“Our daughter Ellie Faith was born at 39 weeks with zero complications or birth trauma. 18 minutes after birth, her breathing started to decline. She was rushed to the NICU, intubated and transferred to a large university hospital near us. Later that evening the medical staff frantically knocked on our door telling us that Ellie was not going to make it and that we should say our final goodbyes to her. Her pulse ox was at 7% and so my husband immediately started to pray. It steadily rose to 60% over the course of just a few minutes. At that point, they were able to place her on ECMO (highest form of life support). She had a miraculous turnaround and was released from the NICU four weeks later. She is a true miracle.

No one ever expects to have a baby in the NICU. When you get pregnant you dream of having the perfect delivery, the perfect newborn phase and all the beauty that comes from a brand new baby. I had the easiest pregnancy out of all three of my pregnancies. It was such a dream. My 3rd baby named Ellie Faith was to be my last baby. I knew going into pregnancy that I would savor every moment. She was everything I had dreamed about.
November 4, 2016, I was scheduled to be induced at 8:30 a.m. My middle child’s labor was only one hour long and my doctor wanted to have a controlled environment so she wouldn’t be born in the car. On the early morning of November 4th, my water broke at 2:30 a.m. I was thrilled, but very nervous that my labor would progress quickly. We got in the car and made it to the hospital. We were checked in and brought to a delivery room at 3:30 a.m. It was an amazing labor and delivery and out of all 3 children the easiest. I had so much peace and literally did not feel one contraction (thank you epidural!). I smiled and laughed and was just so happy! It was everything I had dreamed about. At 9:02 a.m. my sweet Ellie Faith was born. She was perfect. The amazing nurses laid her on my chest and I was able to look into her eyes. I remember thinking how wonderful it was to see her.
For our best stories, subscribe to our free email newsletter

The nurses brought her to the warmer and checked her Apgar scores at 1 and 5 minutes. Apgar is a quick test performed on a baby at 1 and 5 minutes after birth. The 1-minute score determines how well the baby tolerated the birthing process. The 5-minute score tells the nurse how well the baby is doing outside the mother’s womb. Her scores were perfect! The nurses told us that she was 8 pounds, 9 ounces which was my biggest baby. I couldn’t believe it!
