“In late February of 2019, at 34 weeks pregnant with my third baby boy, I fell ill with the flu. Because of my pregnancy, I was especially vulnerable. My uterus was crowding my lungs, which meant although I was coughing almost constantly, I wasn’t able to effectively work the fluid out. Within a couple days, I had pulled a muscle in my abdomen. It sent such a splitting pain down my enormous belly every time I coughed, so I started suppressing the coughing.
Each day, I’d think I’d start seeing the turnaround eventually, because that’s how it always goes when you get sick. You rest, you drink water, and you get better, right?

I went to urgent care on day five thinking they would give me antibiotics or some other medication. I felt like I was dying, and looking back, I know I was. The doctor wrote me off. ‘Take a couple pregnancy-safe over-the-counter meds, wait a few more days, and you will feel better soon.’
But five, six, seven days passed, and I had only gotten worse. I was unable to breathe if I lay flat, so I had to sleep sitting upright. It became harder and harder to stay awake for more than an hour or two at a time, and then I became unable to speak or even open my eyes, though I was conscious.
On day 8, I began having strong contractions. My body was dying, and its primitive response was to get the baby out so it could survive. We called the hospital, and they told me to drink water, rest, and wait. The following morning the contractions were so strong and consistent, I knew I was having my baby. We drove to the hospital where they took one look at me and knew instantly I was dying.
I was rushed in for an emergency caesarian, put under general anesthesia and intubated. Baby Thomas was born, but it was weeks until we could meet each other. Once I was sedated for surgery, I remained on a ventilator for three days, unable to breathe on my own. I was in lung failure, suffering from pneumonia which had turned septic, and my body was shutting down. I had various strep and staph infections caused by influenza, and Tommy was rushed to the children’s hospital under quarantine to be checked and monitored for eight days to make sure he didn’t have all the same infections I had.
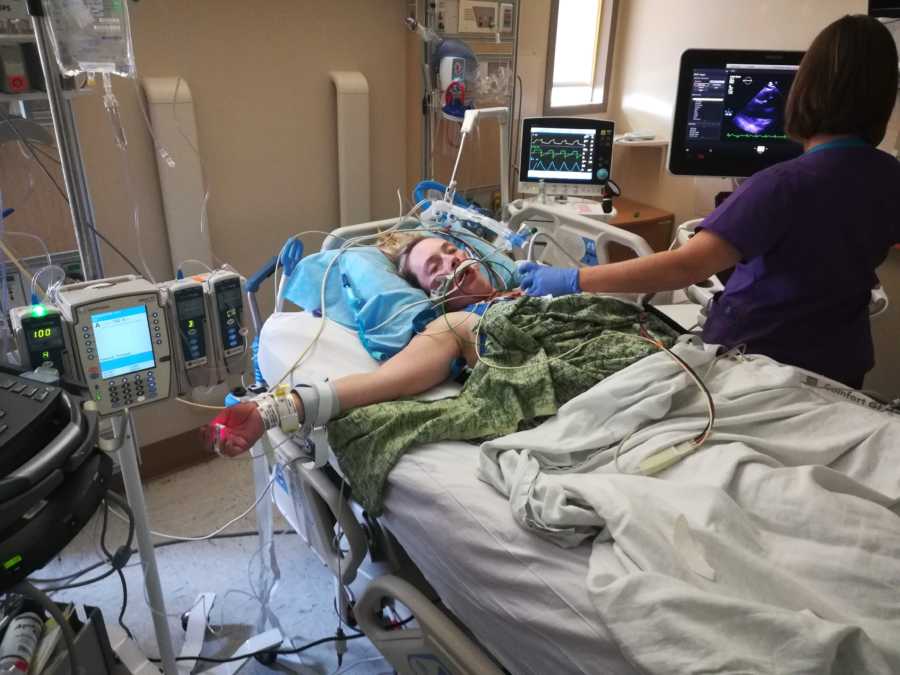
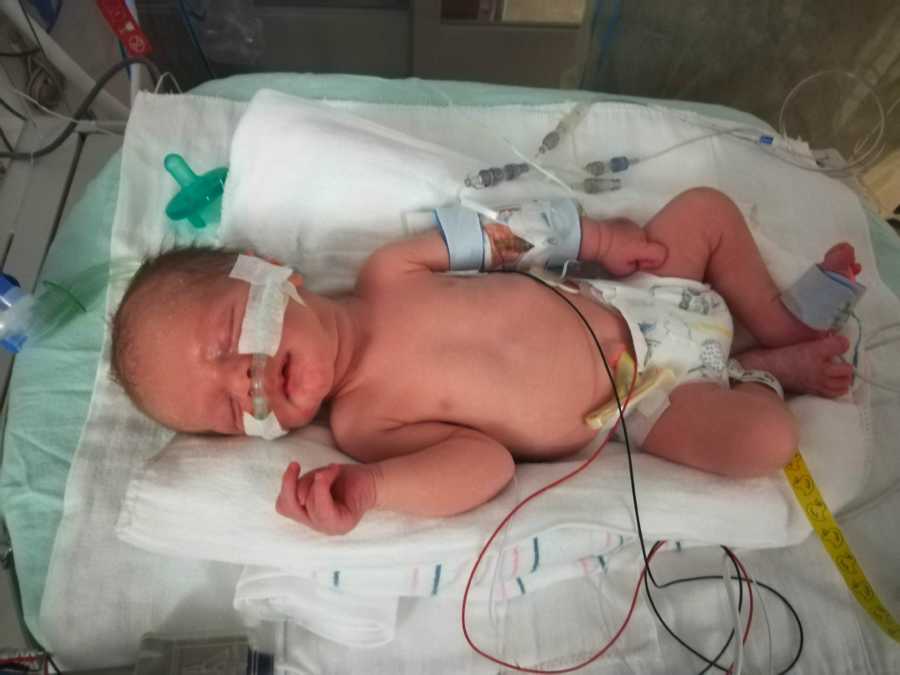
My husband managed this incredibly difficult time with so much grace. He visited me and baby Tommy every day, driving to two separate hospitals an hour away from home each way. He made sure our older two boys were able to maintain some sense of normalcy. He made sure they knew Mommy was in the hospital because she was ‘getting better,’ and did his best to make sure the stress he felt having his wife in a coma didn’t affect them negatively. Eventually he brought Tommy home from the hospital while I was still in a medically induced coma.

