“I was a happy, healthy 32-year-old when I became pregnant for the first time. I had no known risk factors for any pregnancy related complications. I received all the proper prenatal care and my pregnancy was normal until I went into labor naturally at 40 weeks 3 days. My husband and I arrived at the hospital and settled in to await the arrival of our baby boy. I had no idea that the very bed I was settling in would soon become my death bed.

After complaining of some nagging pain in my ribs on my right side, my doctor ordered lab work to check my blood and liver function. She came back to tell me that I had HELLP Syndrome (hemolysis, elevated liver enzymes, low platelets) and the only way for me to get better was to deliver the baby. I’d never even heard of HELLP Syndrome and it was never explained to me how serious of a diagnosis this was. My liver was swelling (hence the pain in my ribs) and my liver enzyme levels were over a hundred times the normal amount, my kidneys were shutting down, and my platelets were well below normal. I was given magnesium sulfate to help prevent a seizure or stroke, and I eventually had a caesarian section due to my labor failing to progress. My little boy was born small, but healthy. All through the night my blood was taken hourly allowing me little to no sleep. I continued on the magnesium sulfate drip for another 24 hours, which felt like fire flowing into the veins in my arm and made my head groggy and easily confused.
Early the next morning I became frantic. Something terrible was happening and I told my husband to find help immediately. All of a sudden the pain in my ribs was excruciating. It felt like knives were stabbing me from every direction. I told whoever was listening that I felt like I was dying, and indeed, I was. A CT scan revealed blood spilling throughout my abdomen. I was bleeding internally uncontrollably. Immediately I was given blood transfusions and platelet transfusions. My husband was told I may not survive; my chances were around 20%. He needed to prepare himself that he may leave the hospital with a baby, but not his wife.
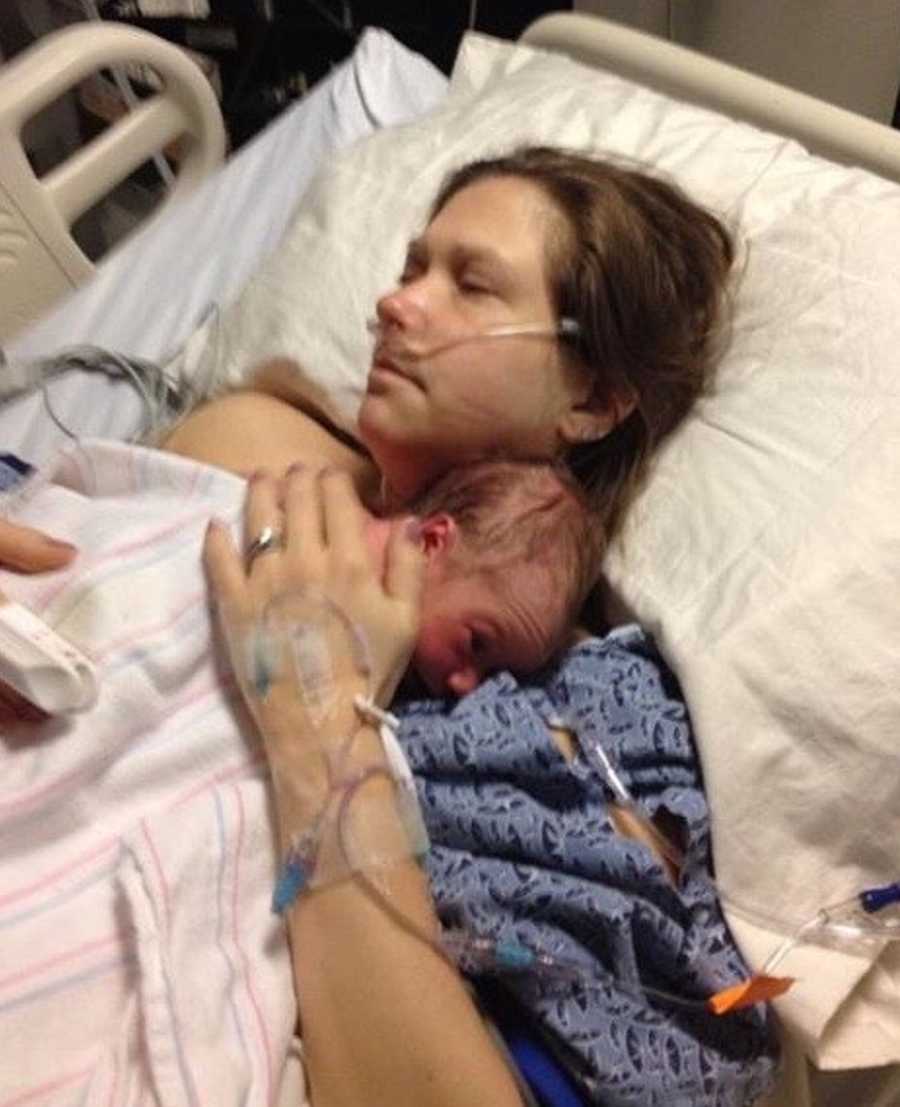
Thankfully, my hospital was equipped with an interventional radiology department and the interventional radiologist was able to stop blood flow to my liver, which in turn stopped the bleeding. Once I woke from surgery, he told me he’d never seen anything like it – that my liver looked like that of a gunshot or knife fight victim, or a victim of a severe car accident. But even still, whether it was the medications or lack of information given to me, I was oblivious to how sick I was. After being stabilized, I was transferred to a larger hospital that was better equipped to handle my care. My baby was transferred as well, but he was in a different ward and I saw very little of him. I spent much of my time swaying in and out of consciousness, and never fully understanding how dire my case was. After an ICU stay and total of 10 days in the hospital, I was sent home to continue recovering. Even before leaving the hospital, no one ever explained to me fully how close to death I was.
