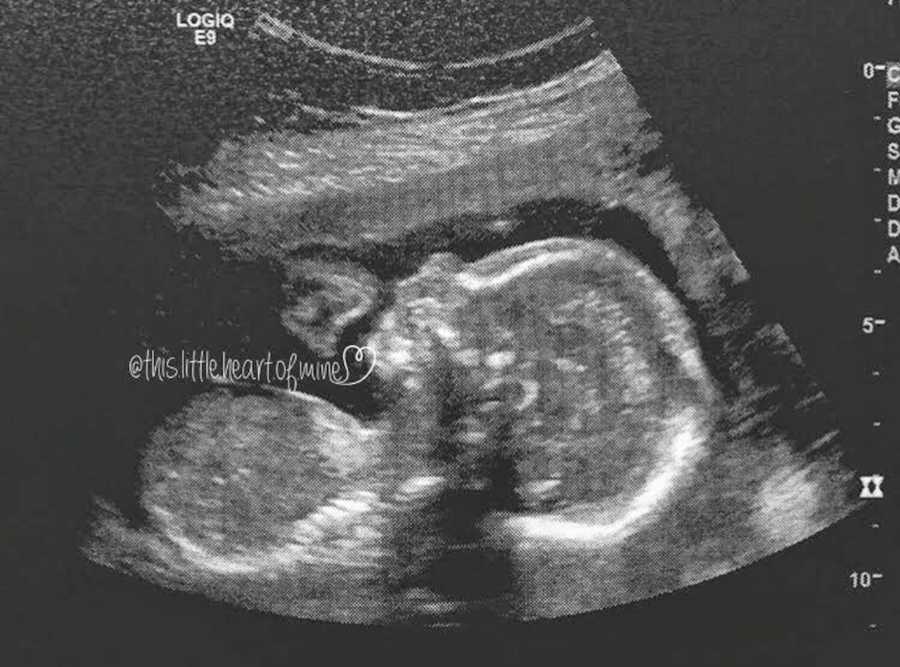
“We were in Winnipeg, headed downtown to the Health Science Centre. We parked our truck on a side street, climbed out and started walking to the hospital. It was such a strange feeling going for this ultrasound. There was no joy or excitement this time, there was no skipping. There was only a sick, empty feeling.

The hospital was grim, full of expecting couples, most of them were somber, some crying. We sat in the waiting room what seemed like hours, our baby kicking away, until finally our turn came. The tech got to work taking images while Kevin and I stared at the screen looking for anything that made sense. Blue and red colors flashed on the screen, was that good? What did it mean? It didn’t take long, and the tech was done. She looked at us and said those words, the ones that changed my identity, ‘I will tell you this, there is something wrong with your baby’s heart.’
A doctor came in, he was tall and thin. He didn’t speak as he took some of his own images. When he finished, he quietly asked us to join him in his office. Silently he began drawing on a blank piece of paper. When he was done, he turned to us, showed us his drawing, and began explaining some of what our future would look like.
It was the first time that I had ever heard of Hypoplastic Left Heart Syndrome. I was shocked. How could anyone survive with only half a functioning heart? How was that even possible? A hole in the heart, sure, but half a heart? It didn’t make sense. One thing that still resonates with us was the grim way the doctor told us, ‘We can attempt to fix it.’ He did not paint us a very promising picture.
Slowly the doctor explained to us about the three stages of surgery, the Norwood, Glenn, and Fontan. So many surgeries, and on such a young child. A wave of sickness washed over me. But the doctor was not finished yet, he continued to tell us that there was a possibility of our baby having some sort of chromosomal abnormality, he advised me to have an amniocentesis done that day. Knowing the risks of an amino I was hesitant to agree. The doctor urged us to go think about it and come back in half an hour. We slowly walked back to the truck hand in hand, and once we were safely inside, I started bawling. I was terrified. I was terrified of the needle, I was terrified it would hurt the baby, and mostly I was terrified what the results might show. But for some reason we knew we needed to do it. I wiped my tears and together we returned to the hospital.
I was frozen with fear, as the doctor and nurse were prepping for the amino with ultrasound guide, that I couldn’t even hold Kevin’s hand. It was over quickly, and once I was cleaned up, we were informed of another appointment we had to attend, two blocks away.
The Variety Heart Centre was quiet. Kevin and I sat down in the waiting room, cartoons playing on the TV. Shortly later a Pediatric cardiologist called us into a room. Walking into the room I had an overwhelming feeling that the day would never end. The cardiologist routinely asked us some questions about my pregnancy and family history, then asked me to lay down for my 4th ultrasound of the day. It was a very short ultrasound. The cardiologist excused herself and returned moments later with printouts of what a HLHS heart looked like, and what it would look like after all 3 surgeries.
