“My road to becoming a mother was not an easy one. I delivered my first baby, in January of 2010. Most people would expect me to continue this article by telling some elaborate birth story with a climatic event leading up to birth of a beautiful baby boy. This was not my experience. My son, Caine, was still born at 21 weeks and 6 days. Not what you were expecting? Neither was I. A year past and I became pregnant again, with another little boy. His birth, and really his short life, are an 18-hour blur of code blues, a very confused newborn intensive care team, and my heart feeling as if it had been ripped from my chest. My son, Brandon 2nd, was born 10 weeks early with more health complications than I care to list. Unable to breathe and allergic to surfactant (a coating to help protect your lungs) I had to make a choice no parent should. The hardest part of my son’s life was letting him go. I can still remember it as if it was yesterday. Holding his tiny frail body, whispering ‘I love you’ while tears rolled off the tip of my nose. Tilting my head up and peering at the nurse through foggy eyes she said to me ‘Sometimes it helps if you tell them it’s ok to go.’ I looked down at my boy, pulled him to my cheek and whispered, ‘It’s ok baby, mommy’s here.’ With those words, he took his final breath.

The death of my son threw me into a deep depression. I developed PTSD and spent 4-5 days at a grief counselor that first year. I also began writing. It started as a letter I wrote to him on the day of his funeral service. All of the things I wish I could have told my son, all of the dreams I had for him, and what an immense impact his short life had upon mine. That following summer, me being the fertile woman that I am, again, became pregnant. On the day of Caine’s birth and death, I had a scheduled anatomy scan. For those unfamiliar with pregnancy and milestones, this is the largest ultrasound you receive when pregnant and typically when you can find out the sex of your baby to be. Nervous and excited I bounced into the ultrasound room. Spending so much time at the hospital and having the kind of losses that I had made me a very familiar face in the birthing hospital, even ultrasound techs at this point in our journey knew me on a first name basis. I went into the dimly lit ultrasound room and laid on the noisy white paper. The tech picked up his wand and slathered it with warm jelly and placed on my lower tummy. His attitude quickly changed. He seemed, uncomfortable and kept tilting his head side to side and turned to me and said, ‘I need to go get the doctor, I’ll be right back.’ After a few minutes, he shuffled in with the doctor who greeted me and said, ‘Let’s take a look at your baby!’ The tech re-gelled the probe and placed it to my belly to show the doctor what he had seen. With watery eyes she turned to me and said ‘Meagan, I’m so sorry. The baby does not have a heartbeat. I’ll give you a few minutes and then we can talk.’ Scream. That’s all I could do. At the top of my lungs and with no remorse to the fact that I was in a very busy maternal fetal medicine clinic I screamed the words ‘No! Why?! Not my baby!’ I’m sure the other pregnant woman in the waiting room though I was being tortured in there. After 20 minutes I opened the door and walked into a completely silent waiting room and not because it was empty but because everyone was staring at me somberly. My labor was induced, and I gave birth to my first daughter, Lotus.
Now here’s where our journey really got interesting. You can imagine, with Lotus being my third loss the grief monster had a tight hold on me. I questioned everything, including whether or not I was really meant to be a mom. That despite how bad I wanted to have children maybe that just wasn’t part of the plan? Just six weeks after Lotus’s death I was pregnant again. At first, no one believed me and even my OB/GYN warned me that sometimes when women have gone through the kind of trauma that I have they experience phantom pregnancies. My first ultrasound was very disappointing, while the doctor was able to measure my uterus and it appeared, I was in fact pregnant, they couldn’t visualize the baby and he believed I had already lost the pregnancy. 3 weeks. That was the length of time I had to wait before I could have another scan to see if there was a baby inside of me. This was my first taste of having hope in the face of immense darkness. I am happy to say that there was a baby inside. That when I went in for that ultrasound my nursing assistant and I cried together as we gawked over the little bean and strong heartbeat.
