“We started trying for baby number two in the fall of 2019, and within a month, I was pregnant. It was thrilling! It had happened so quickly and easily. Everything was right in the world. But as I approached 6 weeks along, I started bleeding heavy red blood and my only thought was, ‘I’m losing my baby.’ I knew going to the ER would be pointless, and it was better to wait until the morning when my OB’s office opened. They got me into the office right away and my doctor was unsure there would be a heartbeat if he did an ultrasound. But there was a heartbeat. And it was a strong one.
After being prescribed medication to help ease the bleeding, which eventually did stop, the pregnancy went on as normal: morning sickness, swaying appetite, weight gain, you name it. At 15 weeks, we found out it was a girl. This was such a happy day. I never imagined being a girl mom.

Then COVID-19 hit and things got really crazy in the world. Thankfully my husband was still allowed to attend doctors’ appointments and we went in for our scheduled 18-week anatomy scan. Three cysts were found on the baby’s brain. My doctor wasn’t too concerned and stated most cysts resolved at birth, but just to be sure, he offered a blood test I could take to see what my chances were for the baby to have a genetic defect. Apparently, cysts on the brain were a small marker for this kind of thing.
This was a hard pill to swallow but I did the test and the odds were very low. We continued onward, feeling reassured everything would be okay. A few weeks later, I had another ultrasound. We were happy to hear the cysts were gone but received some strange news they were having trouble getting a good view of the baby’s heart. The baby was also measuring on the smaller side. I thought, ‘Okay, well, my son was really small too, and he turned out just fine. I just make small babies is all.’ They didn’t elaborate on it much further but sent us to a high-risk pregnancy center 2 days later.

This is when things got really, really heavy. At this point, I was 28 weeks along, not knowing if there was something wrong with my baby or if it was all just a weird dream I would wake up from soon. The initial ultrasound with the sonographer was painfully long. Long and quiet. She didn’t say a word and neither did I nor my husband. A pin could’ve dropped, and we would’ve heard it. I didn’t know much about ultrasounds, and I couldn’t understand why she was spending so much time looking at the baby’s brain and the placenta. Was there something wrong with them?
Finally, the sonographer told us to wait for the doctor and she left the room. I remember sliding off the raised bed and sitting next to my husband. We gripped hands and didn’t say a word to each other. We knew something wasn’t right. The doctor came in and she had a strange look on her face. A bearer of bad news, as they say. It was obvious what was about to come out of her mouth would change our lives forever.
The issues she began listing off seemed endless. ‘Yes, your baby has a heart defect – extreme levocardia and a small hole, but a cardiologist could tell you more. Yes, your baby is growing asymmetrical. This could be identified as IUGR from placental insufficiency. When your baby relaxes inside the womb, the placental artery stiffens, and blood flow has a more difficult time pumping through. Parts of her body are measuring 2 to 4 weeks behind. Your amniotic fluid count is also particularly high, which is why I suspect a genetic defect.’

We also spoke to a genetic counselor who learned all about our family’s medical history to see if there were any links tying to a genetic defect. There were none. They drew my blood, and the results of what could be going on would arrive within a few days. We went home feeling very overwhelmed and in a daze. I was in denial most of the weekend, just trying to not think too much into it. I felt like the baby I had imagined inside of me was no longer there, and the baby I was actually carrying was someone far different. I think in some ways, I temporarily lost a connection to her. It was so strange to me I went through over half my pregnancy believing my baby was just fine.
It was a Monday night when we received the dreaded phone call, the moment that will stick with me for the rest of my life. The geneticist wanted to alert us right away as soon as she got the results. It was almost 8 o’clock at night. My husband and I were standing in our bedroom on speakerphone when she told us they found partial fragments of an extra 18th chromosome. This was linked to a genetic defect called Trisomy 18 or Edward’s Syndrome.

