“On September 14, 2012, our world forever changed. After struggling with infertility, several laparoscopic surgeries for stage IV endometriosis, and aggressive PCOS, we assumed our dreams of having a second baby were not going to happen. In fact, after my last surgery, I was informed one Fallopian tube was completely damaged and to pair that with inconsistent ovulating ovaries would mean that I had very slim odds. But, God gave me a Henry. To say our hearts were overjoyed was an understatement. When we found out we were having a boy, it was truly one of the happiest moments of my life. To realize how close I came to almost losing him and myself brings me to tears even to this day.

I noticed very quickly that this pregnancy felt different from my daughter’s. I was utterly exhausted, but everyone would remind me I had an almost 2-year-old, so…who wouldn’t be exhausted? I would share I was nauseous and not feeling well. Again, who wouldn’t be while pregnant? Due to not feeling well, I wasn’t eating much, but I was gaining a lot of weight and felt swollen. I was told since my daughter and I frequented the pool, I was most likely retaining fluid from that. I remember vacationing in Florida with our family the second week of August and waking up choking. I recall coming out into the family room and my husband and grandparents trying to figure out what was happening. It turned out I was choking on heartburn, something that was a regular occurrence. In fact, I couldn’t so much as drink water without having painful heartburn. When discussing this with providers in my care, I was told I could take something over the counter. Every symptom, dismissed as normal. In fact, I remember at one point someone saying, ‘You worried a lot with your daughter, don’t worry this time.’ To this day, those words haunt me because… what if? What if my story hadn’t ended the way it did?

Two days before his birth, I laid in bed aching from head to toe. I felt like I had the flu. Throughout my pregnancy I would see the PA filling in because my OB was in practice alone, so waiting over an hour was not uncommon. With a toddler, I tried to minimize that. However, my mom agreed to drive to Lexington and keep Ady so I could see my OB. I recall a nurse telling me after I expressed not feeling well, ‘Well you look pretty.’ My blood pressure was slightly elevated, not alarming in any way. But, for me it was very, very high. My OB asked me to lay on my left side and instructed the CNA to check it again. When it was still elevated, she ordered labs. I remember the difficulty finding a vein. After multiple attempts, she asked if I wanted to come back the next day. In that moment, as exhausted as I was, I remember pausing before answering, and then thinking she had to draw them. I didn’t have energy to come back later.
After a very painful and ill night, I decided to call the office the next morning. Something was still very, very wrong. I had taken a shower and just felt the Lord telling me something was wrong. After a few minutes waiting, the receptionist retrieved my labs and uttered 10 words I will never forget, ‘Baby, it’s not good. You need to get here now.’ I knew I hadn’t felt Henry move. I knew I was sick, but nothing could’ve ever prepared me for what was happening. My sweet PA friend, Paula, was filling in that day for my OB’s office. She called me on the way to the hospital and calmed me down, letting me know I would be having Henry that day. When my husband and I arrived at the hospital, the high-risk ER OB met us there. That’s when I knew something was really, really wrong. The lights were off in my delivery room, and the numerous questions I asked were not answered. I do not remember anyone actually explaining what had happened. But, I do remember hearing something like, ‘Yes, that pre-eclampsia and HELLP Syndrome’ are scary. I didn’t actually ever understand what had happened. When my water was broken, it was all blood. Paula’s intuition to request I not have a C-section, most likely saved my life. I would’ve probably hemorrhaged to death. The excruciating pain I was in allowed them to agree to an epidural, despite my tanking platelets. I firmly believe God wrapped His angels and arms around me and my baby boy to protect us from further harm.
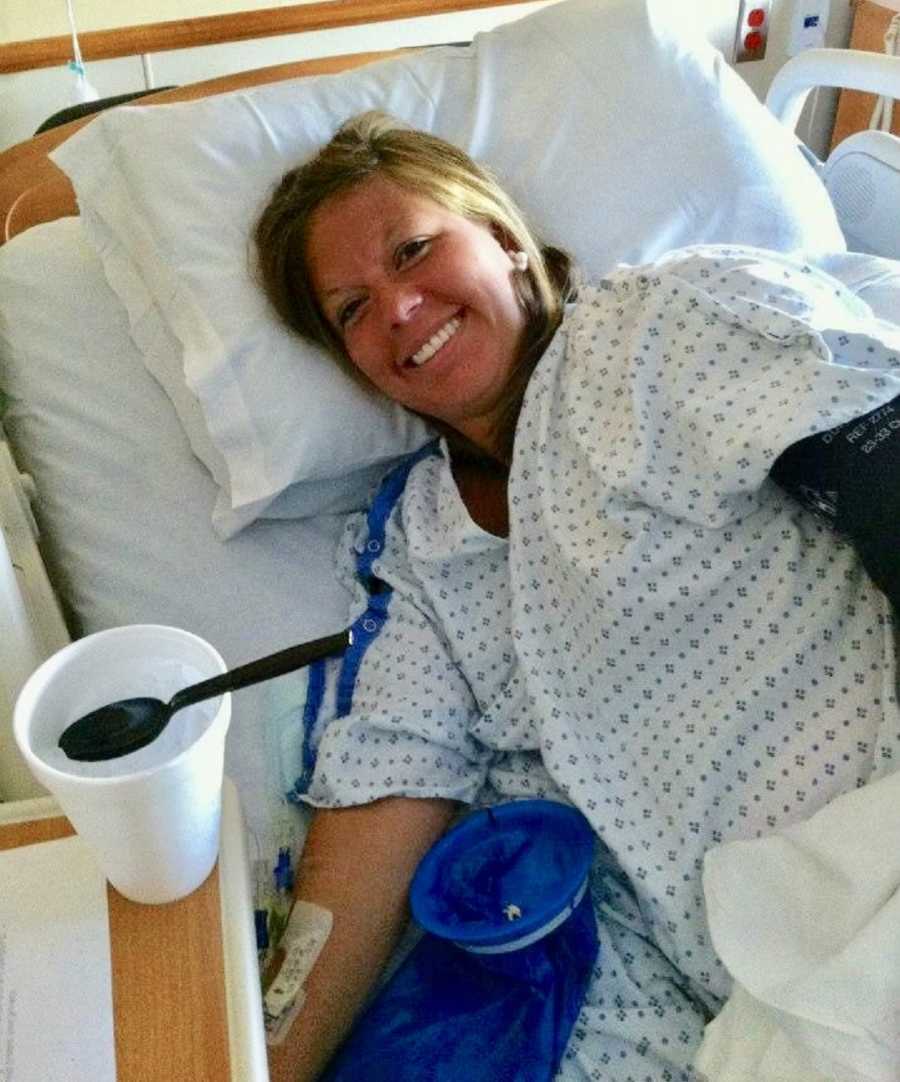
I really questioned throughout my pregnancy how I could love Henry as much as his sister, Ady. As it was time to deliver him, I noticed a lot of people in the room. I was so sick, but I knew something was seriously wrong. The nurse brought me an oxygen mask. In that moment, I remember thinking, ‘I’m not going to die, not today!’ and I fought off the mask. My mom took my hand, came to my bedside, and said, ‘It’s not for you, it’s for Henry.’ I grabbed the mask and rallied. That was the moment I knew I loved him as much as his sister. When everything else in my body was failing me and beginning to shut down, I pushed two times and fought to keep him alive. Miraculously, he was a healthy and perfect 36-week-old little boy. My hospital stay was far from over.
Throughout the course of the next week it was a battle to keep me on the magnesium sulfate, keep my blood pressures down, and me from seizing. There was not education on what had truly happened to me, but one thing is for certain, the hospital team was exceptional. I’m grateful to have had access to care, but many women are not as lucky as I was.