She went over the pictures with detail, all the while explaining that surgeries like these are no longer performed in Winnipeg. What did that mean? She told us that we needed to go to Edmonton or Vancouver for these surgeries and recoveries, 4-6 weeks approximately. The cardiologist finished up by also telling us that our baby’s heart was not sitting on the left side of its chest, but rather was shifted to the right side. Again, I was shocked. How do things like this happen? ‘Sometimes when a baby’s heart doesn’t develop as it should, it shifts,’ she said, and that was the only explanation we got.
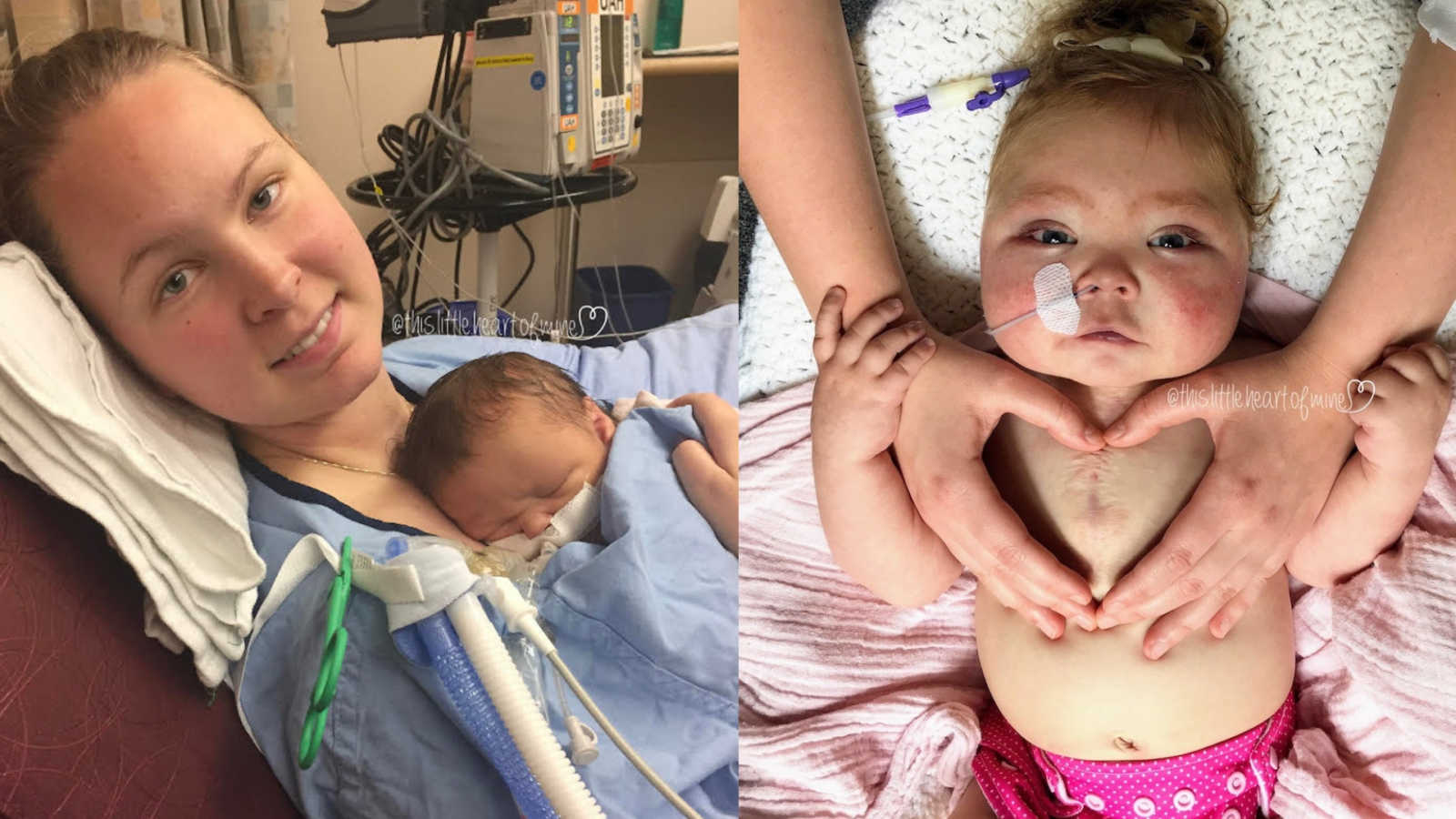
We spent the first 6 months of Ella’s life in the hospital while she tackled 2 open heart surgeries. She fought so hard and showed us so much resiliency. Twice we were sure we were going to lose her, and it was the most heartbreaking, sickening feeling we had ever experienced.

