“I always thought I would get married, have kids, and have a lovely, but ordinary life. But, by the time I turned 30, nothing had really worked out as I had planned, so I decided to embrace my independence, and moved across the country on a whim. This is when, because I wasn’t looking, I met my husband, and all my dreams started to fall into place like magic. We built our dream house in the country, got married in our backyard, and nine months later, our daughter Chloë was born. A couple of years later, we decided to have a second child and complete our perfect family.

At 12 weeks pregnant we traveled to the IWK Health Centre in Halifax, which is three hours from our home on Prince Edward Island. We had gone for a similar assessment for Chloë, based on my age during the pregnancy, so we knew what to expect. When the nurse and the doctor performing the ultrasound became quiet, I wasn’t immediately worried. When they asked us to wait in a consultation room as they found some bloodwork results sent from my doctor at home, I remember telling my husband, ‘I think something is wrong with the baby.’
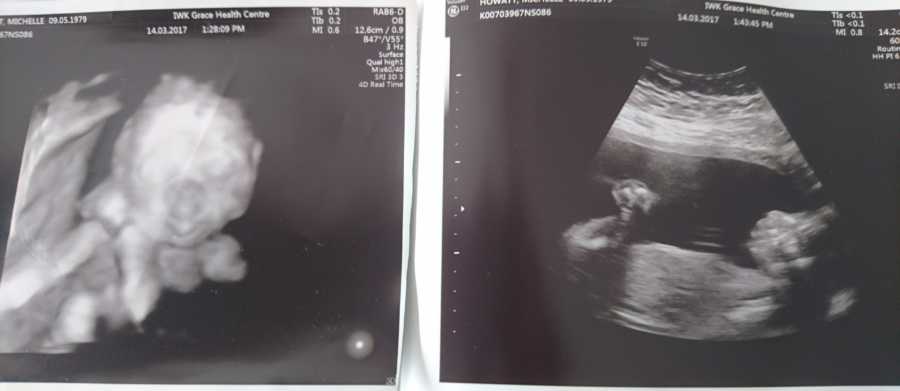
Our baby was measuring an above average nuchal translucency, which is a measurement of fluid at the back of the neck. The doctor said it was a flag, but not definitive. ‘It could be something, it could be nothing.’ The most common reason was Down syndrome. She said if we wanted, we could book an amniocentesis for a definite diagnosis, but there would be a small risk of miscarriage, and I was hesitant to risk the pregnancy without more information. She said we could get a non-invasive blood test done that would, again, not be definitive, but would do a more in-depth screen of potential abnormalities, and we could go from there.
That was the beginning of our roller coaster ride.
The blood screen came back showing increased risks for three different chromosomal defects including Trisomy 21, which is Down syndrome. Trisomy 21 was in fact our best-case scenario, other than no defects at all. I remember I got the call with the results while I was at work. After I hung up, I was in shock. I stared at my computer screen for about 30 minutes before I decided I needed to leave. Nobody at work knew I was pregnant except my supervisor, so I went to tell him I needed to go home. I was barely holding myself together, but managed to say, ‘I just got some test results about the baby…and they’re not good,’ and then I completely fell apart.
I was heartbroken. I called my husband and told him to come home, then I cried for 3 hours straight until my eyes were so swollen they hurt. We had obviously discussed the possibility of this situation, and we had already agreed the test results would not change our desire to continue with the pregnancy, but there is a world of difference between theoretical discussions and the very real possibility that your baby might not survive the pregnancy, and if they do, will have special needs. We decided to go ahead with the amnio because I could not handle not knowing if my baby would at least survive.
We made an appointment for an amnio in Halifax. However, our wonderful fetal assessment doctor knew I really wasn’t comfortable with the amnio. So, instead we did a super in-depth anatomy ultrasound, as the more serious defects would have obvious physical markers. Our ultrasound was perfect: 94th percentile for growth, limbs all perfect proportions, visible nasal bone, etc. Organs looked perfect, but because of the blood screens, she was going to send us for a fetal echo to check for heart defects. We were all ecstatic. Our doctor kept printing ultrasound pictures for us to take because everything was so perfect. She cautioned there could still be issues not detectable by ultrasound, but we felt we had at least ruled out the life-threatening ones. She hugged us as we left.