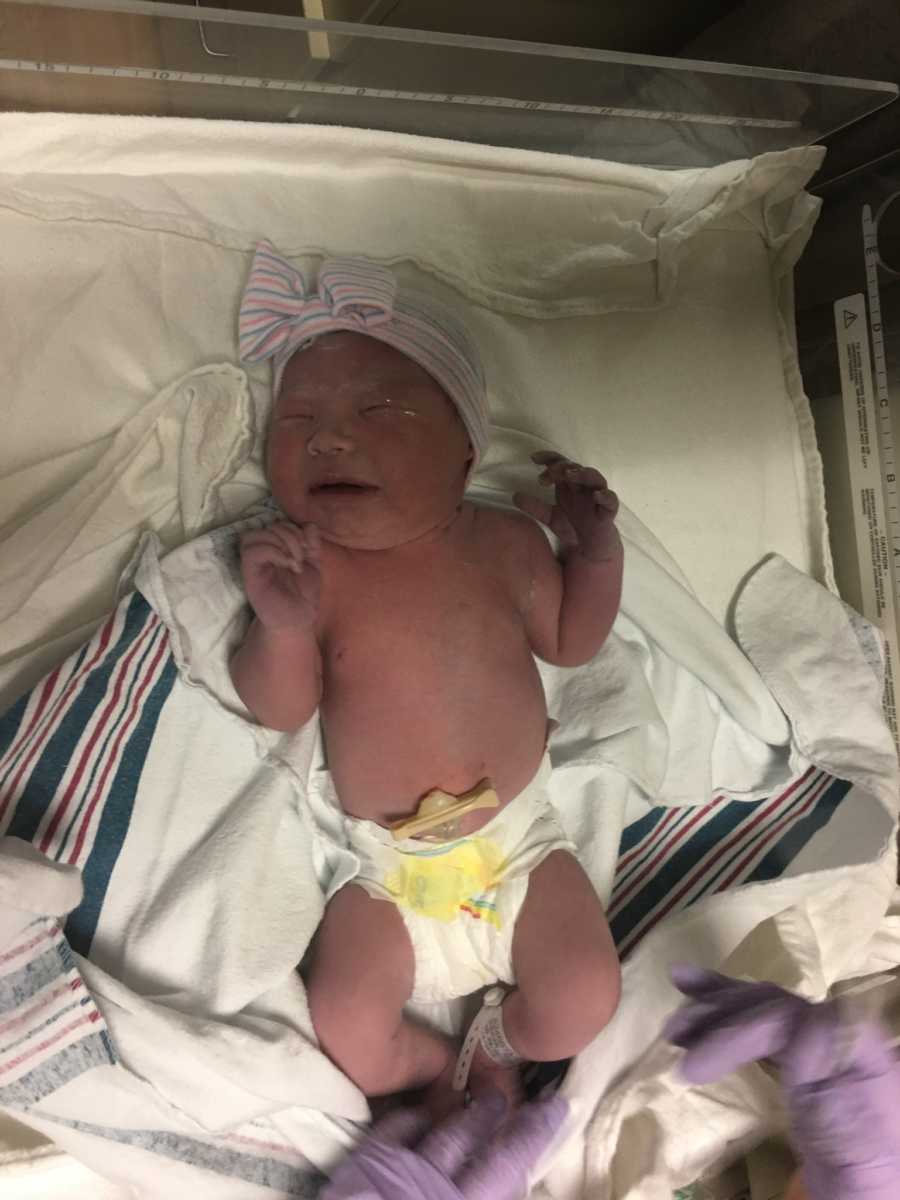
At 9:20 a.m. they wrapped her up in a blanket and brought her back to me. As they brought her back I noticed her head was rocking back and forth and as she tried to breathe it sounded like a tapping noise. It seemed as if every breath was a struggle. I didn’t think much of it and the nurse asked if we wanted a family picture.

After the pictures were taken, the nurse noticed her breathing was getting worse. She went from a normal new baby color to a blue/gray color. The nurse scooped her up and this would be the last time I’d hold her on her birthday.
A frenzy of activity followed. The nurses had called in a pediatrician to help with the situation and I heard ‘I can’t get a pulse ox over 40%.’ My heart sank. I looked at Matt completely blindsided and terrified. This was not how I expected my daughter’s beautiful birthday to be. They continued to work on her where they suctioned her throat, put a mask on with oxygen and took her pulse ox again. Right before they left she said, ‘I got her pulse ox to 100%.’ They told us that they would bring her back after they checked her out in the NICU.
We waited for about an hour and then there was a knock at the door. In walk in 4 nurses, a doctor and a medical student. I immediately thought Ellie had died and they were bringing people to comfort us. The doctor started with ‘we had to intubate her because her heart rate got down into the 60s (normal for baby is around 150).’ I did not hear anything after that. I immediately started to sob. How is it a perfect pregnancy and delivery could end up like this? My whole body went numb and it felt like a bad dream. She told us they would come back and bring us to the NICU in a few minutes.
After a few minutes of processing the fact that the next day, weeks and months of our lives were going to be the complete opposite of our expectations 60 minutes earlier, we decided to text our amazing pastors and fill them in about the situation. Their only reply, ‘we are on our way.’ They walked in about 20 minutes later and started to pray for us. It was a powerful moment, but all I remember is being very quiet and not able to pray. Thank God for others who come along side you to pray when you have no idea what to pray or how to even muster the emotional or physical strength to pray.
We waited patiently until the nurses came back to get us. They brought me a wheelchair and took Matt and I down the hall to the NICU.