Due to the small size of the hospital we had gone to, I had been transferred to a larger one with better equipment. However, I was so unstable the transfer had to happen in under ten minutes. I was flown via helicopter to one of the best, most equipped hospitals in the nation, which happened to be a five minute flight. There, I was put in various beds to keep my body alive.

Being in a coma, particularly after having a baby, is extremely violating. I had urinary and rectal catheters, was being wiped frequently because of postpartum bleeding, and was having my breasts massaged frequently to prevent mastitis, which would add to the existing infections in my body. On top of that, I was being intubated and extubated again and again. My mind struggled, in its drug-addled state, to make associations for what was physically happening to me, and I remember multiple vivid dreams of violent rape and violations, and being drugged against my will.
After multiple failed attempts at bringing me off the ventilator and out of heavy sedation, I was finally able to breathe with the help of a high-flow canula. I remember being so thirsty because the air was blowing in my nose and throat with so much force, but I was on a feeding tube and wasn’t allowed to have any food or fluids.
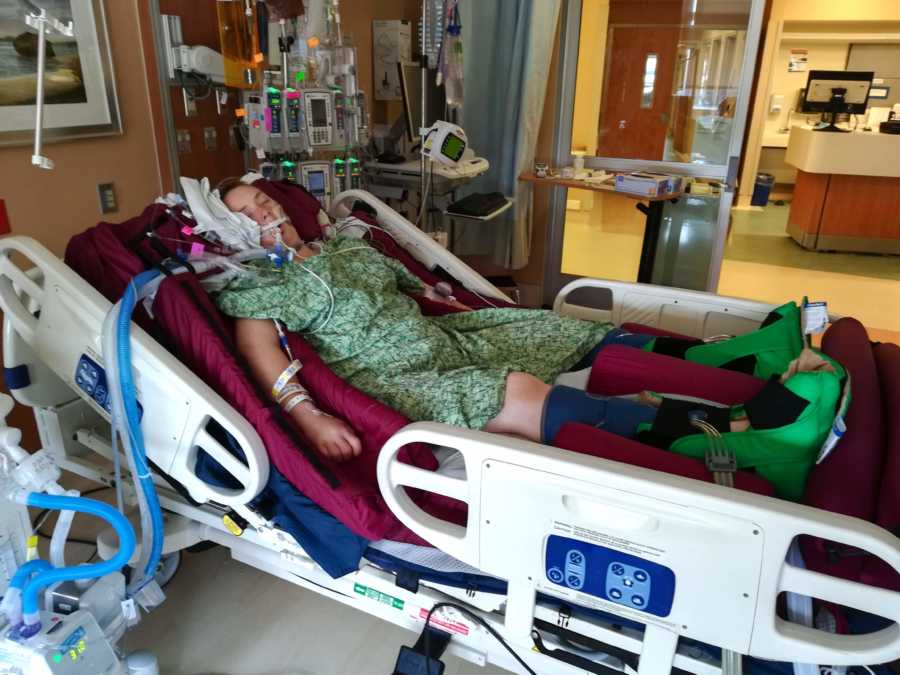
As I woke, my ‘dreams’ transitioned to reality, and at first believed I had been hospitalized for multiple rapes. I was relieved to be safe in the hospital, and relieved to feel the bump on my belly which meant my baby was still with me.
This is when the nurses told me, ‘You aren’t still pregnant, you had your baby 15 days prior, and have been in the hospital since.’ I couldn’t understand, and I thought my baby had been kidnapped from my womb, or had died. I truly believed I had been horrifically violated. Reality was so skewed, and it broke my heart as I tried to understand what had really happened.
After a couple days on the high-flow oxygen, I had started waking up more and was beginning to comprehend everything. But the air flow had become so overstimulating, I began breathing through my mouth, and started suffocating. I coded as my blood oxygen levels tanked. Quickly, I was re-sedated, re-intubated, and the decision was made to give me a tracheotomy. This procedure would allow the high-flow oxygen to flow directly into my windpipe, bypassing my nose and mouth.