Once home, I was in charge of caring for a newborn and of caring for myself. My husband was completing a year of job training that required work weeks of 60-80 hours. We lived far away from any friends or family. I was in a constant haze due to medication and painkillers, while my liver continued to heal. I began to resent the neediness of my newborn baby, when I didn’t have the care I needed myself. I plunged into a dark place of depression and PTSD. I was visited weekly by home nurses. I saw my OB/GYN that delivered my son for my 6-week post op. But none of these people seemed to hear me or recognize that I was suffering emotionally. It seemed that as long as I was physically improving, my mental condition should improve as well. Unfortunately, by this time I’d read up on HELLP Syndrome. I’d discovered that many women in my position die of their livers rupturing, or their babies die. I developed ‘survivor’s guilt’ and spent much of my days wondering what was special about me that my baby and I lived when these other women did not. I felt the manic urge to relive my time in the hospital over and over again, afraid that I would forget details of the event, or I would forget to be grateful that we were alive. I would lie awake all night afraid of falling asleep because maybe I wouldn’t wake up. After all, I was on a cocktail of drugs, including multiple narcotics. Thankfully my chronic pain doctor (a man, nonetheless) noticed my distress and referred me to therapy. I learned some tools and exercises to help control my manic thoughts and I emotionally started to feel better.
During the first year of my son’s life, my health continued to improve and we developed an amazing bond; we’d both survived and thrived after nearly being lost. I started to reach out into the world to find others who’d experienced similar ordeals. I found an amazing place of support in a Facebook group, HELLP Syndrome Survivors. Six years later, some of these women from the internet are still my closest friends. I became involved with the Preeclampsia Foundation, a wonderful organization dedicated to education, support, research, and possible prevention of preeclampsia and other hypertensive disorders of pregnancy. Through the Preeclampsia Foundation’s Champions of Change Summit, I met women who nearly lost their lives due to other pregnancy complications such as hemorrhage, placenta accreta, and amniotic fluid embolism. And it was through all these different pathways that my eyes were opened to just how many of us there are, and that our voices and stories are not being heard.
The United States is the worst developed country in the world to give birth. In our seemingly high tech and medically advanced nation, women are dying (approximately 700 a year) or nearly dying (approximately 50,000 a year) at an alarming rate. Possibly preventable deaths are occurring due to inadequate hospital staff training, failing to follow protocol, improper diagnosis, or simply dismissing patients’ concerns. But there is hope. Two bills are making their way through Congress to try and address maternal mortality and morbidity in the United States, the Maternal Health Accountability Act of 2017 and the Preventing Maternal Deaths Act of 2017. By contacting your local representatives, you can help keep your wives, sisters, daughters, and friends safe during what should be the most amazing and rewarding moments of their lives.
My hope by writing this, it not only draws attention to the issue of maternal mortality and morbidity in the United States, but also will save lives of women who read it. If you are pregnant, do not be afraid to speak up and make yourself heard. You know what is or isn’t normal in your body. Know signs and symptoms of pregnancy disorders and be your own best advocate if you start to exhibit them. Know that many dangerous conditions know no barriers–skin color, ethnicity, socio-economic status, etc. And for those of you strong, brave survivors with stories like mine, please TELL YOUR STORIES! Your stories matter and will make a difference!
I am so grateful for the quick thinking and action of my own doctor. She absolutely saved my life! I am grateful for my husband, family, and friends who’ve supported me the best they can. I am grateful for the support systems, organizations, and networks that exist for women like me, and I am most grateful that I went on to have a second baby boy, complication free, two years after my first. My boys are now 5 years old and 3 years old and we are back home again in Indiana, where our whole family is surrounded by the love and comfort of our family and friends.”

This story was submitted to Love What Matters by Kristin Hinton, 39, of Carmel, Indiana. Have you experienced something similar? We’d like to hear your journey. Submit your own story here, and subscribe to our best stories in our free newsletter here.
Read mores stories like this:
Provide hope for other struggling mothers. SHARE this story on Facebook to help spread awareness.