The relief we felt is indescribable. I remember thinking it would all be some crazy story to tell our baby when they grew up.
However, two weeks later we had the fetal echo, and it showed our baby had multiple complex congenital heart defects: Tetralogy of Fallot (ToF), complete atrio-ventricular septal defect (AVSD), and a right aortic arch. The cardiologist we met with drew us diagrams explaining what each one meant and mentioned the AVSD was specifically common with kids with Down syndrome. He explained that the baby would require at least one open heart surgery within the first year, possibly more. He stressed that while they were serious defects, they were treatable; he said the baby would likely not be running any marathons but would have a good quality of life.
It was all completely overwhelming; neither myself nor my husband knew anyone with severe heart defects. And yet, we felt ridiculously optimistic as we left our appointment. We naively thought that heart defects are ‘fixable.’ We thought the heart defects were the reason for all the abnormal blood screens; maybe the baby would still be ‘normal.’
Six weeks after our ‘perfect’ ultrasound, at 28 weeks pregnant, we went back to Halifax for a check-up, except this time, it wasn’t perfect: The baby had stopped growing. He (or she) was not getting enough blood flow from the umbilical cord and was now only 3rd percentile for growth. The doctor said, ‘We need to admit you. Today.’ She said we would be lucky to get to 32 weeks, more likely it would be around 30.
So, I was admitted to the hospital on modified bedrest (which means I could walk to the bathroom), three hours from home, three hours from my not-quite-two-year-old daughter, with little more than the clothes on my back, and no idea how long I’d be there. My husband did an emergency run to the store to get me some essentials, and then went back home to celebrate my daughter’s second birthday without me; I was gutted I wouldn’t be there for her special day.
I had ultrasounds every other day and was hooked to a fetal heart rate monitor twice a day, along with blood pressure. I remember every day when they would take me in a wheelchair to the ultrasound room, I would be shaking like a leaf, terrified the doctor would say they would need to take the baby today. Every day inside me, was one day safer. I met with one of the neonatologists from the NICU who explained what I could expect after the baby was born. I had never even heard of a neonatologist! Everything was so overwhelming, and all I could do was try to stay calm, and pray my husband was able to make it back before the baby came.
Five days after I was admitted, my husband left our daughter with his parents, and came to stay with me until the baby was born. He didn’t have to wait long… That night, my blood pressure spiked dangerously high. They decided to move us to a Labor and Delivery room ‘as a precaution’ where they could monitor the baby better, as well as my blood pressure. Around 4 a.m., they started a magnesium sulfate drip on IV ‘as a precaution,’ which they give to pre-term babies to reduce the risk of brain damage during delivery. Now I’m terrified, hooked to an IV in a massive, darkened birthing room in the middle of the night, a blood pressure cuff inflating on my arm every 15 minutes, drifting in and out of sleep, as my husband also nods off every couple minutes in an uncomfortable looking chair across the room.
Around 8 a.m. a team of doctors and nurses came in — the baby was moving less and less, and it was time to take him out by C-section. I nodded, not trusting myself to speak, and they started talking amongst themselves about what needed to be done. I will never forget a resident who turned from the group of medical staff, put his hand on my shoulder, and asked if I was okay. I dissolved into tears, unable to say anything; I was so scared our baby was going to die.
The birth itself is kind of a blur, but I remember there must have been about twenty people in the room. When our son was finally born, someone said, ‘He’s out!’ I saw a flurry of movement as the NICU team hurried to stabilize him. He was intubated (a breathing tube) right away, so there was no cry, and he was put directly into an incubator to avoid being overly handled. He was 1lb 13oz, 13 ½’ long. They wheeled him over to me to see before they took him to the NICU, and all I remember was saying, ‘Oh, he’s so cute,’ and then he was gone. My husband stayed with me, holding my hand until I got to Recovery, and then he went to check on our son.