The procedure was done, and I woke up the following day not knowing what had happened, only to discover I was completely unable to talk. I had a trach collar blowing air into my throat, which meant I was no longer uncomfortable or thirsty from the canula, but my vocal chords wouldn’t produce sound as long as I had a hole in my neck.
My lungs still had a lot of healing to do, but I didn’t need to be intubated or sedated once the trach was in. I began weaning off the heavy sedatives and pain killers (which caused all the crazy paranoia, nausea, shaking, muscle paralysis, and other side effects), and was able to learn about my baby. I was devastated I had missed those precious moments after birth during which we would have bonded. I was heartbroken I wouldn’t be able to nurse him. I wept and begged the doctors silently, ‘Please downgrade me out of the Intensive Care Unit so I can finally meet my baby!’ (Kids weren’t allowed in the ICU.)
After a few days that felt eternal, I was meeting milestones like crazy and was moved to a Progressive Care Unit where I could continue my recovery and FINALLY, after 24 days in the hospital, have my kids come visit me and meet my precious new son.
I was so weak I couldn’t walk, I still had my trach and couldn’t speak and I hadn’t showered in a month and didn’t have any of my own clothes so I smelled like hospital. I was so weak I could barely lift my pillow to make myself more comfortable. I still had a feeding tube in my nose and was being formula fed. And yet I was more determined than ever to recover as quickly as possible so I could be with my babies.
One day after moving to the PCU, my husband, mom, and dad were able to bring my baby to me. I cradled his tiny body, rubbed his soft, fine hair, and wept. I wished more than anything I smelled like myself, I could speak to him, sing him a lullaby. My smell and my voice were the two ways I knew I’d be familiar to him after such a long separation, and neither of those features were in working order. I laid him on the bed between my knees and took off all his clothes so I could inspect his perfect body. His cord had already fallen off. He was only seven pounds at four weeks old, and we hadn’t yet reached his due date.
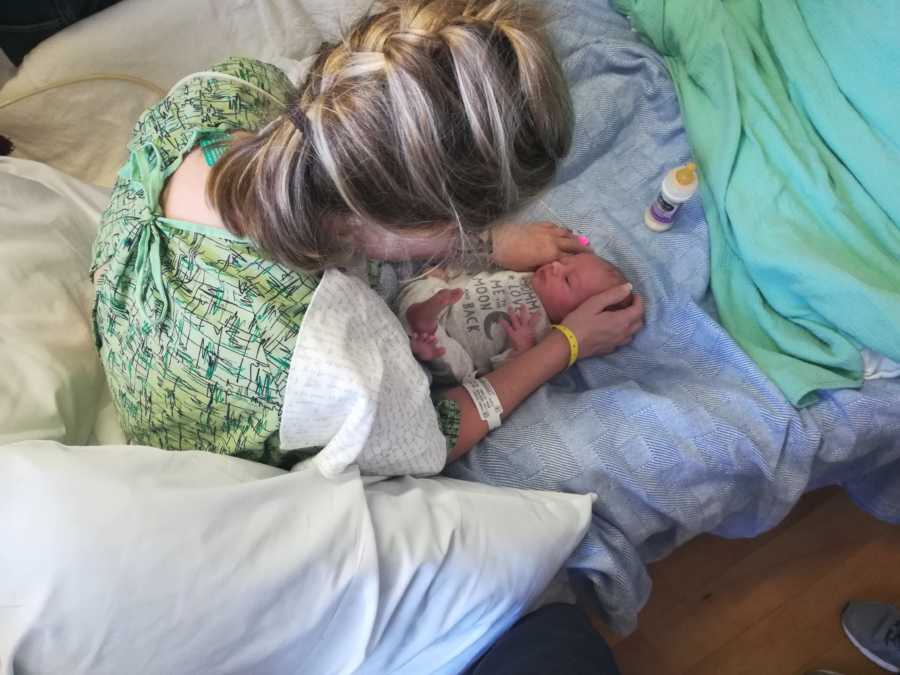
I fed him a bottle and smelled his skin, and cried while Alison Krauss sang ‘Baby Mine’ in the background. I had almost died, been separated from this precious life, and finally been reunited with him, and it was time for him to go home. I had to stay in my hospital bed, alone, while my family walked out with my baby.