My pregnancy with Madeline was very nerve wrecking. The entire time I felt like something was wrong. I chalked these up to what I had gone through before and tried my best to subside the feelings, but they just wouldn’t go away. Around 21 weeks I was going into triage on a weekly basis complaining that something was just not right. At 25 weeks and 5 days, I had a total meltdown and again felt as though something, was wrong so I headed back into triage. The nurse at the desk checking woman in saw me and let out a big sigh after a decent eye roll. ‘Back again?’ she said. The triage nurse quickly brought me into a room. She seemed rather frustrated and distant and with good reason since I had been coming in so often. With a very straight face the nurse turned to me and said ‘Ok, so we are going to go ahead and do an ultrasound to make sure the baby is ok but you should know, your insurance isn’t going to want to keep covering things if nothing is wrong.’ My mucus plug had come out and I was 0% effaced. The nurse apologized profusely to me and with a bewildered look said, ‘How did you know?’ With confidence I looked her straight in the face and said ‘I don’t know. I guess. I just knew something was wrong with the baby.’ Now, I will say that I am rather empathic, and my entire life have gotten these feelings whether about something good or something bad.

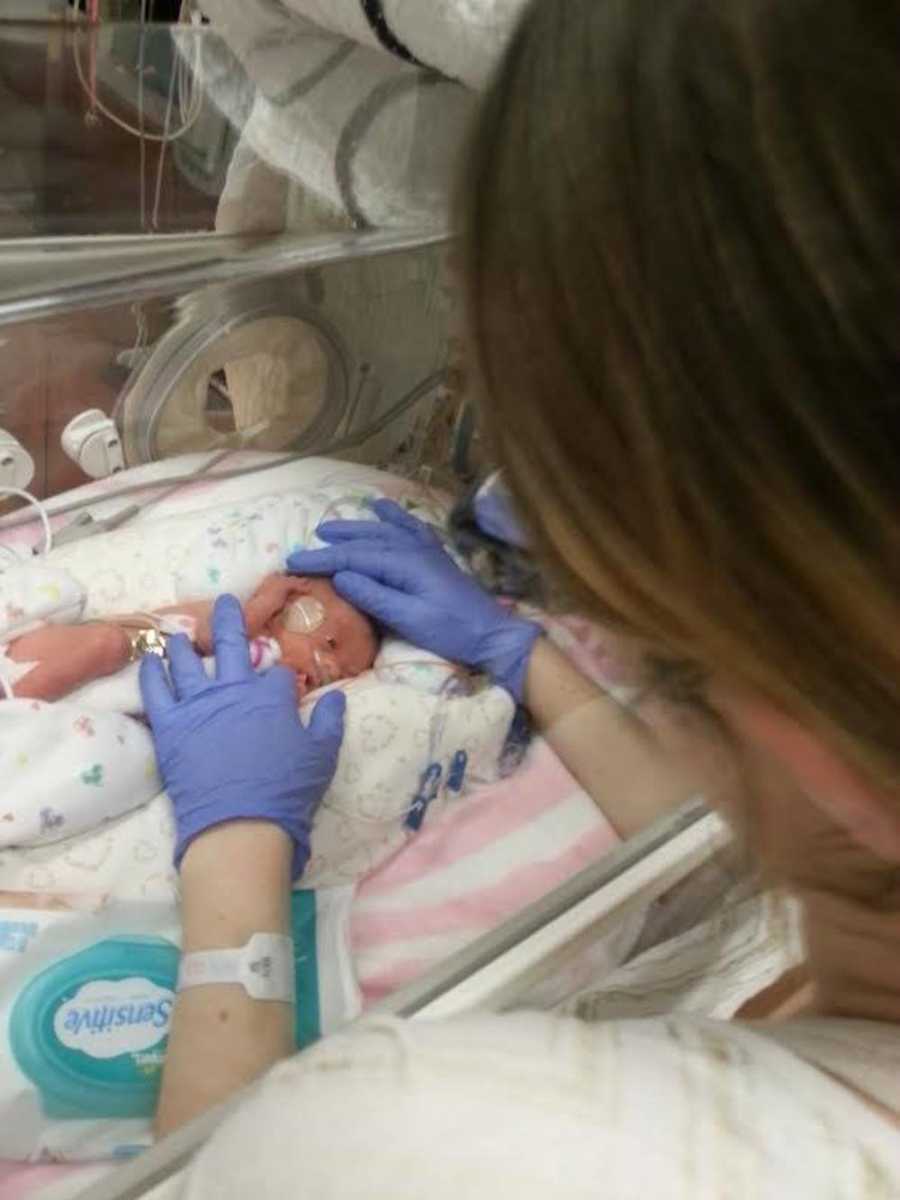
I spent 3 weeks in the hospital on bed rest and on Halloween night, my cervix began dilating and my labor began. After doses of magnesium sulfate to try and slow things down, steroid shots to help her lungs, and a transfer to the labor and delivery floor by that evening we had finally slowed things down. The next morning, I felt amazing, well as amazing as you can feel at 7 months pregnant, on bedrest, and having no food for over a day. The day continued and around 6 PM, doctor Welcome, yes that is her real name, came and introduced herself. She let me know that if things stayed this slow, I could go back upstairs. 