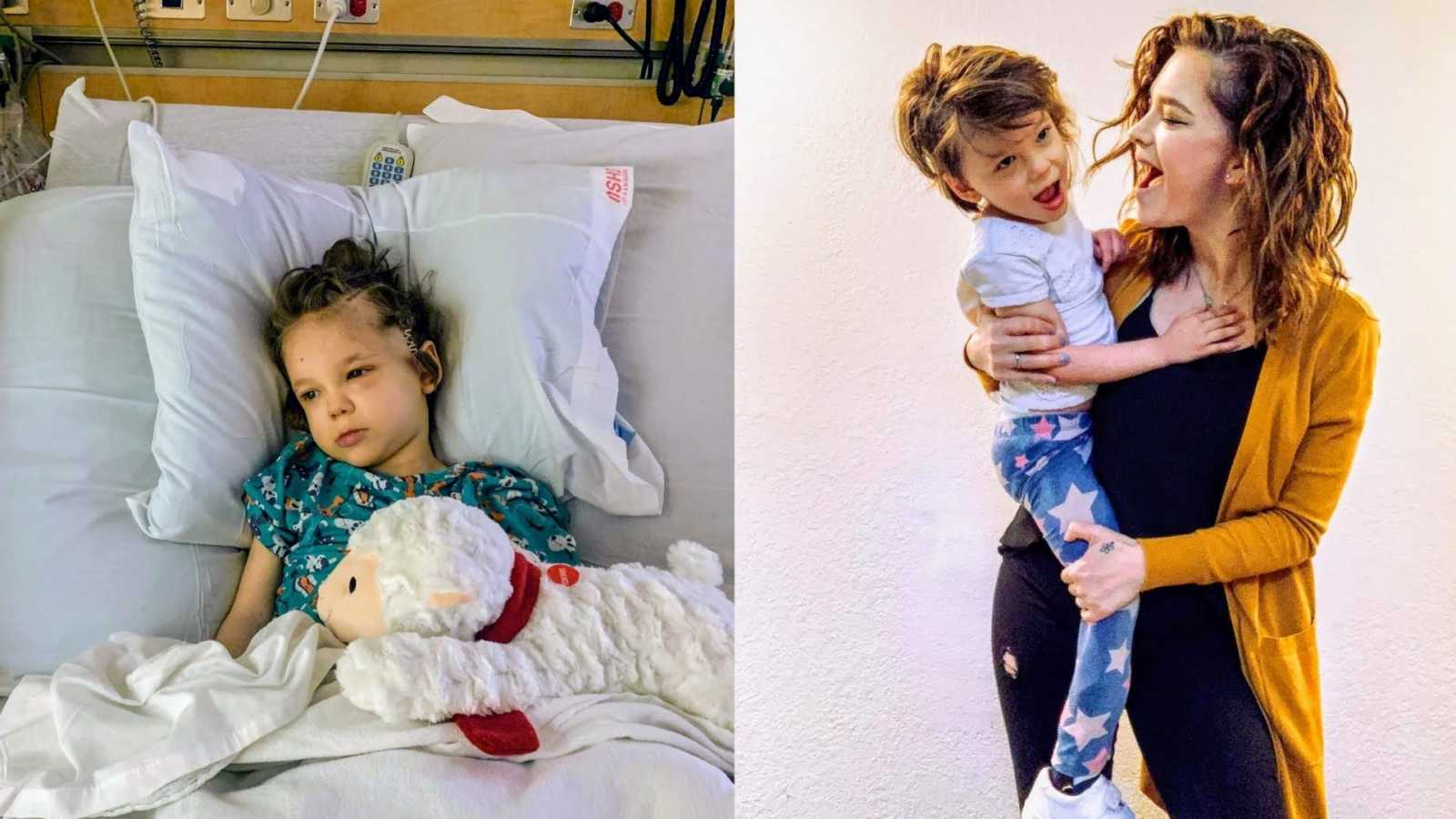
“Annebelle was born a perfectly healthy baby girl. She was 9 pounds, 2 ounces, and arrived at 41 weeks gestation with an uneventful delivery. We spent the usual couple days in the hospital post birth and then took her home. For four blissful days, I was a mother of two amazing, healthy kids. I was faced with the usual new parent woes, breastfeeding difficulties, and zero sleep.
Annie wasn’t adjusting well to breastfeeding and, honestly, breastfeeding her wasn’t as important to me as feeding her. So, we switched to a bottle. We were finally getting her to eat and take the bottle when her eating slowed again. After about 8 hours of not being able to get our five-day old daughter to eat, we took her to the emergency room.
We were assured that she was going to be okay and she was hooked up to the monitor. While sitting in a patient room for what felt like forever, I noticed her oxygen stats dropping. I pointed it out every time someone came to check on her, but I was continually told she was fine, that those monitors aren’t always reading correctly based on movement and other factors.