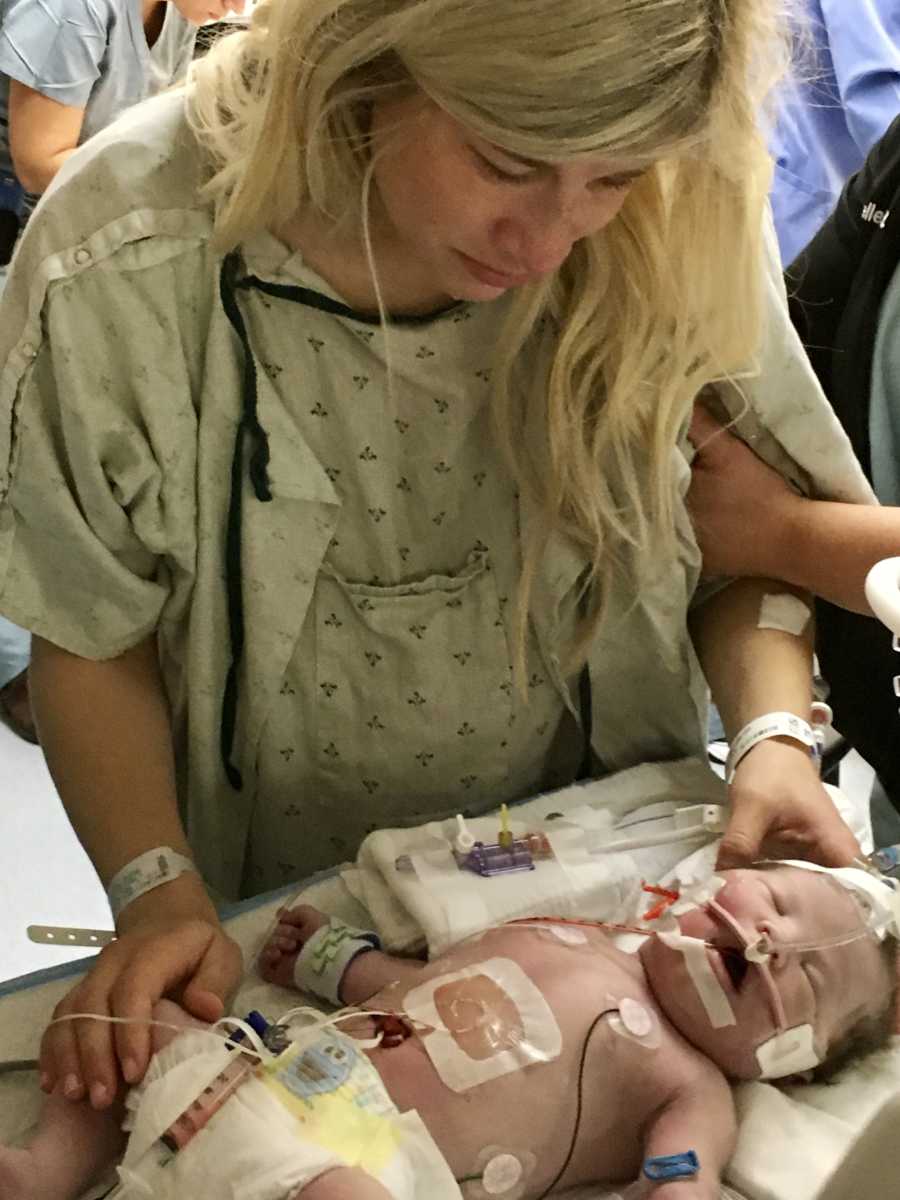
As the door opened, I lost it again. There she was, completely blue and lifeless. Eyes closed, hands cold and motionless, mouth forced open by the plastic tubing down her throat, leads all over her chest, tape across her face and body keeping everything in place, machines and tubes surrounding and running in and out of her tiny plastic box. Her pulse ox was down into the 60% range and there were alarms going off. She looked like an experiment out of a sci-fi movie and it was almost too overwhelming for me. How was this the same perfect baby that I had just delivered 2 hours ago whose blue eyes opened up so perfectly and looked into mine? Through the tears, the nurse attempted to explain how I was allowed to touch her. I was not allowed to rub or lightly touch her because it could make her breathing worse. I placed my hand on her and tried to imagine she was just like my other two children, but couldn’t get past the situation in front of me. If I accidentally nudged a tube or machine, I might break her. My heart was breaking.
The neonatologist approached us and explained they had called a cardiologist from the sister hospital of the one I delivered at to come and examine her. The cardiologist and neonatologist had absolutely no idea what was wrong with her. They checked her heart and lungs which structurally looked perfect. They said there seemed to be an unexplainable ‘wall’ in between her heart and lungs on the echocardiogram. Blood was not making it from her heart to her lungs, unable to retrieve new oxygen. Physically it seemed as if she was running ‘multiple marathons,’ but they had no idea why.
