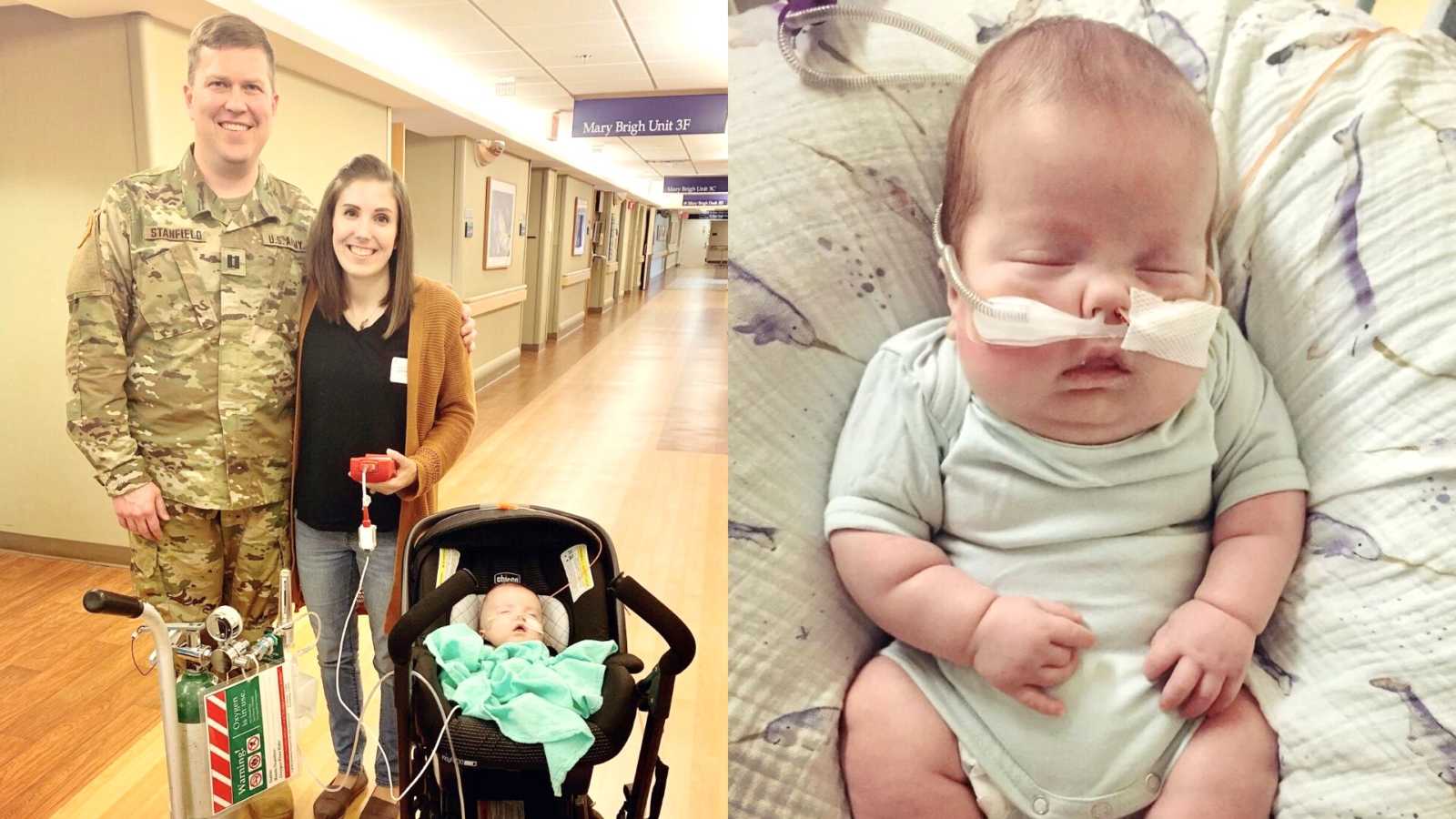
“The path to growing our family has been far from linear. Together, my husband Mark, and I have faced multiple first trimester miscarriages, high blood pressure, hyperemesis, and any number of other issues. Our oldest, Jack, was born in November 2014, after a difficult 9 months, and frightening labor complications. Next came our daughter, Lillian, who was stillborn at 35 weeks in July 2016. Not a day goes by without thought of her, and while we will always grieve her death, she is woven throughout our daily lives in the most beautiful way. Our third born is Lawrence, who arrived in January 2018, after what was likely our most textbook pregnancy, but also the most emotionally challenging, as we feared his death every single day. Then we had Gilbert (nicknamed ‘Ghillie’), who was born via emergency c-section on March 31st, 2019.