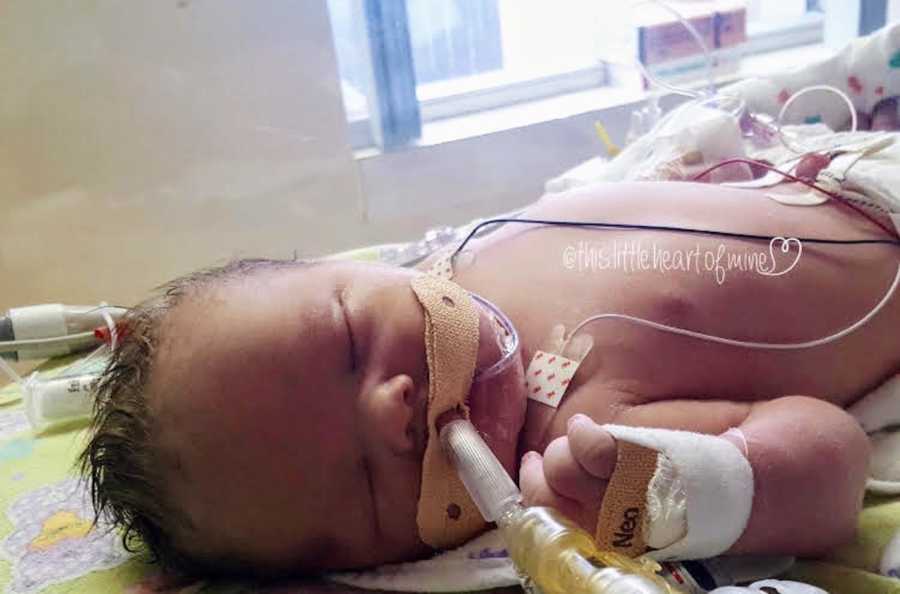
I can think of one of the surgeries that never leaves my memory. It was quite late in the evening when we were finally granted access to the unit. Walking up to Ella’s bed there were so many wire and tubes. She looked more robot than baby to me. An older nurse, with big round glasses and a fleece sweater, was working on all of Ella’s tubes and wires with steady hands. Alcohol swabs were everywhere. Everything looked so disorganized. I remember having a fleeting moment of panic wondering if this nurse was good enough to be taking care of my baby. She was very focused, almost to the point that it seemed she didn’t know what she was doing. I wish now that I knew to look at her as being diligent and see how she was being very careful to ensure Ella was as safe as possible.
We were informed by the Intensivist that Ella’s blood pressure dropped numerous times while the medical team were trying to settle her into the PCICU. Before we were able to come in and see her, they had to stabilize her. She was doing fine now, they just needed to transfer all the OR equipment to their own. A process that can take quite a long time. The nurse continued to work steadily, there seemed to be no end in sight. Kevin and I decided she should go back to the hotel and let her finish up without us being in the way. I started crying as we walked out of the unit. I hated leaving her when she wasn’t completely settled in yet, but I knew there was nothing I could do for her right then.
At around midnight I called in to check on Ella. The receptionist answered the phone and told me that Ella’s nurse was a bit busy at the moment, she placed me on hold. I thought nothing of this as the minutes ticked by, but then the Intensivist answered the call instead of my nurse. She answered by saying, ‘Hi, I was about 5 minutes away from calling you.’ my stomach dropped with those words. Never do you want to hear those words when your baby is only hours post op.
‘Ella is having a little trouble keeping her oxygen and blood pressure levels up. She may need to go on ECMO.’ (ECMO – Extracorporeal membrane oxygenation is a machine that acts as a type of life support for the heart and lungs. There is a 25-65% mortality rate for children placed on ECMO) My chest tightened at her words, I jumped up and started to pace. ‘We have been watching her and we are trying to weigh the pros and cons of going on ECMO for Ella.’ All I could think was if it’s going to help her, then do it! The Intensivist, a very outspoken woman who tells you as it is, then said, ‘It may seem like we are dragging our heals on this, but there are significant risks with being on ECMO.’ She assured me she would call me back shortly, and then she hung up.