The neonatologist then explained to us that The University of Michigan C.S. Mott Children’s Hospital, located over an hour away, was sending a helicopter to come get her. I’ve worked in Michigan hospitals for the last 10 years. Mott is the best children’s hospital in the state, if not the surrounding states. They only take the most urgent/serious cases from across the Midwest and when they send a helicopter to another hospital, it’s because a life needs to be saved. That is when I knew this would be a long uphill climb. The cardiologist said she may need ECMO (Extra Corporeal Membrane Oxygenation) and it is considered the highest form of life support. It bypasses your heart and lungs, taking blood out of a body, removing carbon dioxide, adding oxygen and then pumping it back in allowing the heart and lungs to rest and heal. This is technology that was invented in the mid-80’s and carries roughly a 50% survival rate. Obviously as we were told this, we immediately started Googling it. Those statistics were less than optimistic. My husband Matt, looking for a straightforward, authentic and real bottom-line opinion, asked the neonatologist how sick he really thought she was. The doctor said, ‘This is the second sickest baby I’ve seen this year.’ That made us take a breath. I remember thinking, ‘God is this how it will end? Right after I just met her? How do I tell Emma that her baby sister died?’ Emma had been so excited to have a sister. She and I would talk all the time about what it would be like to play with a sister. They would share a room, play with dolls, dress up and be best friends for life. How do you even begin process this?
We returned to our room to begin to debrief. When it comes to social media, we are fairly private. We don’t say much publicly on Facebook, but I told Matt that we needed everyone we knew to begin to pray for Ellie as soon as possible. So he took to Facebook and posted our first update. Pretty soon prayers began to rise from every corner of the globe. We truly felt a peace and grace enter our room.
The LifeFlight team from University of Michigan hospital arrived along with what felt like 100 pages to sign for the relocation and treatment. They were going to put Ellie on a few medicines on the way to U of M hoping they would improve her breathing. We had to wait at the hospital until 5 p.m. My doctor had approved a special early discharge nearly 2 days early than recommended. Everything inside of me wanted to leave immediately, but the nurses reminded me I had just given birth and they needed to monitor me for at least a few hours. I heard it said before that God had me in a ‘bubble of peace’ and honestly that is exactly how it felt. I did not break down. I didn’t even cry during those few hours that we were apart from Ellie. God was surrounding us in peace and preparing us for what was to come.
Less than eight hours after delivery they discharged me and we checked out of the hospital and drove to Ann Arbor, Michigan, to Mott Children hospital. As we were driving, the gravity of situation started to hit me. I remember thinking to myself over and over, ‘God is good even when life is not.’ Unfortunately, we began our drive during rush hour so it took us a grueling three and a half hours to get there. After just giving birth you feel every turn, every brake, every speed bump on a whole new level. We arrived at the hospital at around 8:30 p.m. almost 12 hours after we met her. I was excited to see Ellie and our spirits were high as we entered the NICU.
The worst night of my life
We arrived, parked, found a wheelchair, went up to the 8th floor and checked in. I could not believe Ellie was in an ICU. I was still in a state of shock. I pushed my feelings aside and hurried to find her room. I was very eager to get any new information from the last time we saw her. We entered the NICU and started walking down a long white hallway. The size of this place was something I had never seen before. There were 50-plus private rooms in the NICU. Each one home to a baby hooked up to countless cords or laying sedated in an incubator. Each baby surrounded by a family who looked back at us through their window with straight, blank faces, emotionally and physically exhausted from the current status of their life.
Ellie’s room was located down at the other end of the floor. It felt like forever to get to her. Matt wheeled me in and there were about five nurses in her room setting up machines, adjusting cords and getting her settled. It was surreal, in a nightmare sort of way. I tried to bond with her, but it was near impossible to not focus on everything happening around her. This is not the birthday that I had imagined for Ellie. This was not the way my baby and I should be spending our first day together. Not only was I completely blindsided by what happened, but no one could tell me why it happened. The doctors still had no idea what went wrong, how to prevent it or if it would happen again.