We went to labor and delivery for decreased fetal movement the evening of his birth, and it felt eerily reminiscent of the days leading up to Lillian’s death. I was only 25 weeks pregnant, and couldn’t officially begin counting kicks until 28 weeks, but I knew that any change in movement could mean something was wrong. At the time, we didn’t know how wrong that something was. He failed two biophysical profiles, and a team of people in blue scrubs rushed me to the OR to prep for a c-section. In a matter of minutes, I was staring up at the bright lights, unable to feel anything below my rib cage. Mark arrived by my side just seconds before we heard the doctor say, ‘He is out!’ He was too small and weak to make any sort of audible cry from behind the sterile drapes, and I was certain he had died.
A whirlwind of activity took place, and Gilbert was quickly taken to the resuscitation room to be stabilized. I couldn’t stop shaking while they stitched me up, as fear of what was to come took hold. It was a few hours until I finally saw him, when they maneuvered the huge neonatal transporter into my postpartum suite. It was such a massive collection of equipment, all designed to keep the littlest life within it alive. He was only 1lb 13oz, and 13 inches long, and wrapped in plastic to protect his paper-thin skin. Humidity clung to the window of his isolette. Amidst my own fog of narcotics and influx of information from doctors, I managed to take his tiny body in. The perfect combination of his brothers and sister, and a surprising amount of thick, dark hair given his young gestational age! He was being transferred to a higher level NICU, which was still part of our medical complex, and only a few blocks away. Mark spent that first night driving back and forth from my room to the NICU.
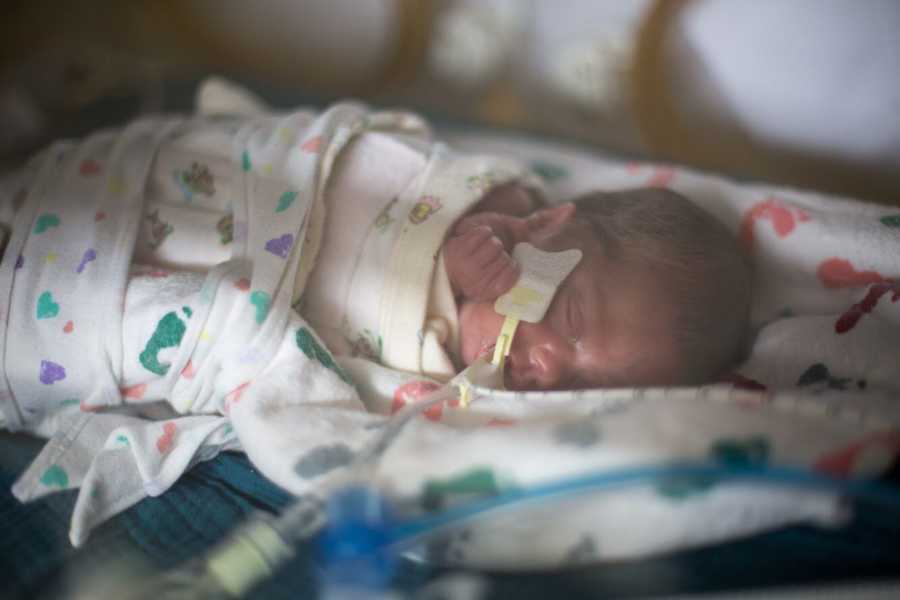
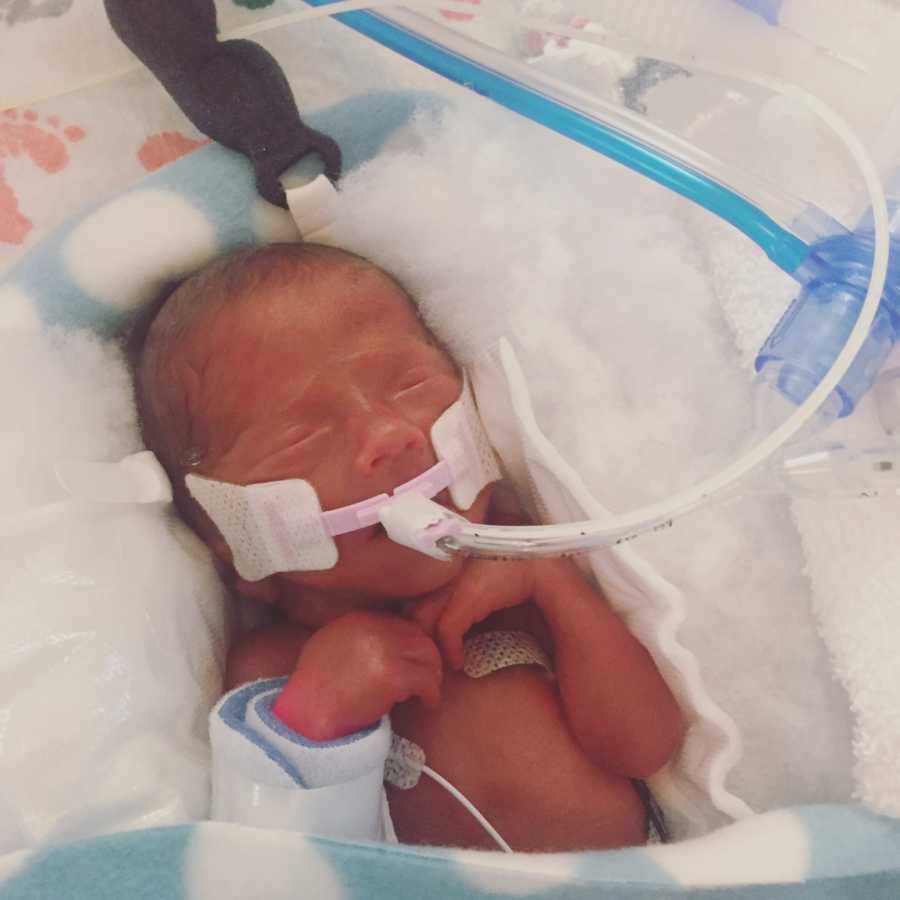