20 minutes later my lower back began to ache, and I felt as though I needed to go to the bathroom. At this point I was unable to use the restroom alone and paged the nurse to come help me. In the 3 minutes it took for her to come into the room my pain in back had gone from 0 to 100 and I felt like I was breaking. She quickly came over and lifted the blanket to see I was fully dilated, and my water bag was bulging out. She slammed the blue code button on the wall and began saying very loudly over the loud speaker ‘Code blue, labor and delivery, holt, NICU team stat.’ I was versed in healthcare enough that this point to know that something was very wrong. I knew that at just 28 weeks and 1 day it was too soon for this baby to be born. Dr. Welcome came rushing in and informed me she would break water and that the baby would likely just fall out. My pain at this point was beyond anything I had felt before and I urged the doctor to move forward. Dr. Welcome broke my water and I immediately felt a release of pressure, I took a huge sigh, and everyone said, ‘Don’t push.’ Still sitting between my legs and now with a room full of what felt like 50 people, Dr. Welcome turned to the closest nurse and said ‘Get me an ultrasound machine and prep for emergency surgery. Meagan, your baby has turned sideways. I am holding her body and preventing the cord from wrapping around her. We are going to have to put you to sleep so we can save your baby.’ What happen next was a complete blur. The last thing I said before they put me to sleep was ‘Save the baby. I don’t care about me, do whatever you have to save my daughter. Please.’ The RT putting me to sleep smiled through his mask and said something I know he shouldn’t have ‘Don’t worry you will both be just fine.’ I woke up from my emergency classical C-section muttering ‘Is the baby dead? Am I dead? I’m going to go see her.’ The nurse sitting in the room with me tried to reassure me that once I had feeling in my legs, I would be able to go see her. This was the first time I saw my mama bear come out. I turned to nurse and said, ‘If you won’t take me to see her, I will crawl if I have to.’ My best friend at the time looked at the nurse and said ‘You might want to read her chart, she’s not kidding.’ I still don’t know of any other mom in that hospital who was wheeled down to the NICU in a full hospital bed. But it was so worth it.