At this point, we had been up since 2:00 a.m. and were exhausted from the day. We asked the staff if there was a place nearby we could stay for the night and because of Ellie’s critical condition they offered us a room down the hall, only about a minute’s walk from her room. At that time of night, there were no doctors to give us an update so we would have to wait until the morning to get an update or prognosis. All we could do was wait, but there was no space in her room for couches or chairs. They had removed anything comfortable and replaced it with a piece of heavy machinery or computer that was actively performing one of Ellie’s basic functions. We retired to the room to get a few hours of sleep to get ready for an early morning meeting with the doctors.
One hour later we were abruptly woken up by a nurse frantically banging on the door. I answered and she said, ‘Hurry. Don’t delay. The doctor wants to see you.’ We got up, quickly threw shoes on and hurried down the hall to see about 25 doctors and nurses standing inside and outside of Ellie’s room. Again, our hearts sank. At that time of night, you don’t have 25 doctors and nurses in a room like that. We walked in and the doctor introduced herself and said, ‘Ellie is a very sick baby. Please, she needs you right now. You need to say goodbye because she is not doing well and will not make it. You can grab her hand and talk to her if you’d like.’
The doctors and nurses began to step away into the hall one by one. They had done everything they could, but it just wasn’t good enough.
We noticed the pulse ox reading was in the teens…14, 16, 19, 20, 17, 16, 13.
I immediately went to the corner of the room and started wailing. I am not sure I can describe the kind of pain (physical and emotional) that I felt in that moment. Matt immediately walked up to the left side of her tiny plastic crate, grabbed her left hand in his right hand and her left foot in his left hand and started to pray for her. He asked me to join him, but I physically could not. It’s not that I didn’t want to pray, but I am not sure I could utter one word of faith in that moment. I asked the doctor, ‘Can you start ECMO?’ She answered ‘No, because we wouldn’t’ be able to get the tubes through her carotid artery. Her blood vessels are almost closed at this point.’
All I could do was cry. All other medical staff was out of the room at this point except for one nurse. She walked up to Ellie’s right side, grabbed her other hand and foot and started to pray alongside my husband. He began to intercede for her. He only remembers saying, ‘Life in Jesus’ name. You will live in Jesus’ name. By His stripes Ellie is healed in Jesus’ name.’ Over and over claiming life in the name of Jesus. He watched as the pulse oximeter continued lower and lower. 13, 11, 10, 8, 7…Ellie only had 7% of the required oxygen that her body needed.
As Matt and the nurse continued to pray, her levels began to go back up. Over the course of 5-10 minutes her level stabilized and dramatically increased, 10, 15, 20, 25, 30, 35, 40, 45, 50, 55, 60. When the doctors had given up and told us to say goodbye, my husband and a stranger stood firm and filled with hope and faith battled for her life. Then God showed up.
The medical staff began to quickly fill the room in. The doctor who had just told us to say our last words to our new baby now said we needed to leave the room because they were going to attempt ECMO. They were not optimistic she would last through the procedure. ECMO requires opening up the carotid artery in the neck and inserting two plastic tubes channeling the patient’s blood into a roller pump that serves as the child’s ‘heart’ and ‘lung’ throughout treatment. The pump sends the blood through an oxygenator, which serves as an artificial lung, infusing the blood with oxygen and removing carbon dioxide and returning it to the patient. One tube takes blood out, the other puts it back in. Doctors were worried that Ellie’s veins and blood vessels were too constricted and her body was too weak for such a procedure. Several times they told us that her odds were not good. Then they escorted us to a small room across the hall.
The next four hours were the longest of our lives. Every minute felt like an hour. We sat in a sterile white room with nothing but two chairs and a box of Kleenex. We rode the waves of faith, uncertainty and despair. One minute we cried and the next minute we sang worship songs. In those moments, your mind plays tricks on you – taking you from dreaming about miraculous healing to making funeral arrangements. I honestly couldn’t utter a prayer. I tried so hard. My momma heart just cried and sang to Jesus. We sang ‘King of my Heart’ by Bethel. There is a line in that song that says, ‘I know you are good. Every time you are good. You’re never going to let me down.’ I remember saying to God, ‘I trust you Jesus. Even if this doesn’t end up how I want. Even if Ellie goes to heaven, I will trust you Jesus.’ Obviously I did not want her to die, but I knew that if she did die that my love for Jesus would be the same. I still trusted in a God who loved me and my little girl deeply, and wept with me during this trial.