I remember being wheeled on the bed from Recovery to my new room on the Newborn/Family ward, going past rooms full of families celebrating their new babies. Balloons, flowers, laughter, and newborn cuddles everywhere, and yet here I was being wheeled to a room with no baby, no balloons, no flowers, and definitely no laughter. I had never enjoyed being pregnant, but right then, I felt so cheated. There would be no celebration for the birth of our son, there would be concern, prayers, and an incubator between us. It felt so unfair, and I cursed my body for failing to keep him safe. This tiny helpless baby with a defective heart, and now he would also have to fight a premature birth as well.
Later, when the drugs had worn off enough to let me move from bed to wheelchair, my husband came to take me to see our son. We decided to name him Mason, which means someone who works with stone, because he was going to move mountains.
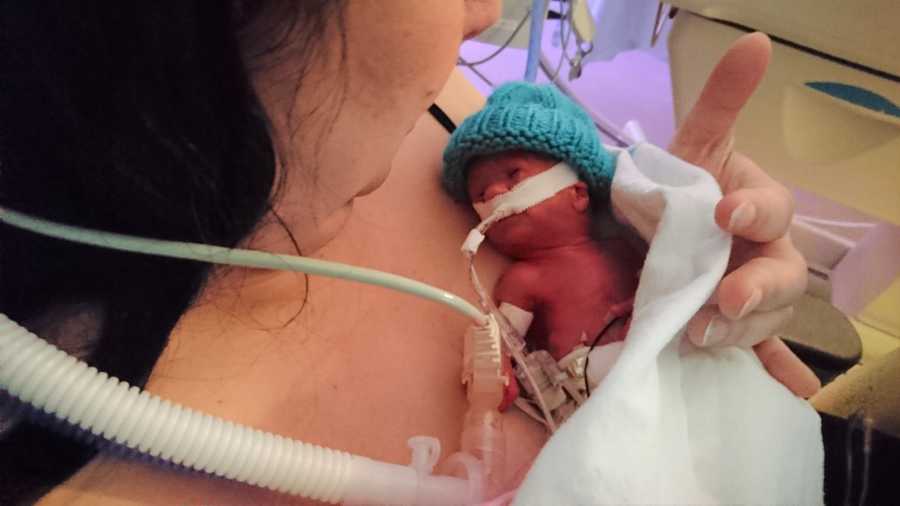
Passing through the double security doors of the NICU for the first time was so intimidating. It was a semi-open ward, and the busy sights and sounds that would very soon become our normal were still completely foreign and overwhelming, and I felt like I wanted to cry. Mason was tiny and red, and looked fragile, and at first, I had trouble reconciling that this little creature, hooked up to so many tubes and wires, was my baby. God bless our nurses, who are absolute angels on earth, for taking control of us, and helping us navigate this strange, unnatural way of learning to bond and care for our child in the most sterile, unnatural of environments, while at the same time, making it seem completely natural.
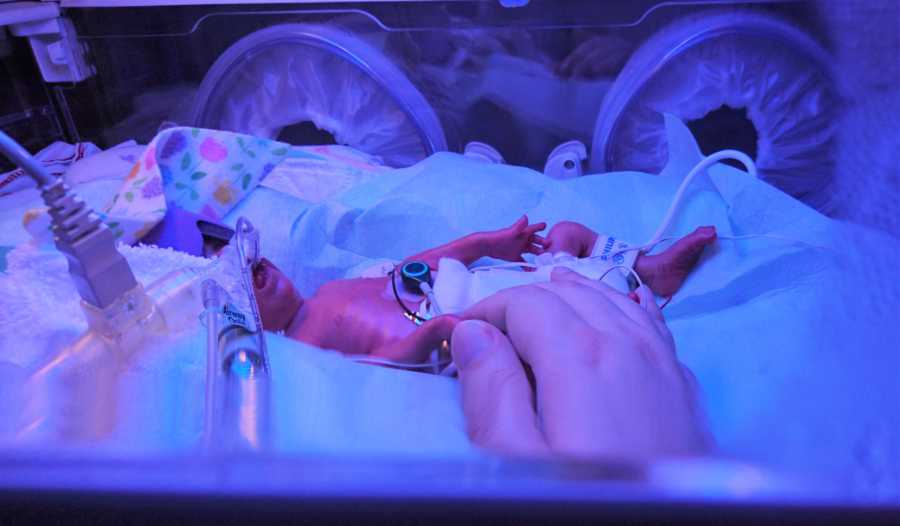
Three days after Mason was born, we were again visiting him beside his incubator, where we would just sit for hours. Because he was so small and fragile, we could only hold him an hour a day, but we would sit beside him so he could hear our voices. He was a fighter from the beginning, already surpassing the doctors’ expectations, and he was gaining strength every day. We were chatting with our nurse when the neonatologist stopped by. He said, ‘We got the genetic quick scan results back, and it confirms your son has Down syndrome. When the full scan comes back next week, we will sit down with the geneticist, okay?’ and that was it.