The neonatologist who had attended Ghillie’s delivery called my room the next morning while I was eating breakfast and awaiting ambulance transport to the hospital where the NICU was located. I could tell from his voice that he didn’t have good news, and I prepared myself as best I could for the worst news — to be told that Gilbert was dying. The mind can’t help but go there after one of your babies died, and this was the just the first of many instances that I envisioned being told of his death. The doctor instead said that Ghillie had suffered severe brain bleeds, which were seen during the biophysical profiles prior to delivery, and confirmed via head ultrasound earlier that morning. ‘Why weren’t we told this sooner?,’ I thought to myself, ‘Obviously they suspected this before he was born, so why didn’t we know too?’ Up until that point I believed his biggest issue was going to be underdeveloped micropreemie lungs, but that wasn’t true. The physician explained that brain bleeds can be common in extremely premature babies, but having them occur in-utero, as in Gilbert’s case, is incredibly rare (probably 1 in 10,000 or less).
‘Is there anything we can do to stop the bleed and remove the blood from his brain?,’ my voice broke as I asked. But all we could do was watch and wait. I felt entirely defeated. Yet again, my body had failed to keep one of our children healthy.
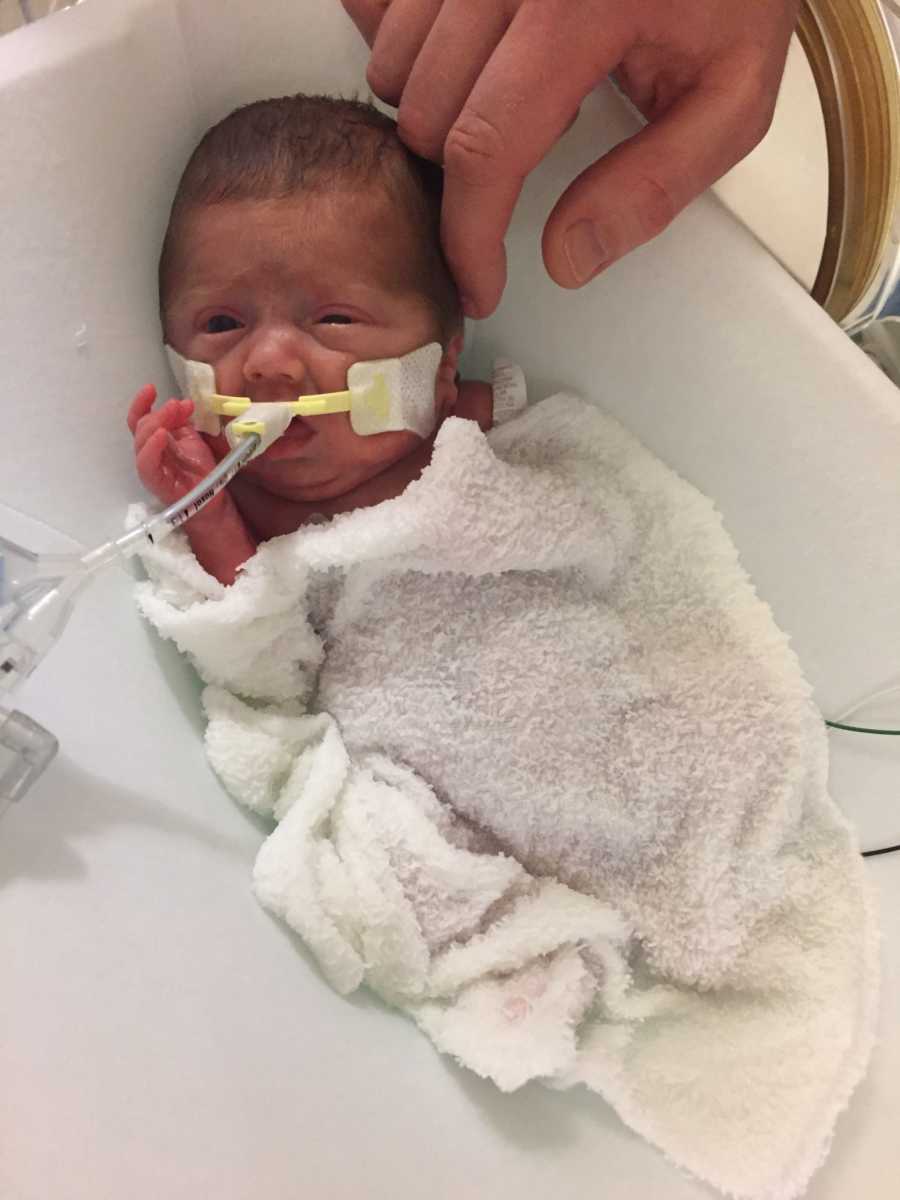
I went to his room as soon as I was transferred to the other hospital. It was a small space, separated from the rest of the unit by glass doors, and reserved for the smallest and sickest of babies. All of the equipment surrounding his isolette made it feel even smaller. His eyes were fused shut since he had been born so early, and his fragile body was covered in wires and tubes. Medication pumped through his body, and