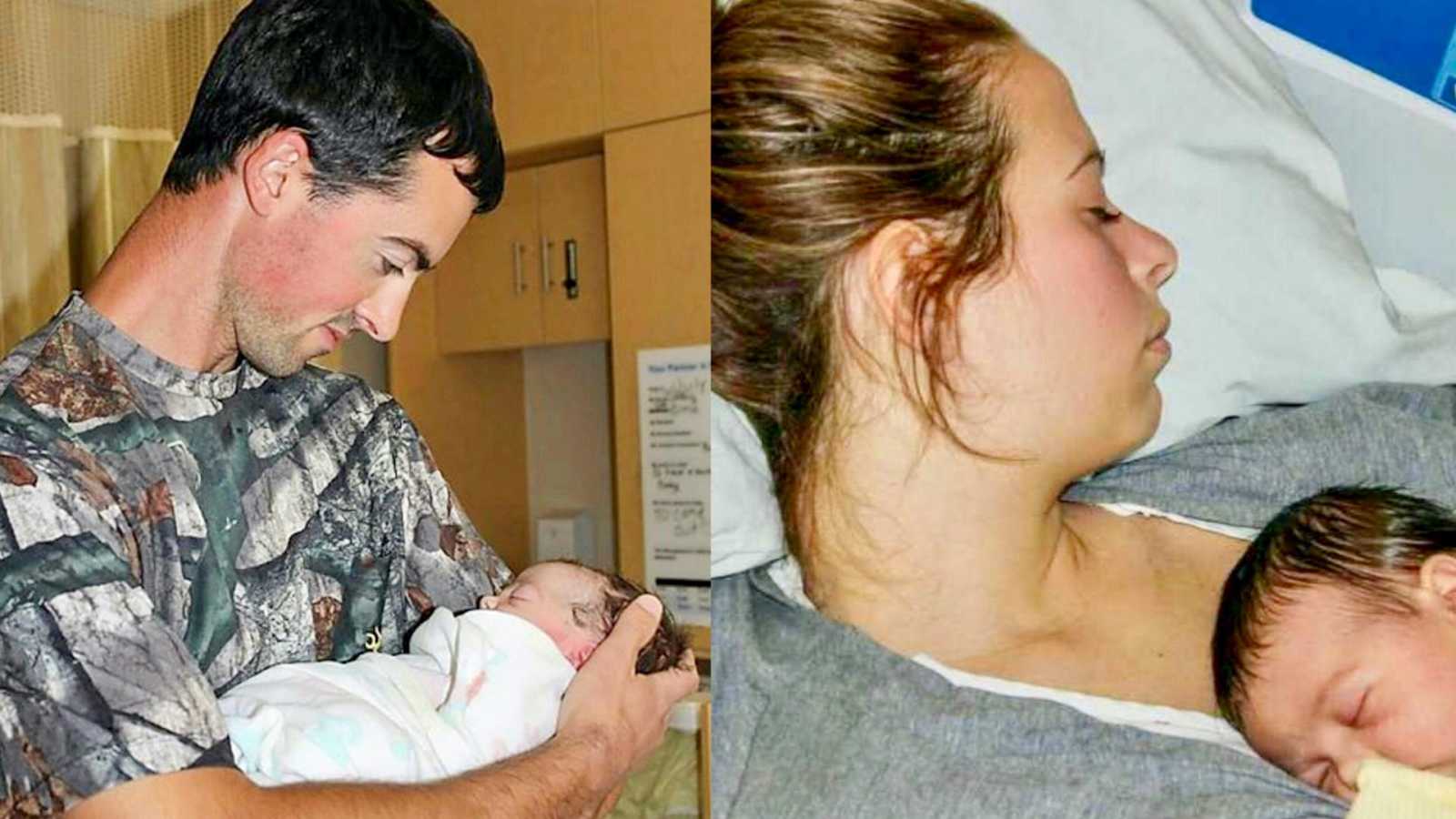
Read Amanda’s side of this story here.
“My feelings going into the last trimester of Amanda’s pregnancy were all good. I can’t recall ever being very nervous about having a child. Our family is fortunate enough to be surrounded by experienced and willing hands. I seem to have a ‘deal with the situation as it presents itself’ kind of attitude. I also knew I had an all-star wife who knew everything about babies, and she would be able to help me along the way. Everything in our lives was very stable at this point, with the exception of one big project. Amanda and I were dealing with the beginning stages of constructing our new home. 90% of my thoughts were focused on this, and Amanda seemed to be enjoying taking care of all things baby related. The pregnancy moved on, and the due date came and went. Finally, we were admitted to the hospital, excited to meet our child.
During the labor process, I was being told the progression was slow, but I didn’t know any different. I remember spending many nights on a small labor room couch, keeping my wife company. I watched Amanda try every trick the nursing staff could think of to get things moving along. Amanda ended up going through a rough delivery, which seemed to have changed her, forever.
Everyone who saw her within the first week of her delivery could tell her appearance and demeanor had changed. I felt as though the wife I knew had suddenly been placed on standby. Amanda’s laid out plans of being the best mom she could be were not ready for deployment. As her husband, I did not see any red flags, or that anything out of the ordinary was happening. I saw an exhausted, physically worn out, and scarred up woman who needed some time to heal. Time was my treatment plan at this point — to get her back on her feet and feeling comfortable again. Unfortunately, my treatment plan didn’t seem to help. As time went on, I saw Amanda constantly questioning herself. She would say, ‘Why am I like this?’ Amanda would be referring to her lack of connection with our child and her daily intrusive thoughts.
