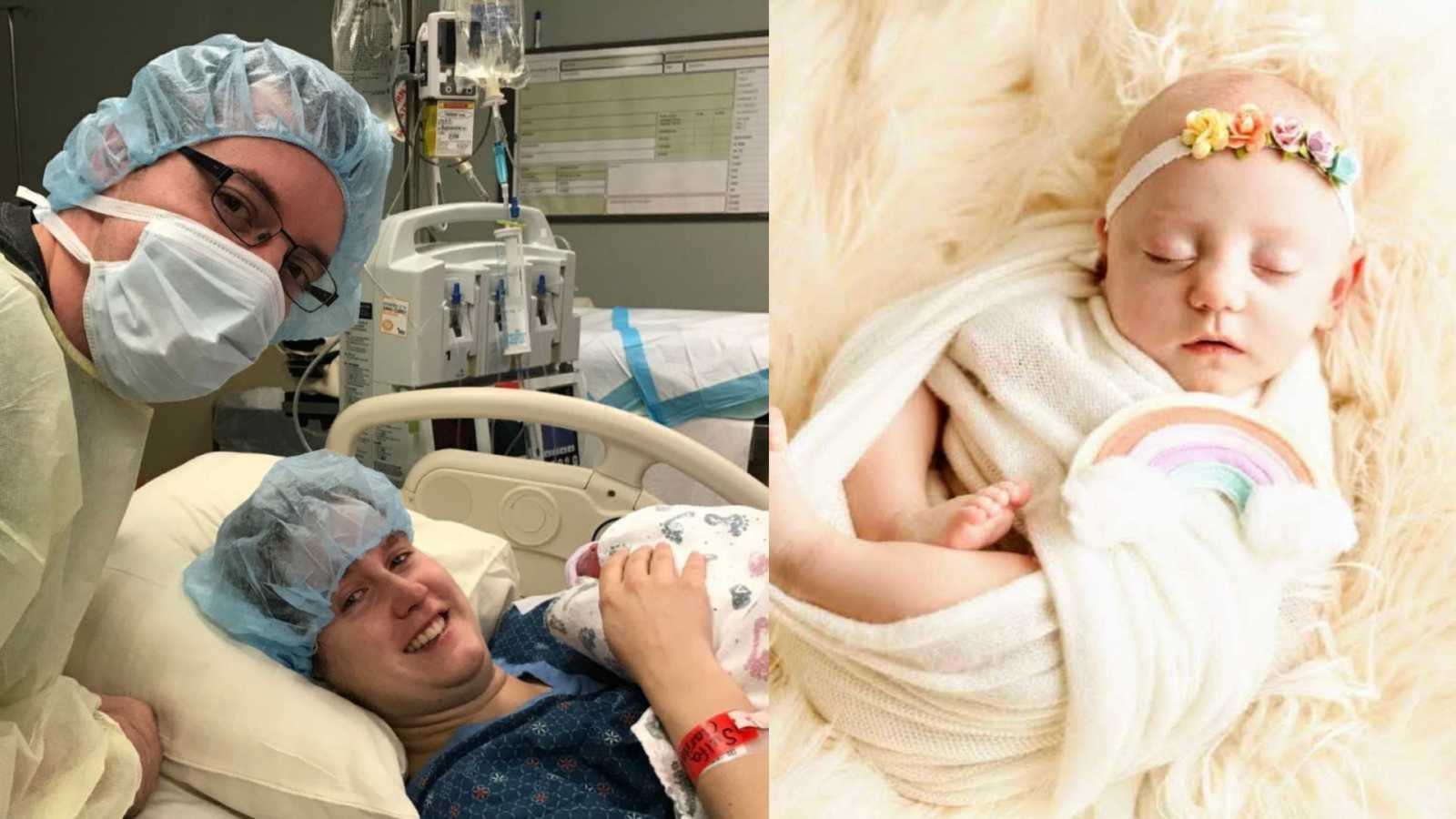
“You’re 4 centimeters dilated. I’ll call your doctor and see what he wants to do, but there may be nothing we can do to stop your labor,’ the triage nurse said after checking my cervix. I was 20 weeks pregnant with our IVF boy/girl twins.