machines were beeping all around him. But none of it mattered, and seemed to melt away as I immediately, and deeply, fell in love with him. That afternoon the doctors escorted us to a conference room, and displayed ultrasound images of his brain on a large projected screen for everyone to see. It was far worse and carried even greater consequences than I could have imagined. The right ventricle of his brain had a Grade IV intraventricular hemorrhage (IVH), the most severe. His left ventricle was a Grade III, the next most severe. They explained that as the brain heals differently than any other area of the body. As blood product is cleared, healthy brain tissue gets absorbed along with it. There was no saying how much of his brain would disappear, but it would probably be a large amount.

Talk of cerebral palsy and special needs quickly followed, which seemed to be certainties in the eyes of the physicians. ‘There’s a high likelihood that he’ll never walk or talk, and he could have a very low quality of life.’ It was a heavy discussion of morbidity and morality, and we were bombarded with statistics of children who faced similar circumstances. At one point we were told he had a 50% chance of survival, which was nothing short of devastating. They asked if we wanted to stop life-saving measures and switch to comfort care based on these projected special needs and possibility of death. To us, that seemed incomprehensible, since he was, for the most part, clinically stable. Having escorted our daughter from morgue to funeral home, planned her memorial service, and accepted that we will carry the weight of grief for a lifetime, special needs were far from our worst-case-scenario. We stood our ground, and said he would be our ‘wayfinder.’ We trusted that he would tell us in his own way if things became too much, and it was time to stop fighting.