I struggled to have any clear memories of this time period, and I believe it is simply due to a prolonged stretch of a less than adequate amount of sleep. I still believed we did not need any outside, professional intervention. I was also quite distracted with the responsibilities of being up with the baby at night and then physically building our new home, all while continuing my full time job. The thought of my wife actually struggling with a serious mental illness never even crossed my mind.
The day Amanda told me she had thoughts of killing herself, I can truthfully say I didn’t believe her and didn’t perceive it as an accurate statement. I had always known my wife to ‘say a few things’ to get a reaction out of me. My treatment plan, at this point, was to get her out of the house and to find something to do as a distraction.
A few days had passed after her initial statement about suicide and not wanting our child. I found my wife in our bedroom, inconsolable and hyperventilating. That was when everything became more than just words. I could see it in her eyes — she would do anything she had to, to put a stop to all the anxiety and horrible thoughts she was having. She was undoubtedly in a very desperate moment, and I was feeling very helpless being unable to calm or comfort her. Along with the feeling of helplessness, I also felt embarrassment.
This part of my story is the most uncomfortable for me to say, but I believe is the most important. Mental illness wears a label, and for most of us that label reads ‘crazy person’ or ‘nut job.’ That was the label I put on mental illness, because I believed it was something completely fabricated in a person’s mind. I never considered the complexity of what the real labels for mental illness read. I knew the help Amanda needed was far more complex than what I could give her at home. She wasn’t safe, Molly wasn’t safe.
Amanda spent some time in confinement on a mental health floor and genuinely seemed to be doing better. After only one or two days, she told me she felt safe. I thought to myself, ‘How could she be so afraid of her own self?’ I later learned to understand, she was very much not in control of her thoughts and feelings. I began to understand through simple analogies that your brain can really let you down sometimes. I suddenly felt like I was taking my own mind for granted, and I would have never realized how all of us can be affected by mental illness. During our stay, even though I was starting to understand things, I would still question if all of this treatment was necessary. I would question the drug pushing by doctors and the uncomfortable therapy sessions. I felt like the doctors were able to treat typical anxiety/depression symptoms, but they seemed to be in unfamiliar territory dealing with some of Amanda’s problems.
Regardless, Amanda showed positive progression, and I felt like we were on the right track. I felt we at least had a treatment plan. When Amanda returned home, I can’t say I fully trusted her to be alone with our child. Some might say, that alone would be a hard thought to deal with. For whatever reason, I always thought things would eventually get better. The naive side of me would also think, ‘She could never do anything harmful like that.’ Fortunately, we had lots of help with watching our daughter, and we were able to help Amanda progress.
My feelings toward Amanda never changed. I saw her as an unwell person, no different than someone with any other illness who needed caring for. I never had any thoughts of creating distance between us to protect the safety of our child. After treatment and medication, we began to see some of the old Amanda come back, which gave us hope. We had a relapse one full year later, but almost felt as if we were prepared for it and knew what to do. Amanda was able to go back to a ‘safe place’ for a quick recovery. I can’t say this discouraged me, because we already had the answers to why it was happening.
The hardest emotions for me now are listening to Amanda retell her unfiltered thoughts of her past experience. What seems to get at a person sometimes are the ‘what if’ thoughts. I find if you are not careful, they can really overwhelm your mind. For me, attending Amanda’s therapy sessions has not only helped in her recovery, but I have learned some essential coping skills as well. I consider myself to be one of the most fortunate husbands involved in this illness. I credit most of our success to family, faith, and friends who helped share the stress and workload. I have gained lots of confidence simply through awareness this is a 100% treatable illness, and we are prepared if we are to ever see it return. Treatment saved my wife’s life, and helped our family become happy again.
What would I tell another father whose wife is struggling?
*If you wife is saying crazy, obscene things, try to remember it is not her. It is the mental illness. Be understanding, and know it will get better with help.
* Reach out to family and friends for support, and even reach out to a PSI Coordinator for local resources.
* Remind her every day how important she is and how great she is doing. Even the smallest sign of improvement, tell her.
* There may be a lot of trial and error when trying a new medication or therapist, and that’s okay. Stick with it.
*Educate yourself on your wife’s struggles, so you have more knowledge and are able to lend her more support.
* Pay attention to the little things she says, and do not be afraid to get help. No matter what kind of help she needs. Amanda’s stay in the hospital is what saved her life, and it helped her regain her strength, both mentally and physically.
* Be there for her. LISTEN when she speaks.
* Help her out with the baby, and encourage her to get some alone time every day. Encourage her to eat healthy snacks and rest often.
Our hope in sharing our experience is families are more aware of the symptoms of postpartum depression/anxiety and will seek help sooner than we did. We thought things would just go back to normal and suffering every day was normal. We are here to tell you it’s not normal, and the sooner you get the help you need, the sooner you will recover. ”

This story was submitted to Love What Matters by Amanda and Dan Brown of Hope for Maine Moms and Families. Follow Amanda’s on Facebook here. Do you have a similar experience? We’d like to hear your important journey. Submit your own story here. Be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read Amanda’s story here:
Read more powerful stories about postpartum depression here:
Do you know someone who could benefit from this story? Please SHARE on Facebook and Instagram to let them know a community of support is available.