Over the course of the last 6 years I have stayed exceptionally quiet about my story. I felt since I lived, and Henry did too, there was no reason to share. In fact, not long after this ordeal happened someone said to me, ‘Well, God is good, you’re here.’ Yes, He is good. And yes, we are both here. But, what we experienced was trauma. I wish I had been better educated to understand the emotional implications of having this birthing experience. Having your motherhood stripped from you from a full hysterectomy in your 20s to keep you alive, and bones that are of an 80-year-old woman today due to it, and high blood pressure medication for life, are wounds. Deep, deep wounds.

Throughout the last two years, being involved with the USA Today investigation on the rising maternal mortality has done more healing for me and my family then we ever imagined could be possible. The reporter who videoed my story loved it so much, she asked to come back and spotlight our family in the front page of our local newspaper. From that, I was asked to come into the studio for a Facebook live interview. I attended the Champions for Change Summit with the Preeclampsia Foundation last weekend with my husband and a hundred other women. I learned from them, grieved with them, and cried with them. I learned that although some of the details were different in our stories, we had a common bond to forever unite us.

I am working with the director of government affairs with AWHONN to take a bipartisan bill to our Senator to create Maternal Mortality Review Committees. I am honored to play a small part in this change. I will be attending a Maternal Health Fair next month to get involved in the Kentucky Perinatal Association.
I am eager to take the scars and wounds, and turn them into stars and change. I refuse any longer to stay complacent and focus only the good news of our story. Yes, on paper it ended well, but emotionally it did not. And what if? What if my doctor hadn’t drawn labs? What if I hadn’t called that next morning? What if?


The United States is the most dangerous place to have a baby in the developed world. This is not okay. We owe it to ourselves, our daughters, and those we have lost to fight until it is the safest place. Women need to feel safe to use their voice when something feels wrong. Providers and all involved staff need to be educated. I have been a childhood educator for over 10 years. Why is there not education and someone to partner with hospitals and women during this crucial time? Aren’t mother’s lives worth it? I remember being told my condition was ‘rare.’ When you stand in a room of 100 other women who are ‘near misses’ and you all grieve and carry the same scars, you learn it is most definitely not rare. In fact, 700-900 women a year are dying and 50,000 are like me, ‘near misses,’ who by the grace of God, are here to share our stories.

I will never take for granted the gift I have to be here: to take my children on vacations, to go on field trips, to snuggle them. All of these things I nearly missed out on being a part of. Every night when I watch my little Henry’s lungs move up and down in his chest long after he has fallen asleep, I thank God for keeping me here. I was made for more than a published article. I will fight until my last breath to keep every mother alive.”

This story was submitted to Love What Matters by Bekah Bischoff, 32, of Louisville, Kentucky. Have you experienced something similar? We’d like to hear your journey. Submit your own story here, and subscribe to our best stories in our free newsletter here.
Read more stories like this:
Provide hope for other struggling mothers. SHARE this story on Facebook to help spread awareness.