A week earlier, we saw the specialist. We found out we were having a boy and a girl. Everything looked great. Monday we had an appointment with my OBGYN. I remember him giving me a high five and telling me I was making it look easy. I was having the easiest pregnancy until suddenly I wasn’t.

Thursday, June 29, 2017 forever changed our lives. It was 8 p.m. and my husband and I were hanging out watching the final episode of West Wing on Netflix. I remember feeling uncomfortable but I was pregnant with twins so I didn’t think too much about it. After the show ended, my husband went to our office to work on his computer and I laid down to watch my own show.
I started noticing that the discomfort was now stronger. I drank a glass of water and lay on my side. Then I realized it was coming and going, and feeling like cramping. I was telling myself there was no way I was having contractions! I was only 20 weeks but still worried, so I downloaded an app on my phone and started tracking the cramping. Sure enough the cramping was happening every 4 to 7 minutes, lasting longer than a minute each. It happened 12 times in an hour. I texted my husband telling him, ‘I think I should call my doctor, I might be having contractions!’
By then I was crying. It was after 9 and I didn’t want to be the crazy pregnant lady calling the doctor’s office late at night. I called and talked to the answering service, gave them my info, and told them what I thought was going on. Within 15 minutes, my doctor called me back. He instructed me to head to the hospital and to go to labor and delivery to get checked out, just to be safe.
After hanging up the phone, I laid on my bed and cried. I wanted to go to sleep and wake up in the morning and have everything be okay. I didn’t want to go to labor and delivery to find out everything was perfectly fine and have everyone look at me like I was crazy. I didn’t want to get there and find out something was wrong. But I also didn’t want to stay home and find out later I should have gone in.
We got in the car and made the 35 minute drive to the hospital. As we drove, the tightening and pain continued. Because it was so late at night, we had to go in through the emergency room and wait to be taken up. Another couple was also there waiting to be taken up to labor and delivery. We were all taken up together and put in rooms next to each other.
The nurses went to their room first. We could hear them laughing and the sound of their baby’s heartbeat. I sat there waiting, hoping I was wrong. That maybe it was all okay and we would soon be sent home. Then the nurse came. She asked about my history and what brought us in. She used the Doppler and checked their heartbeats, both were beating strong. Next she informed us she’d do a cervix check to see if I was dilated. The nurse completed the check and said the words we will never forget: ‘You’re 4 centimeters dilated. I’ll call your doctor and see what he wants to do, but there may be nothing we can do to stop your labor.’
She left the room and my husband and I sat there in silence for a minute. Tears started to roll down my face as he took my hand. I remember telling him we can’t lose them. The nurse came back in and said my doctor wanted to be aggressive. He wanted to admit me and start some medications to hopefully stop my contractions.
I was wheeled into a room, hooked up to an IV, given a catheter, hooked up to monitors, and then the waiting began. The nurse would come in every couple hours to check on me. I remember asking if the contractions had stopped, the medicine they put me on made it so I wasn’t feeling many of them. Each time I was told no, the contractions had not stopped.
The next morning, I was miserable because the magnesium they give you makes you feel awful. They did an ultrasound and both babies were doing great but the contractions continued. They brought in a social worker and a neonatologist from the NICU upstairs. We were told that at 20 weeks it was too early for our babies to be helped if they were to arrive that day. If we could make it to 22 weeks the doctors could try to save them.
Later that morning, our son’s water broke. A couple hours later they checked heartbeats and had a hard time finding them both. They brought in equipment and did an ultrasound and again we heard words that would forever change our lives. ‘Your son no longer has a heartbeat.’ He had moved past my cervix and his heart stopped.
The doctors consulted with each other and decided it was best to try to deliver our son. I tried pushing but nothing happened. The doctor tried to manually assist but it was too painful. I was given an IV medication to help with the pain but as soon as it kicked in, it knocked me out. We tried twice but our son hadn’t moved. The decision was made to give me an epidural and deliver him.
