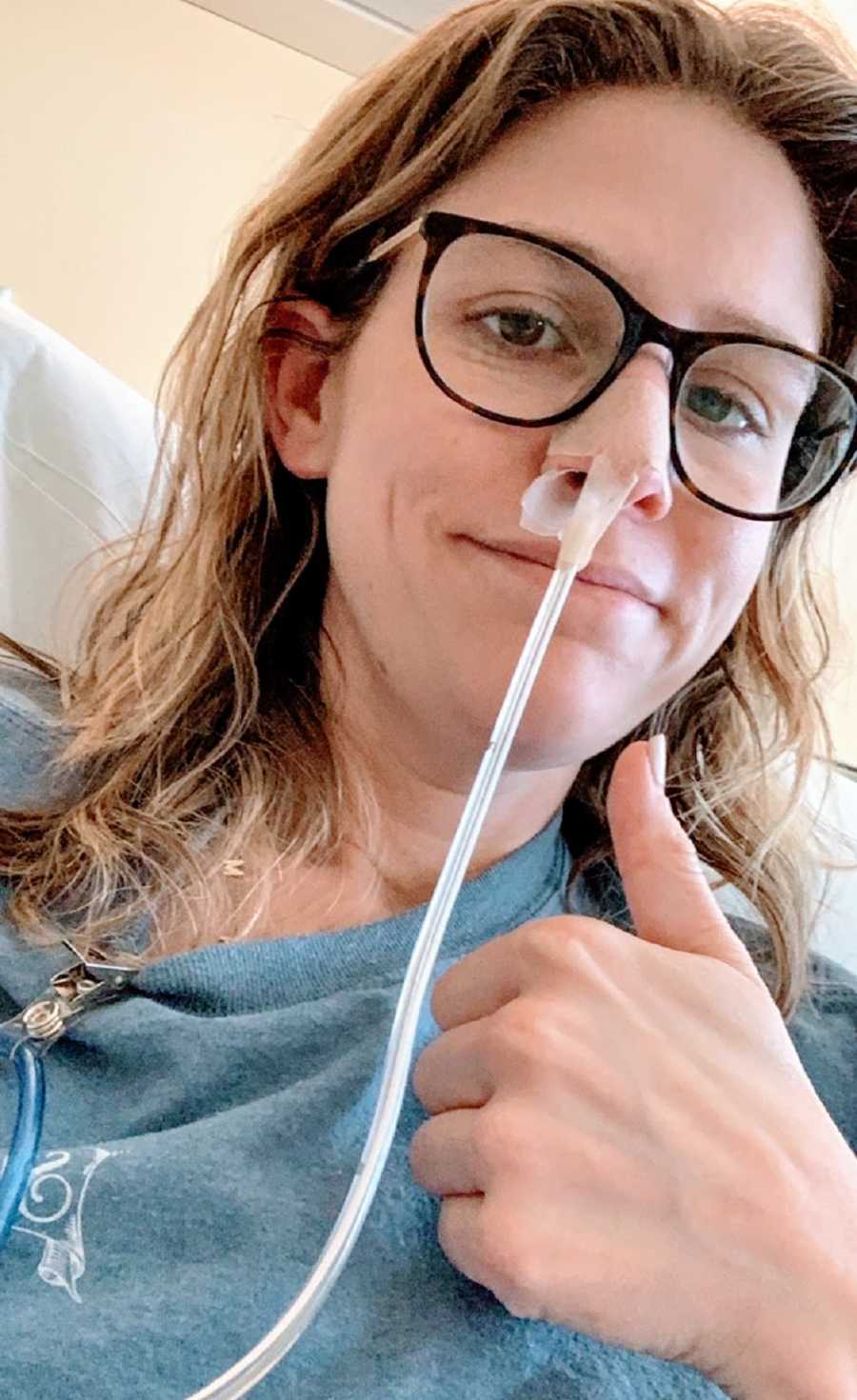
But, it’s time for me to turn 31. Let me apologize in advance for not responding to any happy birthday messages, posts, or texts. It will truly go down as one of the worst days of my life. Reading through medical records now, I just learned that they had to sedate me. It was a bad day.
I started out thinking, ‘Let’s just get it over with.’ I made a medical decision very few know about but have wanted to do for years; it was not a mental breakdown or something I have not prepared for. But yes, you’re right—I am hella f***ing depressed—and yes, you’re right—I’ve got to detox despite being in some of the worst pain of my life. I will say, I had a FANTASTIC nurse looking out for me this day, and I owe a debt of gratitude for her being there to help me through an absolute mental crisis.
We had the wonderful nurse, my dad, the Chaplin, a social worker, come in and do a mental health intervention on me; yes, it was needed, but yes, it was one of the heaviest days of my life. I will say, ‘I am okay with dying. I do not mind leaving this earth. I have lived a lifetime of pain.’ But I do not struggle with suicide anymore, and I can confidently tell you I never will.
Having my son means I will stay alive and I will continue to stay alive as long as I am medically able to do so. As the 1975, say, ‘Your death, it won’t happen to you; it happens to your family and your friends.’ That does not mean things are not okay for me and other people who struggle with depression without suicidal plans, it doesn’t mean things are perfect just because we don’t want to off ourselves. We still need help, we still need support, we still need light in our dark corners of the world.