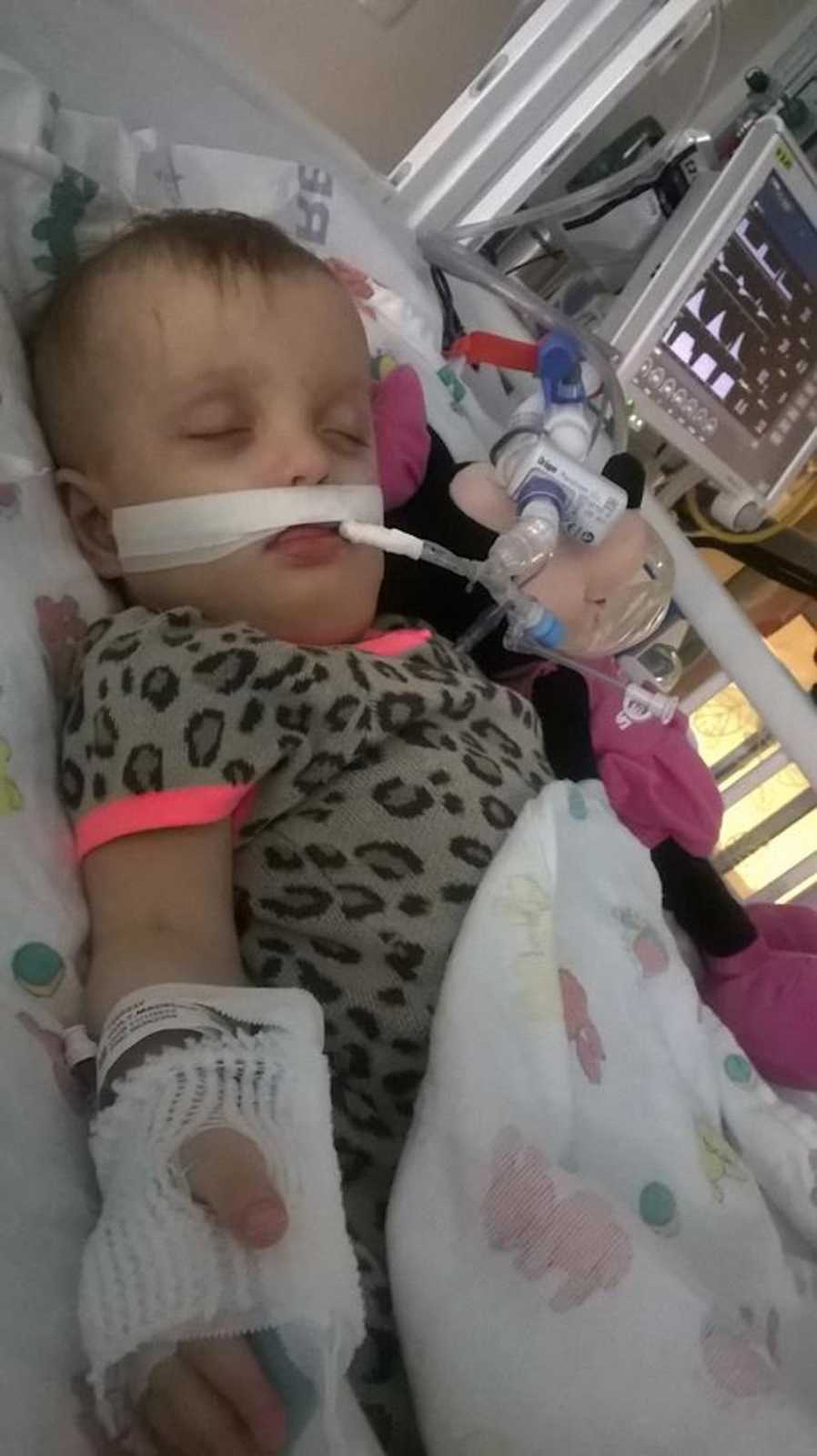
The first time I saw Madeline I knew. I knew it was job to protect her, to fight for her. She came crashing into this world weighing a whopping 2 pounds 3 ounces. From the moment she was born she has defied all medical science. She had no problems from her prematurity and went home with no tubes, no wires, just two days after her expected due date. Most of you would expect this to be the end of our story. The happy ending. Sadly, this was the start of an even bigger journey and what led our family to finding our purpose in this world.