This was a very life-changing moment for us. Within minutes after the phone call, the geneticist sent us pamphlets and fliers over email with all kinds of information on Trisomy 18. The statistics for survival rates were horrifying, and something no parent would ever want to see. I had no words after the phone call. I didn’t say much because the shock I felt was rolling off of me in heavy waves and rendering me speechless. How could this be happening? Was this all a dream… a nightmare? I wasn’t sure.
I sat in the backyard at dusk and watched my husband water the plants. We didn’t say much to each other. We were simply trying to process it. Would our baby survive? How long would she live?

I finally did cry at this point, but I really didn’t know what I was crying for. I still had so many questions. I just kept rubbing my belly and feeling her kicks. How could an active baby such as she be ‘damaged?’ There were still so many unknowns. In particular, PARTIAL Trisomy 18 is one of the rarest conditions. Rarer than Trisomy 18 alone. There really wasn’t much information online regarding partial Trisomy 18. It was strange and also a little unnerving. It made the questions we had double for us. From what we could research, partial Trisomy 18 could, in some cases, have milder symptoms than full Trisomy 18. That was the only bit of hope we could hold onto.
I didn’t anticipate the following 8 weeks to be as hard as they were. From the moment we received Maggie’s diagnosis, I was being monitored twice a week with ultrasounds and fetal monitoring. They were consistently checking her growth, blood flow in the placental arteries, my amniotic fluid count, and contractions.

Within 2 weeks later I went into preterm labor. Around this time, I had also switched doctors after finding a Trisomy friendly one with an amazing reputation. I was so blessed to locate Dr. Wilkes. He vowed to do everything possible to bring my baby into this world alive. I visited the hospital three separate times that month, and at one time my contractions were confirmed to be one minute apart, but I had not dilated at all. I was barely 32 weeks. The future was so uncertain at this point.
After getting through those times, my amniotic fluid count was steadily rising. Anything past 25 cm is considered ‘polyhydramnios.’ My fluid count at one point had been 38 cm. I felt like I was carrying a gigantic water bag. It did wonders to my back. I delivered Maggie at 36+6 weeks. I had gone in for an appointment that Monday and when I found out they weren’t going to do an ultrasound, I demanded one be done. We had already seen an increase in restricted blood flow in the placental arteries, so I was very worried about letting it go unmonitored. After some convincing, they did an ultrasound and my doctor called me an hour after the appointment to ask if I was ready to deliver the next day. At this point, keeping Maggie inside was too dangerous and we didn’t want to risk placental failure and her dying inside of me.
Deliver day was all kinds of rough. I was delivering in an unfamiliar hospital, but it was the hospital with the most advanced NICU care, especially for babies with heart defects. It was a planned c-section and going into surgery was like walking in the dark. We were putting everything into God’s hands.