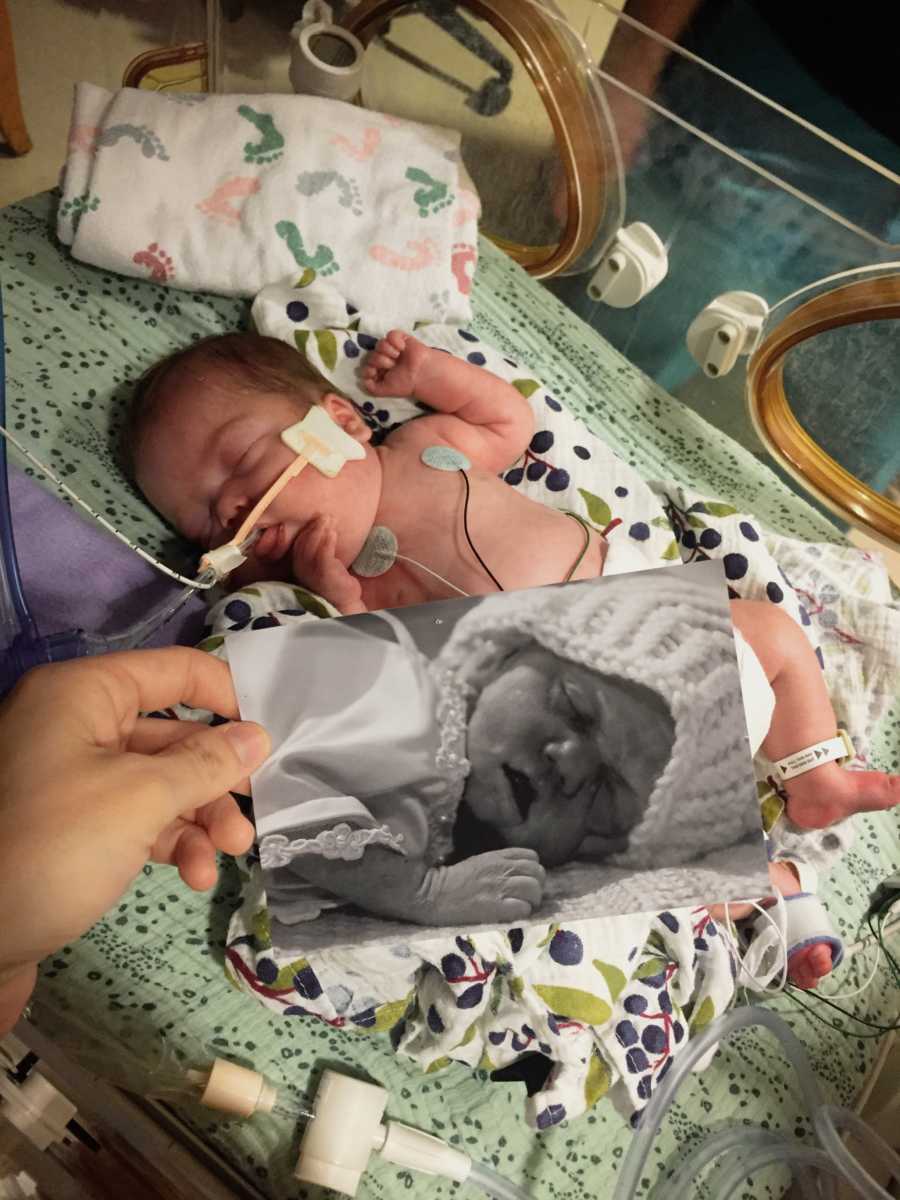
The months that followed were marked by similar conversations, and more statistics regarding special needs. We held steadfast despite it, and maintained that we would rather have a special needs child than a dead one. In the meantime, Gilbert had multiple surgeries, attempts to wean the amount respiratory support he needed, and weekly ultrasounds of his brain. I lost count of the number of times he was resuscitated, and seeing his body lie limply on the table brought back many memories of his sister. I asked just about every variation of, ‘Is my baby dying,’ possible, and always kept my phone nearby, having grown accustomed to calls in the middle of the night to tell us he’d experienced yet another setback in his care. We clung to every shred of normalcy that we could, and learned how to change the smallest diapers, give bed baths, and take his temperature. We read to him for hours on end, and told him about his family. When he was old enough, we started music therapy, and his collection of CDs became known throughout the NICU — everyone’s favorite was his disc of Red Hot Chili Peppers lullabies. He loved being held, which was usually a multi-person affair, because of his respiratory support needs. Eventually, I was able to babywear him too. We vowed to give him and his warrior brain as much sensory input as possible, in a desperate attempt to try and save what neurological connections we could.


The bleeds also put him at high risk for hydrocephalus, or brain swelling, which can be deadly if it goes untreated. Each week we watched the bleed slowly absorb, and brain tissue disappeared right along with it. Around 4 months old he had his first MRI. We had been waiting for higher-fidelity imaging since the beginning, and the opportunity presented itself when we learned he needed a third eye surgery. Since he would already be intubated and sedated for that procedure, they decided to do an extensive MRI at the same time. I went back to the hospital late that night.
‘What did the imaging show?,’ I asked.
I expected it to be the same as usual, and braced myself for another special needs conversation that required a certain level of assertiveness. But instead the doctor told me, ‘It will be better to go over the results tomorrow morning, when more people will be here to help interpret the radiologist’s report.’
That was the first time I cried in the NICU. I knew something was horribly wrong.