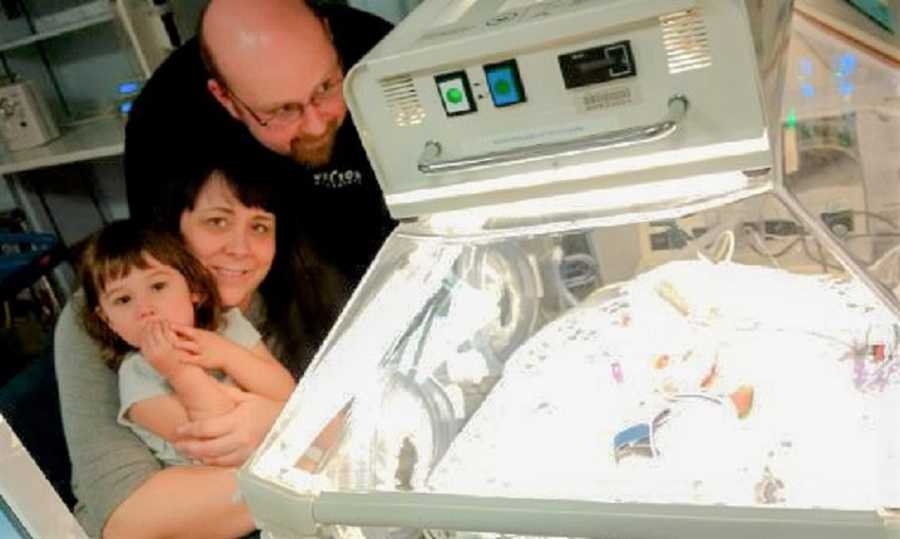
I realize it should not have been a shock. We were told so many times that he had an increased risk of having Down Syndrome. There were so many flags, but I was absolutely in denial, and did not want to see them. So, I was shocked. And heartbroken. And felt guilty for feeling heartbroken. We were quiet – I told my husband I wanted to go back to our room. Our life had been torn to pieces, and I didn’t know how to put it back together in my mind.
Silent tears were streaming down my face as he pushed my wheelchair back to our room. By the time we closed the door to our room behind us, I just put my face in my hands and cried. I cried because I was afraid of what this would mean for his life and that the world could be a scary place for someone with an intellectual disability. I cried because I felt sorry our daughter would have a brother with special needs, instead of a partner-in-crime and confidant. I cried for my husband and I who would have the responsibility of caring for him for the rest of our lives. I cried for the life I thought we would have when we got married, and I cried for the child I had dreamed of having. And most of all I cried because I was his mother, and I was supposed to love him unconditionally, and I was already failing by wishing he were someone other than who he was.
My husband let me cry, then handed me a tissue, and asked, ‘Why are you crying?’ WHY?’ What do you mean, WHY? He continued, ‘If we had known before if we had done the amnio, would it have changed your decision to continue the pregnancy?’ NO! My entire body recoiled at the idea that I would have never known my son, my Mason, my mover-of-mountains. ‘Well then,’ he said, ‘It is what it is, and we’ll handle it as it comes.’ And THAT is the perfect illustration of why I married him. He is our rock.
I would like to say that from that moment I became a convert, one of those parents I kept seeing in Down syndrome support groups that swore Down syndrome was the best thing to ever happen to their family, but the truth is, it took me longer. I loved him, but I still wished he didn’t have that extra little chromosome.
NICU was our first of many challenges – one of Mason’s doctors once said he must have nine lives. We were in NICU in Halifax for 122 days, and Mason battled two infections while we were there, and ended up needing two ‘heart cath’ procedures (cardiac catheterizations), trying to increase blood flow to his lungs due to his heart defects. From NICU, we were transferred to our home hospital for six weeks, as he struggled to master his feedings, and his oxygen requirements. But we were getting closer.