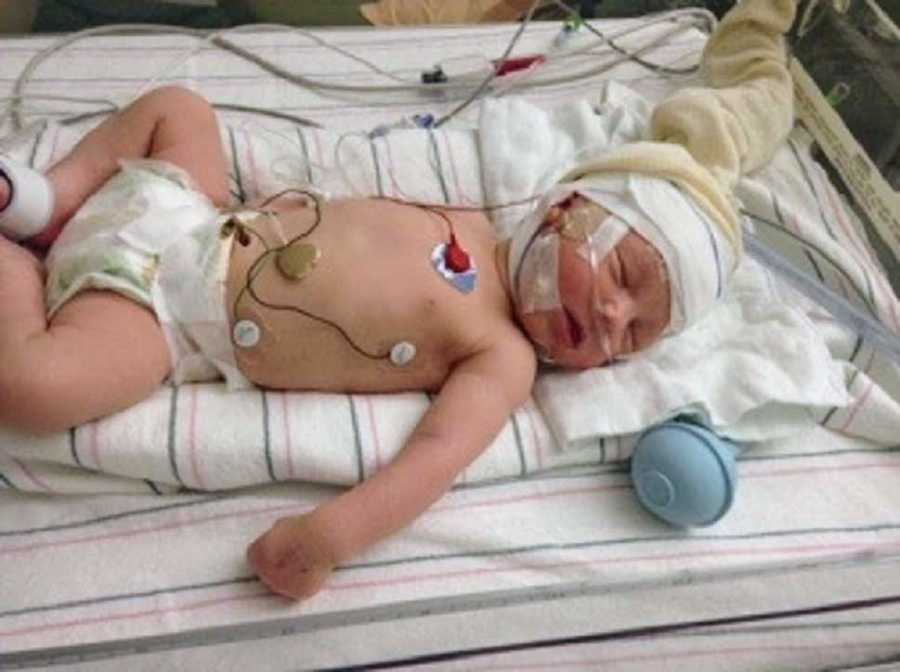
I pointed out that the monitors seemed to be reading correctly and that the waves were matching up with low numbers, but was still dismissed. ‘She’s fine,’ they told me again. The staff at our small military hospital couldn’t find what was wrong with her and were readying to send us home. Before we were sent on our way, they paged for a nurse from Labor and Delivery to give her an IV to run fluids.
The nurse, who I’m pretty sure is our guardian angel, immediately noticed her dropping stats and odd movements and knew she was having seizures. She told the ER doctor to call the nearest children’s hospital and prep us to be transferred to see a neurologist. I ran home while my husband stayed with her and quickly packed a bag in anticipation for a stay in the NICU. I kissed my two-year-old. ‘I’ll be back as soon as I can. I’m just going to go make sure your sister is okay.’
That day, Annebelle was diagnosed with Incontinentia Pigmenti (IP), an extremely rare genetic condition that runs through my family. I had not tested for IP during pregnancy and I had no idea how severe the disorder could affect someone. Annie did not show any earmark signs of the disorder at birth, so I naively assumed we were in the clear.
Incontinentia pigmenti is linked to many neurological disorders, including epilepsy. But because the disorder was so common among my family, and everyone had a relatively mild case, I never dreamed the havoc the disorder could cause. Along with neurological problems, IP also gave Annie blisters on her limbs and dark pigmented swirls that covered her body. Annie spent 7 long days in the NICU before her seizures were finally under control with medication. She was released with a diagnosis of IP and epilepsy, along with extensive damage to one half of her brain.
She was given a poor prognosis and we were warned. ‘She will likely be severely developmentally delayed.’ Have you ever seen a movie where someone gets devastating news and collapses down a wall crying into their hands? That was me. Her whole life flashed before my eyes. Her running and jumping and going to school and playing with her brother, everything I thought she would have and knew she deserved. Learning my daughter would likely be severely disabled was like a punch in the chest. I didn’t love her any less, I didn’t want her any less, I didn’t fight for her any less. But in that moment, our whole life changed.
She was enrolled in Early Intervention through the state and started occupational and physical therapy immediately. While working with Annie and with the help of her therapist, I noticed she had a weakness on her right side. Soon after, she was diagnosed with hemiplegic right sided cerebral palsy. She would have trouble using her right hand, crawling, walking, sitting, talking, and eating. She’d have trouble with speech comprehension and understanding the world around her.

She began seeing a therapist weekly to work on her gross and fine motor skills and help her learn and keep the skills she needs. We’re not totally sure why, but Annie also started having a food aversion. She had been switched from formula to real food and milk when, seemingly out of nowhere, she stopped eating. After trying everything we could think of and only getting her to consume approximately half a cup of yogurt or cottage cheese in an entire day, we talked to her doctor. They decided it was time for her to get a feeding tube.
