“I was born in 1987 with a genetic disease called cystic fibrosis. Back then, CF was not a well-known disease, and after consulting with many different doctors, my parents were finally given the diagnosis when I was a one-year-old. Relieved they had a name for what was wrong with me, they then started the long, never-ending journey of keeping me alive. We lived on a farm in Zimbabwe, and I was the only known CF patient in the country, so I had to fly down to South Africa for treatments and to collect the medications that kept me going. CF affects many organs, but the lungs are usually the most affected, and thus pulmonary rehab and treatment is done as early as possible.
For me, this meant twice-daily nebulising with medication to open up my airways and to allow me to breathe easier. Later, from the age of around eleven, I started to need intravenous antibiotics to help fight the infections in my lungs. This consisted of two-week hospital stays every three months. As you can imagine, I missed a lot of school and a lot of ‘life’ with all these treatments. I remember being so excited to go on a school camping trip, only to miss it due to an unforeseen infection (which happened regularly). To try and alleviate missing school, I started to do my IVs as an outpatient, going to school with a needle in my arm, securely wrapped up, and only having to miss afternoon activities so we could administer medication through my line.
I was empowered to do my own treatments from a young age, and with all my hospital stays I would administer my own medications, only relying on the nurses to bring me my meds and anything else (syringes, needles, tubing, saline bags, etc.) I needed. As a child, being so different and being faced with questions from peers, teachers, friends, and pretty much every one I came into contact with, I was surprisingly confident and okay with my uniqueness. I attribute this confidence to my parents who always made me feel being different made me special and is a good thing. I still believe it to this day.
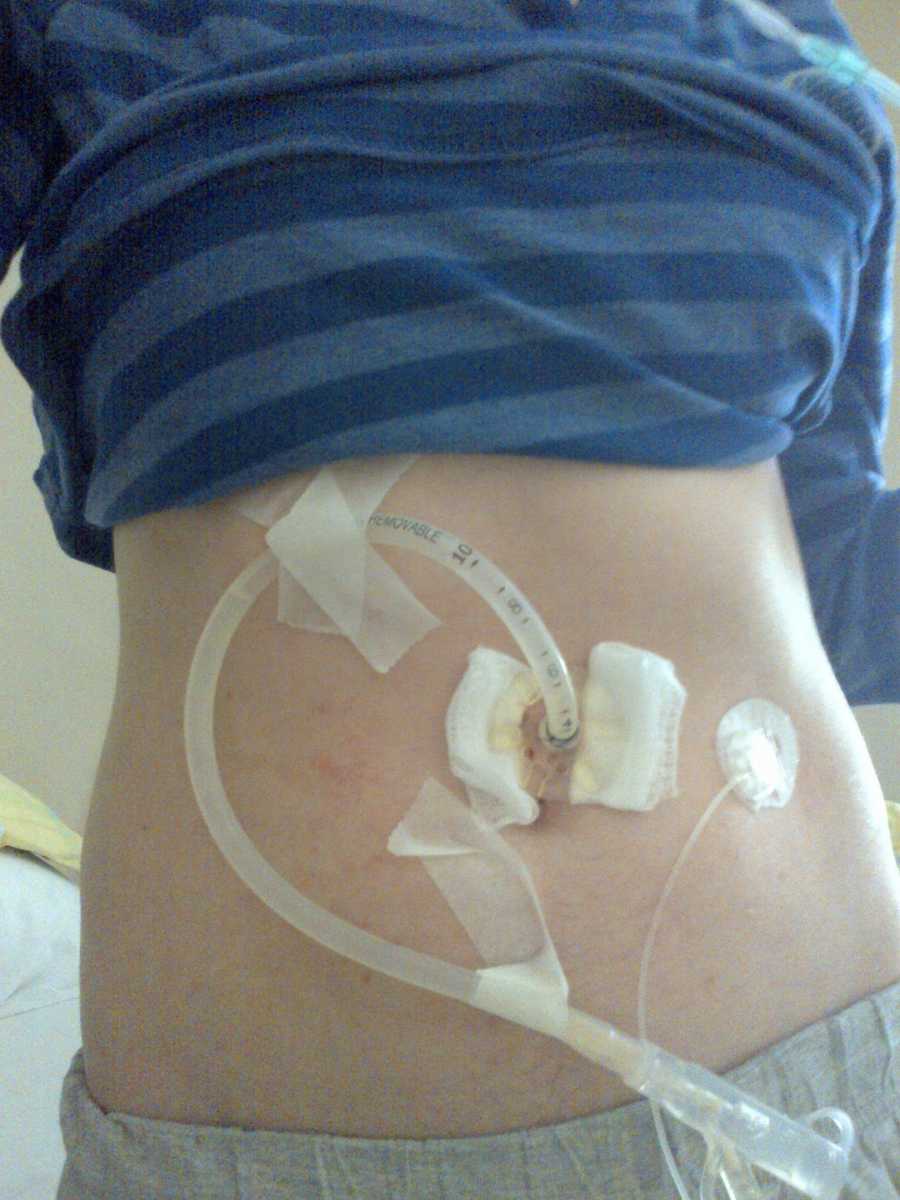
Apart from the lungs, CF also affects the pancreas, and so I need to take artificial enzymes every time I eat something in order to absorb my food. This means weight gain was virtually impossible, and while being ‘skinny’ may sound like a good thing, it’s not! I had to be force-fed throughout the day with protein shakes and anything else that would help my weight, but ultimately, I had to have a permanent stomach tube surgically inserted (this is called a PEG) to feed me throughout the night while I continued to eat as much as I could during the day.
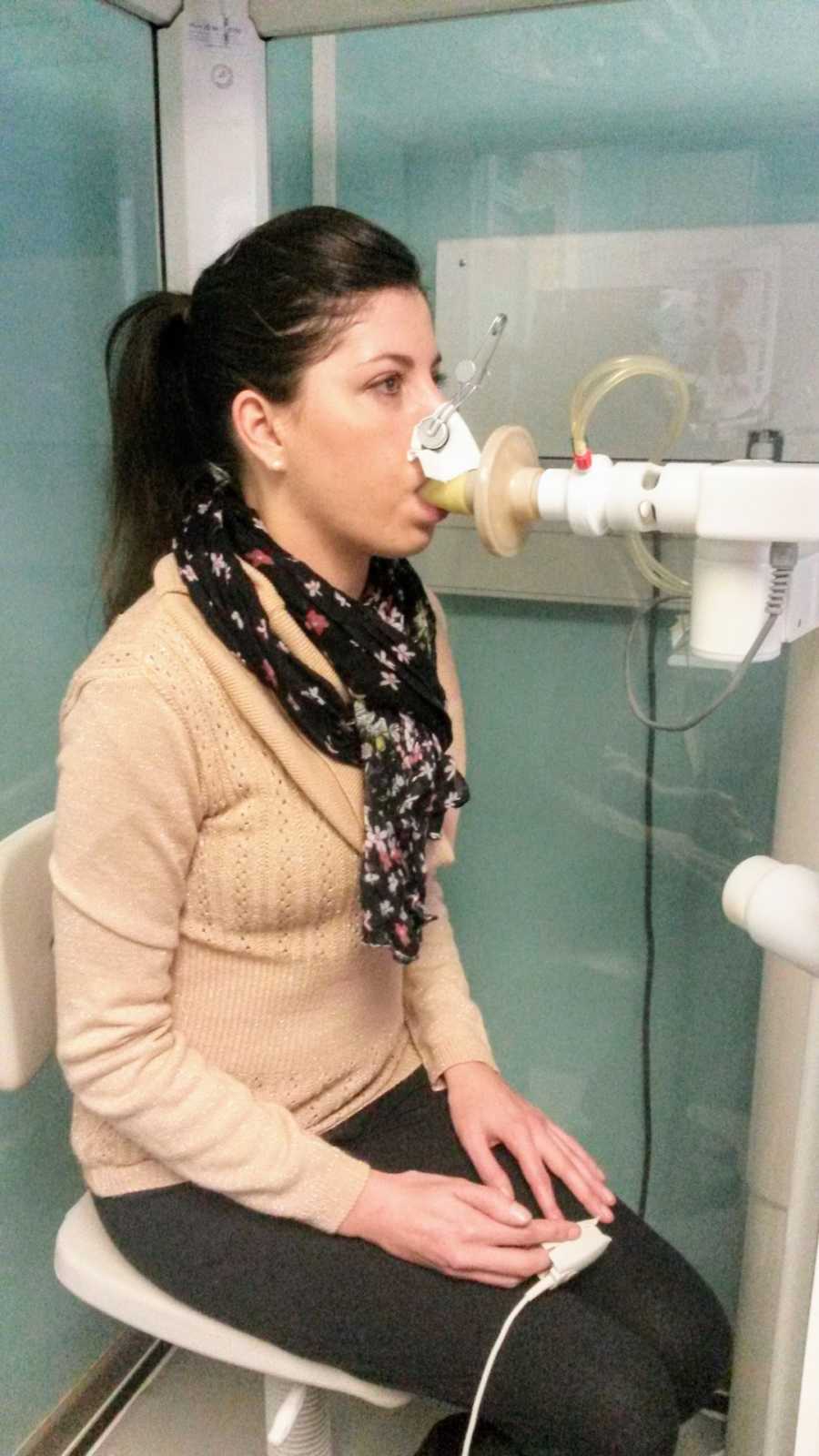