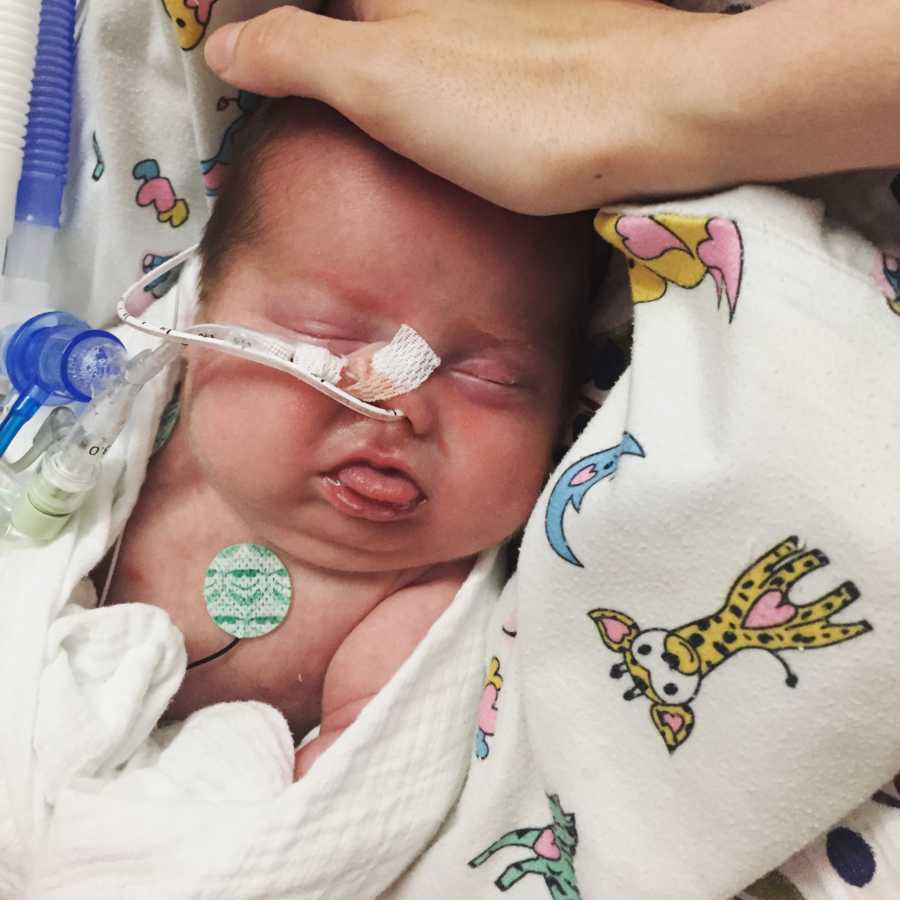
Mark rushed home from the hospital the following morning and they told me Ghillie had developed hydrocephalus. Deep down, I think we knew this was coming, having watched the shape of his head change over recent weeks, and his eyes become more downcast — a classic sign of increased intracranial pressure. When discussing the MRI results, one doctor said, ‘It’s unlikely your son will survive childhood.’ I felt sick, exactly as I had the weeks following Lillian’s death, a physical sensation I will never forget. Gilbert was heavily sedated, and his vital signs were reflecting the impact of his brain swelling. It was one of many times that I wished I could trade places with him. Afterall, I’d already lived years of life and he hadn’t even experienced a breath of fresh air outside hospital walls. It seemed entirely unfair that he was facing these circumstances, and as a mother, I felt utterly helpless.
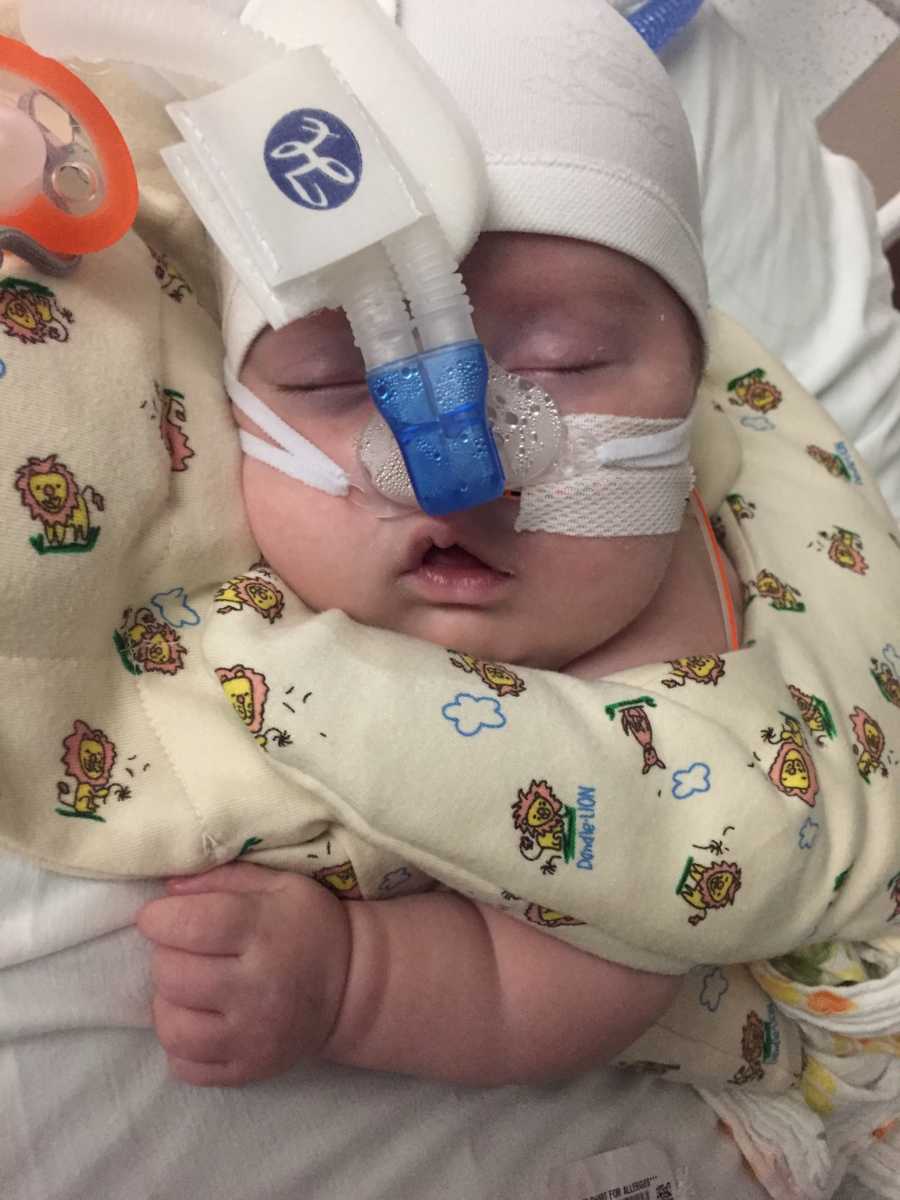
When we met with the neurosurgeon, we were presented with two options: he could either have a shunt placed, or an undergo an endoscopic third ventriculostomy (ETV), which is a newer alternative to a shunt. Continuing to wait would do him no good, and we opted for the ETV, since its success rate is about the same as that of a shunt, but without a lifetime of technology dependence. The day of his surgery, we walked him down to the OR, and kissed him goodbye. I think I held my breath until we got word that it was done, and he was okay. The relief of pressure in his brain had an immediate effect. His vital signs were back within a normal range, and his ventilator settings were the lowest they had been his entire life. Though his journey was far from over, he was holding his own, and proving many people wrong.