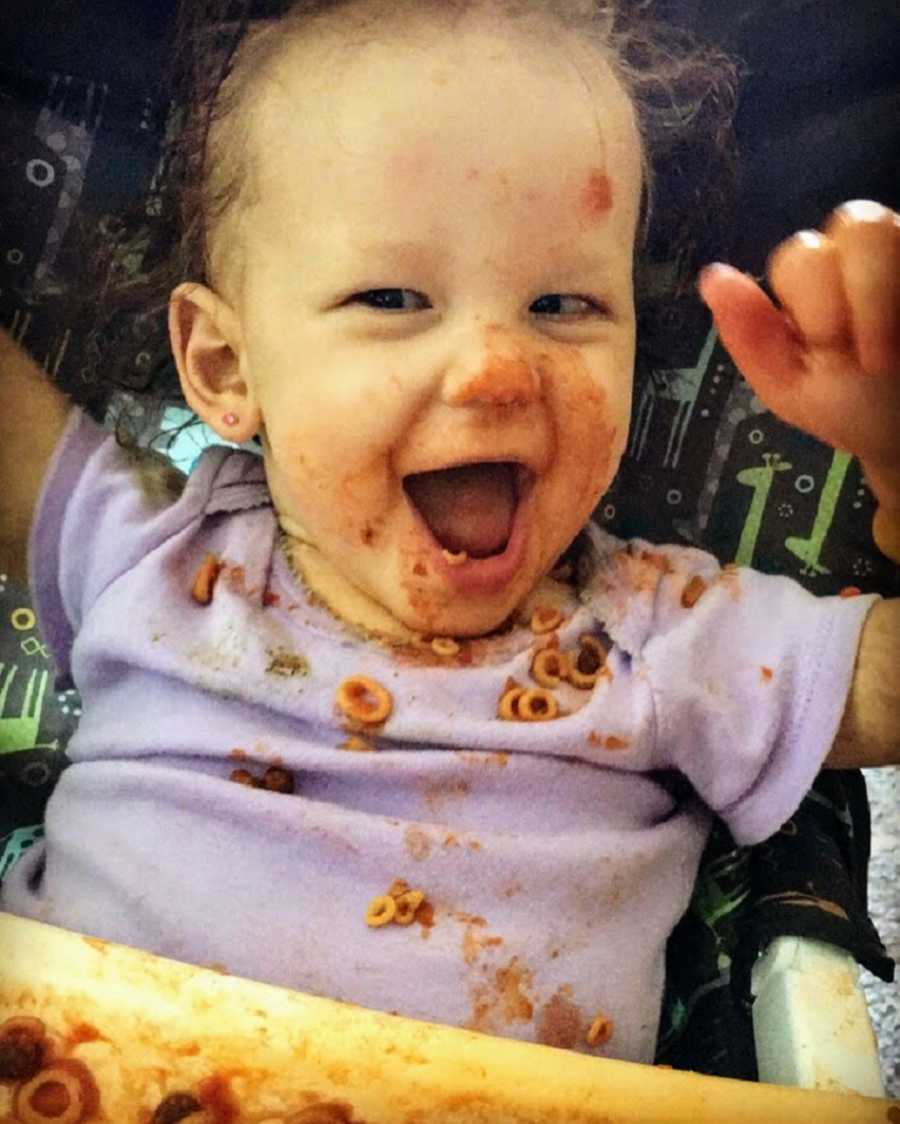
She went into the hospital in August of 2016 and got a feeding tube surgically implanted in her stomach. She has had that feeding tube for almost three years and it still gives her 100% of her nutrition and hydration. She has been working with a feeding therapist and we have our fingers crossed she will be able to get the tube removed one day. All of this occurred just one month into our new life as a special needs family.
In March 2016, a month before her first birthday, Annie was diagnosed with infantile spasms, a rare, catastrophic form of epilepsy. Infantile spasms consist of a physical ‘jackknife’ spasm as well as a hypsarrhythmia in her brain. It is harmful in the fact that it is continuously damaging her brain. She has gone through a round of steroid injections twice a day, followed by four anticonvulsant medications, and the ketogenic diet. None of them worked and her infantile spasms were wreaking havoc on her brain for a year, well over the limit for most babies.
When her infantile spasms finally stopped, it was like a weight had been lifted off our chest. The spasms had greatly affected her and every time she would make a small accomplishment in her development, her spasms would push her farther back than she was before. At one point, she lost everything she had learned. She couldn’t sit or roll or play. She laid on the ground, sometimes barely able to lift her head.