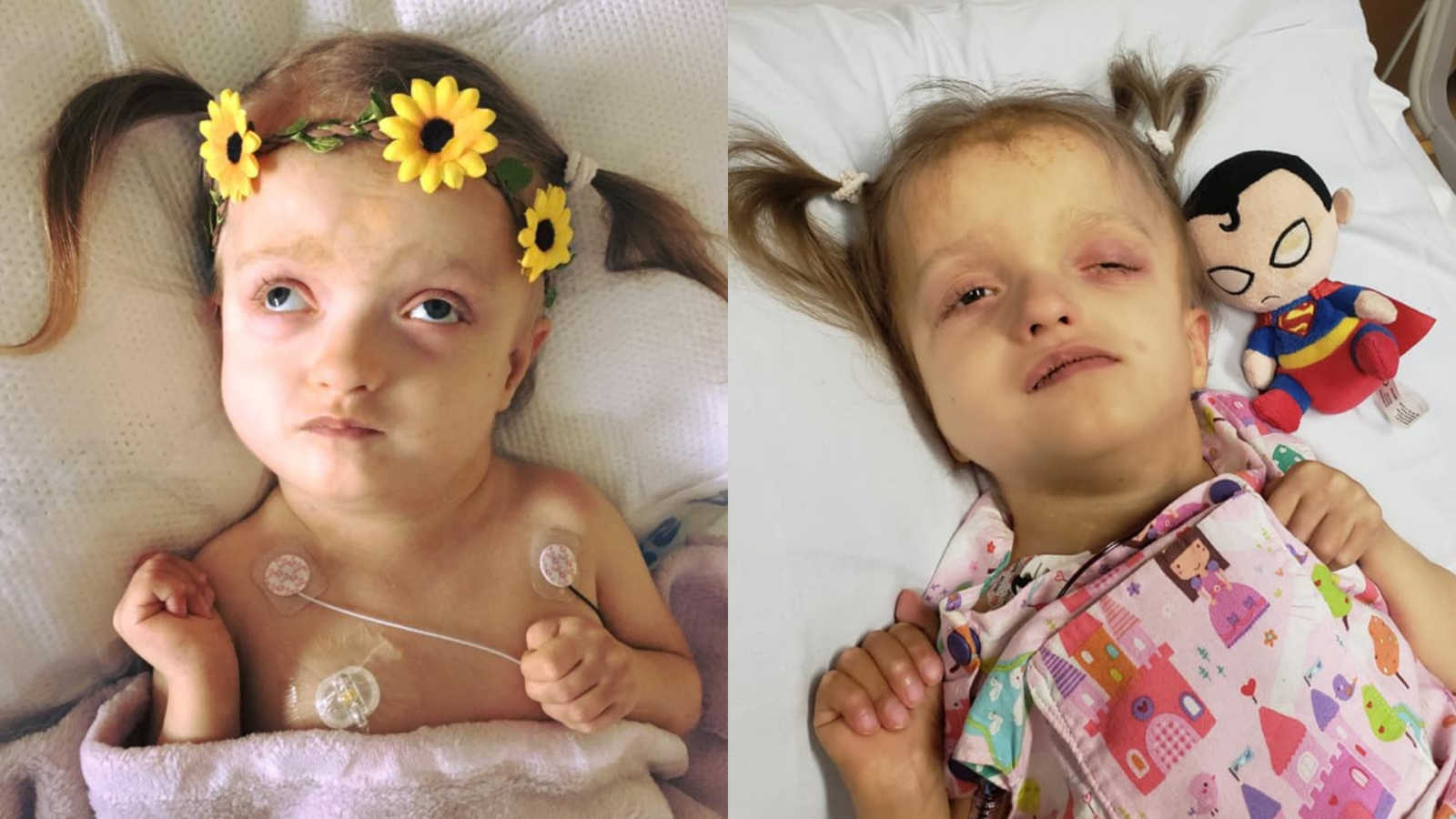
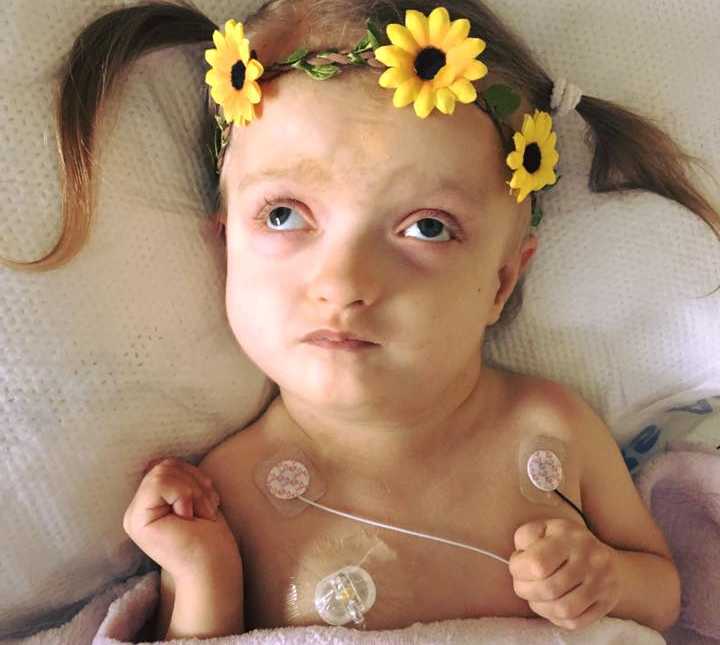
Maddie’s prognosis, the nine-letter word that is supposed to pre-determine how much Madeline would be able to learn and how much time she would be with us before she left this world, has caused problems. Zellweger syndrome. A terminal genetic disease that destroys the white matter of the brain. There is no cure or course of treatment and most children with this devastating disease do not survive past their first year of life. Madeline is deaf, blind, completely dependent on a feeding tube, she has osteoporosis, kidney stones, adrenal insufficiency, sleep apnea, bleeding episodes, very limited mobility, recently went into end stage liver failure, and in January of 2015 developed life threatening seizures. Despite such a grim prognosis I was determined to give Maddie every opportunity possible to learn and grow. I was determined to never give up on hope. By 2 years old Madeline had already beaten every expectation any doctor had for her. She was sitting with little support, was able to roll over, could play independently with toys, had over a 100-word sign language vocabulary and even began speaking words and mimicking sounds. One January morning in 2015, Madeline had her first grand mal seizure. It lasted nearly 2 hours and she was unresponsive to pharmaceuticals. She was taking medications that could knock out a horse, dilaudid, methadone, gabapentin, kepra, phenobarbital, and I was told that my daughter was going to die. That, that uncomfortable talk, that thing that we’re not supposed to talk about had become even more unbearable, because what’s worse than dying? Being told that your toddler’s going to die and there’s nothing the doctors can do about it. Being told ‘regardless of how many medications we give her, no matter how much CPR we perform, she’s going to die.’

Giving up hope was not an option for me, and this was the first time in Madeline’s journey that I had to stand up and say no. When everyone around me was telling me to give up, I took a chance. I did what every 21st century parent does, and what every doctor tells you not to do and I googled it. I found cannabis. I took my child home for one night, April 10th of 2015, Maddie was discharged from Seattle Children’s Hospital with phenobarbital and methadone to keep her comfortable, so I could have one night at home with my baby. I took that