Mason was finally released home 167 days after he was born. He went home with a feeding tube, on 24/7 oxygen, with a lot of medications, and appointments, and therapies…but he was home. He was still very fragile because of his heart defects, and even on oxygen, he was not getting enough oxygen in his blood. Looking back at pictures, his skin was quite greyish, but that’s what we were used to. We were in and out of the hospital every couple of weeks with something or other. We were constantly on high alert, and I sometimes felt more like his nurse than his mother.
Finally, Mason had his two heart repair surgeries (a whole other journey) when he was 9 and 10 months old. When he was finally released home, he was a new boy! His personality was finally starting to shine through, and it was bright as the sun! He had so much energy, he started hitting milestones we had been waiting months to see. His first smile was when he was ten months old, and he rolled over for the first time one day after he turned one. He was still on oxygen 24/7, and a feeding tube, but by the time he turned two years old, his feeding tube was long gone, and he was only on oxygen at night.
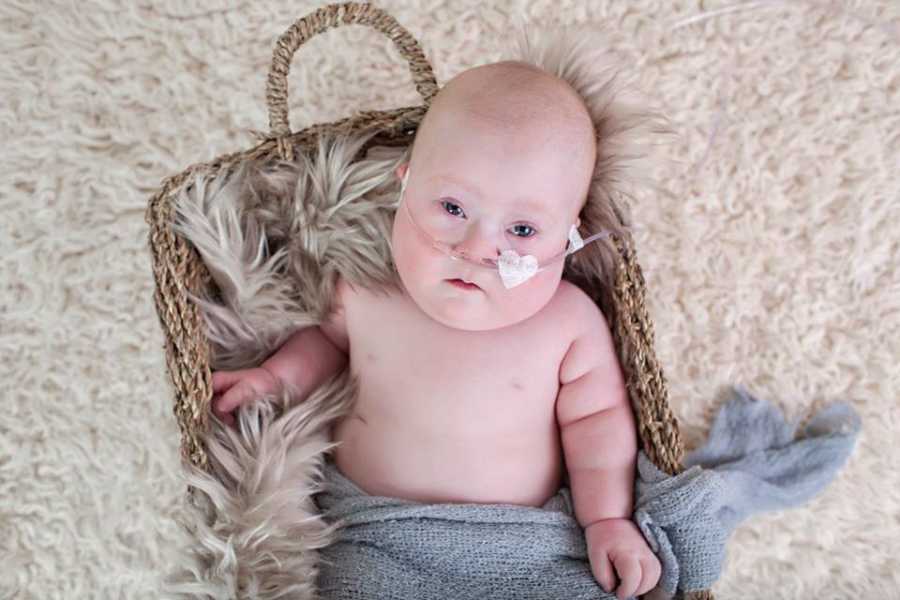
He just turned three in April and continues to be monitored by his cardiologists in Halifax twice a year. He’s had two more ‘heart cath’ procedures but is a fairly healthy boy. He sees a speech-language pathologist, a physiotherapist, and an occupational therapist regularly, as well as regular appointments with his pediatrician. He has mild hearing loss in both ears, and recently got hearing aids to help with speech development.