A faulty pancreas also eventually led to me becoming a diabetic, requiring insulin with all my meals. This has made my dietary requirements quite complicated, as I need to eat A LOT to keep up my weight, but I can’t have too many carbohydrates due to my diabetes, and I have had to increase my enzyme dose dramatically for every meal. I’ve never known a day in my life when I could eat anything I wanted without having to calculate how many enzymes I need to take, and later, how many units of insulin to inject. It’s exhausting!
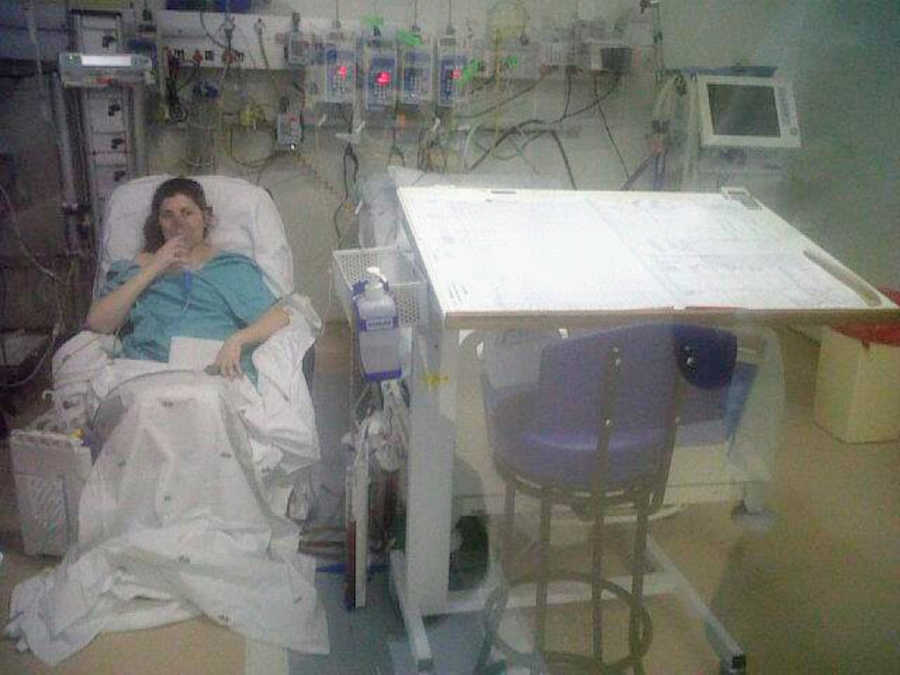
Apart from all the inconveniences of my disease, there are also real and painful physical characteristics that accompany it. I could never do any sport at school, as I got short of breath very quickly. As my disease progressed and my lungs deteriorated, so did my ability to breathe, to the point where every single breath was hard work. I would take a deep breath in only to feel a small amount of oxygen enter my failing lungs. The muscles around my lungs would spasm and leave me in constant pain as I continued to use all my strength to just keep breathing. I was put on 24/7 oxygen, which allowed me to breathe a little easier, but if I took this off even for a minute, to wash my face for example, I would start to go blue and feel faint as my oxygen levels dropped.