one night and met with a naturopathic doctor, I got her authorized to use cannabis, and I found someone to donate cannabis oil. I decided to give cannabis is shot. I want to be real for a minute and say that I wasn’t trying to stop the seizures, I was trying to hold my baby while she died and not have the drugs take her away from me. I wanted to hold my baby while she peacefully passed away instead of convulsing out of control.

Taking a chance, starting cannabis, was the absolute best thing I did for my daughter. She stopped having grandmal seizures. She breathes during every tonic clonic seizure she does have, and all those drugs, THC has helped wean her off of 24 of them, and with the help of terpenes she has remained opiate free for over a year.
Returning to the same facility that sent my child home to die was not easy. Facing the same the doctors that signed the paperwork that read ‘Madeline is out of medical options’ wasn’t just hard it was terrifying. But our family made a choice to do things in a way no parent or family had done before. To choose to not be like most people who chose to fight, place blame and hide things. We chose understanding, education, and above all, we chose to have hope even when it seems impossible. By having this attitude, by choosing to be different, we have drastically changed the way doctors, nurses, and other health care workers practice medicine. Maddie’s legacy has made an immense impact in the lives of every healthcare worker who cares for her.
Now, our family is on a mission to help other families, and thus how The Hand That Heals was born. It started when my partner, Chad and I saw a need to connect. To share. To inspire others who feel lost or alone. Being a writer and a very resource savvy family, I was sick of seeing the same old fluffy blogs with tips on how to make your life better but all through a filtered lenses. What I mean by that is there’s no realness, there’s no struggle shown. Our world has become so obsessed with what filter will look best and choosing to only share the beautiful side we have forgotten how to embrace the beauty in what may seem tragic. We have forgotten have to live and love our whole life. Our lifestyle blog is a multi-dimensional collection of the resources and experience we have gained, the places we see, people we meet, and the many aspects of our day to day life. With no fluff or filters just our real selves.