I sank onto the couch and started crying into my hands. I relayed what the Intensivist said to me to a worried Kevin. I thought in those moments that we were going to lose our daughter, I truly believed it. It was the worst feeling I had ever felt. Minutes later the Intensivist called me back, with tears in my voice I answered my phone. Ella was in fact going to need to be placed on ECMO, she needed to give her heart a rest. Sobbing, I asked if we should come in. Our Intensivist’s answer was firm, ‘We have to close down the unit and turn it into a temporary OR for the surgeon to place her on ECMO. There is no point, you wouldn’t be able to see her anyways. Just try and get some sleep.’ I nodded even though she couldn’t see me, and just begged that they take care of Ella.
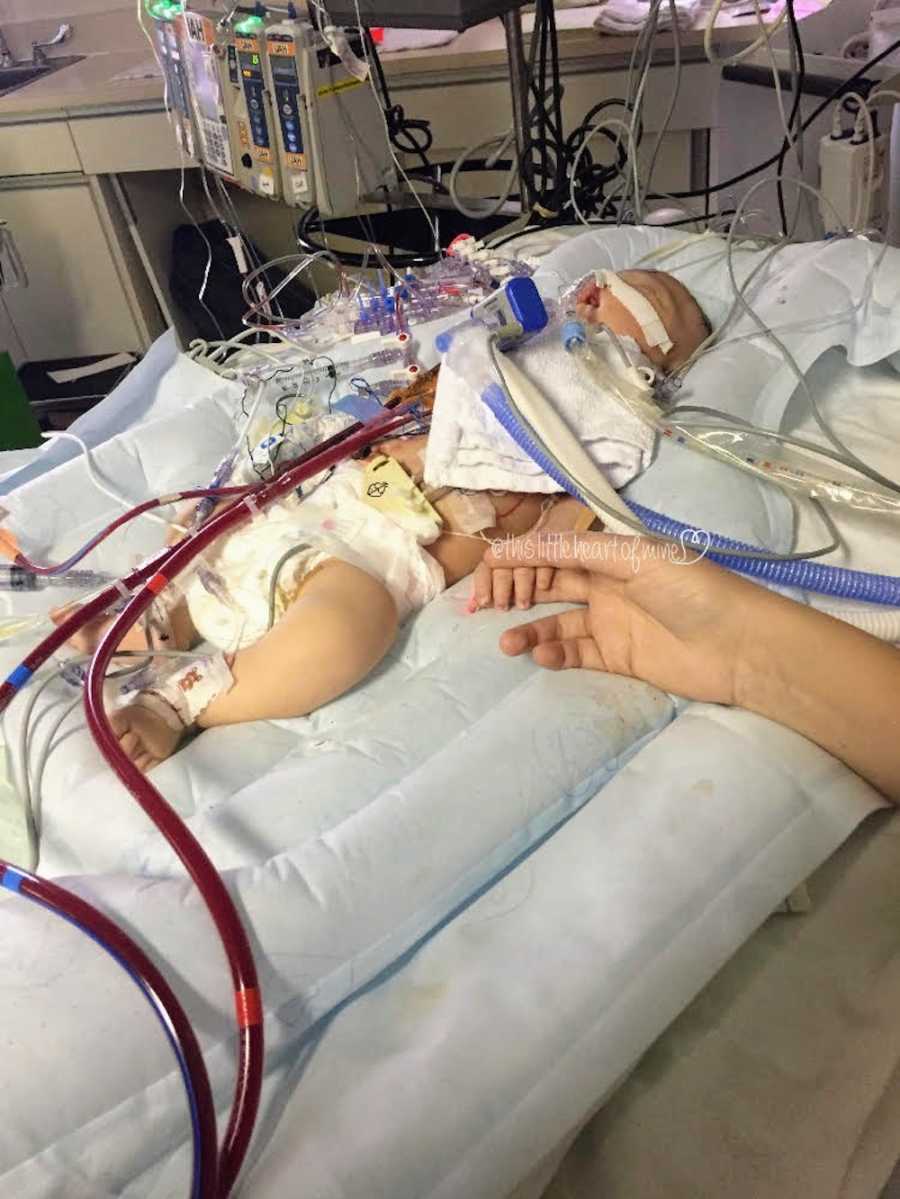
Ella was successful placed on ECMO. Kevin and I did not get any sleep, I sobbed while Kevin comforted me. That night was easily the worst night of our lives.
Ella is 16 months now, and is the biggest blessing in our lives, she has taught us so much in such a short time. We don’t know what God’s plan for Ella’s future holds, whether or not she will be able to have her 3rd stage surgery, or if we will have to look at other options for her.
