“In August of 2015, we became pregnant for the first time. We along with family and friends were so overjoyed. I remember family members telling me years ago that all of my mom’s sisters’ first pregnancies ended in miscarriage, except my mom with me. She was the opposite of the ‘I am 1 in 4’ statistic, and I survived. When I became pregnant I didn’t think of this at first. We had a confirmation scan around 8 weeks, and everything was looking good. After that we decided to tell everyone, and make an adorable announcement on Facebook, email, and text to surprise everyone. Just days after, I began spotting pink. I called my doctor immediately, to which they responded, ‘that can be normal.’ I let it go on for a few days, and finally begged to have another ultrasound.

We arrived at the hospital for our scan, and the tech was very friendly. I had worked in Radiology at a point in my career, so I knew they were not allowed to tell us anything official. When she started getting quiet, didn’t show me the screen, and stepped out of the room, I just cried. My husband didn’t understand, saying that we had no confirmation that the baby wasn’t there. I explained to him I just knew from how she acted. She came back into the room, said she had spoken to the doctor, and to come to my scheduled appointment the next day. We went home that night not knowing that our child had passed, and that I was in the process of a miscarriage. Not even a simple phone call was made to tell me what was going on. I went to the appointment the following day as instructed, stressed, anxious, and sitting in a waiting room full of pregnant women and small children. I kept thinking to myself, ‘is my child alive? Why can’t someone just tell me what’s going on?’ They proceeded to lead me to a room after almost a half hour wait. The doctor came in, and just said, ‘I’m sorry.’ My husband and I immediately cried together and were too in shock to say, ‘Why didn’t you call us?!’
Grief flooded us in that moment, and I went into planner mode asking what I needed to do next. They discussed the options of having a D&C, waiting it out to see if the baby would come out on its own, or to take medication to help it along. At this point, we knew the baby was gone, and I did not want to risk scarring from a D&C or other OB complications. I opted for the medication. That night, I sat at home, looking at the prescription bottle, knowing that as soon as I took those pills, the nightmare would begin. The nurses, doctors, and pharmacist all told me it wasn’t going to be pretty, and that it would bring on contractions like a regular birth, only I could bleed dangerously. I took the medication, and just sat looking out at the lake from my bedroom window and cried. I was saying I was sorry to the baby I would only ever know inside of me and wishing I could understand why this happened. I felt like I had let him or her down. We just had the genetic testing days prior to find out the gender. Now I would never know. We simply called him/her Baby T. We talked about gender neutral names, but just kept them between my husband and myself.
I got onto Facebook, and wrote an announcement that we had lost baby T. I posted a beautiful picture and said, ‘A person’s a person no matter how small. We are heartbroken to say that Baby T has moved on to heaven. The doctor assured us we did nothing wrong, that I am healthy, and we should be able to get pregnant again soon. 20% of pregnancies end in miscarriage, and we just happened to be one of those couples this time. I don’t regret telling friends or family, because after seeing that heartbeat for the first time, that was enough to be overjoyed and willing to celebrate a life no matter how short it may have been. We appreciate the prayers and thoughts over the next few physically and emotionally painful days. I felt those who care for us should know, and please understand that discussing further at this point only brings pain. We look to the future and will always be thankful for our first pregnancy.’

That night and into the next day was unimaginable pain and horrendous amounts of blood. I tried sitting in the tub with hot water, I took the medication they gave me, but nothing would stop the waves of pain. Knowing I was laboring out our child, and not having him or her at the end of it made it that much harder. Finally, the bleeding became too much. I called my doctor’s office, and they waited 2 hours to return my call. I was already on my way to the emergency room. I had begun to feel weak, faint, sweating, and losing large sums of blood. The ER doctor was so kind and took my situation seriously. They ran blood work and ultrasounds immediately. They wanted to know if I had passed ‘the sac,’ so he ordered an ultrasound to see if intervention was necessary. My husband had to stay back in the room. I will never forget sitting alone in that room waiting and crying to myself. Crying not only about the physical pain but the emotional pain. The ultrasound tech who came in to do the scan I had not met, but she knew why I was there. She asked me, ‘Why are you crying?’ I said I lost a baby, to which she replied, ‘You’ll get pregnant again.’ I was stunned. Like our child was replaceable. I spent the rest of the scan silently crying to myself.