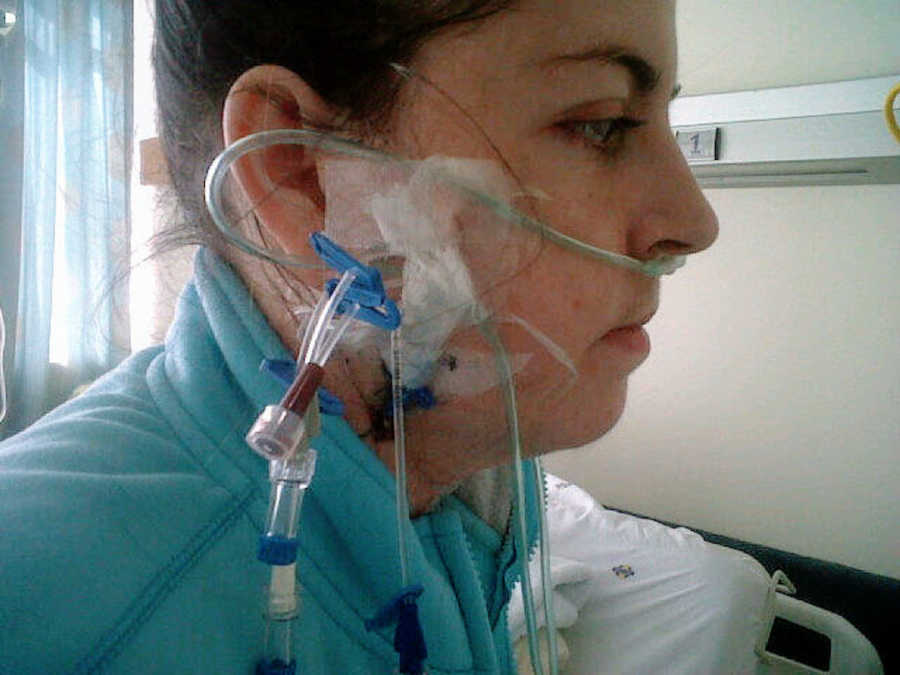
This was the point where I was listed for a double lung transplant. By then (age 24), my veins had also given up with the hundreds of needles they had to endure and I had to have a portacath inserted. This was (another) permanent tube inserted under the skin in my chest, which went into one of my main veins that travelled to my heart. Instead of having IVs in a vein in my arm, they would insert the needle into this portacath each time. Added to this was an insulin pump, as my insulin requirements increased and I needed to have insulin injected into my system overnight to account for the tube feeding I was getting. I had tubes coming out from everywhere, and it was a full-time job to keep my body going.
At this point I was now living in South Africa, as I was just too sick to travel back and forth, and I was told after the transplant I would need to live in Johannesburg permanently so I was close to my transplant center. My incredible mom moved down with me and was my caretaker for about a year while I awaited new lungs. I was completely bedridden, coughing my lungs out as I fought infections daily. I only left the sanctuary of my little apartment for doctor’s check-ups or to be admitted to hospital. I spent more time in hospital than I did out, and my life was at a standstill.
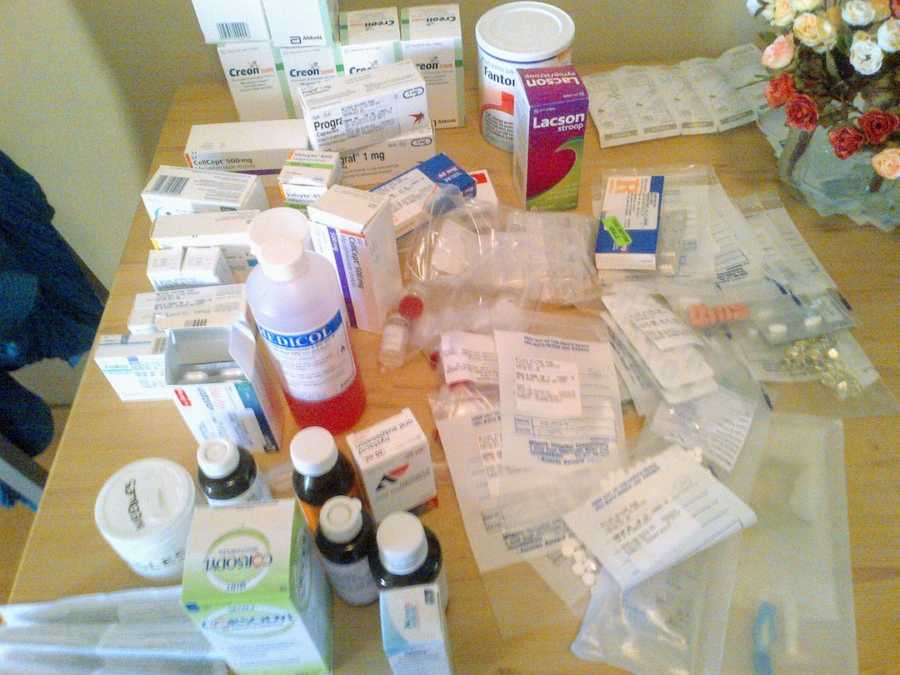
My friends were all finishing university, getting engaged, living on their own, or traveling the world, while I was in bed with my mom having to brush my hair for me because I was too weak to do so myself. They give you a 50% chance of survival for a lung transplant, and while this sounds terrifying, when you are dying, a 50% chance at a real shot at life is more than enough motivation to keep going. Through all my hospital stays, I met and become friends with others that suffered from CF. I have fond memories of us all playing poker with bottle caps we had collected from our IV medicine bottles used as poker chips.