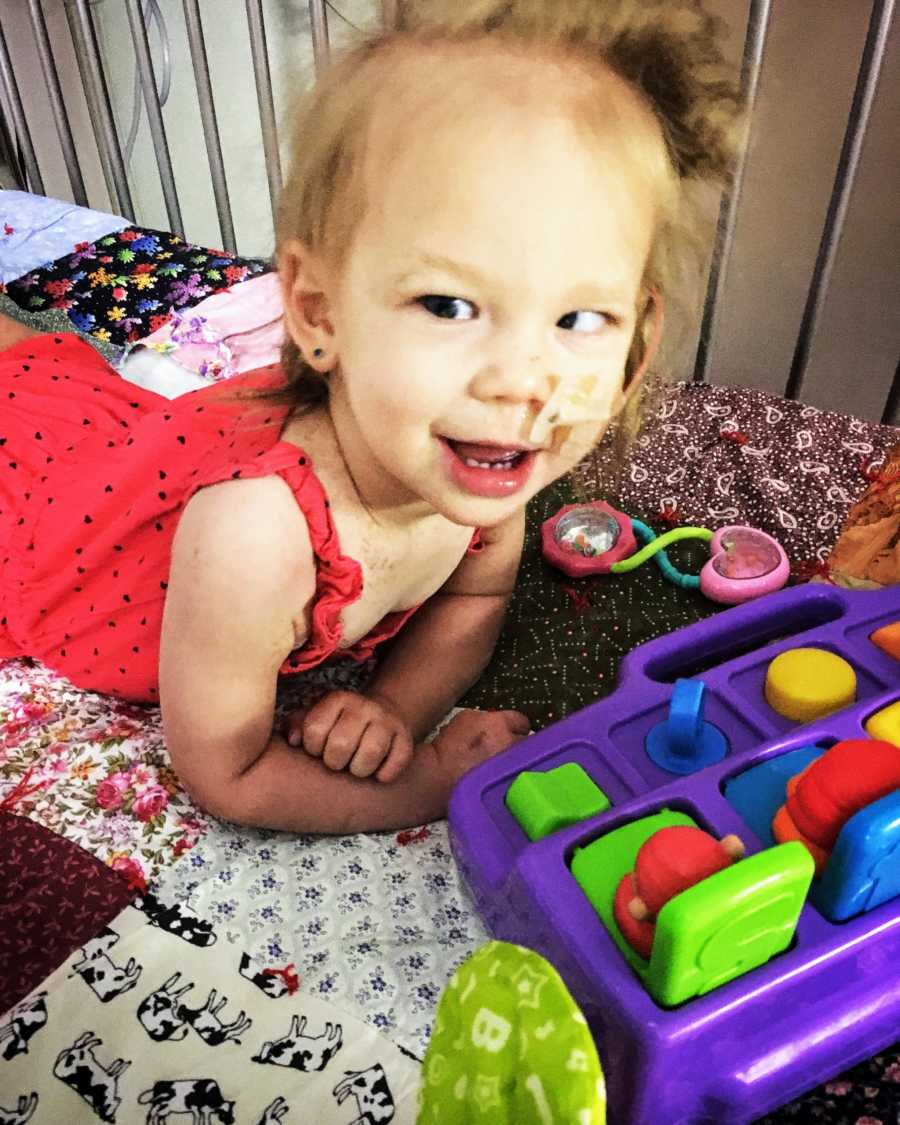
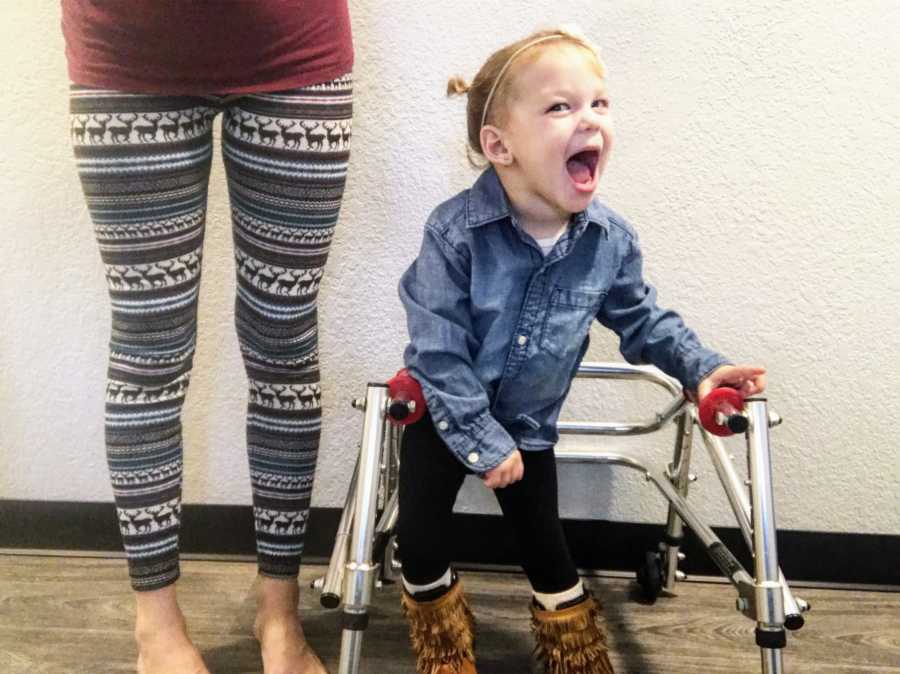
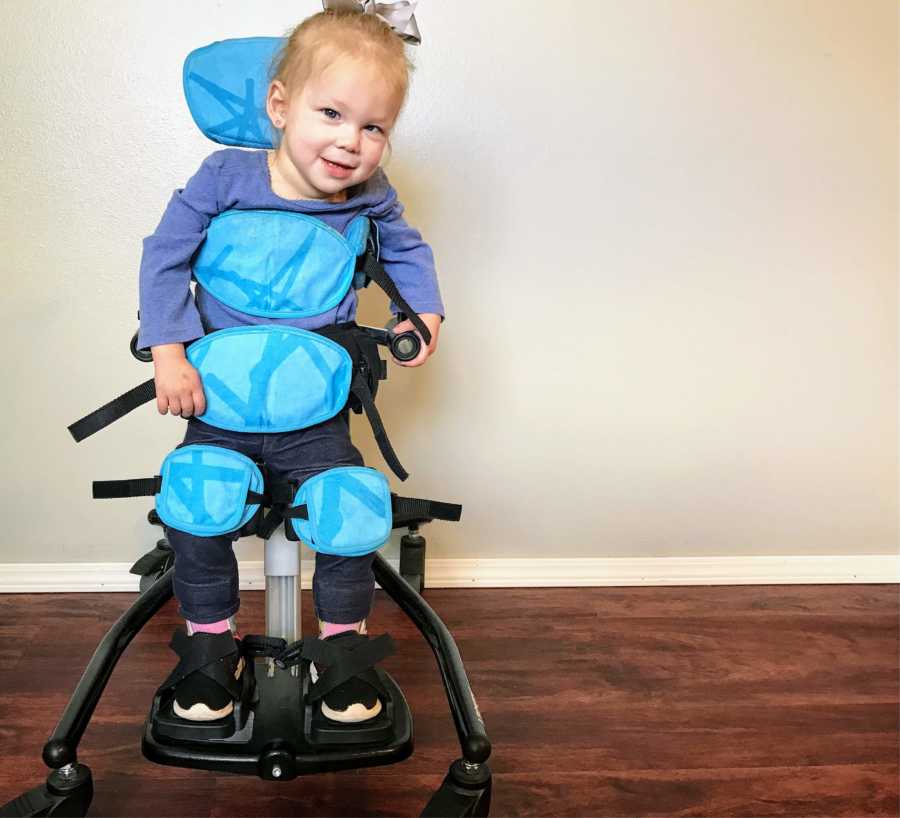
We had a blissful two months of seizure freedom. Experiencing seizure freedom as a mother was 90% happiness and bliss, and 10% constant paranoia that you might have seen a small seizure when your child made a funny face or simply moved their head in an abnormal way.
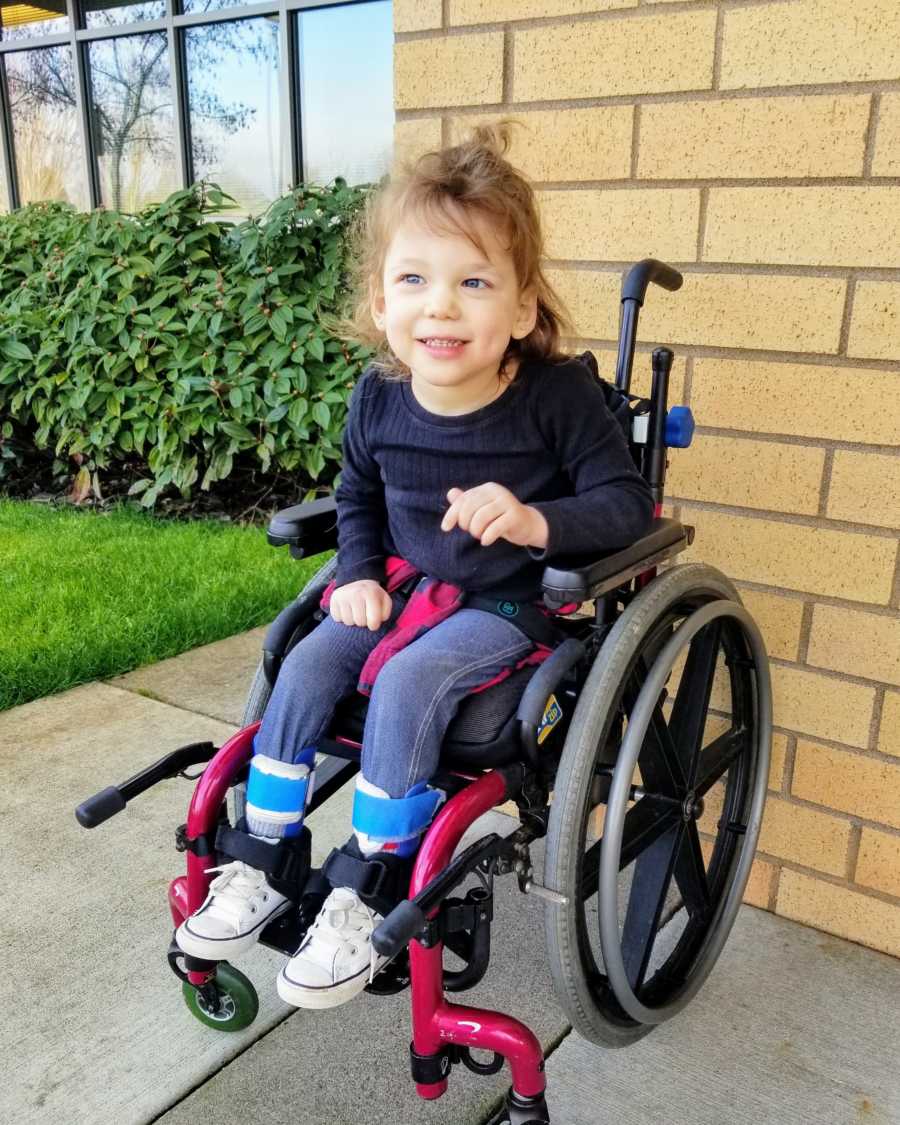
About two months after her infantile spasms were gone, I noticed her having focal seizures again, the ones she was diagnosed with at birth. I immediately called her neurologist and we hopped back on the roller coaster of finding medications that would work for her. Those two months were the longest she went without a seizure during her entire life. We spent the next two years trying every medication and therapy we could think of. Her seizures were getting more frequent, longer, and more intense. In March 2018, she was approved for a Vagul Nerve Stimulator, a small device implanted in the chest that connects to your vagul nerve to stop seizures.