During this time, I’m also dealing with withdrawals from opiates. This is my third official detox following surgery. I’m someone who relies on chronic pain medication/opiates outside of the hospital, and I take this responsibly. I don’t crave the drug or the high if I take too many (I also don’t like my head being messed with). I know I need this for pain, so I use them the way they’re meant to be taken. However, when you’re hooked up to an IV pumping these into your veins for two weeks straight, your body will get addicted. I have SUCH RESPECT for addicts who are able to handle detox, withdrawals, and not picking up a drug again. IT IS HARD. Your body experiences the absolute worst; fevers, chills, ants in your veins, shakes, I mean you name it. It’s not the high you end up craving, as many have said, and what I learned supervising addicts, it’s the damn withdrawal people can’t get through.
So yeah, that was fun, and again, great birthday. Can I please re-do 31? Like, really.
After almost 3 weeks of being separated from my family, I was finally released on TPN (this feeds me through a PICC line through my heart) to hold me over through my G/J tube replacement surgery.
Here is my conundrum: I am actually very happy.

I hit 30 and I was like, hey, I kinda like myself and life. I don’t know what it was, but it just happened. I am still unfiltered, swear all the time (I had an ex once say it was the most unattractive thing to hear a woman curse, and I’m sorry I just disagree—I chose my best friend BECAUSE she cursed, and there’s just nothing like the ‘f” word), laugh like crazy, I’m goofy, and PLEASE don’t get me started on music. I’m so thankful for the people who are now in my life and for the amazing things I do have. And damn, the good times are REALLY good. I love having fun and just being an idiot.

Here’s the flip side—the bad times are REALLY bad.
So what do you choose? How do you keep going this way? How do you cope with a lifetime of pain amidst all of the fleeting moments of happiness? It’s a hard answer, and I don’t have it yet. And please don’t tell me to pray about it, because I am still not talking with the man upstairs. I so appreciate other people praying for me, I truly do; but it is going to be a long time before I can for myself, and unless you have experienced the level of suffering myself and other chronic illness patients have faced, I just don’t know how to explain it any better.
To quote a recent book I read, Bath Haus by PJ Vernon, ‘There is no worse pain than deciding to live.’
So here’s where I’ll end. I’m choosing to live. I’m choosing to survive. I’m choosing to fight. It’s not an easy decision, and it’s not one I have taken lightly, haven’t cried over, or haven’t talked out through hours of therapy (mental health matters, y’all). I’ve got a long road ahead. I’m still facing that partial/total stomach removal. I’m still facing a lifetime of pain, hospital stays, and operations. But I’m also facing those moments when my son cuddles up in my lap, music loud, windows down in the car with my friends, family game nights spent laughing so hard I’m crying.
The trade-off can be worth it. I’ll just need a little help while I’m still here.”

This story was submitted to Love What Matters by Lindsay Worsham Dickerson. You can follow her journey on her blog and Instagram. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this here:
Provide hope for someone struggling. SHARE this story on Facebook and Instagram to let them know a community of support is available.