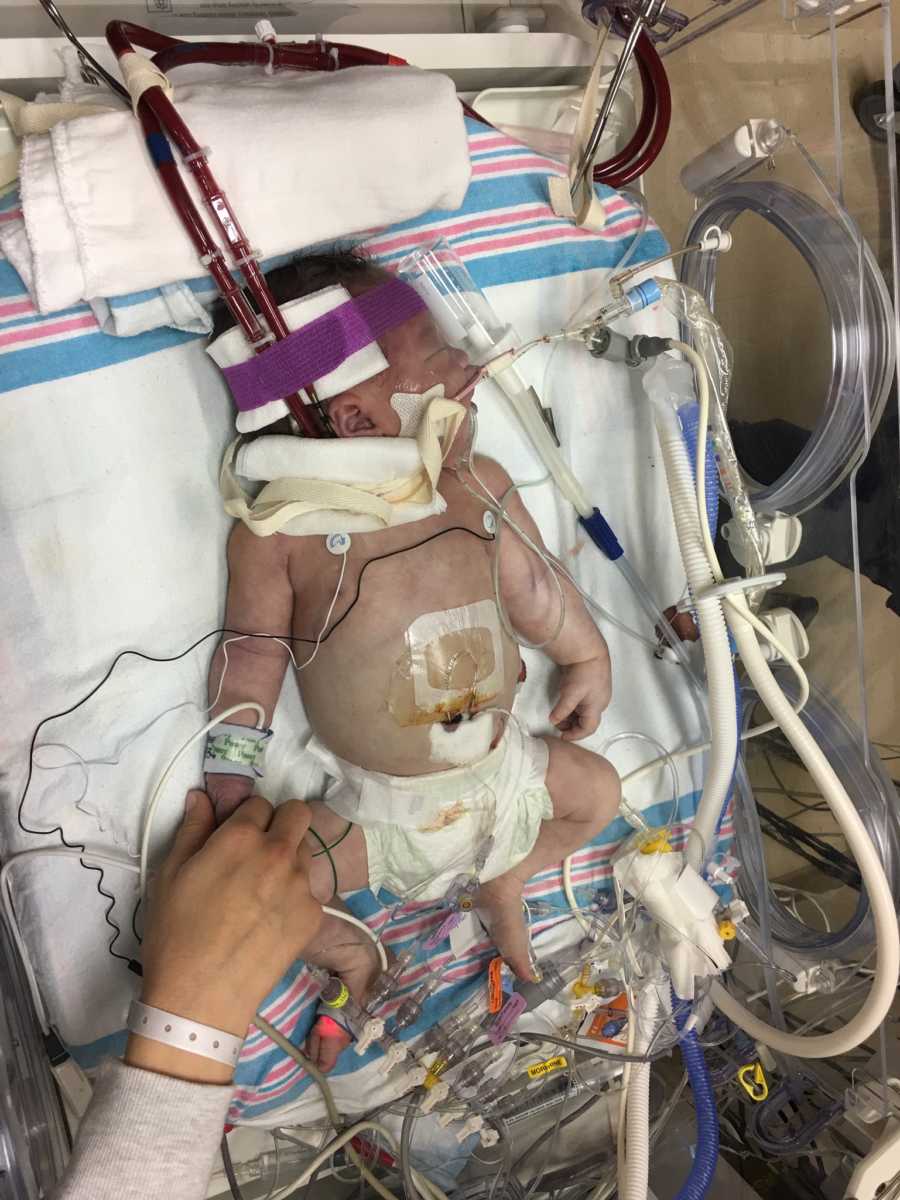
The doctor entered at about 2 a.m. and said, ‘It took a lot longer than expected, but she was successfully placed on ECMO. We are not sure if she will last through the night.’ 24 hours after my water broke, we finally had our first piece of good news. We told the doctor that we were going to bed and she said, ‘Are you guys ok?’ We both managed to squeeze out a ‘Yea.’ She looked quite surprised and said, ‘Wow, I would be a puddle on the floor right now if I were you.’ The only way we could explain not being a complete mess was a supernatural grace around us and the glorious fact that she was alive after being told she would die.