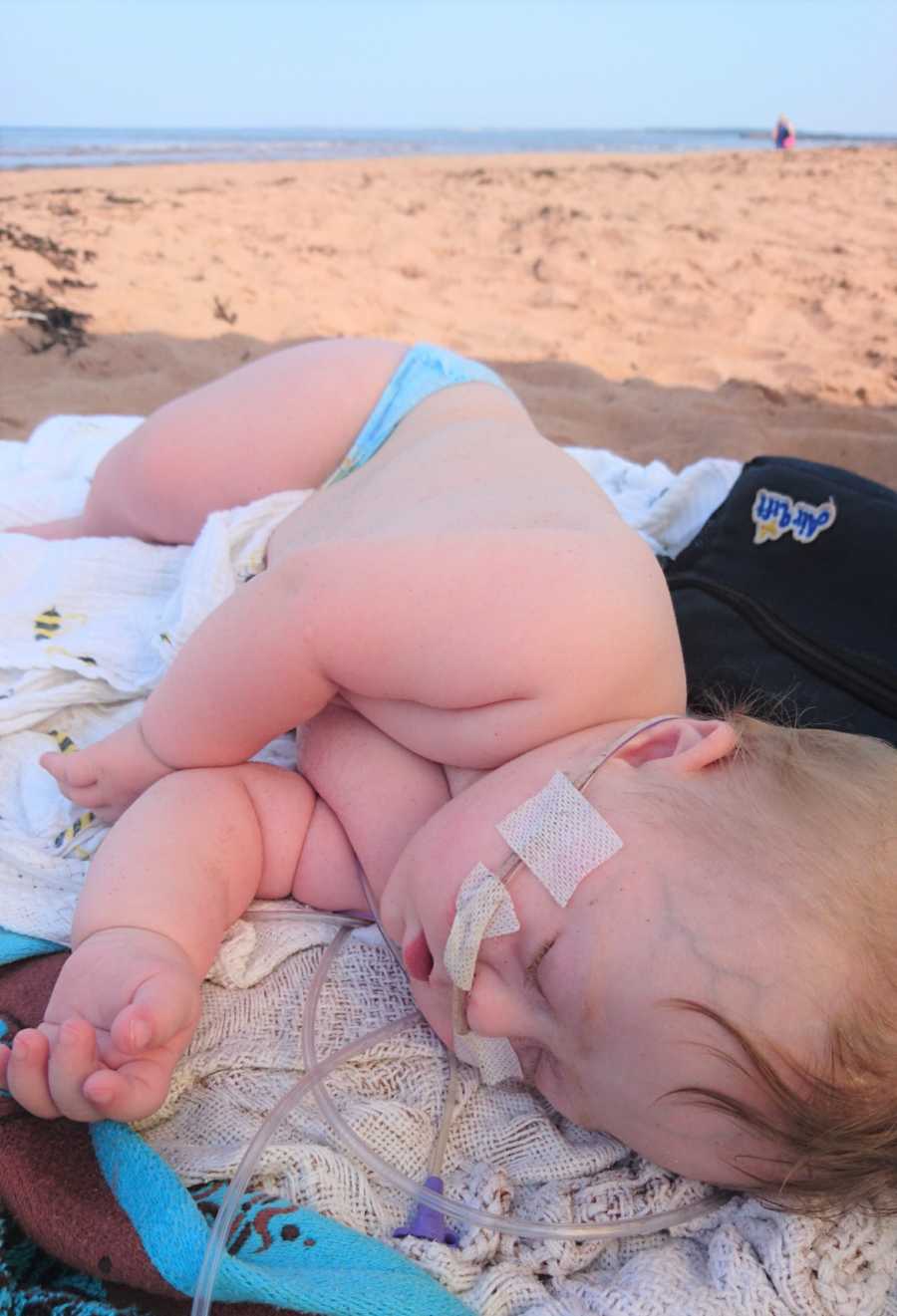
Mason is a ray of light in our family. He is an instant mood brightener – his giggle is impossible to resist. He is so easy-going and lovable. He loves music, trucks, dinosaurs, and Frozen (thanks to his big sister). Chloë and Mason are absolutely partners-in-crime — Chloë is Mason’s best teacher, cheerleader, and friend, all rolled together. The bond they have is an amazing thing to see, and I have no doubt it will only get stronger.