One thing I couldn’t help but think during this time is I could’ve done things differently. I could’ve easily chosen a different route for her, one that might not ensure her survival so much. But that wasn’t the path I chose. There was a reason I chose full intervention, and that was because I could feel Maggie’s strength. I felt her spirit, her love, her tiny little body having night parties, and long naps during the day. She was a strong baby, and something told me she wanted to live. I did everything possible to give her that chance.
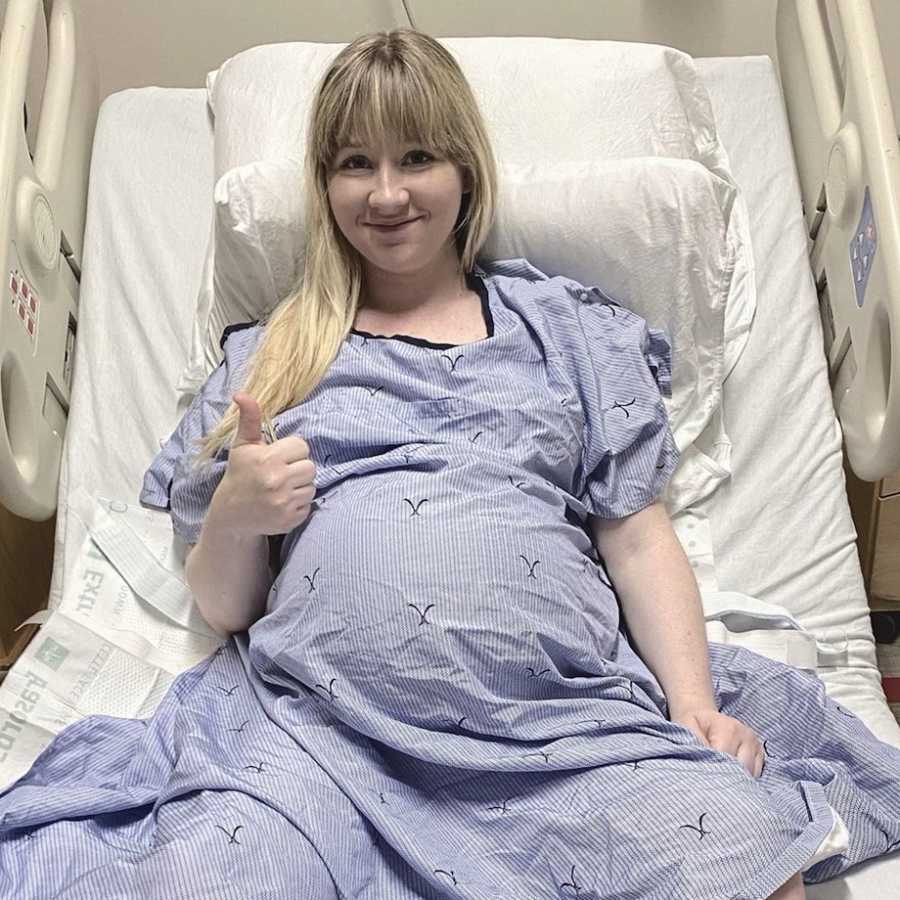
The entire surgery from start to finish took about one hour. I felt no pain or temperature, but I could feel every pull and tug on my stomach, which was one of the strangest sensations. While my husband sat behind my head and my view was entirely blocked by a raised sheet, it was mere minutes before Maggie was pulled out. When I didn’t hear her immediate cry, which is normally the ‘good’ sound you look for, I lost it emotionally. At this point, I was so terrified for her well-being it was causing a rapid spike in my heart rate and I felt like I could no longer breathe. Oxygen was given to me and all I could do was wait and try to calm myself down with deep breaths.
Finally, after what felt like an eternity, I heard a tiny little cry – once, twice – from across the room. I lost it again but in a good way. My husband was brought over to see her and the neonatologist came over to me to briefly inform me of her condition. She appeared to be breathing super well and only needed a little help with oxygen but was otherwise stable and ready to head to the NICU floor. This is when I was able to see her for the first time as the nurses brought her over to me. I was immediately SHOCKED by how tiny she was. Only 3 pounds, 10 ounces. Her entire head fit snug inside the nurse’s hand, she had an oxygen cannula taped under her tiny nose, and her eyes were closed.

I started speaking to her and calling her by name and her eyes began to flutter. I can only hope she was able to recognize her mommy’s voice. I couldn’t believe she was finally here. She was taken away after but a small moment while my husband followed, and I was left to wait for them to stitch me up. When it was all over, I received the kindest farewell from a few nurses reassuring me Maggie would be well taken care of and my doctor came to thank me for trusting him to deliver our special baby. He told me we both know who’s in charge now and he would say a prayer for special Maggie. This really warmed my heart.


The next 3 months would go on to be incredibly trying, and full of ups and downs. Maggie received her first surgery at just 22 hours old, and she went on to have four more. After her initial release from the NICU, she ended up back in the hospital another two times. But every day she fought. She’s a heart, g-tube fed, trach and vent dependent warrior who has endured time and time again, and from the brink of death, she has survived. She’s ‘Miracle Maggie’ – so we call her – and she’s here to tell her story.”

This story was submitted to Love What Matters by Charity Nelson from Las Vegas, NV. You can follow their journey on Instagram and Facebook. Be sure to subscribe to our free email newsletter for our best stories.
Read more touching stories like this:
Provide hope for someone struggling. SHARE this story on Facebook to let them know a community of support is available.