The blog is just one piece of our company. We also self-publish books and this year completed a book we have been working on for almost 6 years, A Different Kind of Journey; Effectively Advocating for Your Medically Complex Child. While the title sounds like your typical self-help book it is the farthest thing from that, it truly is a welcome guide to the parenting club no one wants to join. While there are plenty of tips and guidance for parents new to world of medical complexity it also offers a very real look at what we have gone through during our journey. Stories of how we have been affected by doing or not doing certain things.
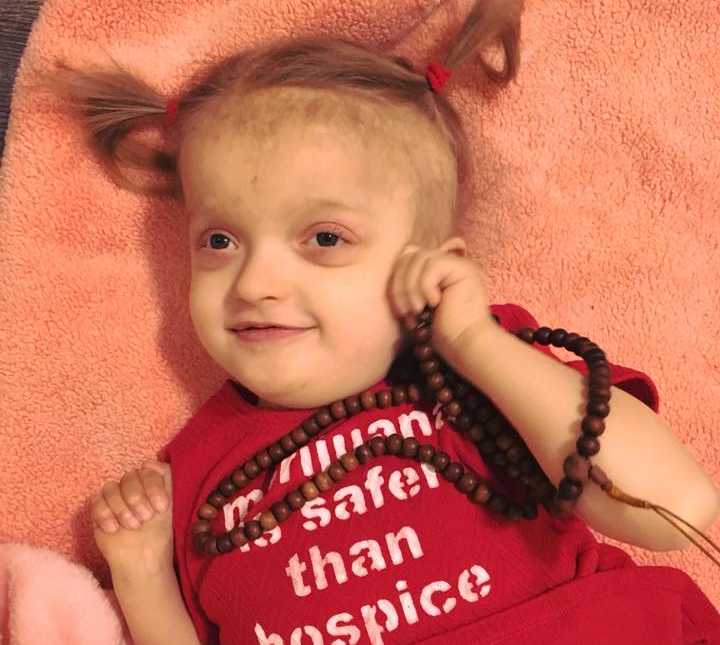
When we aren’t volunteering or running our family owned business then we are giving motivational speeches. Empowering other people in our community to stand up for those without a voice, breaking down the stigma surrounding infant and child loss, and helping others to see that with hope and love you will be just fine.
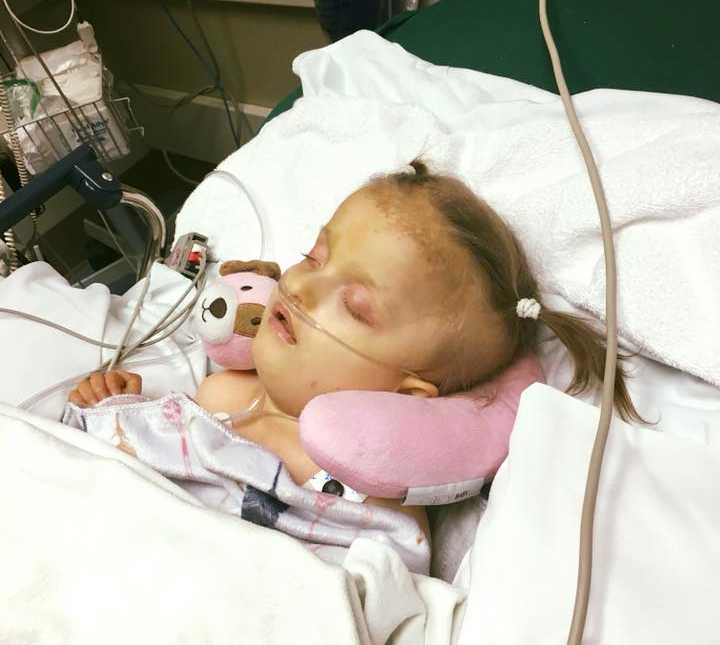
I’m sure most people are reading this article thinking, wow this family has it all together. How do you they do it? How do they stay so strong? Want to know the truth? Our ‘secret’ so to speak? There is no secret. We do not possess some sort of super human power to overcome. We are strong, because being strong is the only choice we have, because at the end of the day, if Maddie was your daughter, wouldn’t you do the same? Chad and I see what we do as a duty. A responsibility to our children and our community to do better. To be better and to always help others.