We kept each other company and gave each other hope as we battled this disease no one else could relate to. Because we all had chest infections, we could easily make each other very sick and so we had to wear masks and keep apart from each other. A fact the movie ‘Five Feet Apart’ highlighted well. Many of my friends died awaiting a transplant or shortly after—leaving me heartbroken and having to deal with not only the physical traits of CF, but also the psychological ones, too. Finally my time came—my doctor came into my room during one of my hospital stays and informed me they had found a donor!!! I was so happy, scared, and overwhelmed.
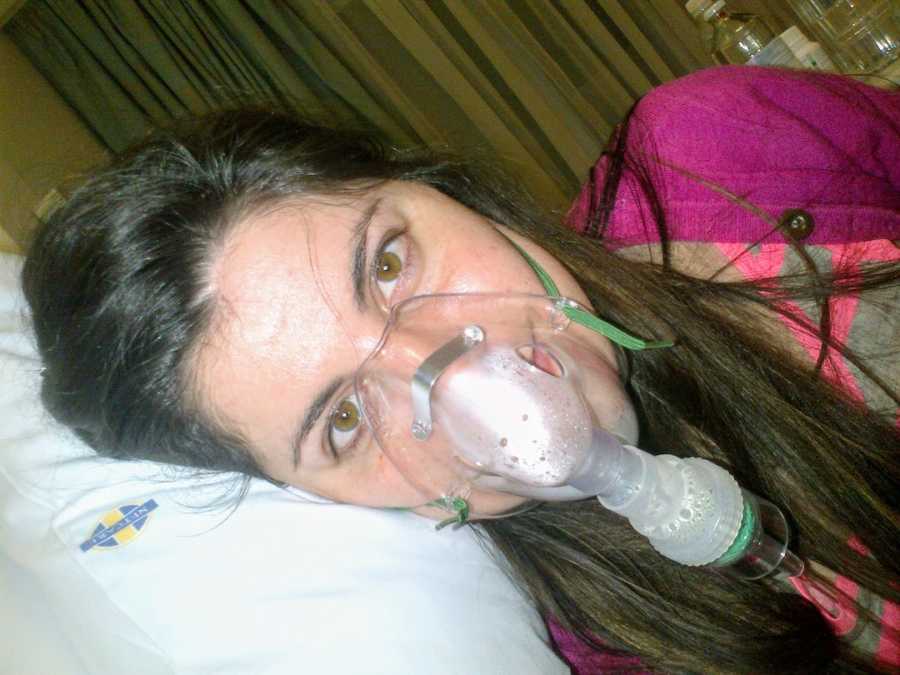
I called my mom who drove to the hospital, along with my younger brother who was also living in South Africa. We called my dad who got on a flight from Zimbabwe, but unfortunately didn’t make it in time to see me go into surgery. My special aunt and family friends also joined us at the hospital and waited with my family as the eight-hour surgery took place. I was weaned off the ventilator a day later and don’t remember too much, only that I could see my mom and dad waving at me from the other side of the glass door in ICU. I was in a little ‘fish bowl’ glass room with no visitors allowed in for the first five days. This was very hard, as all I wanted to do was hug my family and say, ‘WE DID IT!’