The next few weeks were hard. I had to go into the lab every week to have my HCG levels tested. In order to try and get pregnant again and to assure my body had passed the remnants of our child, the levels needed to be zero. Every week they would slowly creep down, and I would find myself praying for the next Monday to come so I could be tested again. Once my levels were zero, I called my doctors asking advice, what I should or should not do, anything I should be concerned about, and the response I received was, ‘Call us when you’re pregnant.’ I was floored. I came home and told my husband I was not going to be just another chart in their office, and we were finding a new OB.
Two months went by. We were with a new office. My new OB had dealt with high risk and didn’t see any concerns for another pregnancy. He gave us the green light after one menstrual cycle to try again, and in December of 2016 I became pregnant with my daughter. Little did I know the hurricane of events that was about to occur over the following 8 months.
My first scan looked great, so I continued on as normal. I started having horrible nausea and vomiting and chalked it up to normal pregnancy sickness. It wasn’t just in the morning, but all day long, until finally one day I was vomiting bile and dry heaving. I was so weak and disoriented that I called the on-call OB, and they said I needed to go to the ER. Turns out I was severely dehydrated and diagnosed with Hyperemesis Gravidarum. I couldn’t hold down water or crackers, so I had to go in a few times to receive IV transfusions of fluid. Up until this point my labs were normal, no protein in my urine, and blood pressure was within normal range.
Into my second trimester, my blood pressure started climbing slowly. I am typically one who runs 120/80 at the highest, and more so into the 110/70s range. When my pressures started reading into the 140s over high 80’s I became concerned. The doctor didn’t feel they were high enough to do anything about it at that time. I started swelling, having back aches, trouble sleeping, and just thought it was all normal pregnancy symptoms. I went into my doctor’s office with lists of what I was experiencing and didn’t leave a single thing out. Just as I began regaining my appetite, it came time for the glucose test. I failed ‘borderline’ so I was diagnosed with gestational diabetes. I had no precursors to this disease. I didn’t smoke, I wasn’t obese, I didn’t have a family history. I was so confused. They set me up with a specialist to teach me how to eat on a strictly controlled diet for the remainder of my pregnancy.
While most women gain weight, I was losing or staying pretty regular. It was towards the end of my second trimester that I noticed heavy swelling. By the time my baby shower rolled around, my blood pressure was so high I went to the emergency room. It was 165/98. This was extremely high for my ranges. When I returned home, I was out shopping with my husband. I was hot and asked if I could stay in the car while he ran inside. I noticed a small star in my vison that looked like a rainbow of color. It started spreading through my field of vision and becoming larger. I called my husband right away and said we need to go to the hospital. I ran to the labor and delivery, and my blood pressure had skyrocketed. By this point my vision was becoming a black cloud in my left eye. They laid me down, hooked me up to the monitor and called my doctor. My doctor then decided to put me on a low dose of blood pressure medication. At this point, the damage had already begun. Little did I know I would have my daughter just 12 days later.
I went in for my regular appointments, biweekly non-stress tests, and ultrasounds every other week. My pressures were still high, but not as high as they had been, and baby was looking good. After about a week on the medication, I started noticing I wasn’t feel well. I knew something just wasn’t right. My doctor assured me my climbing pressures weren’t anything to worry about, and I had presence of protein in my urine but not enough to worry about. He would send me to a specialist for peace of mind. What I didn’t know is that peace of mind visit would end up being an immediate action plan to save the lives of myself and my baby who was only 31 weeks gestation. They did another ultrasound, mind you I just had one done 3 days prior, and the doctor came in immediately. He said the baby’s fluid levels were becoming dangerously low, that I was Preeclamptic, and I needed to deliver by the end of that week. I was in shock. He instructed me to call my husband and get me to the hospital where I was to deliver, not to stop at home to grab a bag, toothbrush, nothing.