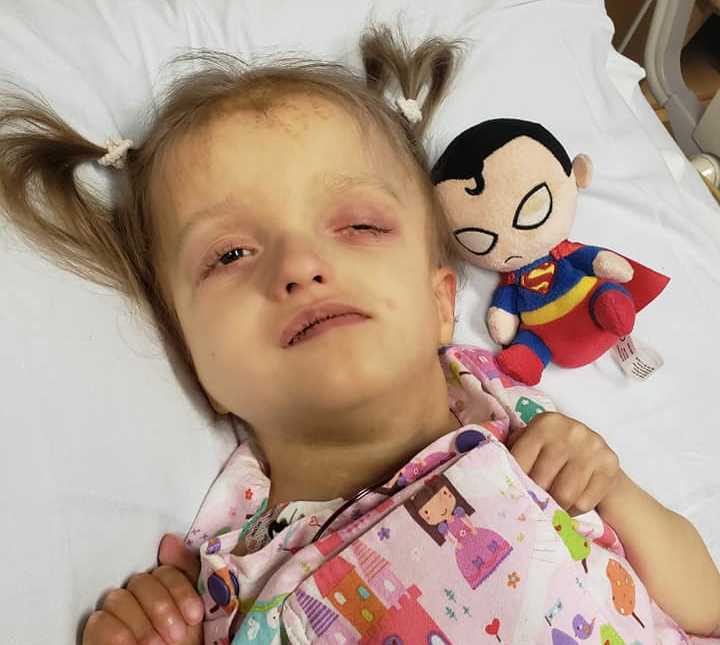
By sharing we hope to empower other people, from all walks of life to embrace their own beautiful tragic journey. Be bold. Remove your filters and embrace all that is you.”
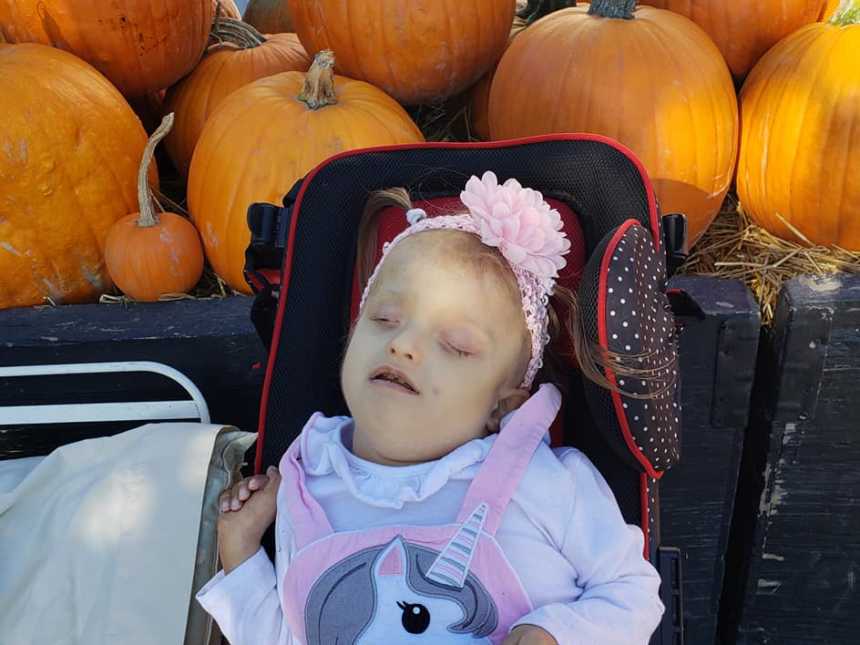
This story was submitted to Love What Matters by Meagan Holt. Follow their journey on their website, Facebook, and Instagram. Submit your story here. For our best stories, subscribe to our free email newsletter.
SHARE this story on Facebook, Twitter or Instagram to encourage acceptance and inclusion, let others know there is a community of support available.