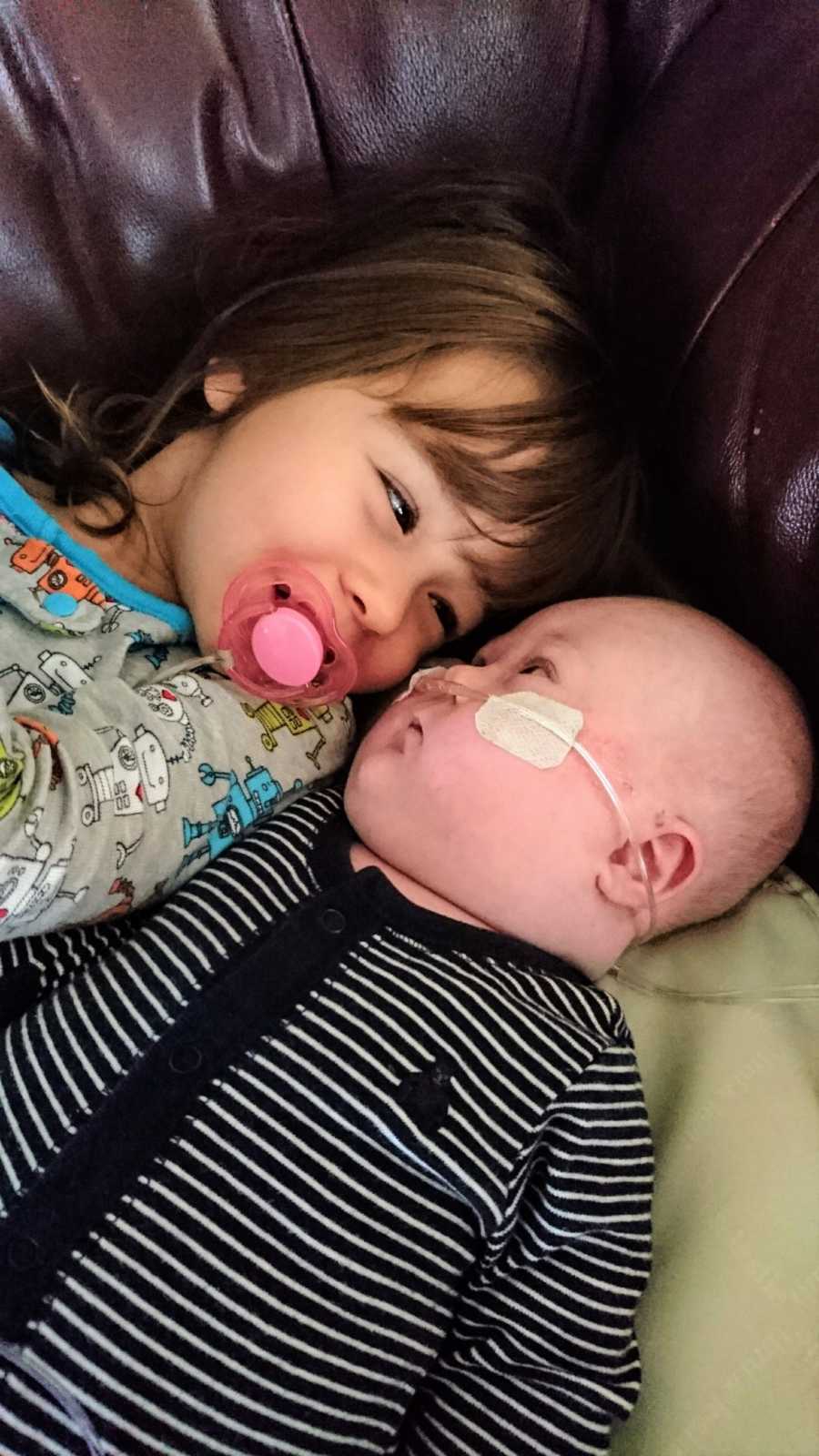
He is not perfect, he is not always happy; he is himself, his own person. He is stubborn, SO stubborn. And when he’s focused on doing something, he’s not interested in you or anyone else. But he completes our family. He’s taught us perspective on what is truly important, and that sometimes you might not get the life you wanted, but you might get something better – an extraordinary life.

I’ve also learned it is okay to be afraid of the unknown. It’s okay to grieve the life you thought you wanted. It’s common for parents of kids with special needs. But by daring to embrace your extraordinary life, you learn so much more about the trivial things that make life beautiful. You learn to appreciate the hard-won victories, and you learn to love unconditionally.

So yes, I’ve officially become a convert: Down syndrome IS the best thing to ever happen to our family. Because Mason has Down syndrome, and I would not change one single tiny thing about him, especially not one tiny extra chromosome.”

This story was submitted to Love What Matters by Michelle Scheyen-Howatt. You can follow her journey on Instagram and their blog. Submit your own story here and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Help us show compassion is contagious SHARE this story on Facebook with family and friends.