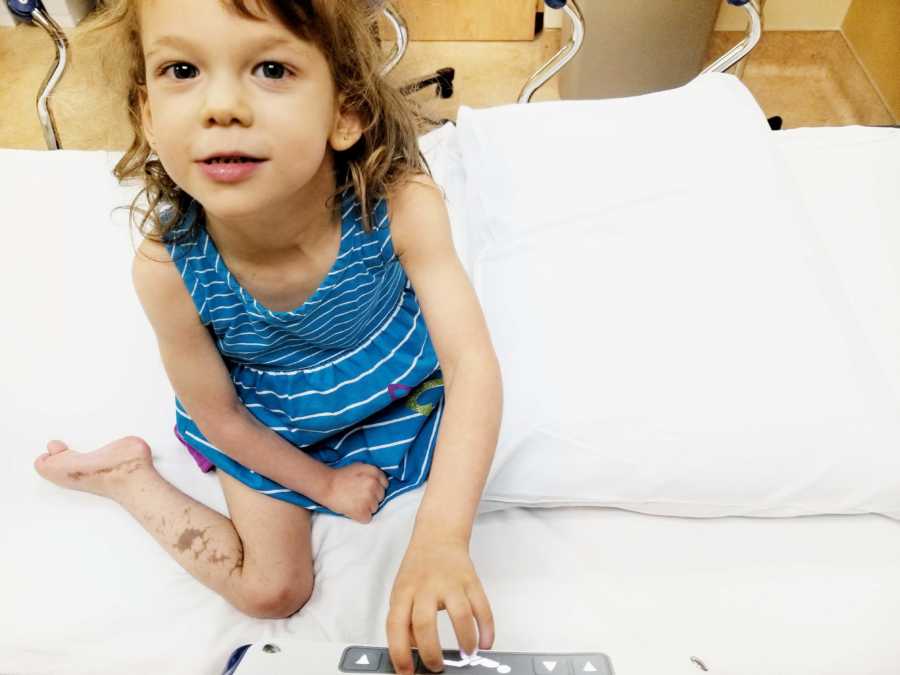
After months of checking and adjusting, we accepted the fact that the device was not working for her. She was still having multiple seizures a day and they were getting worse. Her quality of life was depleting and her development was regressing. At this point, her neurologist had brought up an extreme brain surgery to treat Annie’s epilepsy. But we knew it wasn’t curative so we dismissed the idea.
At the end of 2018, when Annie was 3.5 years old, her epilepsy was taking over her life. She was having seizures all day, every day. She was throwing up almost daily from her seizures. She lost her ability to speak the few words she knew and was officially considered non-verbal. Therapies seemed pointless. She was not able to absorb the information and would frequently have a big seizure and sleep through the rest of the session.
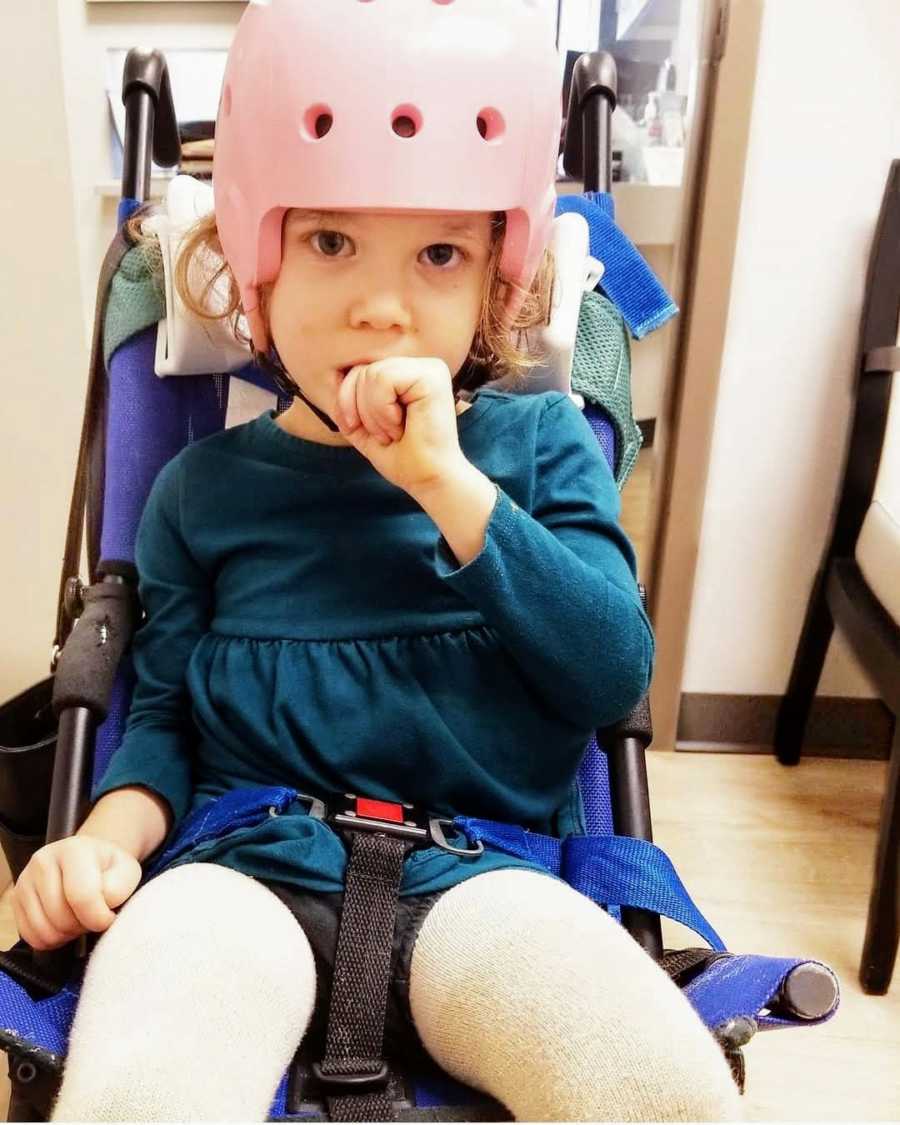
We finally decided to look into the surgery her neurologist had suggested. We had gotten to the point where her quality of life and risk of SUDEP (sudden unexpected death of epilepsy patients) were far scarier than brain surgery.