The next morning we woke up devastated, but not defeated. We walked into her room that first morning and noticed they added a bunch of wires to her head. The nurse explained that she had 11 seizures from 2 a.m. to 7 a.m. after going on ECMO and that the EEG monitor connected to her head would pick them up if she had more. Regardless of whether she lived, we knew the possibilities of long-term brain damage. Something new to believe for. Would she be brain-dead or mentally handicapped? Would we ever get to take her home to us? These questions were swirling in my head, but I knew that God was faithful.
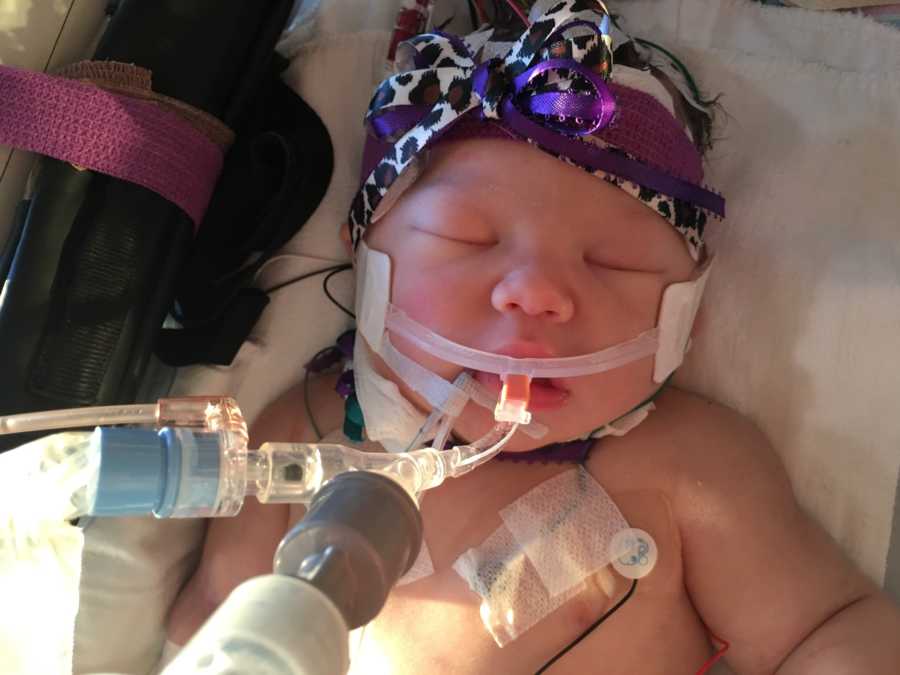
Each morning in the NICU, the doctors and nurses working first shift would go room by room talking through each case and the plan/goals for the day. They would start each day with the most serious cases and work their way down. That morning they started with Ellie at 7 a.m. sharp. We quickly found their meetings were filled with lots of useful information including what they were planning on doing with Ellie for the day, new information on what they thought happened and anything else pertinent for the day or week. Matt took meticulous notes. They told us that out of 50 plus babies on the floor she was the sickest one in the NICU and that they were concerned that her organs may start to shut down because of how long they were deprived of oxygen.
At this point we had no idea if she would ever come out of this. They had diagnosed her with PPHN (persistent pulmonary hypertension of the newborn) and HIE (hypoxic ischemic encephalopothy), but they couldn’t tell me WHY it happened. They said it was a ‘fluke.