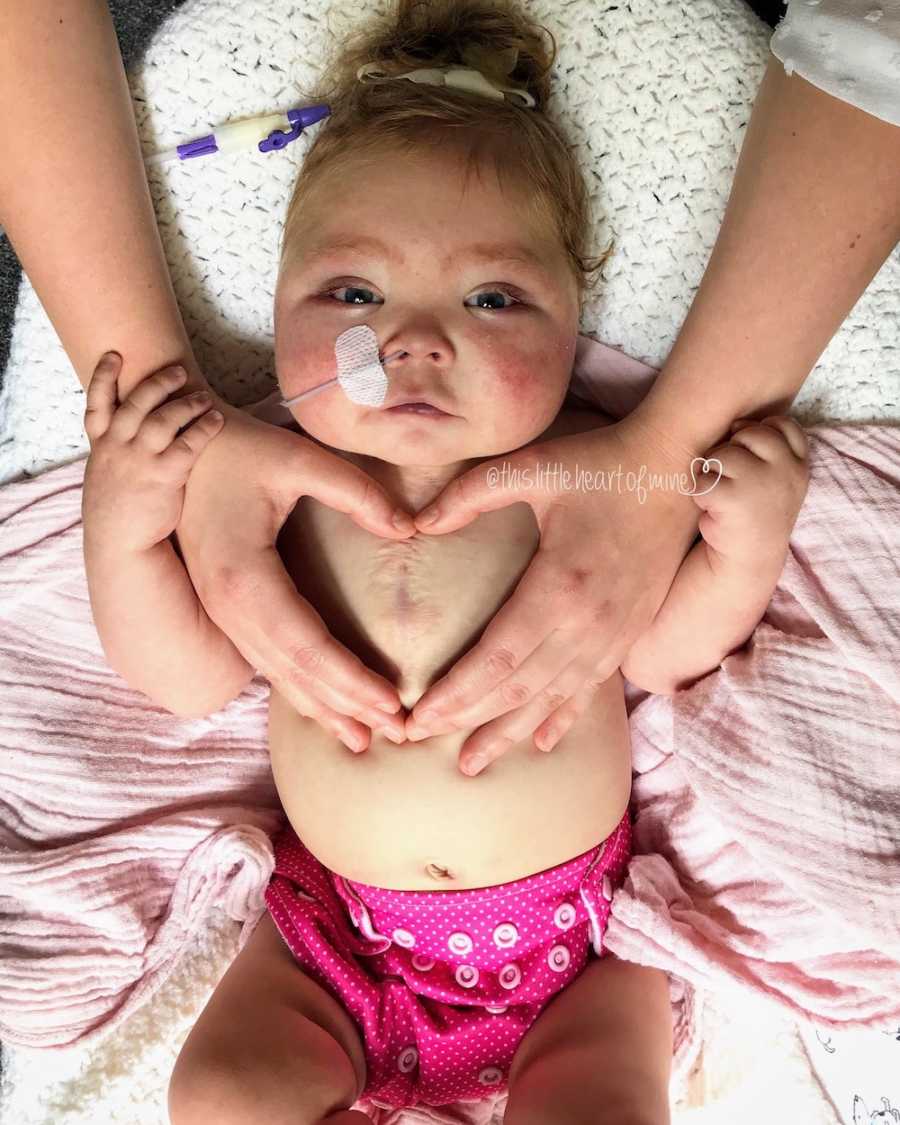
What we do know is that every day God has given us with Ella, has been a beautiful gift that we have treasured. We try not to focus too much of our time looking into Ella’s future, but to instead be in the present with her, enjoy her. My favorite thing about Ella right now is the silly faces she will give me, she will frown up at me as if to say, ‘@hat are you going on about?’, and of course I laugh because it just is so darn comical.


My laughter encourages her, and she will do it over and over again, grinning as soon as I laugh. Last evening, I spent a good half hour running around the house like a goof just to hear her fits of giggles, and she would sign ‘more, more’, every time I stopped to catch my breath. Kevin and I loved every second of it. These will be the memories that we will treasure. Quality over Quantity, the years may be short but let them be good!
We try not to focus too much of our time looking into Ella’s future, but to instead be in the present with her, enjoy her, and always count our blessings.”

This story was submitted to Love What Matters by Jaimee Waldner of Brandon, Manitoba. Follow their journey here. Submit your story here. For our best stories, subscribe to our free email newsletter.
SHARE this story on Facebook or Twitter if you know someone who may benefit from this story