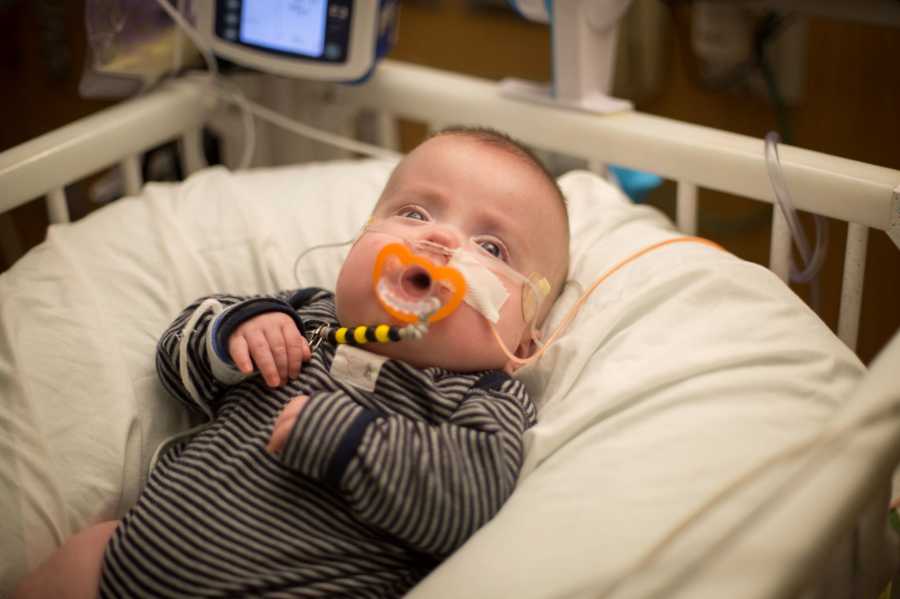
On September 24th, 2019, after 177 days in the NICU, Gilbert finally came home. He still needs 24/7 oxygen, and has a g-tube while we continue to work on feeding. His brain was just one small part of an entire constellation. Chronic lung disease and bronchopulmonary dysplasia, tracheobronchcomalacia, retinopathy of prematurity, and severe osteopenia are just a handful of his other health issues. He will be followed by neurosurgery for years to come, to make sure the ETV is continuing to function, and his brain will continue to be monitored for swelling. Right now he has MRIs every other month, and his head circumference is measured weekly. We keep track of various neurological signs daily, and are always on the lookout hydrocephalus. It is a constant source of worry, as we don’t want to damage any of his remaining brain. Life at home has its own nuances as well, some of which we expected but others we were entirely unprepared for. He has at least one follow-up appointment every single week for the time being, and we’re slowly learning how to handle questions and comments from strangers who see his medical equipment. These range anywhere from words of pity to the downright offensive, and though we always want to use them as opportunities to educate, sometimes it’s a lost cause.