She met with her neurology team and neurosurgeon and was approved for the surgery. On April 6, 2019, Annebelle was admitted to the surgical floor and her amazing surgeons performed a left side hemispherotomy. During the longest 10 hours of my life, they removed most of her left hemisphere and disconnected what they did leave in. She spent four days in the hospital resting and recovering. She was pretty sedated and spent the majority of the time sleeping or quietly watching TV.
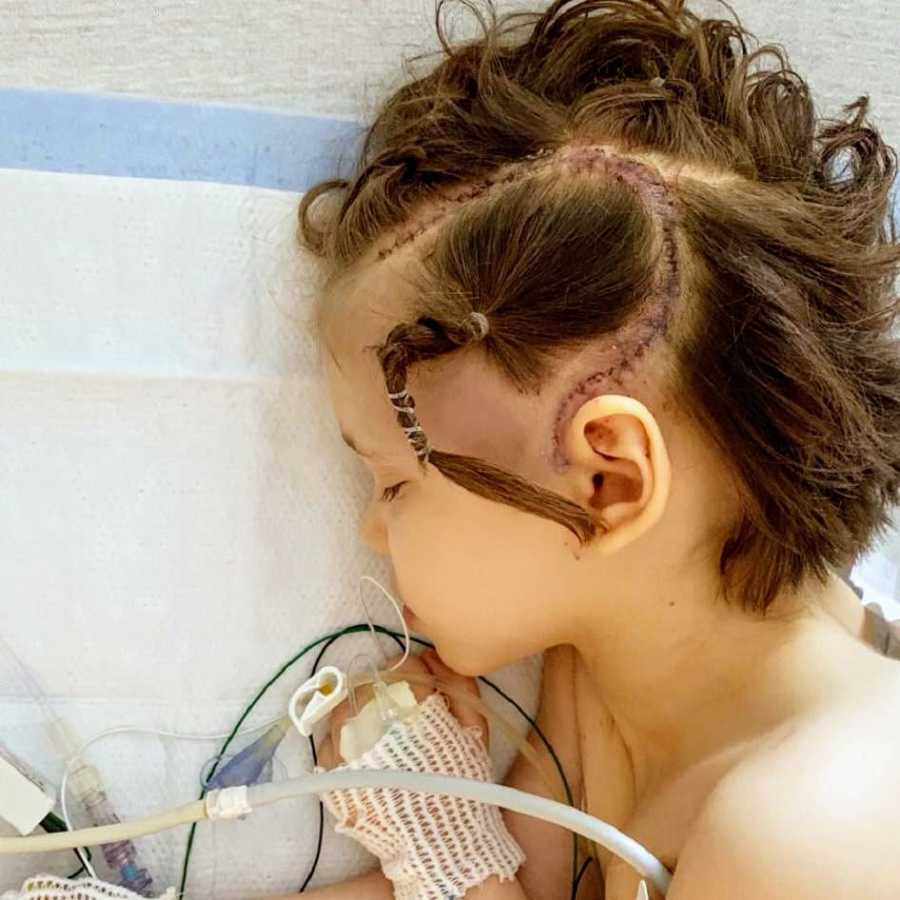
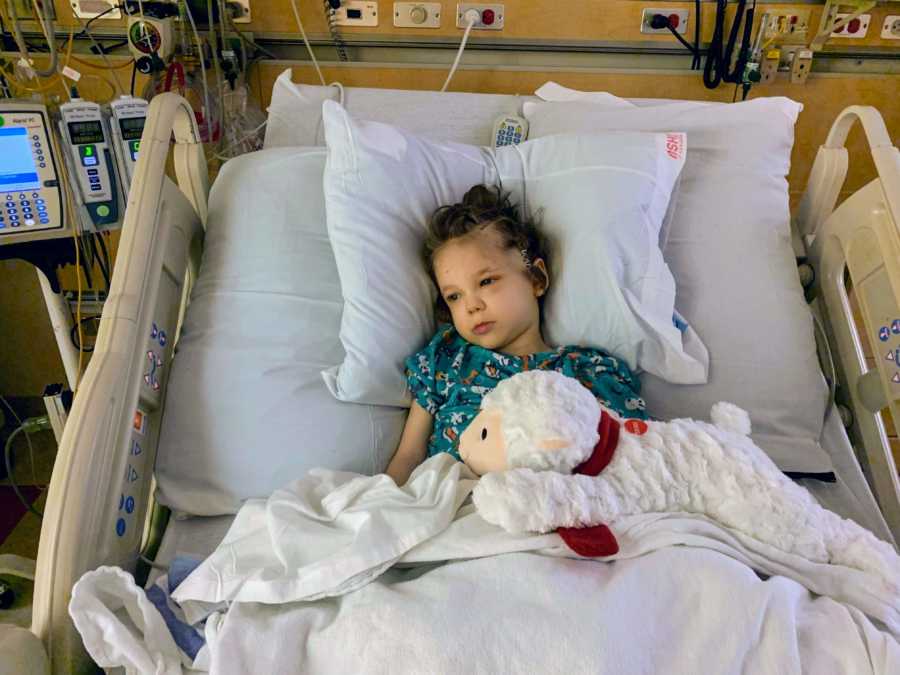
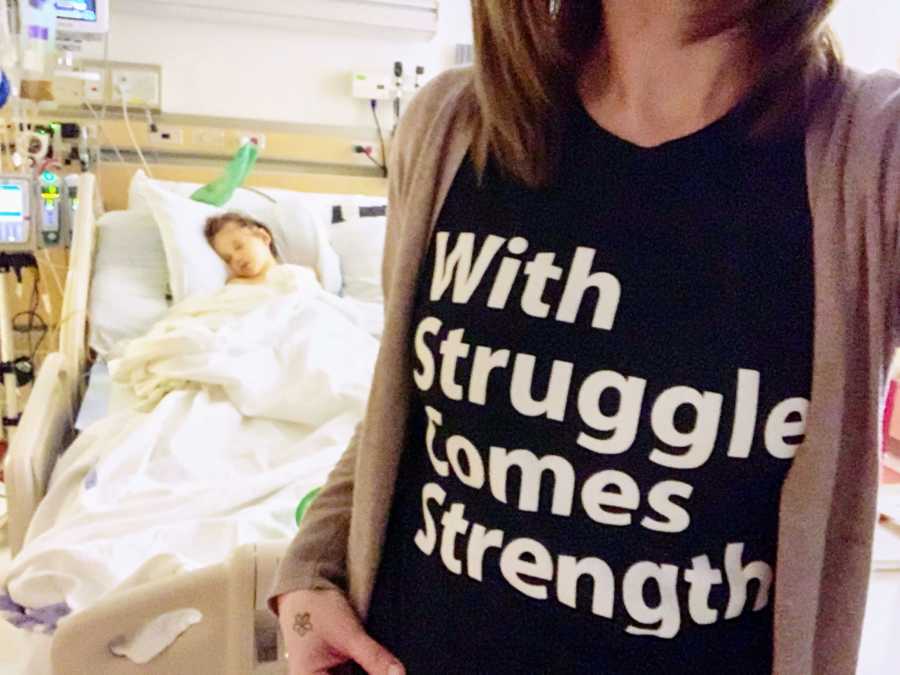
On the third day, I woke up and walked over to her. I was at a point where I hadn’t seen my child smile or look at me. I still didn’t know if she even knew I was in the room. Suddenly, she smiled and looked at me and said, ‘Hi.’ In that tiny little moment, everything she had gone through and every decision we had made for her was validated. My baby girl was coming back to me even though she had lost half her brain.

Over the next month she went back to therapy and settled nicely into her life at home. She has not had a seizure since her surgery. She is using her right hand more than before and is more vocal and babbling. She is more open to mobility and crawls faster than ever. She’s eating solid food and is brighter and more alert than she ever was. As it turns out, life with half her brain is exponentially better than a life with a full brain that is constantly throwing chaos around.
We still have a long way to go on her journey, but things are already looking up. This surgery opened doors for her that I thought would be forever shut. Her life is full of infinite possibilities and I can’t wait to see her explore all of them.”



This story was submitted to Love What Matters by Katie Ball of Our Disabled Life. You can follow her journey on Instagram here. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories.
Read more from special needs moms:
Provide hope for someone struggling. SHARE this story on Facebook with family and friends.