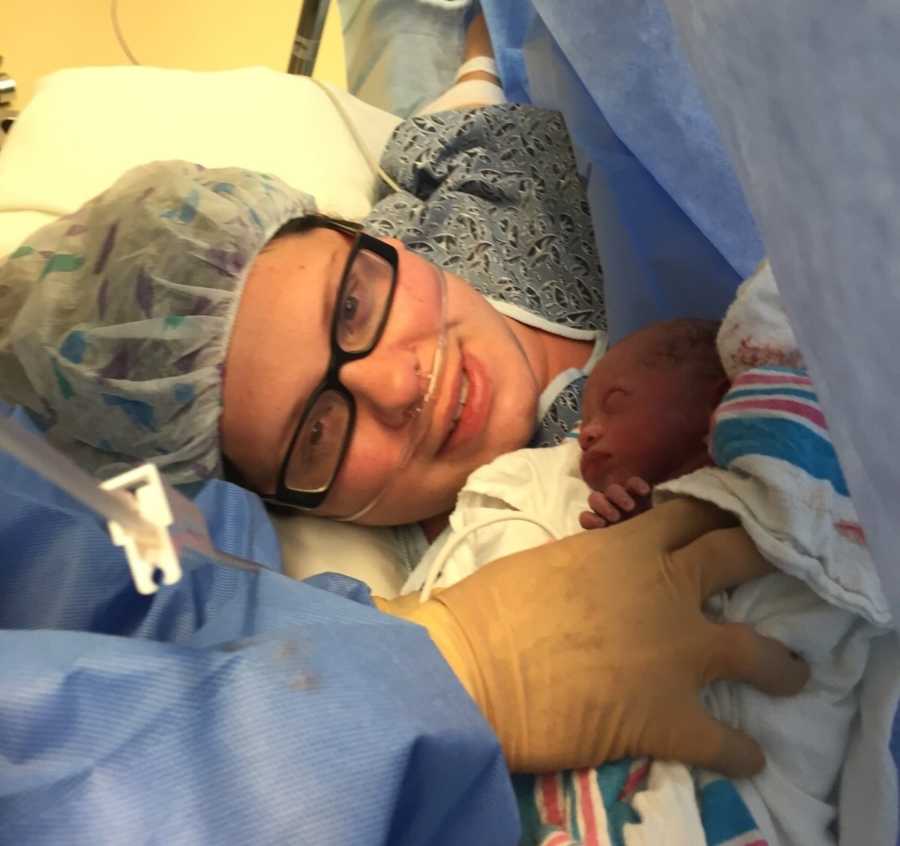
We arrived at the hospital where I was to have Emma, and they started prepping me immediately. I was given IV fluids, magnesium, and steroid injections to help my babies premature lungs develop. I went in on a Tuesday and waited until that Friday for a scheduled C-section. I can still hear the sounds of the leg cuffs blowing up full of air to keep blood moving through my body, and the blood pressure cuff that went off every hour to track my pressures. All I could do was lay there and wait. Friday morning came, I was prepped for surgery, and after missing my spinal block numerous times, Emma Chloe came out with a cry. It was then I uttered her name for the first time through tears of joy. I was so grateful to hear that cry, even in my daze of whatever meds they gave me to lower my pressure and ease my anxiety.
I remember them saying, ‘Open your eyes, look at your baby,’ and I had a brief moment of her cheek next to mine. She had stopped crying then, I gave her a quick kiss, and they rushed her off to the NICU. She was 3 lbs 8 oz and 16 inches of perfection in my eyes. The next few hours I don’t remember. They took me back to my room where I remember vomiting, and then sleeping almost all afternoon. I woke up asking to go see the baby, not knowing how long I had been out. I was weak, disoriented, but thankful it was over. Emma was doing great, and I just had to be patient for her to mature enough to come home.