At 8:05 p.m. on Friday, June 30, 2017, our son James Lawrence was delivered stillborn. It was one of the most devastating moments of our lives. He was wrapped in a blanket and placed in the cold warmer. We were told when we were ready, we could hold him. We held him, talked to him, took pictures with him, called our families and let them talk to him. We kept James with us until around 6 a.m. the next morning, which allowed us time to say goodbye. We let him leave with our nurse before her shift ended, I knew I couldn’t bear to send him with someone new.
Our doctor told us we could maybe expect to have 4 to 5 hours between our son’s birth and our daughter’s. After James was born the contractions stopped and my cervix closed. I was eventually moved to the antepartum unit and put on bedrest. I was allowed out of bed to use the bathroom and shower.
For 4 weeks my hospital room felt calm and safe. I was surrounded by doctors and nurses who checked on me throughout the day. Any questions or concerns were quickly addressed. But once again my labor spontaneously started and again they were unable to stop it. I prayed the same would not happen with my daughter.
On Wednesday, July 26, 2017 our daughter Amelia Jane was born in an operating room surrounded by doctors and nurses. Her first cry was the most amazing sound I’ve ever heard. I remember letting out the biggest sigh of relief. We made it. Our daughter was born breathing, her heart beating, she had a chance.
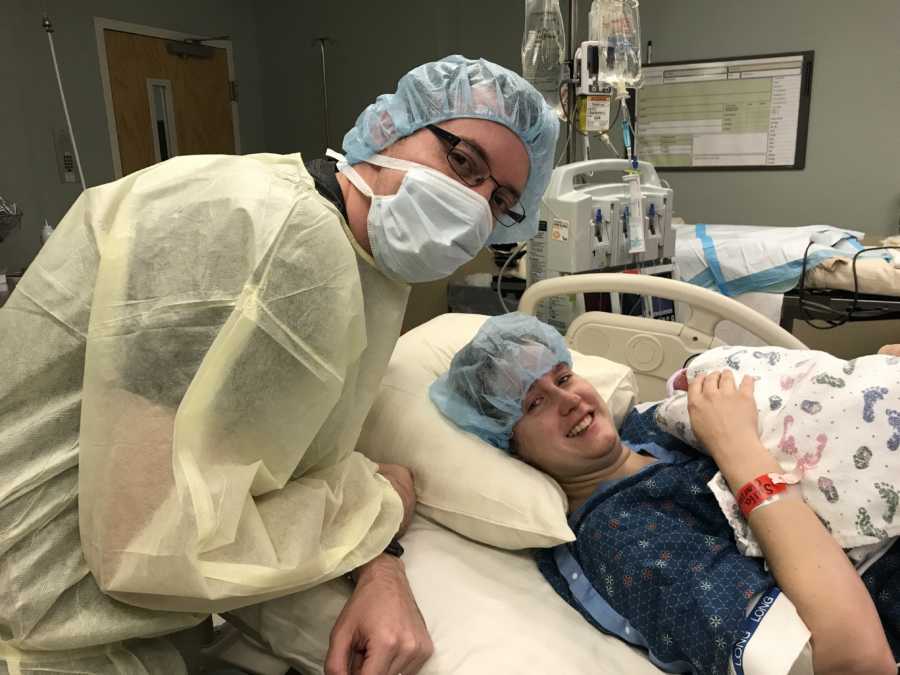
Amelia spent 141 days in the NICU before being discharged. Today Amelia is thriving and we are continually learning to navigate life without James. How can something be such a blessing and at the same time such a curse. We share our journey in hopes that it might help others who find themselves on a similar path.”


This story was written by Michelle Herder. You can follow her on Instagram here and her blog here. A version of her story was written here. Submit your own story here, and subscribe to our free newsletter for our best stories.
Read more stories like this:
Provide hope for someone struggling. SHARE this story on Facebook and Instagram to let them know a community of support is available.