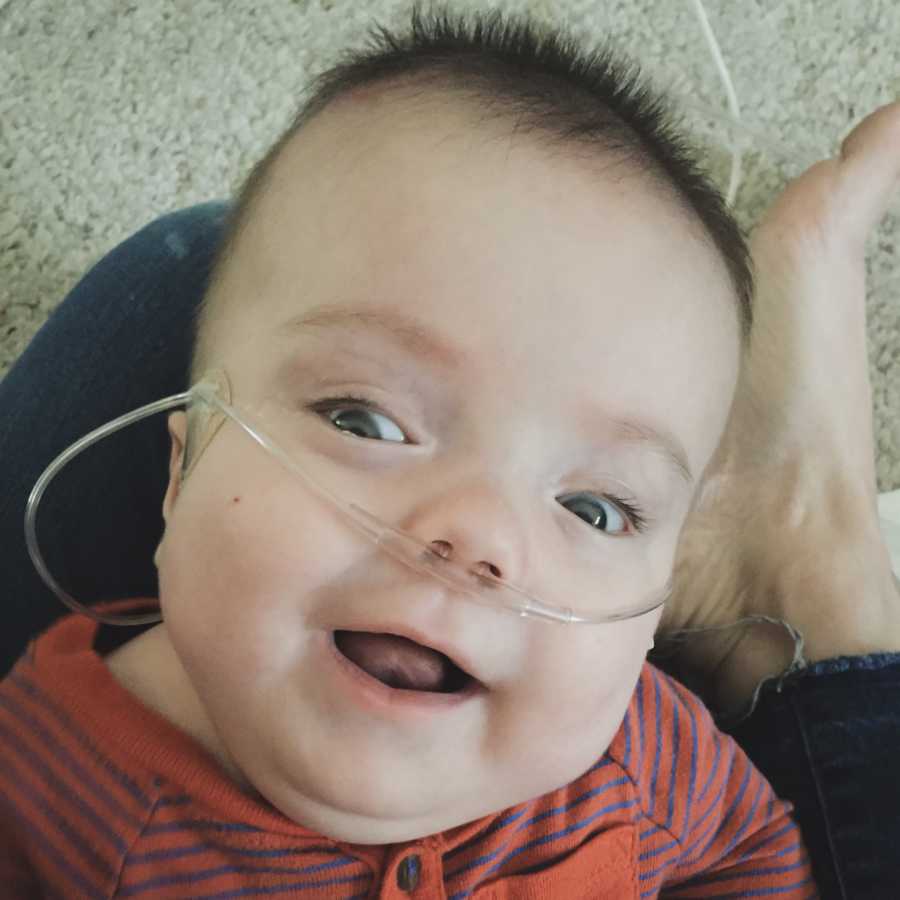
Against all odds, he is thriving. He recently began to smile, enjoys anything tactile, and still loves to snuggle. He is peppered with sensory input from his brothers, who are thrilled he is home, and always settles down with talk of his sister. He is already doing things that many people said he never would, and we like to joke that he’s leaving a trail of middle fingers behind him for the naysayers. There is no crystal ball that can predict what his neurodevelopment will look like in the end, and we continue to stand by our belief that special needs have no bearing on the value of his life. Yet we can’t help but wonder how much ‘Gilbert’ we’ve lost as his brain has literally disappeared before our eyes. We try to stay realistic about his prognosis while simultaneously holding onto hope that his neuropathways will rewire. From his earliest and most difficult of days, we’ve said we’ll love him in any condition, and that remains just as true in the present. In Scottish, the term ‘ghillie’ refers to a guide who leads hunting and fishing expeditions, and that nickname serves him well. He will forever be our wayfinder, showing us the way, and helping us navigate whatever lies ahead.”

This story was submitted to Love What Matters by Anna Stanfield of Minnesota. You can follow her journey on Instagram. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more powerful stories like this:
Provide strength and encouragement for others. SHARE this story on Facebook with your friends and family.