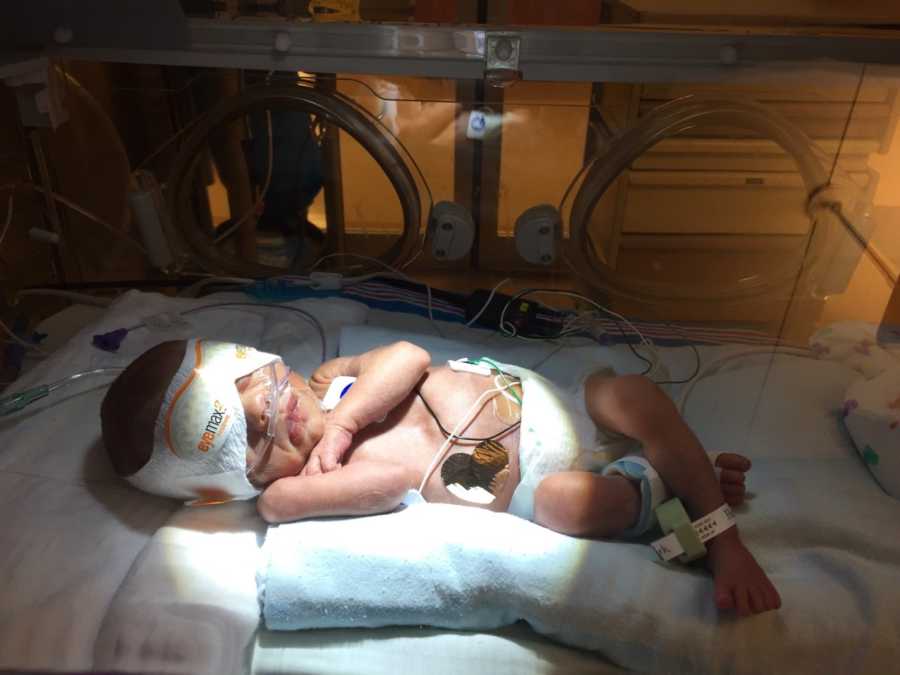
Two days later they decided to send me home on the third day. My pressures were good, labs were to be expected after C-section, so they thought I was ready. That night, my blood pressure skyrocketed to 180/99. They called the doctor and increased my blood pressure meds. This made it come down, so they released me the next day. The moment I went home I just wanted to be back in the NICU with my child, but I knew I needed some rest. The next morning, I woke with a rattling in the lungs. It sounded like crackling and wheezing, and I could almost feel it. I called my doctor, and he said it could be from the anesthetic. He sent me to the emergency room to be looked at. My blood pressure at intake was 175/100. They took me to the big room, you know the scary ones with the big lights that they bring traumas into. I knew it was serious. I had X-ray techs arriving to do a chest x ray, techs putting EKG leads all over my body, and phlebotomists drawing vile upon vile of blood. The only answer they could give me was that my potassium was low from urinating out all the fluid I had taken on, so I sat with a 7 hour drip and they released me.
I spent the rest of the night in the NICU and got to hold my daughter for the first time. I will never forget this, because two days later, I would almost lose my life. I was swollen, pale, weak, with lips cracked and bleeding, nose bleeds, and blood pressure through the roof. Little did I know this picture of me holding her might be my last, as I was admitted to the ICU that night with Post-Partum HELLP syndrome.

The next morning, I woke up seeing giant yellow bubbles in my vision. The bubbles then started turning to black spots, pinhole vision, and eventually black holes. The ER scanned me for a stroke and couldn’t find ‘as much as a clogged sinus,’ they said. My blood pressure was still high. I wanted answers. They told me to see an eye doctor, and sent… me… home. The next day I saw the retinal specialist who informed me I was experiencing bilateral serous retinal detachment and could go blind from the high pressure I had experienced. He called my OB and was scolding him saying, ‘Why didn’t you do something about this? Your patient has organ damage!’ So, I insisted on being readmitted.
You know things are serious when specialists start coming into your room, and the hospitalist that took my case sat down and began explaining my results. I looked right at him and said, ‘It’s HELLP syndrome, isn’t it?’ He looked taken aback that I knew what it was. Lucky for me I had read up on everything that could go wrong during a pregnancy. Little did I know I was about to become a statistic, and part of the 0.5% affected by this deadly disease. And even worse, the ‘cure for HELLP is birth.’ I was 5 days postpartum…
The hospitalist gave me the option of transferring me to a Chicago hospital where I may not make it on the trip in the ambulance, or to move me to the ICU and start treatment immediately. I decided to stay put, to not risk losing my life on the interstate and being an hour away from my daughter who was only days old. As they wheeled me into the ICU, shock set in. I thought this was it, I was going to die. I began to sob uncontrollably, as they placed not one but two new IVs in my arms. The reason for this was the medications couldn’t mix, or it could stop my heart. I spent what seemed like an eternity in that ICU, with little to no vision, not being able to see my daughter, and constantly fearing this was the end. After the first night, by the grace of God, my numbers started improving, pressures dropped significantly, and I appeared to be on the road to recovery. I felt like I was born again, given a second chance at life, to make a difference. It took months for my vision to recover, and I still have permanent damage in one eye.