I was on a lot of meds, so the pain was okay, but I was too out of it to notice I was breathing on my own! No oxygen tubes!! It actually took me a few months to truly comprehend this and trust my new lungs to do their job. I would constantly look at the oxygen monitor to check if I was still breathing okay. It really was a fish-out-of-water experience as I learned how to adjust to breathing on land! My recovery was not a smooth one, and along with a few other issues I had a lot of fluid accumulating around my lungs, which was making it difficult to breathe. The fix was a simple but scary one—a pleural tap, where a needle is inserted into the pleural cavity between your ribs and lungs, and the fluid then drains out.
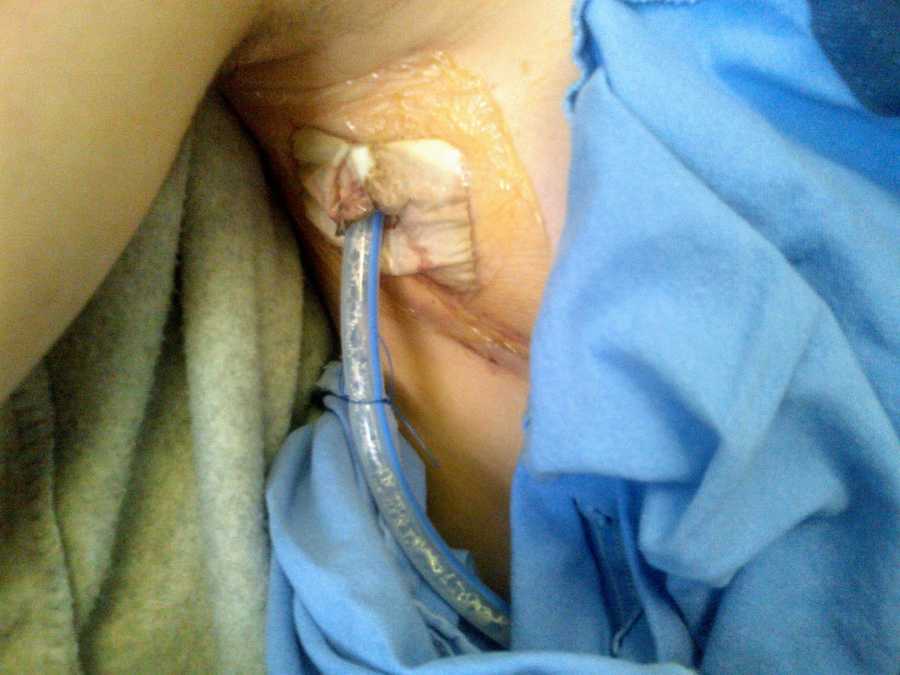
I had immediate relief, but needed the procedure done again a week later and then again another week later. The third time was NOT lucky. My usual doctor was not around, and another doctor did the procedure and ended up puncturing BOTH OF MY NEW LUNGS!! I felt the needle go in too deep and told her to stop, but it was too late (the procedure is done while you are awake). She then did the other lung, and the same thing happened. The needle went in too deep and popped my other lung. I couldn’t breathe and was put onto oxygen once again. This was something my team had never had happen before, and they now had to work out how to fix my deflated lungs.