The sorrow I felt was indescribable. And instead of letting it destroy me, I used it as a catalyst. I was so determined, by the touch of my sweet baby, to heal as quickly as possible. I would not be kept from him any longer.
Later that day, I became fixated on improvement. I asked the doctors what they wanted to see from me. Want to see me walk to the end of the hall and back? Done. You’re worried I keep vomiting up this horrible formula? Great. I want the feeding tube out immediately. I began to understand the degree to which I could control my own healing. I could advocate for myself, medically and also mentally. I wanted my voice back, in every sense. I requested my doctor come and remove my trach.
That night, the ENT came and removed it, and I was able to speak again. My spirits were lifted so much by this small victory! The following morning, a doctor came and spoke with me about my discharge options. He said, It looks like you will be able to leave the hospital in a week, but will probably need to go to a rehab facility for a few weeks to fully recover.’ The thought of leaving the hospital was thrilling, but the thought of weeks in a patient rehab center was bleak and depressing. I wanted to go home so badly.
Around lunch time, my family came back, this time with all three of my boys, and I was able to tell them how much I loved them and had missed them. ‘I am so sorry I had been sick for so long, and I am working so hard to come home and be with you.’ It was exhausting having so much energy in the tiny hospital room after a month of solitude, but it fed my determination to return home.
I was discharged finally with no medical equipment required except a walker to assist me around the house. I called my family, who had just gotten home from visiting me, and shared the good news. We were elated! My mom and dad drove me home and bought me a cheeseburger on the way, of which I could only eat about two bites. When I got home, my dad and husband carried me up the flight of stairs, and I couldn’t wait to begin the rapid process of strength-building. Being back with my little boys would heal me.

Once I was home, everything felt so surreal. I was overjoyed to be home with my family, to be free from the loneliness of the hospital. Had I really lost an entire month? My kids were jarred from such a long separation and sudden reunion with their mother, my husband was eager for things to return to normal (as was I), and I had a one-month old baby to start bonding with. I had hoped I would be able to re-lactate and nurse him. I had heard stories of women building up their milk supply after a long period of not nursing, and even of a woman who had never had a baby training her body to lactate. After the first day home from the hospital, I understood given how much radiation I had received in the many x-rays on my lungs, all of the medicines I had received, and my degree of weakness, it would be unhealthy for me to force my body to give even more of my already limited strength and energy to milk production, not to mention the risks of exposing my new baby to the radiation and drugs still in my system. I needed to focus on healing myself, and it was the right decision. I do think bonding was harder, but our long separation and my emotional resistance due to trauma had more to do with it than bottle feeding.
Of course, the general anxiety and absence of their mother did affect my other kids. When we were reunited after a month of separation, the boys were afraid. They weren’t allowed to visit me in the ICU due to the germ exposure to both the patients and the visitors, so they never saw me unconscious or with dozens of tubes, needles, and monitors attached to me. But once I was awake, recovering consistently, and moved to the PCU, they came to visit me and were nervous the whole time, as if I had become unfamiliar to them. I was thrilled to see them and wanted to hold them, but was so weak from weeks of bed rest I couldn’t lift them. They took turns sitting on me for short periods, and became restless in the little hospital room, so they ended up watching a show on someone’s phone for most of our visit, just so they wouldn’t be disruptive to other patients.
Now, eight months after the event, we’re finalizing all the cleanup efforts like follow-up appointments, additional health issues, and bills, and are focusing our efforts on emotional and mental healing. It’s been a long, hard process, but we’re so grounded in gratitude our family remains whole.
There are miracles in motherhood.”

This story was submitted to Love What Matters by Tess Frame of San Diego, CA. Follow her journey on Instagram. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more unbelievable stories of women beating all odds for their children here:
Please SHARE this story on Facebook and Instagram to encourage others to cherish every moment and love what matters most.