Our days were spent living in the NICU, trying to give my child every ounce of my attention between the plethora of doctors’ appointments I had to endure. General practitioner, OB, Cardiologist, neurologist, retinal specialist and so on. Luckily a cardiologist took my situation seriously, and found I was suffering from pericardial effusion, and mitral valve regurgitation from the extreme blood pressure. I decided I was going to make the best of the situation and be thankful that we were simply ALIVE.
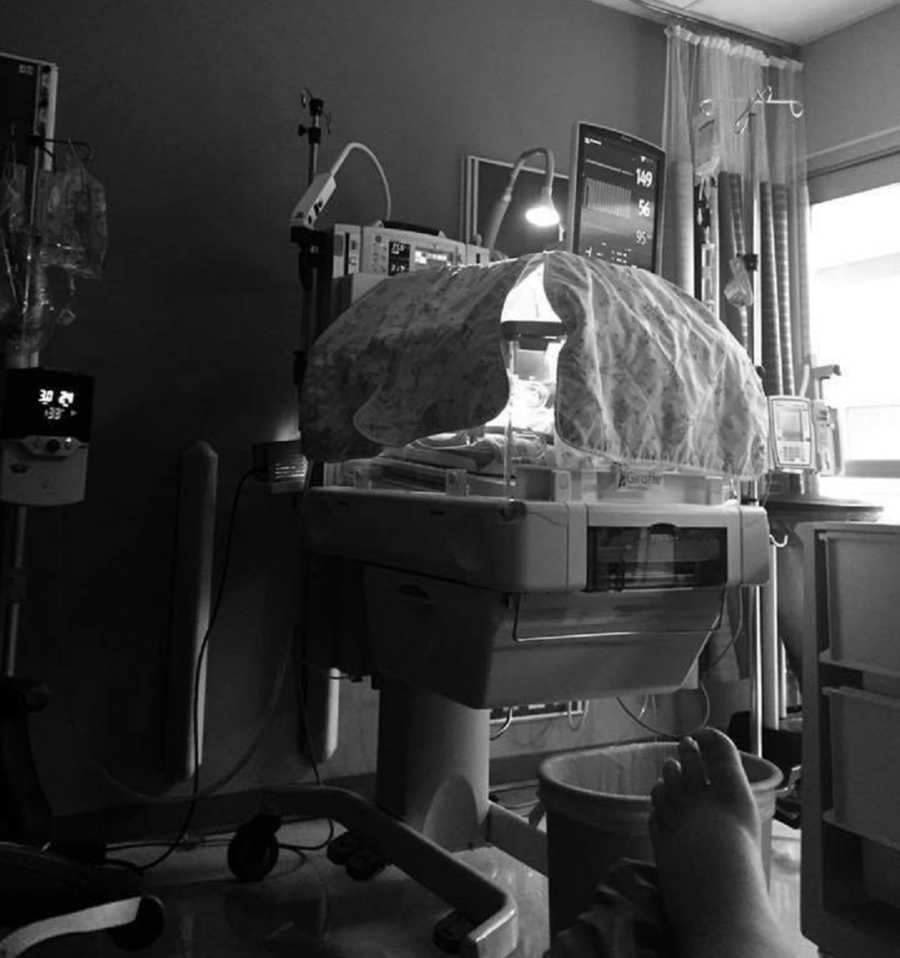
We survived what some don’t, and I would have to be patient, but my baby would be coming home with me. We spent four weeks to the day in that NICU, which became our second home, and its staff our second family. Now, my daughter’s sweet smiling picture graces the Hallway of Hope, which is the hall that leads to the secure NICU Unit. These photos give other scared families hope, that you can get through this, and there are so many others who have gone from fighting to thriving.

Today outside of my job as a business professor, I work with a not-for-profit who helps NICU and bereaved families. I attend conferences to learn more about this rare disease, and I share my story in hopes that one day it may save a life. I needed to share my story, and to help others who so selflessly helped us. Our voices and experiences will be heard around the world, and we CAN and WILL make a difference.”



This story was submitted to Love What Matters by Stephanie Trendowski, 34, of Crown Point, Indiana. Have you experienced something similar? We’d like to hear your journey. Submit your own story here, and subscribe to our best stories in our free newsletter here.
Provide hope for other struggling mothers. SHARE this story on Facebook to help spread awareness.