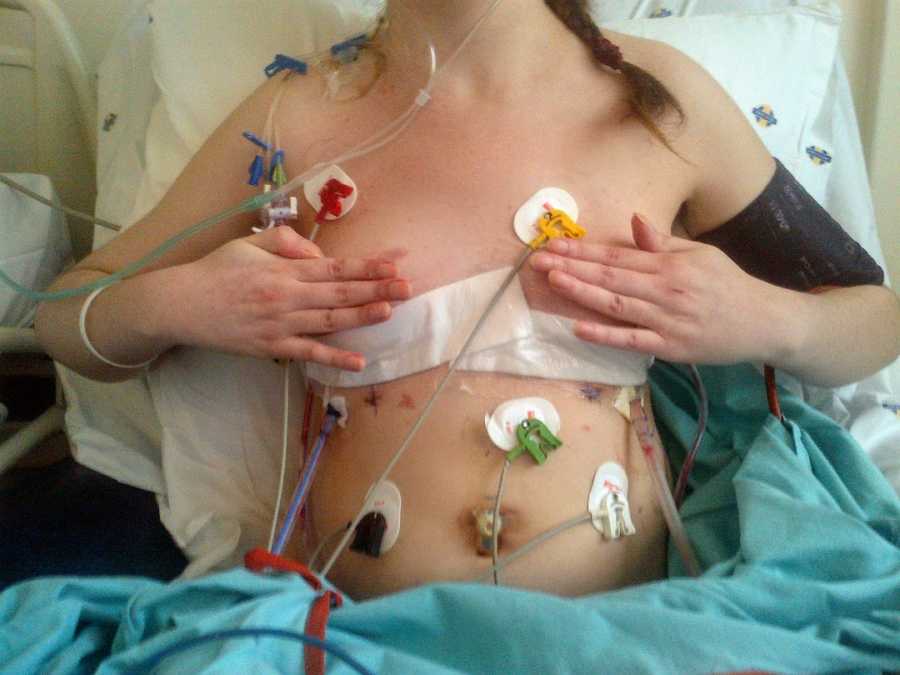
I had large chest tubes inserted, and then some more, and then even more! Some of these got infected and I ended up back in the ICU fighting for my life while my other organs struggled to keep up with everything. My surgeon and doctor made international calls all over the world to see what other specialists recommended, and everyone was stumped. I was losing hope as I lay in the hospital, unable to breathe once again. Eventually, my surgeon did an experimental surgery that made use of my own blood to essentially clot the holes in my lungs. This worked, and three months after my initial transplant surgery I went home!!!!
Now, my new life with my new lungs could begin. But where does someone who has spent their whole life sick even start? I had no university education, not many friends in South Africa, and very little confidence in the ‘real world.’ It felt like I had been kept in a zoo and then finally released into the wild, but I didn’t have the instincts to survive. My mom moved back to Zimbabwe and I found a roommate to move into my flat with me. I started blogging and doing odd jobs, and before I knew it I was helping agencies with their social media marketing needs.

I then built up my own client base and started up my own company, which I still run today. I also co-founded a charity called TELL (Transplant Education for Living Legacies), where we aim to raise awareness about organ donation in South Africa and end the transplant waiting list. Travis had followed my story on Twitter and used to wish me well on my recovery. After my transplant, I met one of his best friends who then put us in touch and we started dating. We fell in love soon after and are now happily married (we had a small COVID-friendly family wedding in 2020) and have bought a house together.

March was my eighth year with my new lungs (I celebrate my ‘lungaversary’ every year) and they are still doing incredibly well. I had a case of rejection a few years ago which we managed to sort out. I do still need to take my enzymes with every meal, along with insulin, but I don’t have my portacath or stomach tube any more. Because your body never accepts a new organ, I also need to take a handful of anti-rejection medication twice a day, but this really is a small price to pay to be able to breathe. I don’t need to nebulise or do any lung rehab, but I do see a biokineticist three times a week to ensure I maintain general strength and to treat the muscles that were so badly affected when I couldn’t breathe.
I cannot compare my life before and after transplant—they feel like two completely different lives. This said, life by nature is not easy, so even though I am loving life with my new lungs, it has not been a walk in the park. My mom was diagnosed with stage-four breast cancer shortly after my recovery and passed away three years later. A week prior to her death, my amazing aunt and uncle, who had looked after me in South Africa, were involved in a helicopter accident and they did not survive. The political situation in Zimbabwe led to our farm being stolen the same year as my transplant.

My family had to frantically try pack up our entire farm life in 48 hours, including moving all our animals to safety. We lost everything, and they had to start over by renting a small house in the city and renting a factory to carry on with business. I am so grateful to my donor for giving me a first chance at life. Every day is a blessing, and I am always reminded of how hard life can be—I have lived it, I have survived it, and I continue to fight for it.”

This story was submitted to Love What Matters by Fawn Kruger of Johannesburg, South Africa. You can follow her journey on Instagram, Twitter, and her website. Submit your own story here, and be sure to subscribe to our free email newsletter for our best stories, and YouTube for our best videos.
Read more stories like this:
Provide beauty and strength for others. SHARE this story on Facebook with friends and family.