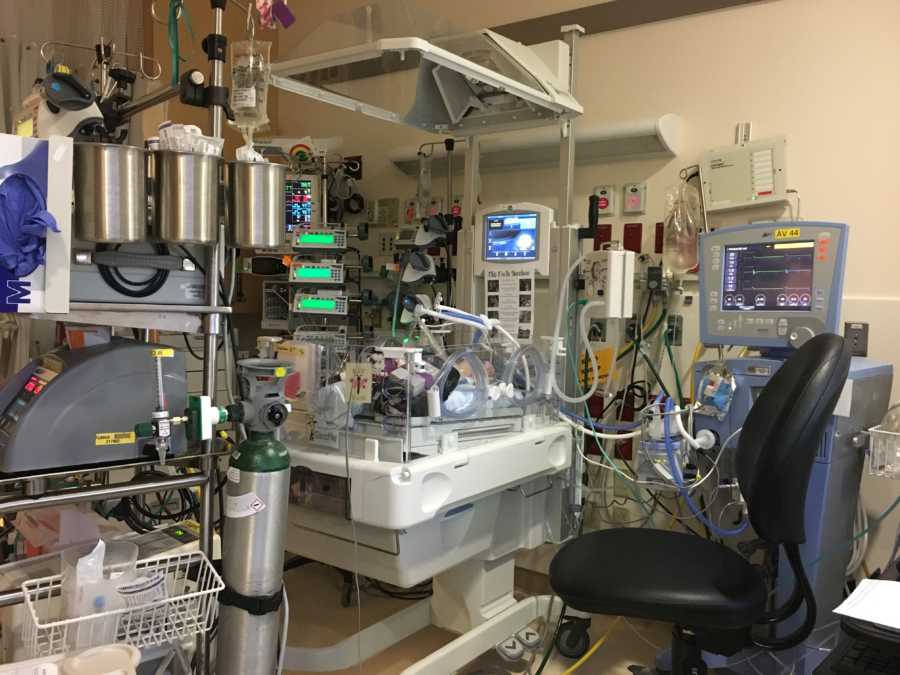
After that first day, her healing was nothing short of MIRACULOUS!
24 hours later she began processing oxygen on her own.
24 hours later she was taken off several medications, became very active and her kidneys began functioning at full strength.
24 hours later she successfully completed a trial off of ECMO.
24 hours later she was taken off of ECMO.
12 hours later she was taken off of the ventilator, began breathing on her own and moved to a CPAP machine. I was able to hold her for the first time since she was 18 minutes old.
24 hours later she was downgraded from a CPAP machine to a simple nasal cannula. She’s began feedings and tried to breastfeed.
7 days after her birth, doctors and nurses said that in more than 20 years of experience they have never seen a baby come off of ECMO and a ventilator on the same day. This level of recovery is simply unprecedented in the medical field.
7 days from her birth, we began talking about transferring her to a hospital closer to home.
12 days after her birth we transferred back to the hospital I delivered at to work on feeding and weaning from her hydrocortisone medication.
13 days from her birth she completely surpassed her goal of eating, which was 80cc’s, and fed consistently every 3 hours 100cc’s plus without fail.
14-25 days after her birth she continued to be a light to everyone who met her. We had multiple people tell us they didn’t believe in God until they heard about Ellie’s story.
25 days after her birth we went home with a perfectly healthy baby.
Even though the NICU was an incredibly hard place to be, we experienced the darkest and brightest pieces of human life. From a glimpse of the depths of death to the supernatural intervention of God breathing new life. From the vast potential of human hands and minds to the power of the unity of thousands of people coming together in spirit for one cause. It’s been like watching every sermon, verse, devotional, word on faith and healing happen in front of my eyes in real-time. It’s a beautiful thing to say that you’ve witnessed and experienced those things.

Ellie Faith is doing amazing now. We daily look at her and thank God for her life. She has completely changed my thinking in life. I have a new appreciation for my children and my husband. My relationship with Jesus would not be where it is today if I didn’t go through all of the health problems with Ellie.

She was diagnosed with brain damage in her Thalamus and the Parietal from the extreme lack of oxygen and is currently in Physical and Occupational therapy 3 times a week and speech once a week for Hypotonia (low muscle tone). The doctors have said she is about 6 months cognitively and physically behind, but they honestly cannot believe that she is doing as well as she is. She stuns every single medical professional she meets. She is complete miracle and has changed so many lives already.

I pray that my beautiful Ellie, who taught me so much about Faith, also teaches you about Faith. That you will realize that Jesus will always be with you in the hard times in life. Keep going because He is right with you.”
This story was submitted to Love What Matters by Melissa Sheehan, 32, of Ladera Ranch, California. Submit your own story here, and subscribe to our best stories in our free newsletter here.
SHARE this incredible story on Facebook if you believe miracles can and DO happen!

